User:QuackGuru/Sand 1
green apple flavor
Flavors Enhance Nicotine Vapor Self-administration in Male Mice Cited by and Cited by reviews.
https://pubmed.ncbi.nlm.nih.gov/37919490/ wait for review
https://mdwiki.org/wiki/User_talk:QuackGuru/Sand_1
 | |||
| |||
| Names | |||
|---|---|---|---|
| Trade names | Nicorette, Nicotrol | ||
| |||
| Clinical data | |||
| WHO AWaRe | UnlinkedWikibase error: ⧼unlinkedwikibase-error-statements-entity-not-set⧽ | ||
| Dependence risk | Physical: Low–moderate[3] Psychological: High[4][5] | ||
| Addiction risk | Very high[6] | ||
| Pregnancy category |
| ||
| Routes of use | Inhalation; insufflation; oral – buccal, sublingual, and ingestion; transdermal; rectal | ||
| External links | |||
| AHFS/Drugs.com | Monograph | ||
| Legal | |||
| Legal status |
| ||
| Pharmacokinetics | |||
| Protein binding | <5% | ||
| Metabolism | Primarily hepatic: CYP2A6, CYP2B6, FMO3, others | ||
| Metabolites | Cotinine | ||
| Elimination half-life | 1–2 hours; 20 hours active metabolite | ||
| Excretion | Renal, urine pH-dependent;[7] 10–20% (gum), 30% (inhaled); 10–30% (intranasal) | ||
| Identifiers | |||
| CAS Number |
| ||
| PubChem CID | |||
| IUPHAR/BPS | |||
| DrugBank | |||
| ChemSpider | |||
| UNII | |||
| KEGG | |||
| ChEBI | |||
| ChEMBL | |||
| PDB ligand | |||
| ATC code | |||
| Chemical and physical data | |||
| Formula | C10H14N2 | ||
| Molar mass | 162.236 g·mol−1 | ||
| 3D model (JSmol) | |||
| Chirality | Chiral | ||
| Density | 1.01 g/cm3 | ||
| Melting point | −79 °C (−110 °F) | ||
| Boiling point | 247 °C (477 °F) | ||
| |||
| |||
References
- ↑ "The Medicines (Products Other Than Veterinary Drugs) (General Sale List) Amendment Order 2001". legislation.gov.uk. Retrieved 2 August 2022.
- ↑ Nicotine. PubChem Compound Database. United States National Library of Medicine – National Center for Biotechnology Information. 16 February 2019. Retrieved 12 July 2024.
- ↑ McLaughlin I, Dani JA, De Biasi M (2015). "Nicotine Withdrawal". The Neuropharmacology of Nicotine Dependence. Current Topics in Behavioral Neurosciences. Vol. 24. pp. 99–123. doi:10.1007/978-3-319-13482-6_4. ISBN 978-3-319-13481-9. PMC 4542051. PMID 25638335.
- ↑ Cite error: Invalid
<ref>tag; no text was provided for refs namedDependence-withdrawal - ↑ Cosci F, Pistelli F, Lazzarini N, Carrozzi L (2011). "Nicotine dependence and psychological distress: outcomes and clinical implications in smoking cessation". Psychology Research and Behavior Management. 4: 119–28. doi:10.2147/prbm.s14243. PMC 3218785. PMID 22114542.
- ↑ Hollinger MA (19 October 2007). Introduction to Pharmacology (Third ed.). Abingdon: CRC Press. pp. 222–223. ISBN 978-1-4200-4742-4.
- ↑ Landoni JH. "Nicotine (PIM)". INCHEM. International Programme on Chemical Safety. Retrieved 29 January 2019.
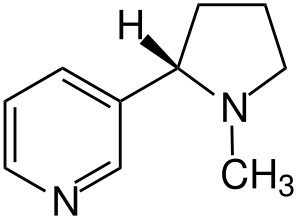 | |
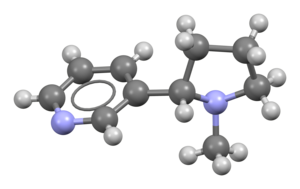 Top: Skeleton representation of a nicotine molecule
Bottom : Ball-and-stick model of a nicotine molecule | |
| Names | |
|---|---|
| Trade names | Nicorette, Nicotrol |
| |
| Clinical data | |
| WHO AWaRe | UnlinkedWikibase error: ⧼unlinkedwikibase-error-statements-entity-not-set⧽ |
| Dependence risk | Physical: Varies[3] Psychological: Mild to severe and from short-lasting to continuous[4] |
| Addiction risk | Very high[5] |
| Pregnancy category |
|
| Routes of use | Inhalation; insufflation; oral – buccal, sublingual, and ingestion; transdermal; rectal |
| External links | |
| AHFS/Drugs.com | Monograph |
| Legal | |
| Legal status |
|
| Pharmacokinetics | |
| Protein binding | <5% |
| Metabolism | Primarily hepatic: CYP2A6, CYP2B6, FMO3, others |
| Metabolites | Cotinine |
| Elimination half-life | 1–2 hours; 20 hours active metabolite |
| Excretion | Renal, urine pH-dependent;[6] 10–20% (gum), 30% (inhaled); 10–30% (intranasal) |
| Identifiers | |
| CAS Number |
|
| PubChem CID | |
| IUPHAR/BPS | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEBI | |
| ChEMBL | |
| PDB ligand | |
| ATC code | |
| Chemical and physical data | |
| Formula | C10H14N2 |
| Molar mass | 162.236 g·mol−1 |
| 3D model (JSmol) | |
| Chirality | Chiral |
| Density | 1.01 g/cm3 |
| Melting point | −79 °C (−110 °F) |
| Boiling point | 247 °C (477 °F) |
| |
| |
| Part of a series on |
| Tobacco |
|---|
 |
Nicotine is a stimulant and potent parasympathomimetic alkaloid that is produced in the nightshade family of plants.[7] It is the nicotine in tobacco that makes it popular.[8] The tobacco species Nicotiana tabacum is a major, non-food industrial crop that is extensively cultivated in several countries.[9] It is this species of tobacco that is mainly associated with consumer products.[8] Nicotine is one of the most widely used recreational drugs[10] and has a damaging impact on public health worldwide.[11] Prolonged drug abuse leads to reliance and consequently withdrawal symptoms upon discontinuing use.[12] Nicotine replacement products are used for smoking cessation to curtail the desire to smoke and to relieve withdrawal symptoms, thereby helping to maintain complete smoking abstinence.[13] Nicotine acts as a receptor agonist at most nicotinic acetylcholine receptors (nAChRs),[14] except at two nicotinic receptor subunits (nAChRα9 and nAChRα10) where it acts as a receptor antagonist.[15]
Nicotine constitutes approximately 0.6–3.0% of the dry weight of tobacco.[16] Usually consistent concentrations of nicotine varying from 2–7 μg/kg (20–70 millionths of a percent wet weight) are found in edible plants in the family Solanaceae, such as potatoes, tomatoes, and eggplant.[17] Nicotine obtained from food is generally trivial unless exceedingly high amounts of certain vegetables are eaten.[17] It functions as an antiherbivore toxin; consequently, nicotine was widely used as an insecticide[18][19] and the Environmental Protection Agency banned its use in the US in 2014.[20] Neonicotinoids (structurally similar to nicotine[21]) such as imidacloprid are widely used, and have been associated with an array of issues to the environment.[22] Outdoor use of three neonicotinoid insecticides were banned in the European Union in 2018.[23]
Nicotine is highly addictive[24][25][26] and is one of the most difficult addictions to do away with.[27] An average cigarette yields about 2 mg of absorbed nicotine; high amounts can be more harmful.[28] Nicotine addiction involves drug-reinforced behavior, compulsive use, and relapse following abstinence.[29] Nicotine dependence involves tolerance, sensitization,[30] physical dependence, psychological dependence,[31] and dependence can cause distress.[32][33] Nicotine withdrawal symptoms include depressed mood, stress, anxiety, irritability, difficulty concentrating, and sleep disturbances.[34] Mild nicotine withdrawal symptoms are measurable in unrestricted smokers, who experience normal moods only as their blood nicotine levels peak, with each cigarette.[35] On quitting, withdrawal symptoms worsen sharply, then gradually improve to a normal state.[35]
Nicotine itself is associated with a variety of health harms.[36][37] This includes an elevated risk of cardiovascular, respiratory, and gastrointestinal disease.[36] Children, youth,[38] and young adults are especially sensitive to the effects of nicotine[39] and it can harm adolescent brain development.[40][41][42] It also damages other growing organs during this period.[43] Nicotine is potentially harmful to non-users.[44][45][46] The International Agency for Research on Cancer does not consider nicotine to be a carcinogen, though several studies demonstrate it is carcinogenic.[36] Nicotine causes birth defects in humans (e.g., alters typical progression of brain development[47]) and is considered a teratogen.[48] The median lethal dose of nicotine in humans is unknown.[49] At low amounts, it has a mild analgesic effect.[50] High doses are known to cause nicotine poisoning,[51] organ failure, and death through paralysis of respiratory muscles,[52] though serious or fatal overdoses are rare.[53]
Uses
Medical
The primary therapeutic use of nicotine is treating nicotine dependence to eliminate smoking and the damage it does to health. Controlled levels of nicotine are given to patients through gums, dermal patches, lozenges, inhalers, or nasal sprays to wean them off their dependence. A 2018 Cochrane Collaboration review found high-quality evidence that all current forms of nicotine replacement therapy (gum, patch, lozenges, inhaler, and nasal spray) increase the chances of successfully quitting smoking by 50–60%, regardless of setting.[13]
Combining nicotine patch use with a faster acting nicotine replacement, like gum or spray, improves the odds of treatment success.[54] Studies indicate that opting for 4 mg of nicotine gum increases the chances of successfully quitting versus a 2 mg dosage.[54]
Nicotine is being researched in studies for possible benefit in treating Parkinson's disease, dementia, ADHD, depression, and sarcoma.[55] The available evidence suggests that nicotine (or nicotinic receptor drugs) have a potential for treating Parkinson's disease, although the detailed courses of treatment have not been established.[56] Studies in 2001 and 2007 found a benefit for administering transdermal nicotine to a limited number of elderly people with advanced dementia and considerable behavioral issues.[57] Under certain conditions, nicotine may improve symptoms of depression.[58] Two studies conducted in 1996 of adults with ADHD were administered a nicotine patch or a nicotine-free patch.[57] Although it is hard to interpret acute drug supervised studies, the results showed no improvement associated with irritability or aggression.[57] 7 mg of transdermal nicotine compared to placebo was administered over a week period to young adults with autism spectrum disorder and aggressive behavior in a 2018 study.[57] Although aggression continued in the nicotine group, there was a decrease in aggression.[57] The decrease in aggression was not statistically meaningful.[57] Nicotine can cause muscle sarcomas in A/J mice.[59] Long-term nicotine use in A/J mice causes leiomyosarcomas and rhabdomyosarcomas.[59] This suggests nicotine directly participates in initiating cancer.[59]
In contrast to recreational nicotine products, which have been designed to maximize the likelihood of addiction, nicotine replacement products are designed to minimize addictiveness.[51]: 112 The more quickly a dose of nicotine is delivered and absorbed, the higher the addiction risk.[32]
Pesticide
In nicotine-producing plants, nicotine functions as an antiherbivory chemical.[60] Nicotine has been used as an insecticide since at least the 1690s, in the form of tobacco extracts[61] (although other components of tobacco also seem to have pesticide effects).[62] The Environmental Protection Agency banned its use in the US in 2014.[20] Nicotine pesticides have not been commercially available in the US since 2014.[63] Homemade pesticides are banned on organic crops[64] and caution is recommended with using nicotine in a pesticide formulation for small gardeners.[65] Nicotine pesticides have been banned in the EU since 2009.[66] Foods are imported from countries in which nicotine pesticides are allowed, such as China, but foods may not exceed maximum nicotine levels.[66][67] Neonicotinoids, such as imidacloprid, which are derived from and structurally similar to nicotine, are widely used as agricultural and veterinary pesticides as of 2016.[68][61] Neonicotinoids such as imidacloprid have been associated with an array of impacts to the environment.[22] Outdoor use of three neonicotinoid insecticides were banned in the European Union in 2018.[23]
Metal accumulation
The tobacco plant can accumulate potentially toxic elements from soil contaminated with heavy metals.[9] Certain potentially toxic elements such as arsenic, cadmium, and lead have been demonstrated to be potential dangers to end-users.[9]
Performance
Nicotine-containing products are sometimes used for the performance-enhancing effects of nicotine on cognition.[69] A 2010 meta-analysis of 41 double-blind, placebo-controlled studies concluded that nicotine or smoking had significant positive effects on aspects of fine motor abilities, alerting and orienting attention, and episodic and working memory.[70] A 2015 review noted that stimulation of the α4β2 nicotinic receptor is responsible for certain improvements in attentional performance;[71] among the nicotinic receptor subtypes, nicotine has the highest binding affinity at the α4β2 receptor (ki=1 nM), which is also the biological target that mediates nicotine's addictive properties.[72] Nicotine has potential beneficial effects, but it also has paradoxical effects, which may be due to the inverted U-shape of the dose-response curve or pharmacokinetic features.[73]
Recreational
Nicotine is used as a recreational drug.[74] It is widely used, highly addictive and hard to discontinue.[25] This commonly abused drug has a damaging impact on public health worldwide.[11] Nicotine is often used compulsively,[75] and dependence can develop within days.[75][76] Recreational drug users commonly use nicotine for its mood-altering effects.[32] Recreational nicotine products include chewing tobacco,[citation needed], cigars,[77] cigarettes,[77] e-cigarettes,[78] snuff,[citation needed] pipe tobacco,[77] nicotine pouches,[79] and snus.[citation needed] Alcohol infused with tobacco is called nicotini.[80] It may include undisclosed ingredients.[81]
Contraindications
Nicotine use for tobacco cessation has few contraindications.[82]
It is not known whether nicotine replacement therapy is effective for smoking cessation in adolescents, as of 2014.[83] It is therefore not recommended to adolescents.[84] It is not safe to use nicotine during pregnancy[85] or breastfeeding.[86] The use of nicotine replacement therapy during pregnancy is controversial.[87] This is because research indicates that the developing fetal brain is susceptible to the harmful effects of nicotine.[87] As a result, the efficacy and safety of using nicotine replacement therapy during pregnancy remains a topic of debate among healthcare providers.[87]
Precautions are needed when using NRT in people who have had a myocardial infarction within two weeks, a serious or worsening angina pectoris, and/or a serious underlying arrhythmia.[84] Using nicotine products during cancer treatment is contraindicated, as nicotine promotes tumor growth, but temporary use of NRTs to quit smoking may be advised for harm reduction.[88]
Nicotine gum is contraindicated in individuals with temporomandibular joint disease.[89] People with chronic nasal disorders and severe reactive airway disease require additional precautions when using nicotine nasal sprays.[84] Nicotine in any form is contraindicated in individuals with a known hypersensitivity to nicotine.[89][84]
Adverse effects

Although it is safer than inhaled tobacco smoke,[36] nicotine itself is associated with a variety of health harms.[36][37] Strong evidence shows that nicotine contributes to disease processes in the lungs, kidneys, heart, liver, and other organs.[91] Nicotine influences fibrosis in various bodily systems by modifying fibroblast activity.[91] Nicotine use substantially elevates catecholamine levels and other hormonal concentrations in the blood, which could lead to profound effects on several organ systems.[91] The maximum harm reduction attainable for smokers is to quit all nicotine use.[92] It is linked to serious morbidity and mortality globally[27] and also poses health risks to certain vulnerable groups such as pregnant women and fetuses, children, and adolescents.[93] Any significant favorable effect of nicotine on people has not been demonstrated.[36]
A 2018 Cochrane Collaboration review lists nine main adverse events related to nicotine replacement therapy: headache, dizziness/light-headedness, nausea/vomiting, gastro-intestinal symptoms, sleep/dream problems, non-ischemic palpitations and chest pain, skin reactions, oral/nasal reactions and hiccups.[94] Many of these were also common in the placebo group without nicotine.[94] Palpitations and chest pain were deemed "rare" and there was no evidence of an increased number of serious cardiac problems compared to the placebo group, even in people with established cardiac disease.[13] Nicotine replacement therapy is often used in smoking cessation, although there is little evidence on the safety and efficacy of their long-term use.[95]
Serious adverse events due to the use of nicotine replacement therapy are extremely rare.[13] At low amounts, it has a mild analgesic effect.[50] At sufficiently high doses, nicotine may result in nausea, vomiting, diarrhea, salivation, bradyarrhythmia, and possibly seizures and hypoventilation.[93]
| Route of administration | Dosage form | Associated side effects of nicotine | Sources |
|---|---|---|---|
| Buccal | Nicotine gum | Indigestion, nausea, hiccups, traumatic injury to oral mucosa or teeth, irritation or tingling of the mouth and throat, oral mucosal ulceration, jaw-muscle ache, burping, gum sticking to teeth, unpleasant taste, dizziness, lightheadedness, headache, and insomnia. | [13][89] |
| Lozenge | Nausea, dyspepsia, flatulence, headache, upper respiratory tract infections, irritation (i.e., a burning sensation), hiccups, sore throat, coughing, dry lips, and oral mucosal ulceration. | [13][89] | |
| Transdermal | Transdermal patch |
Application site reactions (i.e., pruritus, burning, or erythema), diarrhea, dyspepsia, abdominal pain, dry mouth, nausea, dizziness, nervousness or restlessness, headache, vivid dreams or other sleep disturbances, and irritability. | [13][89][96] |
| Intranasal | Nasal spray | Runny nose, nasopharyngeal and ocular irritation, watery eyes, sneezing, and coughing. | [13][89][97] |
| Oral inhalation | Inhaler | Dyspepsia, oropharyngeal irritation (e.g., coughing, irritation of the mouth and throat), rhinitis, and headache. | [13][89][98] |
| All (nonspecific) | Peripheral vasoconstriction, tachycardia (i.e., fast heart rate), elevated blood pressure, increased alertness and cognitive performance. | [89][97] | |
Sleep
Nicotine reduces the amount of rapid eye movement (REM) sleep, slow-wave sleep (SWS), and total sleep time in healthy nonsmokers given nicotine via a transdermal patch, and the reduction is dose-dependent.[99] Acute nicotine intoxication has been found to significantly reduce total sleep time and increase REM latency, sleep onset latency, and non-rapid eye movement (NREM) stage 2 sleep time.[99][100] Depressive non-smokers experience mood and sleep improvements under nicotine administration; however, subsequent nicotine withdrawal has a negative effect on both mood and sleep.[101]
Cardiovascular system
Some researchers, particularly those supporting tobacco harm reduction, hold the position that "most of the harm caused by tobacco use is derived from exposure to combustion products of tobacco".[102] Others disagree, "the relative contributions of nicotine versus non-nicotine components of TC [tobacco cigarette] smoke are unknown".[102] The effects of inhaled nicotine are difficult to isolate from the smoke constituents (oral nicotine delivery has been studied) and "understanding the role of nicotine in cardiopulmonary disease is extraordinarily difficult".[102]
Research has shown that nicotine activates the sympathetic nervous system, constricting coronary arteries, reducing coronary blood flow reserve, and causing transient increases in heart rate, blood pressure, and myocardial contractability.[102] The adverse events of nicotine can be attributed to its dose-dependent effects, with the toxic cardiovascular effects at higher doses.[95] Nicotine use is associated with unfavorable cardiac effects.[103] Because of this, the use of nicotine replacement products should be used cautiously.[103]
The known effects of nicotine on the cardiovascular system are numerous and complex.[104] In favor of a continuous effect on blood pressure is the awareness that muscle sympathetic stimulation is recurrently elevated in smokers, thought to be a result of nicotine.[105] Nicotine may help cause chronic hypertension to lead to accelerated or malignant hypertension by worsening vasoconstriction.[105] Heart rate and blood pressure becomes elevated irrespective of the type of nicotine product used.[105] Elevated heart rate causes a rise in cardiac output.[105] Nicotine can increase serum cholesterol levels,[106] lower coronary blood flow,[105] and constrict blood vessels.[107]
Nicotine is the key component of tobacco smoke causing an increased chance of the cardiovascular disease and cardiac arrest connected with smoking which is thought to be triggered by arrhythmias.[108] A 2018 Cochrane review found that, in rare cases, nicotine replacement therapy can cause non-ischemic chest pain (i.e., chest pain that is unrelated to a heart attack) and heart palpitations, but does not increase the incidence of serious cardiac adverse events (i.e., myocardial infarction, stroke, and cardiac death) relative to controls.[13]
Nicotine appears to increase oxidative stress and the inflammatory burden and accelerate atherosclerosis to increase the risk for cardiovascular disease.[109] However, it is unclear whether nicotine and cotinine affect vascular smooth muscle cell phenotypic switching to a proliferative, migratory phenotype and atherosclerosis development and vascular smooth muscle cell senescence, characteristic of a more advanced plaque.[109] The summation of these events is relevant in the context of atherosclerosis severity as they promote an unstable atherosclerotic cap prone to rupture.[109] A ruptured plaque may block an artery and lead to ischemia, restricted tissue blood flow, which impairs tissue oxygenation and pathological endpoints, such as a heart attack or stroke, by blocking arteries in the heart or brain.[109]
A 2016 review of the cardiovascular toxicity of nicotine concluded, "Based on current knowledge, we believe that the cardiovascular risks of nicotine from e-cigarette use in people without CVD are quite low. We have concerns that nicotine from e-cigarettes could pose some risk for users with CVD."[105] Twenty-five tobacco smokers were exposed to vaping with and without nicotine, and sham vaping (with the e-cigarette turned off) under specific vaping conditions (25 puffs with puff duration of 4 seconds every 30 seconds) in a 2018 randomized crossover trial.[110] No modifications of cardiovascular parameters or oxidative stress were observed with sham vaping and no-nicotine vaping.[110] Instead, vaping with nicotine resulted in the modification of cardiovascular parameters and increased plasma myeloperoxidase.[110] Thus, based on these results, it seems that e-cigarettes' effects on cardiovascular and oxidative stress are due to nicotine and not to high-temperature e-cigarette vehicle vaporization.[110]
Blood-brain barrier

Nicotine is a stimulant that acts as a nicotinic acetylcholine receptor agonist.[111] Its high lipophilicity allows for rapid (10–20 seconds after inhalation) transit across the blood-brain barrier (BBB).[111] Chronic exposure to nicotine disrupts TJ proteins and results in an ionic imbalance within the BBB microenvironment.[111] Consequently, this causes ischemic hypoxia and exacerbates stroke-associated brain edema and neuronal injury.[111] Nicotine exposure alters BBB permeability through TJ protein modulation.[111] It does not affect ZO-1, 2; claudin-1, -3; or -5 TJ protein expression, however, it disrupts the distribution of claudin-3 and ZO-1 TJ proteins.[111] Moreover, nicotine-induced BBB impairment has been shown to involve decreased ZO-1 expression, which affects brain homeostasis.[111] Similarly, static- or flow-based in vitro BBB model studies have reported tobacco-induced alterations in TJ protein expression and re-distribution, which increases intracellular ROS/RNS and the secretory profile of various pro-inflammatory markers.[111] This oxidative stress promotes atherosclerotic lesions and injures biliary epithelial cells (BECs) and TJ proteins via low-density lipoprotein oxidation enhanced by ROS activity.[111] Moreover, this results in increased transcytotic activity across the BBB through induced pinocytosis.[111]
Direct nicotine binding to nicotinic acetylcholine receptors on BECs induces acetylcholine-dependent nitric oxide (NO) release via activation of neurovascular endothelial NO synthase.[111] Here, increased NO2 enhances vascular membrane permeability at the BBB.[111] Furthermore, chronic nicotine administration compromises BBB integrity through TJ protein loss and alteration (ZO-1, claudin-3, and JAM-1).[111] It affects regulated BBB transport and receptor systems that are essential for normal BBB function, as well as decrease the functional activity of ion transporters.[111] Nicotine has been shown to decrease TEER and disturb the BBB transport system, which leads to increased xenobiotic uptake.[111] Nicotine affects the functional activity of ion transporters, including Na+, K+, 2Cl– cotransporter and Na+, K+-ATPase on BECs and inhibits P-gp activity in the CNS.[111] Studies indicate that the H+/organic cation antiporter system is involved in blood-to-brain nicotine transport across BBB endothelial cells TR-BBB13.[111] The precipitated ion gradient change induces brain edema, which further disrupts BBB integrity.[111]
Reinforcement disorders
ΔFosB accumulation from excessive drug use
Top: this depicts the initial effects of high dose exposure to an addictive drug on gene expression in the nucleus accumbens for various Fos family proteins (i.e., c-Fos, FosB, ΔFosB, Fra1, and Fra2).
Bottom: this illustrates the progressive increase in ΔFosB expression in the nucleus accumbens following repeated twice daily drug binges, where these phosphorylated (35–37 kilodalton) ΔFosB isoforms persist in the D1-type medium spiny neurons of the nucleus accumbens for up to 2 months.[112][113] |
Nicotine is highly addictive[24][25][26] and is one of the most difficult addictions to do away with.[27] Nicotine replacement products provide lower amounts of nicotine at a slower speed and are generally less addictive than smoking.[114] US FDA-endorsed nicotine replacement products raise blood nicotine levels more slowly and at decreased amounts relative to traditional cigarettes.[115] As a result, these products exhibit a reduced likelihood of addiction.[115] Its addictiveness depends on the form[116] and in the manner in which it was used.[117]
The potential for nicotine addiction is greater in the brains of children and adolescents.[50] First-time nicotine users develop a dependence reportedly 32% of the time.[118] There may be other substances in cigarette smoke other than nicotine that may enhance its addictiveness.[116] While nicotine is clearly the primary reinforcer in tobacco and e-cigarettes, added flavors may also act as rewards and/or reinforcers in their own right.[119] A 2022 study demonstrated how vaping-related reinforcement behavior is elevated in male mice when self-administering menthol or green-apple flavored e-liquid compared to no flavor e-liquids.[120] Farnesol, a component of green apple flavor, has been shown to significantly increase nicotine-reward related behavior by altering baseline firing of GABA neurons and upregulating nAChR function, especially in male mice.[120]
Nicotine dependence involves aspects of both psychological dependence and physical dependence, since discontinuation of extended use has been shown to produce both affective (e.g., anxiety, irritability, craving, anhedonia) and somatic (mild motor dysfunctions such as tremor) withdrawal symptoms.[34] Psychological disorders can vary from being relatively low in intensity to severe and from being short-lasting to continuous.[4] Withdrawal symptoms peak in one to three days[121] and can persist for several weeks.[122] Some people experience symptoms for 6 months or longer.[123]
Normal between-cigarettes discontinuation, in unrestricted smokers, causes mild but measurable nicotine withdrawal symptoms.[35] These include mildly worse mood, stress, anxiety, cognition, and sleep, all of which briefly return to normal with the next cigarette.[35] Smokers have a worse mood than they typically would have if they were not nicotine-dependent; they experience normal moods only immediately after smoking.[35] Nicotine dependence is associated with poor sleep quality and shorter sleep duration among smokers.[124][125]
In dependent smokers, withdrawal causes impairments in memory and attention, and smoking during withdrawal returns these cognitive abilities to pre-withdrawal levels.[126] The temporarily increased cognitive levels of smokers after inhaling smoke are offset by periods of cognitive decline during nicotine withdrawal.[35] Therefore, the overall daily cognitive levels of smokers and non-smokers are roughly similar.[35]
Nicotine activates the mesolimbic pathway and induces long-term ΔFosB expression (i.e., produces phosphorylated ΔFosB isoforms) in the nucleus accumbens when inhaled or injected frequently or at high doses, but not necessarily when ingested.[127][128][129] Consequently, high daily exposure (possibly excluding oral route) to nicotine can cause ΔFosB overexpression in the nucleus accumbens, resulting in nicotine addiction.[127][128]
Cancer
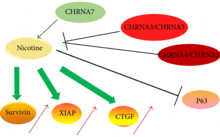
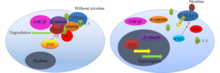

Although the International Agency for Research on Cancer does not consider nicotine to be a carcinogen, several studies demonstrate it is carcinogenic.[36] Nicotine is reportedly directly associated with causing the following cancers: small-cell and non-small-cell lung carcinomas, in addition to head and neck, gastric, pancreatic, gallbladder, liver, colon, breast, cervical, bladder, and kidney cancers.[131] It has a strong tumor-inducing effect on several kinds of cancers.[37] This is because nicotinic receptors are present on the surfaces of both tumor and immune cells, which allows nicotine to directly impact the "tumor microenvironment".[37]
Low levels of nicotine stimulate cell proliferation,[132] while high levels are cytotoxic.[88] In cancer cells, nicotine promotes the epithelial–mesenchymal transition which makes the cancer cells more resistant to drugs that treat cancer.[133] Nicotine may inhibit the antitumor immune response.[88] It has also been reported that exposure to nicotine adversely affects dendritic cells, a cell type that has an important role in anticancer immunosurveillance.[88]
Tobacco-specific nitrosamines are formed through the nitrosation of tobacco alkaloids during the tobacco curing and fermentation process.[134] Nicotine in the mouth and stomach can react to form the tobacco-specific nitrosamine N-Nitrosonornicotine (NNN),[135] a known group 1 carcinogen.[136] The potential for nicotine to facilitate cancer development and progression may extend to non-tobacco forms of nicotine delivery such as nicotine patch, nicotine gum, and nicotine lozenge.[37]
Because it can form nitrosamine compounds (particularly NNN and nicotine-derived nitrosamine ketone (NNK)) through a conversion process, nicotine itself exhibits a strong potential for causing cancer.[137] About 10% of breathed in nicotine is estimated to convert to these nitrosamine compounds.[137] Nitrosamine carcinogenicity is thought to be a result of enhanced DNA methylation and may lead to an agonist response on the nicotinic acetylcholine receptors, which acts to encourage tumors to grow, stay alive, and penetrate into neighboring tissues.[137]
Nicotine inherently possesses properties that encourages the growth of tumors.[138] Several lines of evidence indicate that nicotine may contribute to the development of cancer.[88] Evidence from experimental in vitro studies on cell cultures, in vivo studies on rodents as well as studies on humans inclusive of epidemiological studies indicate that nicotine itself, independent of other tobacco constituents, may stimulate a number of effects of importance in cancer development.[88] Nicotine promotes lung cancer development and accelerates its proliferation, angiogenesis, migration, invasion and epithelial–mesenchymal transition (EMT), via its influence on nAChRs receptors, whose presence has been confirmed in lung cancer cells.[44] A 2019 study showed that mice exposed to nicotine delivered by means of electronic cigarette aerosol develop lung adenocarcinoma.[139] This suggests the need for caution when using nicotine replacement therapies and e-cigarettes.[139]
Strong evidence shows that nicotine encourages the development of cancer.[91] Nicotine, one of the primary cancer-causing agents in cigarettes, affects the angiogenic process.[140] Nicotine acts as a powerful activator of angiogenesis.[141] In experimental and animal models of cancer, nicotine promotes angiogenesis and accelerates tumor growth.[142] For instance, in mice with colon cancer tumors (HT-29), nicotine leads to elevated vascular endothelial growth factor expression and increased microvascular density.[142] Additionally, nicotine induces angiogenesis in lung cancer, where its systemic administration to mice bearing LLC tumors enhances tumor growth by accelerating tumor angiogenesis.[142] Nicotine also promotes angiogenesis in gastric tumors through the upregulation of cytochrome c oxidase subunit 2 and vascular endothelial growth factor receptor 2.[142] In addition, nicotine also accelerated the growth of syngenic colon CMT93 tumor cells by inducing angiogenesis through the recruitment of bone marrow derived EPCs within the tumor.[142] Nicotine also interacts with β2-adrenergic receptors and activates the downstream COX 2 pathway, which can cause cell proliferation in gastric carcinoma and colon cancer.[143]
Nicotine exposure promotes anchorage-independent growth of A549, MDA-MB-468 and MCF-7 cell lines by downregulation of anoikis.[144] Nicotine treatment induces changes in gene expression associated with EMT in lung and breast cancer cells.[144] In colon tumor tissues from HT-29 cell-bearing BALB/c mice, vascular endothelial growth factor expression is elevated by nicotine which correlates with enhanced microvessel density.[144] Nicotine stimulation of nicotinic acetylcholine receptor (nAChRs) enhances SW620 and LOVO colorectal cancer cell invasion and metastasis in vitro via the activation of p38 mitogen-activated protein kinases signaling pathway.[144] Similarly, nicotine pretreatment stimulates the activation of alpha-9 nicotinic receptor which mediates MCF-7 and MDA-MB-231 breast cancer cell migration via the expression of epithelial mesenchymal transition markers.[144] Furthermore, implantation of CD18/HPAF pancreatic cancer cells into immuno-deficient mice, demonstrates that nicotine treatment activates alpha-7 nicotinic receptor and mediates tumor metastasis via Janus kinase 2 (JAK2)/STAT3 signaling in synergy with mitogen activated protein kinase (Ras/Raf/MEK/ERK1/2) signaling pathway.[144]
Studies indicated nicotine is able to induce cancer directly via promoting proliferation, inhibiting apoptosis of cancer cells, and stimulating tumor angiogenesis.[130] These findings suggest that nicotinic acetylcholine receptors are the central regulatory module of multiple downstream oncogenic signaling pathways in mediating the cellular responses of nicotine and its derivatives.[130] And nicotinic acetylcholine receptors mediated effects of nicotine function in coalition with the mutagenic effects of the cancerogenic nitrosamine derivatives and reactive oxygen species activated by intracellular nicotine to promote tumor development and progression in tobacco related cancers.[130]
The affinity of NNK for alpha-7 nicotinic receptor is 1,300 times higher than that of nicotine, whereas the affinity of NNN for heteromeric α–β nAChRs is 5,000 times higher than that of nicotine.[130] Thus NNK and NNN can cause displacement of nicotine from these receptors as a result of their higher affinity for nicotinic acetylcholine receptors.[130] Therefore nitrosamines may cause many of the cardiovascular, neuropsychological, and cancer-stimulating effects similar to nicotine.[130] Thus, nicotine, NNK, and NNN bind to nicotinic acetylcholine receptors and other receptors, leading to activation of the serine/threonine kinase AKT, protein kinase A (PKA), and other factors.[130] Accelerated tumor growth was observed after systemic administration of nicotine in xenograft mouse model.[130]
Nicotine and NNK promote the synthesis and release of adrenaline and noradrenaline to promote the proliferation and migration of pancreatic cancer cells.[130] Nicotine promotes metastasis of pancreatic cancer through alpha-7 nicotinic receptor mediated Mucin-4 (MUC4) upregulation.[130] Chronic exposure to nicotine leads to increased expression of MUC4 in pancreatic cancer through activation of the alpha-7 nicotinic receptor/JAK2/STAT3 and the MEK/ERK1/ERK2 signaling cascade.[130] And tobacco smoking induces chronic inflammation to trigger the development of pancreatic cancer.[130] The oncogenic effects of nicotinic acetylcholine receptor signaling in pancreatic cancer are also supported by the animal experiments, and N-nitroso compounds, formed from nicotine by nitrosation during the processing of tobacco plants, can cause pancreatic cancer in Syrian golden hamsters.[130]
Nicotinic acetylcholine receptors mediated the nicotine activation of the oncogenic YAP1 of the Hippo signaling pathway in esophageal cancer.[130] The upregulation of YAP1 in esophageal cancer samples is significantly associated with the smoking history of the patients, and the effects are regulated by protein kinase C signaling, as protein kinase C specific inhibitor can abolish the activation of YAP1 by nicotine treatment.[130] Nicotine promotes head and neck cancer through activation of endogenous FOXM1 activity by loss of heterozygosity involving the whole of chromosome 13 and copy number abnormality in oral keratinocytes.[130] Cellular and molecular studies on nicotinic acetylcholine receptors indicate that chronic exposure to nicotine or nicotine-derived carcinogenic nitrosamines upregulates the alpha-7 nicotinic receptor and alpha-9 nicotinic receptor and desensitizes the heteromeric alpha-4 beta-2 nicotinic receptor to activate the oncogenic pathways, promotes tumor angiogenesis, and inhibits drug induced apoptosis in multiple types of cancers.[130]
In addition to promoting angiogenesis, nicotine could recruit alpha-7 nicotinic receptors to boost vasculogenesis.[145] A 2011 study shows that nicotine induced proliferation, migration and tube formation also in ECFCs and that this effect was inhibited by mecamylamine or α-bungarotoxin.[145] Moreover, nicotine triggered EPC mobilization from bone marrow in a cohort of mice xenografted with colorectal cancer cells, thereby fostering tumor growth and vascularization.[145] The pro-angiogenic effect of nicotine was, therefore, likely to be mediated by nicotinic acetylcholine receptors.[145]
Genotoxicity
Nicotine causes DNA damage in several types of human cells as judged by assays for genotoxicity such as the comet assay, cytokinesis-block micronucleus test and chromosome aberrations test. In humans, this damage can happen in primary parotid gland cells,[146] lymphocytes,[147] and respiratory tract cells.[148]
Youth
Youth are especially vulnerable as a consequence of the impact of nicotine on the growing neural tissue, possibility of being addicted for life, aggressive industry promotion, and the ease of obtaining nicotine products.[50] Nicotine can harm adolescent brain development, which continues into the early to mid-20s.[42] Exposure to nicotine during adolescence also damages other growing organs.[43] Young people who use nicotine products in any form, including e-cigarettes, are uniquely at risk for long-lasting effects.[149] It leads to irreversible alterations in the growing brains of youth and young adults.[150] Nicotine exposure during adolescence adversely affects cognitive development.[93] Nicotine consumption during adolescence is associated with cognitive impairment post-adolescent with diminished attention span and increased impulsivity.[40] Adolescent nicotine consumption is associated with the long-term neurochemical and behavioral altercations which suggests that nicotine is capable of exerting epigenetic alterations in the neural genome.[40]
In such a critical phase of human development, nicotine exposure may prime the brain's reward system increasing pleasing effects of other substances of abuse.[151] As evidence of this, youngsters vaping e-cigarettes display a greater risk of co-occurring alcohol and/or marijuana use.[151]
Pregnancy and breastfeeding
Nicotine has been shown to produce birth defects in some animal species, but not others.[152] It is considered a teratogen.[48] In animal studies that resulted in birth defects, researchers found that nicotine negatively affects fetal brain development and pregnancy outcomes;[152][51] the negative effects on early brain development are associated with abnormalities in brain metabolism and neurotransmitter system function.[153] Nicotine crosses the placenta and is found in the breast milk of mothers who smoke as well as mothers who inhale passive smoke.[154]
Nicotine exposure in utero is responsible for several complications of pregnancy and birth: pregnant women who smoke are at greater risk for both miscarriage and stillbirth and infants exposed to nicotine in utero tend to have lower birth weights.[47] Some evidence suggests that in utero nicotine exposure influences the occurrence of certain conditions later in life, including type 2 diabetes, obesity, hypertension, neurobehavioral defects, respiratory dysfunction, and infertility.[155]
Children exposed to nicotine before birth are susceptible to having several long-long health issues such as reduced function of the endocrine, reproductive, respiratory, cardiovascular, and nervous systems.[47] Nicotine is on the California's Proposition 65 list of chemicals known to the state to cause cancer, birth defects, or other reproductive harm.[154]
Multigenerational effects
The multigenerational epigenetic effect of nicotine on lung function has been demonstrated.[156] The use of any nicotine-infused product during pregnancy or during pregnancy and during the breastfeeding, postpartum period leads to the "concurrent exposure of three generations to nicotine".[157]
Bystanders

People are involuntarily exposed to nicotine from second-hand and third-hand aerosol, as well as second-hand and third-hand smoke.[26] The majority of review articles concluding that second-hand smoking does not represent a health risk are written by authors who have an association with the tobacco industry.[159] There is about a 20% increase in the risk of developing lung cancer among never-smokers who are exposed to second-hand smoke.[160] A 2014 study has shown that non-users absorb nicotine from exhaled e-cigarette aerosol at amounts comparable with exposure to second-hand smoke as assessed by salivary cotinine levels.[161] The impacts on health from inadvertent or second-hand and third-hand exposure to nicotine from nicotine products that do not involve combustion are not clearly understood.[162]
Nicotine is potentially harmful to non-users.[44][45][46] A 2019 analyses of the health risk of e-cigarette use for bystanders indicate that exposure may be associated with systemic effects of nicotine action and increased risk of tumors.[44] Second-hand exposure to nicotine and other chemicals in indoor places may result in serious adverse effects.[50] Exhaled nicotine from an e-cigarette can deposit onto surfaces and subsequently negatively affect the health of those exposed (third-hand exposure).[163] There is evidence that nicotine metabolites in serum, as well as saliva and urine cotinine levels, are superimposable among non-using adults secondhandedly exposed to e-cigarettes and conventional cigarettes.[151] The health impacts of exposure to nicotine in infants and children are not clear.[93]
The carcinogenic tobacco-specific n-nitrosamines are known risk factors for head and neck cancers.[164] Nicotine from e-cigarette aerosol or e-liquid may remain on the surface for several weeks or even months and react with the environment to form tobacco-specific n-nitrosamines compounds along with nitric acid, which can result in inhalation, ingestion, or dermal exposure to carcinogens.[164]
The tobacco industry financed independent organizations to create research that seemed not connected to the tobacco industry and would bolster its image.[165] The tobacco industry documents indicated the tobacco industry rejected scholarly research that did not agree with their view that environmental tobacco smoke is a minor risk to health.[165] In 1981, Takeshi Hirayama's paper was published in The BMJ which become a historic study on environmental tobacco smoke and lung cancer in cohabiting partners.[165] The tobacco industry publicly denounced Hirayama's paper, but privately it knew that some of its own advisors had determined the research was sound.[165] Tobacco industry documents showed that as soon as 1975 the tobacco industry knew that environmental tobacco smoke can be damaging to health.[165] A 2001 review concluded that the "Industry documents illustrate a deliberate strategy to use scientific consultants to discredit the science on ETS [environmental tobacco smoke]".[165] The tobacco industry acknowledged that it could not state that environmental tobacco smoke is safe and recognized the concern would have a “devastating effect on sales”.[165]
Overdose

Nicotine is a harmful poison.[36] It is unlikely that a person would overdose on nicotine through smoking alone. The US Food and Drug Administration (FDA) stated in 2013 that there are no significant safety concerns associated with the use of more than one form of over-the-counter (OTC) nicotine replacement therapy at the same time, or using OTC NRT at the same time as another nicotine-containing product, like cigarettes.[166] The median lethal dose of nicotine in humans is unknown.[49][28] Nevertheless, nicotine has a relatively high toxicity in comparison to many other alkaloids such as caffeine, which has an LD50 of 127 mg/kg when administered to mice.[167] At sufficiently high doses, it is associated with nicotine poisoning,[51] which, while common in children, rarely results in significant morbidity or death.[152] Fatal dose outcomes is 0.5–1.0 mg per kg body weight for an adult and likely as low as 0.1–0.2 mg per kg body weight for a child.[50] As low as 2 mg of nicotine has resulted in toxicity in children.[168]
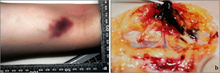
The initial symptoms of a nicotine overdose typically include nausea, vomiting, diarrhea, hypersalivation, abdominal pain, tachycardia (rapid heart rate), hypertension (high blood pressure), tachypnea (rapid breathing), headache, dizziness, pallor (pale skin), auditory or visual disturbances, and perspiration, followed shortly after by marked bradycardia (slow heart rate), bradypnea (slow breathing), and hypotension (low blood pressure).[152] An increased respiratory rate (i.e., tachypnea) is one of the primary signs of nicotine poisoning.[152] At sufficiently high doses, somnolence (sleepiness or drowsiness), confusion, syncope (loss of consciousness from fainting), shortness of breath, marked weakness, seizures, and coma may occur.[6][152] Lethal nicotine poisoning rapidly produces seizures, and death – which may occur within minutes – is believed to be due to respiratory paralysis.[152]
There has been several reports on cases of poisoning from intraperitoneal nicotine and nicotine-containing products, mainly in infants.[169] However, few have reported about poisoning from intravenous nicotine in adults.[169]
Toxicity
Today nicotine is less commonly used in agricultural insecticides, which was a main source of poisoning. More recent cases of poisoning typically appear to be in the form of green tobacco sickness,[152] accidental ingestion of tobacco or tobacco products, or ingestion of nicotine-containing plants.[170][171][172] People who harvest or cultivate tobacco may experience green tobacco sickness, a type of nicotine poisoning caused by dermal exposure to wet tobacco leaves. This occurs most commonly in young, inexperienced tobacco harvesters who do not consume tobacco.[170][173] People can be exposed to nicotine in the workplace by breathing it in, skin absorption, swallowing it, or eye contact. The Occupational Safety and Health Administration (OSHA) has set the legal limit (permissible exposure limit) for nicotine exposure in the workplace as 0.5 mg/m3 skin exposure over an 8-hour workday. The US National Institute for Occupational Safety and Health (NIOSH) has set a recommended exposure limit (REL) of 0.5 mg/m3 skin exposure over an 8-hour workday. At environmental levels of 5 mg/m3, nicotine is immediately dangerous to life and health.[174]
Drug interactions
Pharmacodynamic
- Potential interaction with sympathomimetic drugs (adrenergic agonists) and sympatholytic drugs (alpha-blockers and beta-blockers).[89]
Pharmacokinetic
Nicotine and cigarette smoke both induce the expression of liver enzymes (e.g., certain cytochrome P450 proteins) which metabolize drugs, leading to the potential for alterations in drug metabolism.[89]
- Smoking cessation may decrease the metabolism of acetaminophen, beta-blockers, caffeine, oxazepam, pentazocine, propoxyphene, theophylline, and tricyclic antidepressants, leading to higher plasma concentrations of these drugs.[89]
- Possible alteration of nicotine absorption through the skin from the transdermal nicotine patch by drugs that cause vasodilation or vasoconstriction.[89]
- Possible alteration of nicotine absorption through the nasal cavity from the nicotine nasal spray by nasal vasoconstrictors (e.g., xylometazoline).[89]
- Possible alteration of nicotine absorption through oral mucosa from nicotine gum and lozenges by food and drink that modify salivary pH.[89]
Pharmacology
Pharmacodynamics
Nicotine acts as a receptor agonist at most nicotinic acetylcholine receptors (nAChRs),[15][175] except at two nicotinic receptor subunits (nAChRα9 and nAChRα10) where it acts as a receptor antagonist.[15] Such antagonism results in mild analgesia.
Central nervous system

By binding to nicotinic acetylcholine receptors in the brain, nicotine elicits its psychoactive effects and increases the levels of several neurotransmitters in various brain structures – acting as a sort of "volume control".[176][177] Nicotine has a higher affinity for nicotinic receptors in the brain than those in skeletal muscle, though at toxic doses it can induce contractions and respiratory paralysis.[178] Nicotine's selectivity is thought to be due to a particular amino acid difference on these receptor subtypes.[179] Nicotine is unusual in comparison to most drugs, as its profile changes from stimulant to sedative with increasing dosages, a phenomenon known as "Nesbitt's paradox" after the doctor who first described it in 1969.[180][181] At very high doses it dampens neuronal activity.[182] Nicotine induces both behavioral stimulation and anxiety in animals.[6] Research into nicotine's most predominant metabolite, cotinine, suggests that some of nicotine's psychoactive effects are mediated by cotinine.[183]
Nicotine activates nicotinic receptors (particularly α4β2 nicotinic receptors, but also α5 nAChRs) on neurons that innervate the ventral tegmental area and within the mesolimbic pathway where it appears to cause the release of dopamine.[184][185] This nicotine-induced dopamine release occurs at least partially through activation of the cholinergic–dopaminergic reward link in the ventral tegmental area.[185][186] Nicotine can modulate the firing rate of the ventral tegmental area neurons.[186] Nicotine also appears to induce the release of endogenous opioids that activate opioid pathways in the reward system.[184] These actions are largely responsible for the strongly reinforcing effects of nicotine, which often occur in the absence of euphoria;[184] however, mild euphoria from nicotine use can occur in some individuals.[184] Chronic nicotine use inhibits class I and II histone deacetylases in the striatum, where this effect plays a role in nicotine addiction.[187][188]
Sympathetic nervous system
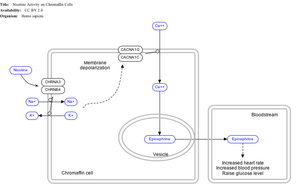
Nicotine also activates the sympathetic nervous system,[189] acting via splanchnic nerves to the adrenal medulla, stimulating the release of epinephrine. Acetylcholine released by preganglionic sympathetic fibers of these nerves acts on nicotinic acetylcholine receptors, causing the release of epinephrine (and norepinephrine) into the bloodstream.
Adrenal medulla
By binding to ganglion type nicotinic receptors in the adrenal medulla, nicotine increases flow of adrenaline (epinephrine), a stimulating hormone and neurotransmitter. By binding to the receptors, it causes cell depolarization and an influx of calcium through voltage-gated calcium channels. Calcium triggers the exocytosis of chromaffin granules and thus the release of epinephrine (and norepinephrine) into the bloodstream. The release of epinephrine (adrenaline) causes an increase in heart rate, blood pressure and respiration, as well as higher blood glucose levels.[190]
Pharmacokinetics
As nicotine enters the body, it is distributed quickly through the bloodstream and crosses the blood–brain barrier reaching the brain within 10–20 seconds after inhalation.[192] The elimination half-life of nicotine in the body is around two hours.[193] Nicotine is primarily excreted in urine and urinary concentrations vary depending upon urine flow rate and urine pH.[6]
The amount of nicotine absorbed by the body from smoking can depend on many factors, including the types of tobacco, whether the smoke is inhaled, and whether a filter is used. However, it has been found that the nicotine yield of individual products has only a small effect (4.4%) on the blood concentration of nicotine,[194] suggesting "the assumed health advantage of switching to lower-tar and lower-nicotine cigarettes may be largely offset by the tendency of smokers to compensate by increasing inhalation".
Nicotine has a half-life of 1–2 hours. Cotinine is an active metabolite of nicotine that remains in the blood with a half-life of 18–20 hours, making it easier to analyze.[195]
Nicotine is metabolized in the liver by cytochrome P450 enzymes (mostly CYP2A6, and also by CYP2B6) and FMO3, which selectively metabolizes (S)-nicotine. A major metabolite is cotinine. Other primary metabolites include nicotine N'-oxide, nornicotine, nicotine isomethonium ion, 2-hydroxynicotine and nicotine glucuronide.[196] Under some conditions, other substances may be formed such as myosmine.[197][198]
Glucuronidation and oxidative metabolism of nicotine to cotinine are both inhibited by menthol, an additive to mentholated cigarettes, thus increasing the half-life of nicotine in vivo.[199]
Metabolism
Nicotine decreases hunger and as a consequence food consumption,[200] alongside increasing energy expenditure.[201] The majority of research shows that nicotine reduces body weight, but some researchers have found that nicotine may result in weight gain under specific types of eating habits in animal models.[200] Nicotine effect on weight appears to result from nicotine's stimulation of α3β4 nAChR receptors located in the POMC neurons in the arcuate nucleus and subsequently the melanocortin system, especially the melanocortin-4 receptors on second-order neurons in the paraventricular nucleus of the hypothalamus, thus modulating feeding inhibition.[186][200] POMC neurons are a precursor of the melanocortin system, a critical regulator of body weight and peripheral tissue such as skin and hair.[200]
Chemistry
| NFPA 704 safety square | |
|---|---|
The fire diamond hazard sign for nicotine |
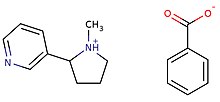
Nicotine is a hygroscopic, colorless to yellow-brown, oily liquid, that is readily soluble in alcohol, ether or light petroleum. It is miscible with water in its neutral amine base form between 60 °C and 210 °C. It is a dibasic nitrogenous base, having Kb1=1×10−6, Kb2=1×10−11.[202] It readily forms ammonium salts with acids that are usually solid and water-soluble. Its flash point is 95 °C and its auto-ignition temperature is 244 °C.[203] Nicotine is readily volatile (vapor pressure 5.5 Pa at 25 °C)[202] On exposure to ultraviolet light or various oxidizing agents, nicotine is converted to nicotine oxide, nicotinic acid (niacin, vitamin B3), and methylamine.[204]
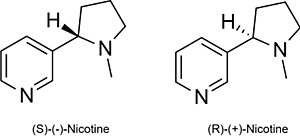
Nicotine is chiral and hence optically active, having two enantiomeric forms. The naturally occurring form of nicotine is levorotatory with a specific rotation of [α]D=–166.4° ((−)-nicotine). The dextrorotatory form, (+)-nicotine is physiologically less active than (−)-nicotine. (−)-nicotine is more toxic than (+)-nicotine.[205] The salts of (+)-nicotine are usually dextrorotatory; this conversion between levorotatory and dextrorotatory upon protonation is common among alkaloids.[204] The hydrochloride and sulfate salts become optically inactive if heated in a closed vessel above 180 °C.[204] Anabasine is a structural isomer of nicotine, as both compounds have the molecular formula {{chem2|auto=1|C10H14N2}.
Nicotine that is found in natural tobacco is primarily (99%) the S-enantiomer.[206] Conversely, the most common chemistry synthetic methods for generating nicotine yields a product that is approximately equal proportions of the S- and R-enantiomers.[207] This suggests that tobacco-derived and synthetic nicotine can be determined by measuring the ratio of the two different enantiomers, although means exist for adjusting the relative levels of the enantiomers or performing a synthesis that only leads to the S-enantiomer. There is limited data on the relative physiological effects of these two enantiomers, especially in people. However, the studies to date indicate that (S)-nicotine is more potent than (R)-nicotine and (S)-nicotine causes stronger sensations or irritation than (R)-nicotine. Studies have not been adequate to determine the relative addictiveness of the two enantiomers in people.
Pod mod e-cigarettes use nicotine in the form of a protonated nicotine, rather than free-base nicotine found in earlier generations.[208]
Occurrence
Nicotine is a secondary metabolite produced in a variety of plants in the family Solanaceae, most notably in tobacco Nicotiana tabacum, where it can be found at high concentrations of 0.5 to 7.5%.[209] Nicotine is also found in the leaves of other tobacco species, such as Nicotiana rustica.[8] Nicotine production is strongly induced in response to wounding as part of a jasmonate-dependent reaction.[210] Specialist insects on tobacco, such as the tobacco hornworm (Manduca sexta), have a number of adaptations to the detoxification and even adaptive re-purposing of nicotine.[211] Nicotine is also found at low concentrations in the nectar of tobacco plants, where it may promote outcrossing by affecting the behavior of hummingbird pollinators.[212]
Nicotine occurs in smaller amounts (varying from 2–7 μg/kg, or 20–70 millionths of a percent wet weight[17]) in other Solanaceaeous plants, including some crop species such as potatoes, tomatoes, eggplant, and peppers,[17][213] as well as non-crop species such as Duboisia hopwoodii.[202] The amounts of nicotine in tomatoes lowers substantially as the fruit ripens.[17] Nicotine content in tea leaves is greatly inconsistent and in some cases considerably greater than in the Solanaceae fruits.[17] Nicotine content in tea leaves is greatly inconsistent and in some cases considerably greater than in the Solanaceae fruits.[17]
A 1999 report found "In some papers it is suggested that the contribution of dietary nicotine intake is significant when compared with exposure to ETS [environmental tobacco smoke] or by active smoking of small numbers of cigarettes. Others consider the dietary intake to be negligible unless inordinately large amounts of specific vegetables are consumed."[17] Whilst food consumption levels of dietary nicotine are insignificant compared with moderate second-hand smoke exposure, the consumption of high quantities might contribute to low-level elevations in serum cotinine (e.g. 80 g of eggplant is equivalent to approximately 0.01 ng/ml of serum cotinine).[214] The amount of nicotine eaten per day is roughly around 1.4 and 2.25 μg/day at the 95th percentile.[17] These numbers may be low due to insufficient food intake data.[17] The concentrations of nicotine in vegetables are difficult to measure accurately, since they are very low (parts per billion range).[215]
Preparation
The first laboratory preparation of nicotine (as its racemate) was described in 1904.[216]
The starting material was an N-substituted pyrrole derivative, which was heated to convert it by a [1,5] sigmatropic shift to the isomer with a carbon bond between the pyrrole and pyridine rings, followed by methylation and selective reduction of the pyrrole ring using tin and hydrochloric acid.[216][217] Many other syntheses of nicotine, in both racemic and chiral forms have since been published.[218]
Biosynthesis

The biosynthetic pathway of nicotine involves a coupling reaction between the two cyclic structures that comprise nicotine. Metabolic studies show that the pyridine ring of nicotine is derived from niacin (nicotinic acid) while the pyrrolidine is derived from N-methyl-Δ1-pyrrollidium cation.[219][220] Biosynthesis of the two component structures proceeds via two independent syntheses, the NAD pathway for niacin and the tropane pathway for N-methyl-Δ1-pyrrollidium cation.
The NAD pathway in the genus Nicotiana begins with the oxidation of aspartic acid into α-imino succinate by aspartate oxidase (AO). This is followed by a condensation with glyceraldehyde-3-phosphate and a cyclization catalyzed by quinolinate synthase (QS) to give quinolinic acid. Quinolinic acid then reacts with phosphoribosyl pyrophosphate catalyzed by quinolinic acid phosphoribosyl transferase (QPT) to form niacin mononucleotide (NaMN). The reaction now proceeds via the NAD salvage cycle to produce niacin via the conversion of nicotinamide by the enzyme nicotinamidase.[citation needed]
The N-methyl-Δ1-pyrrollidium cation used in the synthesis of nicotine is an intermediate in the synthesis of tropane-derived alkaloids. Biosynthesis begins with decarboxylation of ornithine by ornithine decarboxylase (ODC) to produce putrescine. Putrescine is then converted into N-methyl putrescine via methylation by SAM catalyzed by putrescine N-methyltransferase (PMT). N-methylputrescine then undergoes deamination into 4-methylaminobutanal by the N-methylputrescine oxidase (MPO) enzyme, 4-methylaminobutanal then spontaneously cyclize into N-methyl-Δ1-pyrrollidium cation.[citation needed]
The final step in the synthesis of nicotine is the coupling between N-methyl-Δ1-pyrrollidium cation and niacin. Although studies conclude some form of coupling between the two component structures, the definite process and mechanism remains undetermined. The current agreed theory involves the conversion of niacin into 2,5-dihydropyridine through 3,6-dihydronicotinic acid. The 2,5-dihydropyridine intermediate would then react with N-methyl-Δ1-pyrrollidium cation to form enantiomerically pure (−)-nicotine.[221]
Detection in body fluids
Nicotine can be quantified in blood, plasma, or urine to confirm a diagnosis of poisoning or to facilitate a medicolegal death investigation. Urinary or salivary cotinine concentrations are frequently measured for the purposes of pre-employment and health insurance medical screening programs. Careful interpretation of results is important, since passive exposure to cigarette smoke can result in significant accumulation of nicotine, followed by the appearance of its metabolites in various body fluids.[222][223] Nicotine use is not regulated in competitive sports programs.[224]
Methods for analysis of enantiomers
Methods for measuring the two enantiomers are straightforward and include normal-phase liquid chromatography,[206] liquid chromatography with a chiral column.[225] However, since methods can be used to alter the two enantiomers, it may not be possible to distinguish tobacco-derived from synthetic nicotine simply by measuring the levels of the two enantiomers. A new approach uses hydrogen and deuterium nuclear magnetic resonance to distinguish tobacco-derived and synthetic nicotine based on differences the substrates used in the natural synthetic pathway performed in the tobacco plant and the substrates most used in synthesis.[226] Another approach measures the carbon-14 content which also differs between natural and laboratory-based tobacco.[227] These methods remain to be fully evaluated and validated using a wide range of samples.
History, society, and culture

Nicotine was originally isolated from the tobacco plant in 1828 by chemists Wilhelm Heinrich Posselt and Karl Ludwig Reimann from Germany, who believed it was a poison.[228][229] Its chemical empirical formula was described by Melsens in 1843,[230] its structure was discovered by Adolf Pinner and Richard Wolffenstein in 1893,[231][232][233][clarification needed] and it was first synthesized by Amé Pictet and A. Rotschy in 1904.[216][234]
Nicotine is named after the tobacco plant Nicotiana tabacum, which in turn is named after the French ambassador in Portugal, Jean Nicot de Villemain, who sent tobacco and seeds to Paris in 1560, presented to the French King,[235] and who promoted their medicinal use. Smoking was believed to protect against illness, particularly the plague.[235] In 1610, Francis Bacon noted that trying to give up tobacco use was very hard.[236]
Tobacco was introduced to Europe in 1559, and by the late 17th century, it was used not only for smoking but also as an insecticide. After World War II, over 2,500 tons of nicotine insecticide were used worldwide, but by the 1980s the use of nicotine insecticide had declined below 200 tons. This was due to the availability of other insecticides that are cheaper and less harmful to mammals.[19]
The nicotine content of popular American-brand cigarettes has increased over time, and one study found that there was an average increase of 1.78% per year between the years of 1998 and 2005.[237]
Although methods of production of synthetic nicotine have existed for decades,[238] it was believed that the cost of making nicotine by laboratory synthesis was cost prohibitive compared to extracting nicotine from tobacco.[239] However, recently synthetic nicotine started to be found in different brands of e-cigarettes and oral pouches and marketed as "tobacco-free."[240]
The US FDA is tasked with reviewing tobacco products such as e-cigarettes and determining which can be authorized for sale. In response to the likelihood that FDA would not authorize many e-cigarettes to be marketed, e-cigarette companies began marketing products that they claimed to contain nicotine that were not made or derived from tobacco, but contained synthetic nicotine instead, and thus, would be outside FDA's tobacco regulatory authority.[241] Similarly, nicotine pouches that claimed to contain non-tobacco (synthetic) nicotine were also introduced. The cost of synthetic nicotine has decreased as the market for the product increased. In March 2022, the U.S. Congress passed a law (the Consolidated Appropriations Act, 2022) that expanded FDA's tobacco regulatory authority to include tobacco products containing nicotine from any source, thereby including products made with synthetic nicotine.
Legal status
In the US, nicotine products and nicotine replacement therapy products like Nicotrol are only available to people 21 and above; proof of age is required; not for sale in vending machine or from any source where proof of age cannot be verified. In some states[where?], these products are only available to persons over the age of 21.[medical citation needed][where?] Many states in the US have implemented a Tobacco 21 law for tobacco products, raising the minimum age from 18 to 21.[242] As of December 2019, the minimum age to sell any tobacco product is in the US is 21 at the federal level.[243] This law is not applicable to nicotine-free e-liquids or to the devices themselves.[244]
In the European Union, the minimum age to purchase nicotine products is 18. However, there is no minimum age requirement to use tobacco or nicotine products.[245]
Following the United Kingdom's withdrawal from the European Union, The Tobacco Products and Nicotine Inhaling Products (Amendment) (EU Exit) Regulations 2020 took the place of the EU's Tobacco Products Directive (TPD) as the governing regulatory instrument.[246]
In media
In some anti-smoking literature, the harm that tobacco smoking and nicotine addiction does is personified as Nick O'Teen, represented as a humanoid with some aspect of a cigarette or cigarette butt about him or his clothes and hat.[247] Nick O'Teen was a villain that was created for the Health Education Council.[247] The character was featured in three animated anti-smoking public service announcements in which he tries to get kids addicted to cigarettes before being foiled by the DC Comics character Superman.[247]
Nicotine was often compared to caffeine in advertisements in the 1980s by the tobacco industry, and later in the 2010s by the e-cigarette industry, in an effort to reduce the stigmatization and the public perception of the risks associated with nicotine use.[248]
Research
Central nervous system
While acute/initial nicotine intake causes activation of neuronal nicotine receptors, chronic low doses of nicotine use leads to desensitization of those receptors (due to the development of tolerance) and results in an antidepressant effect, with early research showing low dose nicotine patches could be an effective treatment of major depressive disorder in non-smokers.[249]
Though tobacco smoking is associated with an increased risk of Alzheimer's disease,[250] there is evidence that nicotine itself has the potential to prevent and treat Alzheimer's disease.[251]
Smoking is associated with a decreased risk of Parkinson's Disease; however, it is unknown whether this is due to people with healthier brain dopaminergic reward centers (the area of the brain affected by Parkinson's) being more likely to enjoy smoking and thus pick up the habit, nicotine directly acting as a neuroprotective agent, or other compounds in cigarette smoke acting as neuroprotective agents.[252]
Immune system
Immune cells of both the Innate immune system and adaptive immune systems frequently express the α2, α5, α6, α7, α9, and α10 subunits of nicotinic acetylcholine receptors.[253] Evidence suggests that nicotinic receptors which contain these subunits are involved in the regulation of immune function.[253]
Optopharmacology
A photoactivatable form of nicotine, which releases nicotine when exposed to ultraviolet light with certain conditions, has been developed for studying nicotinic acetylcholine receptors in brain tissue.[254]
Oral health
Several in vitro studies have investigated the potential effects of nicotine on a range of oral cells. A recent systematic review concluded that nicotine was unlikely to be cytotoxic to oral cells in vitro in most physiological conditions but further research is needed.[255] Understanding the potential role of nicotine in oral health has become increasingly important given the recent introduction of novel nicotine products and their potential role in helping smokers quit.[256]
See also
Bibliography
- McNeill, A; Brose, LS; Calder, R; Bauld, L; Robson, D (February 2018). "Evidence review of e-cigarettes and heated tobacco products 2018" (PDF). UK: Public Health England. pp. 1–243.
References
- ↑ "The Medicines (Products Other Than Veterinary Drugs) (General Sale List) Amendment Order 2001". legislation.gov.uk. 2001.
- ↑ "Nicotine". PubChem Compound Database. United States National Library of Medicine – National Center for Biotechnology Information. 7 May 2022.
- ↑ Bucklin, Matthew (January 2021). "A 5-Factor Framework for Assessing Tobacco Use Disorder". Tobacco Use Insights. 14: 1179173X2199835. doi:10.1177/1179173X21998355. PMC 7922618. PMID 33716514.
- ↑ 4.0 4.1 Cosci F, Pistelli F, Lazzarini N, Carrozzi L (September 2011). "Nicotine dependence and psychological distress: outcomes and clinical implications in smoking cessation". Psychology Research and Behavior Management. 4: 119–28. doi:10.2147/prbm.s14243. PMC 3218785. PMID 22114542.
- ↑ Hollinger MA (19 October 2007). Introduction to Pharmacology (Third ed.). Abingdon: CRC Press. pp. 222–223. ISBN 978-1-4200-4742-4.
- ↑ 6.0 6.1 6.2 6.3 Landoni JH. "Nicotine (PIM)". INCHEM. International Programme on Chemical Safety. Retrieved 29 January 2019.
- ↑ Abou-Donia M (5 February 2015). Mammalian Toxicology. John Wiley & Sons. pp. 587–. ISBN 978-1-118-68285-2.
- ↑ 8.0 8.1 8.2 Laszlo, Csaba; Kaminski, Kacper; Guan, Haifeng; Fatarova, Maria; Wei, Jianbing; Bergounioux, Alexandre; Schlage, Walter K.; Schorderet-Weber, Sandra; Guy, Philippe A.; Ivanov, Nikolai V.; Lamottke, Kai; Hoeng, Julia (21 November 2022). "Fractionation and Extraction Optimization of Potentially Valuable Compounds and Their Profiling in Six Varieties of Two Nicotiana Species". Molecules. 27 (22): 8105. doi:10.3390/molecules27228105.
- ↑ 9.0 9.1 9.2 Rehman, Muhammad Zia ur; Rizwan, Muhammad; Sohail, Muhammad Irfan; Ali, Shafaqat; Waris, Aisha A.; Khalid, Hinnan; Naeem, Asif; Ahmad, Hamaad Raza; Rauf, Arslan (June 2019). "Opportunities and challenges in the remediation of metal-contaminated soils by using tobacco (Nicotiana tabacum L.): a critical review". Environmental Science and Pollution Research. 26 (18): 18053–18070. doi:10.1007/s11356-019-05391-9.
- ↑ Funk D., P. Marinelli, and A. Le. (2006). "Biological Processes Underlying Co-use of Alcohol and Nicotine: Neuronal Mechanisms, Crosstolerance, and Genetic Factors". Alcohol Research and Health. 29 (3): 186–192. PMC 6527043. PMID 17373407.
{{cite journal}}: CS1 maint: uses authors parameter (link) - ↑ 11.0 11.1 Sajja RK, Rahman S, Cucullo L (March 2016). "Drugs of abuse and blood-brain barrier endothelial dysfunction: A focus on the role of oxidative stress". Journal of Cerebral Blood Flow and Metabolism. 36 (3): 539–54. doi:10.1177/0271678X15616978. PMC 4794105. PMID 26661236.
- ↑ Flatscher-Bader, Traute; Wilce, Peter A. (2009). "The effect of alcohol and nicotine abuse on gene expression in the brain". Nutrition Research Reviews. 22 (2): 148–162. doi:10.1017/S0954422409990114. ISSN 0954-4224. PMID 19900347.
- ↑ 13.00 13.01 13.02 13.03 13.04 13.05 13.06 13.07 13.08 13.09 13.10 Hartmann-Boyce J, Chepkin SC, Ye W, Bullen C, Lancaster T (May 2018). "Nicotine replacement therapy versus control for smoking cessation". The Cochrane Database of Systematic Reviews. 5: CD000146. doi:10.1002/14651858.CD000146.pub5. PMC 6353172. PMID 29852054.
There is high-quality evidence that all of the licensed forms of NRT (gum, transdermal patch, nasal spray, inhalator and sublingual tablets/lozenges) can help people who make a quit attempt to increase their chances of successfully stopping smoking. NRTs increase the rate of quitting by 50% to 60%, regardless of setting, and further research is very unlikely to change our confidence in the estimate of the effect. The relative effectiveness of NRT appears to be largely independent of the intensity of additional support provided to the individual.
A meta-analysis of adverse events associated with NRT included 92 RCTs and 28 observational studies, and addressed a possible excess of chest pains and heart palpitations among users of NRT compared with placebo groups (Mills 2010). The authors report an OR of 2.06 (95% CI 1.51 to 2.82) across 12 studies. We replicated this data collection exercise and analysis where data were available (included and excluded) in this review, and detected a similar but slightly lower estimate, OR 1.88 (95% CI 1.37 to 2.57; 15 studies; 11,074 participants; OR rather than RR calculated for comparison; Analysis 6.1). Chest pains and heart palpitations were an extremely rare event, occurring at a rate of 2.5% in the NRT groups compared with 1.4% in the control groups in the 15 trials in which they were reported at all. A recent network meta-analysis of cardiovascular events associated with smoking cessation pharmacotherapies (Mills 2014), including 21 RCTs comparing NRT with placebo, found statistically significant evidence that the rate of cardiovascular events with NRT was higher (RR 2.29 95% CI 1.39 to 3.82). However, when only serious adverse cardiac events (myocardial infarction, stroke and cardiovascular death) were considered, the finding was not statistically significant (RR 1.95 95% CI 0.26 to 4.30). - ↑ Picciotto, Marina R; Calarco, Cali A (2020). "Nicotinic Acetylcholine Receptor Signaling in the Hypothalamus: Mechanisms Related to Nicotine's Effects on Food Intake". Nicotine & Tobacco Research. 22 (2): 152–163. doi:10.1093/ntr/ntz010. ISSN 1462-2203. PMC 7297099. PMID 30690485.
- ↑ 15.0 15.1 15.2 "Nicotinic acetylcholine receptors: Introduction". IUPHAR Database. International Union of Basic and Clinical Pharmacology. Archived from the original on 29 June 2017. Retrieved 1 September 2014.
- ↑ "Smoking and Tobacco Control Monograph No. 9" (PDF). Archived (PDF) from the original on 9 October 2022. Retrieved 19 December 2012.
- ↑ 17.0 17.1 17.2 17.3 17.4 17.5 17.6 17.7 17.8 17.9 Siegmund, Barbara; Leitner, Erich; Pfannhauser, Werner (1 August 1999). "Determination of the Nicotine Content of Various Edible Nightshades (Solanaceae) and Their Products and Estimation of the Associated Dietary Nicotine Intake". Journal of Agricultural and Food Chemistry. 47 (8): 3113–3120. doi:10.1021/jf990089w. PMID 10552617.
- ↑ Rodgman A, Perfetti TA (2009). The chemical components of tobacco and tobacco smoke. Boca Raton, FL: CRC Press. ISBN 978-1-4200-7883-1. LCCN 2008018913.[page needed]
- ↑ 19.0 19.1 Ujváry I (1999). "Nicotine and Other Insecticidal Alkaloids". In Yamamoto I, Casida J (eds.). Nicotinoid Insecticides and the Nicotinic Acetylcholine Receptor. Tokyo: Springer-Verlag. pp. 29–69.
- ↑ 20.0 20.1 "Nicotine; Product Cancellation Order". Federal Register. Environmental Protection Agency. 3 June 2009.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ Terayama, H; Sakabe, K; Kiyoshima, D; Qu, N; Sato, T; Suyama, K; Hayashi, S; Sakurai, K; Todaka, E; Mori, C (30 September 2022). "Effect of Neonicotinoid Pesticides on Japanese Water Systems: Review with Focus on Reproductive Toxicity". International journal of molecular sciences. 23 (19). doi:10.3390/ijms231911567. PMID 36232869.
- ↑ 22.0 22.1 Voorhees, Jennifer P.; Phillips, Bryn M.; Anderson, Brian S.; Tjeerdema, Ron S.; Page, Barbara (2020). "Comparison of the Relative Efficacies of Granulated Activated Carbon and Biochar to Reduce Chlorpyrifos and Imidacloprid Loading and Toxicity Using Laboratory Bench Scale Experiments". Bulletin of Environmental Contamination and Toxicology. 104 (3): 327–332. doi:10.1007/s00128-020-02790-4. ISSN 0007-4861.
- ↑ 23.0 23.1 Butler, Declan (27 April 2018). "Scientists hail European ban on bee-harming pesticides". Nature. doi:10.1038/d41586-018-04987-4. ISSN 0028-0836.
- ↑ 24.0 24.1 Grana, Rachel; Benowitz, Neal; Glantz, Stanton A. (13 May 2014). "E-Cigarettes: A Scientific Review". Circulation. 129 (19): 1972–1986. doi:10.1161/circulationaha.114.007667. PMC 4018182. PMID 24821826.
- ↑ 25.0 25.1 25.2 Siqueira LM (January 2017). "Nicotine and Tobacco as Substances of Abuse in Children and Adolescents". Pediatrics. 139 (1): e20163436. doi:10.1542/peds.2016-3436. PMID 27994114.
- ↑ 26.0 26.1 26.2 Marcham, Cheryl L.; Springston, John P. (2019). "Electronic cigarettes in the indoor environment". Reviews on Environmental Health. 34 (2): 105–124. doi:10.1515/reveh-2019-0012. ISSN 2191-0308. PMID 31112510. S2CID 135122336.
- ↑ 27.0 27.1 27.2 Widysanto A, Combest FE, Dhakal A, Saadabadi A (10 November 2020). "Nicotine Addiction". StatPearls Publishing. PMID 29763090.
- ↑ 28.0 28.1 Mayer B (January 2014). "How much nicotine kills a human? Tracing back the generally accepted lethal dose to dubious self-experiments in the nineteenth century". Archives of Toxicology. 88 (1): 5–7. doi:10.1007/s00204-013-1127-0. PMC 3880486. PMID 24091634.
- ↑ Caponnetto P, Campagna D, Papale G, Russo C, Polosa R (February 2012). "The emerging phenomenon of electronic cigarettes". Expert Review of Respiratory Medicine. 6 (1): 63–74. doi:10.1586/ers.11.92. PMID 22283580. S2CID 207223131.
- ↑ Jain R, Mukherjee K, Balhara YP (April 2008). "The role of NMDA receptor antagonists in nicotine tolerance, sensitization, and physical dependence: a preclinical review". Yonsei Medical Journal. 49 (2): 175–88. doi:10.3349/ymj.2008.49.2.175. PMC 2615322. PMID 18452252.
- ↑ Miyasato, K. (March 2013). "[Psychiatric and psychological features of nicotine dependence]". Nihon Rinsho. Japanese Journal of Clinical Medicine (in 日本語). 71 (3): 477–481. PMID 23631239.
- ↑ 32.0 32.1 32.2 Parrott AC (July 2015). "Why all stimulant drugs are damaging to recreational users: an empirical overview and psychobiological explanation" (PDF). Human Psychopharmacology. 30 (4): 213–24. doi:10.1002/hup.2468. PMID 26216554. S2CID 7408200.
- ↑ Parrott AC (March 2006). "Nicotine psychobiology: how chronic-dose prospective studies can illuminate some of the theoretical issues from acute-dose research" (PDF). Psychopharmacology. 184 (3–4): 567–76. doi:10.1007/s00213-005-0294-y. PMID 16463194. S2CID 11356233.
- ↑ 34.0 34.1 D'Souza MS, Markou A (July 2011). "Neuronal mechanisms underlying development of nicotine dependence: implications for novel smoking-cessation treatments". Addiction Science & Clinical Practice. 6 (1): 4–16. PMC 3188825. PMID 22003417.
Withdrawal symptoms upon cessation of nicotine intake: Chronic nicotine use induces neuroadaptations in the brain's reward system that result in the development of nicotine dependence. Thus, nicotine-dependent smokers must continue nicotine intake to avoid distressing somatic and affective withdrawal symptoms. Newly abstinent smokers experience symptoms such as depressed mood, anxiety, irritability, difficulty concentrating, craving, bradycardia, insomnia, gastrointestinal discomfort, and weight gain (Shiffman and Jarvik, 1976; Hughes et al., 1991). Experimental animals, such as rats and mice, exhibit a nicotine withdrawal syndrome that, like the human syndrome, includes both somatic signs and a negative affective state (Watkins et al., 2000; Malin et al., 2006). The somatic signs of nicotine withdrawal include rearing, jumping, shakes, abdominal constrictions, chewing, scratching, and facial tremors. The negative affective state of nicotine withdrawal is characterized by decreased responsiveness to previously rewarding stimuli, a state called anhedonia.
- ↑ 35.0 35.1 35.2 35.3 35.4 35.5 35.6 Parrott AC (April 2003). "Cigarette-Derived Nicotine is not a Medicine" (PDF). The World Journal of Biological Psychiatry. 4 (2): 49–55. doi:10.3109/15622970309167951. ISSN 1562-2975. PMID 12692774. S2CID 26903942.
- ↑ 36.0 36.1 36.2 36.3 36.4 36.5 36.6 36.7 Chaturvedi, Pankaj; Mishra, Aseem; Datta, Sourav; Sinukumar, Snita; Joshi, Poonam; Garg, Apurva (2015). "Harmful effects of nicotine". Indian Journal of Medical and Paediatric Oncology. 36 (1): 24. doi:10.4103/0971-5851.151771. ISSN 0971-5851. PMC 4363846. PMID 25810571.
- ↑ 37.0 37.1 37.2 37.3 37.4 Mravec, Boris; Tibensky, Miroslav; Horvathova, Lubica; Babal, Pavel (2020). "E-Cigarettes and Cancer Risk". Cancer Prevention Research. 13 (2): 137–144. doi:10.1158/1940-6207.CAPR-19-0346. ISSN 1940-6207. PMID 31619443.
- ↑ Gilley, Meghan; Beno, Suzanne (June 2020). "Vaping implications for children and youth". Current Opinion in Pediatrics. 32 (3): 343–348. doi:10.1097/MOP.0000000000000889. ISSN 1040-8703. PMID 32332326.
- ↑ Dinardo, Perry; Rome, Ellen S. (2019). "Vaping: The new wave of nicotine addiction". Cleveland Clinic Journal of Medicine. 86 (12): 789–798. doi:10.3949/ccjm.86a.19118. ISSN 0891-1150. PMID 31821136.
- ↑ 40.0 40.1 40.2 Yuan, Menglu; Cross, Sarah J.; Loughlin, Sandra E.; Leslie, Frances M. (2015). "Nicotine and the adolescent brain". The Journal of Physiology. 593 (16): 3397–3412. doi:10.1113/JP270492. ISSN 0022-3751. PMC 4560573. PMID 26018031.
- ↑ Peterson, Lisa A.; Hecht, Stephen S. (2017). "Tobacco, e-cigarettes, and child health". Current Opinion in Pediatrics. 29 (2): 225–230. doi:10.1097/MOP.0000000000000456. ISSN 1040-8703. PMC 5598780. PMID 28059903.
- ↑ 42.0 42.1 "Quick Facts on the Risks of E-cigarettes for Kids, Teens, and Young Adults". Centers for Disease Control and Prevention. 7 July 2021.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ↑ 43.0 43.1 Strongin, Robert M. (12 June 2019). "E-Cigarette Chemistry and Analytical Detection". Annual review of analytical chemistry (Palo Alto, Calif.). Annual Reviews. 12 (1): 23–39. doi:10.1146/annurev-anchem-061318-115329. ISSN 1936-1327. PMC 6565477. PMID 30848928.
- ↑ 44.0 44.1 44.2 44.3 Merecz-Sadowska, Anna; Sitarek, Przemyslaw; Zielinska-Blizniewska, Hanna; Malinowska, Katarzyna; Zajdel, Karolina; Zakonnik, Lukasz; Zajdel, Radoslaw (19 January 2020). "A Summary of In Vitro and In Vivo Studies Evaluating the Impact of E-Cigarette Exposure on Living Organisms and the Environment". International Journal of Molecular Sciences. 21 (2): 652. doi:10.3390/ijms21020652. PMC 7013895. PMID 31963832.
 This article incorporates text by Anna Merecz-Sadowska, Przemyslaw Sitarek, Hanna Zielinska-Blizniewska, Katarzyna Malinowska, Karolina Zajdel, Lukasz Zakonnik, and Radoslaw Zajdel available under the CC BY 4.0 license.
This article incorporates text by Anna Merecz-Sadowska, Przemyslaw Sitarek, Hanna Zielinska-Blizniewska, Katarzyna Malinowska, Karolina Zajdel, Lukasz Zakonnik, and Radoslaw Zajdel available under the CC BY 4.0 license.
- ↑ 45.0 45.1 Znyk, Małgorzata; Jurewicz, Joanna; Kaleta, Dorota (21 June 2021). "Exposure to Heated Tobacco Products and Adverse Health Effects, a Systematic Review". International Journal of Environmental Research and Public Health. 18 (12): 6651. doi:10.3390/ijerph18126651. PMC 8296358. PMID 34205612.
- ↑ 46.0 46.1 Park, Jin-Ah; Crotty Alexander, Laura E.; Christiani, David C. (10 February 2022). "Vaping and Lung Inflammation and Injury". Annual Review of Physiology. 84 (1): 611–629. doi:10.1146/annurev-physiol-061121-040014. PMC 10228557. PMID 34724436.
{{cite journal}}: Check|pmc=value (help) - ↑ 47.0 47.1 47.2 Holbrook BD (June 2016). "The effects of nicotine on human fetal development". Birth Defects Research. Part C, Embryo Today. 108 (2): 181–92. doi:10.1002/bdrc.21128. PMID 27297020.
- ↑ 48.0 48.1 Kohlmeier KA (June 2015). "Nicotine during pregnancy: changes induced in neurotransmission, which could heighten proclivity to addict and induce maladaptive control of attention". Journal of Developmental Origins of Health and Disease. 6 (3): 169–81. doi:10.1017/S2040174414000531. PMID 25385318. S2CID 29298949.
- ↑ 49.0 49.1 "Nicotine". European Chemicals Agency: Committee for Risk Assessment. September 2015. Retrieved 23 January 2019.
- ↑ 50.0 50.1 50.2 50.3 50.4 50.5 Schraufnagel DE (March 2015). "Electronic Cigarettes: Vulnerability of Youth". Pediatric Allergy, Immunology, and Pulmonology. 28 (1): 2–6. doi:10.1089/ped.2015.0490. PMC 4359356. PMID 25830075.
- ↑ 51.0 51.1 51.2 51.3 National Center for Chronic Disease Prevention Health Promotion (US) Office on Smoking Health (2014). The Health Consequences of Smoking—50 Years of Progress: A Report of the Surgeon General, Chapter 5 - Nicotine. Surgeon General of the United States. pp. 107–138. PMID 24455788.
- ↑ Effah, Felix; Taiwo, Benjamin; Baines, Deborah; Bailey, Alexis; Marczylo, Tim (3 October 2022). "Pulmonary effects of e-liquid flavors: a systematic review". Journal of Toxicology and Environmental Health Part B: Critical Review. 25 (7): 343–371. doi:10.1080/10937404.2022.2124563.
- ↑ Lavoie FW, Harris TM (1991). "Fatal nicotine ingestion". The Journal of Emergency Medicine. 9 (3): 133–136. doi:10.1016/0736-4679(91)90318-a. PMID 2050970.
- ↑ 54.0 54.1 Theodoulou, Annika; Chepkin, Samantha C; Ye, Weiyu; Fanshawe, Thomas R; Bullen, Chris; Hartmann-Boyce, Jamie; Livingstone-Banks, Jonathan; Hajizadeh, Anisa; Lindson, Nicola (19 June 2023). "Different doses, durations and modes of delivery of nicotine replacement therapy for smoking cessation". Cochrane Database of Systematic Reviews. 2023 (6). doi:10.1002/14651858.CD013308.pub2. PMC 10278922. PMID 37335995.
{{cite journal}}: Check|pmc=value (help) - ↑ "The MIND Study - Why Nicotine?". MIND. 2024.
- ↑ Thiriez, Claire; Villafane, Gabriel; Grapin, Frédérique; Fenelon, Gilles; Remy, Philippe; Cesaro, Pierre (July 2011). "Can nicotine be used medicinally in Parkinson's disease?". Expert Review of Clinical Pharmacology. 4 (4): 429–436. doi:10.1586/ecp.11.27. PMID 22114853.
- ↑ 57.0 57.1 57.2 57.3 57.4 57.5 Lewis, Alan S.; Picciotto, Marina R. (2020). "Regulation of aggressive behaviors by nicotinic acetylcholine receptors: Animal models, human genetics, and clinical studies". Neuropharmacology. 167: 107929. doi:10.1016/j.neuropharm.2019.107929}. ISSN 0028-3908. PMC 7080580. PMID 32058178.
- ↑ Picciotto, Marina R.; Lewis, Alan S.; van Schalkwyk, Gerrit I.; Mineur, Yann S. (September 2015). "Mood and anxiety regulation by nicotinic acetylcholine receptors: A potential pathway to modulate aggression and related behavioral states". Neuropharmacology. 96: 235–243. doi:10.1016/j.neuropharm.2014.12.028. PMC 4486625. PMID 25582289.
- ↑ 59.0 59.1 59.2 Russo, Patrizia; Cardinale, Alessio; Margaritora, Stefano; Cesario, Alfredo (November 2012). "Nicotinic receptor and tobacco-related cancer". Life Sciences. 91 (21–22): 1087–1092. doi:10.1016/j.lfs.2012.05.003. PMID 22705232.
- ↑ Liu, Hai; Kotova, Tatyana I.; Timko, Michael P. (14 November 2019). "Increased Leaf Nicotine Content by Targeting Transcription Factor Gene Expression in Commercial Flue-Cured Tobacco (Nicotiana tabacum L.)". Genes. 10 (11): 930. doi:10.3390/genes10110930.
- ↑ 61.0 61.1 Tomizawa M, Casida JE (2005). "Neonicotinoid insecticide toxicology: mechanisms of selective action" (PDF). Annual Review of Pharmacology and Toxicology. 45: 247–68. doi:10.1146/annurev.pharmtox.45.120403.095930. PMID 15822177. Archived from the original (PDF) on 29 October 2018. Retrieved 29 October 2018.
- ↑ "Tobacco and its evil cousin nicotine are good as a pesticide – American Chemical Society". American Chemical Society. Retrieved 29 October 2018.
- ↑ USEPA (3 June 2009). "Nicotine; Product Cancellation Order". Federal Register: 26695–26696. Retrieved 8 April 2012.
- ↑ US Code of Federal Regulations.7 CFR 205.602 – Nonsynthetic substances prohibited for use in organic crop production
- ↑ Tharp C (5 September 2014). "Safety for Homemade Remedies for Pest Control" (PDF). Montana Pesticide Bulletin. Montana State University. Archived from the original (PDF) on 5 September 2014. Retrieved 21 September 2020.
- ↑ 66.0 66.1 Michalski B, Herrmann M, Solecki R (July 2017). "[How does a pesticide residue turn into a contaminant?]". Bundesgesundheitsblatt - Gesundheitsforschung - Gesundheitsschutz (in Deutsch). 60 (7): 768–773. doi:10.1007/s00103-017-2556-3. PMID 28508955. S2CID 22662492.
- ↑ European Food Safety Authority (7 May 2009). "Potential risks for public health due to the presence of nicotine in wild mushrooms". EFSA Journal. 7 (5): 286r. doi:10.2903/j.efsa.2009.286r.
- ↑ Abreu-Villaça Y, Levin ED (February 2017). "Developmental neurotoxicity of succeeding generations of insecticides". Environment International. 99: 55–77. doi:10.1016/j.envint.2016.11.019. PMC 5285268. PMID 27908457.
- ↑ Valentine G, Sofuoglu M (May 2018). "Cognitive Effects of Nicotine: Recent Progress". Current Neuropharmacology. Bentham Science Publishers. 16 (4): 403–414. doi:10.2174/1570159X15666171103152136. PMC 6018192. PMID 29110618.
- ↑ Heishman SJ, Kleykamp BA, Singleton EG (July 2010). "Meta-analysis of the acute effects of nicotine and smoking on human performance". Psychopharmacology. 210 (4): 453–69. doi:10.1007/s00213-010-1848-1. PMC 3151730. PMID 20414766.
- ↑ Sarter M (August 2015). "Behavioral-Cognitive Targets for Cholinergic Enhancement". Current Opinion in Behavioral Sciences. 4: 22–26. doi:10.1016/j.cobeha.2015.01.004. PMC 5466806. PMID 28607947.
- ↑ "Nicotine: Biological activity". IUPHAR/BPS Guide to Pharmacology. International Union of Basic and Clinical Pharmacology. Retrieved 7 February 2016.
Kis as follows; α2β4=9900nM [5], α3β2=14nM [1], α3β4=187nM [1], α4β2=1nM [4,6]. Due to the heterogeneity of nACh channels we have not tagged a primary drug target for nicotine, although the α4β2 is reported to be the predominant high affinity subtype in the brain which mediates nicotine addiction
- ↑ Majdi A, Kamari F, Vafaee MS, Sadigh-Eteghad S (October 2017). "Revisiting nicotine's role in the ageing brain and cognitive impairment" (PDF). Reviews in the Neurosciences. 28 (7): 767–781. doi:10.1515/revneuro-2017-0008. PMID 28586306. S2CID 3758298. Archived from the original (PDF) on 5 August 2020. Retrieved 25 May 2020.
- ↑ Uban, Kristina A.; Horton, Megan K.; Jacobus, Joanna; Heyser, Charles; Thompson, Wesley K.; Tapert, Susan F.; Madden, Pamela A.F.; Sowell, Elizabeth R. (August 2018). "Biospecimens and the ABCD study: Rationale, methods of collection, measurement and early data". Developmental Cognitive Neuroscience. 32: 97–106. doi:10.1016/j.dcn.2018.03.005. PMC 6487488. PMID 29606560.
- ↑ 75.0 75.1 Stolerman IP, Jarvis MJ (January 1995). "The scientific case that nicotine is addictive". Psychopharmacology. 117 (1): 2–10, discussion 14–20. doi:10.1007/BF02245088. PMID 7724697. S2CID 8731555.
- ↑ Wilder N, Daley C, Sugarman J, Partridge J (April 2016). "Nicotine without smoke: Tobacco harm reduction". UK: Royal College of Physicians. pp. 58, 125.
- ↑ 77.0 77.1 77.2 El Sayed KA, Sylvester PW (June 2007). "Biocatalytic and semisynthetic studies of the anticancer tobacco cembranoids". Expert Opinion on Investigational Drugs. 16 (6): 877–87. doi:10.1517/13543784.16.6.877. PMID 17501699. S2CID 21302112.
- ↑ Rahman MA, Hann N, Wilson A, Worrall-Carter L (2014). "Electronic cigarettes: patterns of use, health effects, use in smoking cessation and regulatory issues". Tobacco Induced Diseases. 12 (1): 21. doi:10.1186/1617-9625-12-21. PMC 4350653. PMID 25745382.
- ↑ Speciale, Zachary; Rao, Sanjana; Yang, Shengping; Nugent, Kenneth (January 2023). "An Analysis of Nicotine Pouch Use by Middle School and High School Students Surveyed by the National Youth Tobacco Survey in 2021 and a Review of the Literature". Journal of Primary Care & Community Health. 14: 215013192311699. doi:10.1177/21501319231169994. PMC 10159243. PMID 37128171.
{{cite journal}}: Check|pmc=value (help) - ↑ Lachenmeier, Dirk W.; Breaux, Theodore A.; Kuballa, Thomas; Schlee, Claudia; Monakhova, Yulia B. (September 2014). "Composition of distilled Perique tobacco liqueur: A connoisseur's spirit or a health risk due to nicotine?". Food Chemistry. 159: 230–235. doi:10.1016/j.foodchem.2014.02.152. PMID 24767049.
- ↑ "2003: The 3rd Annual Year In Ideas; Nicotini, The". The New York Times Magazine. 14 December 2003. Archived from the original on 27 May 2015.
- ↑ Little MA, Ebbert JO (2016). "The safety of treatments for tobacco use disorder". Expert Opinion on Drug Safety. 15 (3): 333–41. doi:10.1517/14740338.2016.1131817. PMID 26715118. S2CID 12064318.
- ↑ Aubin HJ, Luquiens A, Berlin I (February 2014). "Pharmacotherapy for smoking cessation: pharmacological principles and clinical practice". British Journal of Clinical Pharmacology. 77 (2): 324–36. doi:10.1111/bcp.12116. PMC 4014023. PMID 23488726.
- ↑ 84.0 84.1 84.2 84.3 Bailey SR, Crew EE, Riske EC, Ammerman S, Robinson TN, Killen JD (April 2012). "Efficacy and tolerability of pharmacotherapies to aid smoking cessation in adolescents". Paediatric Drugs. 14 (2): 91–108. doi:10.2165/11594370-000000000-00000. PMC 3319092. PMID 22248234.
- ↑ "Electronic Cigarettes – What are the health effects of using e-cigarettes?" (PDF). Centers for Disease Control and Prevention. 22 February 2018. Archived (PDF) from the original on 9 October 2022.
Nicotine is a health danger for pregnant women and their developing babies.
- ↑ Bruin JE, Gerstein HC, Holloway AC (August 2010). "Long-term consequences of fetal and neonatal nicotine exposure: a critical review". Toxicological Sciences. 116 (2): 364–74. doi:10.1093/toxsci/kfq103. PMC 2905398. PMID 20363831.
there is no safe dose of nicotine during pregnancy... The general consensus among clinicians is that more information is needed about the risks of NRT use during pregnancy before well-informed definitive recommendations can be made to pregnant women... Overall, the evidence provided in this review overwhelmingly indicates that nicotine should no longer be considered the safe component of cigarette smoke. In fact, many of the adverse postnatal health outcomes associated with maternal smoking during pregnancy may be attributable, at least in part, to nicotine alone.
- ↑ 87.0 87.1 87.2 Forest S (1 March 2010). "Controversy and evidence about nicotine replacement therapy in pregnancy". MCN: The American Journal of Maternal/Child Nursing. 35 (2): 89–95. doi:10.1097/NMC.0b013e3181cafba4. PMID 20215949. S2CID 27085986.
- ↑ 88.0 88.1 88.2 88.3 88.4 88.5 Sanner, Tore; Grimsrud, Tom K. (31 August 2015). "Nicotine: Carcinogenicity and Effects on Response to Cancer Treatment – A Review". Frontiers in Oncology. 5: 196. doi:10.3389/fonc.2015.00196. ISSN 2234-943X. PMC 4553893. PMID 26380225.
 This article incorporates text by Tore Sanner, and Tom K. Grimsrud available under the CC BY 4.0 license.
This article incorporates text by Tore Sanner, and Tom K. Grimsrud available under the CC BY 4.0 license.
- ↑ 89.00 89.01 89.02 89.03 89.04 89.05 89.06 89.07 89.08 89.09 89.10 89.11 89.12 89.13 "Nicotine". Drugs.com. American Society of Health-System Pharmacists. Retrieved 24 January 2019.
- ↑ Detailed reference list is located at a separate image page.
- ↑ 91.0 91.1 91.2 91.3 Jensen, Kendal; Nizamutdinov, Damir; Guerrier, Micheleine; Afroze, Syeda; Dostal, David; Glaser, Shannon (December 2012). "General mechanisms of nicotine‐induced fibrogenesis". The FASEB Journal. 26 (12): 4778–4787. doi:10.1096/fj.12-206458. PMC 3509054. PMID 22906950.
- ↑ "Electronic nicotine delivery systems" (PDF). World Health Organization. 21 July 2014. p. 10.
- ↑ 93.0 93.1 93.2 93.3 England, Lucinda J.; Bunnell, Rebecca E.; Pechacek, Terry F.; Tong, Van T.; McAfee, Tim A. (August 2015). "Nicotine and the Developing Human". American Journal of Preventive Medicine. 49 (2): 286–93. doi:10.1016/j.amepre.2015.01.015. ISSN 0749-3797. PMC 4594223. PMID 25794473.
- ↑ 94.0 94.1 Hartmann-Boyce, Jamie; Chepkin, Samantha C; Ye, Weiyu; Bullen, Chris; Lancaster, Tim (31 May 2018). "Nicotine replacement therapy versus control for smoking cessation". Cochrane Database of Systematic Reviews. 5: Appendix 3. doi:10.1002/14651858.CD000146.pub5. PMC 6353172. PMID 29852054.
- ↑ 95.0 95.1 Li, Zong-Zhuang; Dai, Qiu-Yan (2012). "Pathogenesis of Abdominal Aortic Aneurysms: Role of Nicotine and Nicotinic Acetylcholine Receptors". Mediators of Inflammation. 2012: 1–8. doi:10.1155/2012/103120. PMC 3317239. PMID 22529515.
 This article incorporates text by Zong-Zhuang Li and Qiu-Yan Dai available under the CC BY 3.0 license.
This article incorporates text by Zong-Zhuang Li and Qiu-Yan Dai available under the CC BY 3.0 license.
- ↑ "Nicotine Transdermal Patch" (PDF). United States Food and Drug Administration. Retrieved 24 January 2019.
- ↑ 97.0 97.1 "Nicotrol NS" (PDF). United States Food and Drug Administration. Retrieved 24 January 2019.
- ↑ "Nicotrol" (PDF). Pfizer. Retrieved 24 January 2019.
- ↑ 99.0 99.1 Garcia AN, Salloum IM (October 2015). "Polysomnographic sleep disturbances in nicotine, caffeine, alcohol, cocaine, opioid, and cannabis use: A focused review". The American Journal on Addictions. 24 (7): 590–8. doi:10.1111/ajad.12291. PMID 26346395. S2CID 22703103.
- ↑ Boutrel B, Koob GF (September 2004). "What keeps us awake: the neuropharmacology of stimulants and wakefulness-promoting medications". Sleep. 27 (6): 1181–94. doi:10.1093/sleep/27.6.1181. PMID 15532213.
- ↑ Jaehne A, Loessl B, Bárkai Z, Riemann D, Hornyak M (October 2009). "Effects of nicotine on sleep during consumption, withdrawal and replacement therapy". Sleep Medicine Reviews (Review). 13 (5): 363–77. doi:10.1016/j.smrv.2008.12.003. PMID 19345124.
- ↑ 102.0 102.1 102.2 102.3 La Rosa, Giusy; Vernooij, Robin; Qureshi, Maria; Polosa, Riccardo; O’Leary, Renée (April 2023). "Clinical testing of the cardiovascular effects of e-cigarette substitution for smoking: a living systematic review". Internal and Emergency Medicine. 18 (3): 917–928. doi:10.1007/s11739-022-03161-z. PMC 10081981. PMID 36609804.
{{cite journal}}: Check|pmc=value (help) This article incorporates text by Giusy La Rosa, Robin Vernooij, Maria Qureshi, Riccardo Polosa, and Renée O’Leary available under the CC BY 4.0 license.
This article incorporates text by Giusy La Rosa, Robin Vernooij, Maria Qureshi, Riccardo Polosa, and Renée O’Leary available under the CC BY 4.0 license.
- ↑ 103.0 103.1 "Cardiac adverse effects of nicotine replacement therapy". Prescrire international. 24 (166): 292–3. December 2015. PMID 26788573.
- ↑ Tarran, Robert; Barr, R Graham; Benowitz, Neal L; Bhatnagar, Aruni; Chu, Hong W; Dalton, Pamela; Doerschuk, Claire M; Drummond, M Bradley; Gold, Diane R; Goniewicz, Maciej L; Gross, Eric R; Hansel, Nadia N; Hopke, Philip K; Kloner, Robert A; Mikheev, Vladimir B; Neczypor, Evan W; Pinkerton, Kent E; Postow, Lisa; Rahman, Irfan; Samet, Jonathan M; Salathe, Matthias; Stoney, Catherine M; Tsao, Philip S; Widome, Rachel; Xia, Tian; Xiao, DaLiao; Wold, Loren E (2021). "E-Cigarettes and Cardiopulmonary Health". Function. 2 (2). doi:10.1093/function/zqab004. ISSN 2633-8823. PMC 7948134. PMID 33748758.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ↑ 105.0 105.1 105.2 105.3 105.4 105.5 Benowitz, Neal L.; Burbank, Andrea D. (2016). "Cardiovascular toxicity of nicotine: Implications for electronic cigarette use". Trends in Cardiovascular Medicine. 26 (6): 515–23. doi:10.1016/j.tcm.2016.03.001. ISSN 1050-1738. PMC 4958544. PMID 27079891.
- ↑ Jerry JM, Collins GB, Streem D (2015). "E-cigarettes: Safe to recommend to patients?". Cleve Clin J Med. 82 (8): 521–6. doi:10.3949/ccjm.82a.14054. PMID 26270431.
- ↑ Benowitz, Neal L.; Fraiman, Joseph B. (2017). "Cardiovascular effects of electronic cigarettes". Nature Reviews Cardiology. 14 (8): 447–456. doi:10.1038/nrcardio.2017.36. ISSN 1759-5002. PMC 5519136. PMID 28332500.
- ↑ Hanna, ST (March 2006). "Nicotine effect on cardiovascular system and ion channels". Journal of cardiovascular pharmacology. 47 (3): 348–58. doi:10.1097/01.fjc.0000205984.13395.9e. PMID 16633075.
- ↑ 109.0 109.1 109.2 109.3 Centner, Ann Marie; Bhide, Pradeep G.; Salazar, Gloria (2020). "Nicotine in Senescence and Atherosclerosis". Cells. 9 (4): 1035. doi:10.3390/cells9041035. ISSN 2073-4409. PMC 7226537. PMID 32331221.
 This article incorporates text by Ann Marie Centner, Pradeep G. Bhide, and Gloria Salazar available under the CC BY 4.0 license.
This article incorporates text by Ann Marie Centner, Pradeep G. Bhide, and Gloria Salazar available under the CC BY 4.0 license.
- ↑ 110.0 110.1 110.2 110.3 Emma, Rosalia; Caruso, Massimo; Campagna, Davide; Pulvirenti, Roberta; Li Volti, Giovanni (September 2022). "The Impact of Tobacco Cigarettes, Vaping Products and Tobacco Heating Products on Oxidative Stress". Antioxidants. 11 (9): 1829. doi:10.3390/antiox11091829.
 This article incorporates text by Rosalia Emma, Massimo Caruso, Davide Campagna, Roberta Pulvirenti, and Giovanni Li Volti available under the CC BY 4.0 license.
This article incorporates text by Rosalia Emma, Massimo Caruso, Davide Campagna, Roberta Pulvirenti, and Giovanni Li Volti available under the CC BY 4.0 license.
- ↑ 111.00 111.01 111.02 111.03 111.04 111.05 111.06 111.07 111.08 111.09 111.10 111.11 111.12 111.13 111.14 111.15 111.16 111.17 111.18 111.19 111.20 Pimentel, Emely; Sivalingam, Kalaiselvi; Doke, Mayur; Samikkannu, Thangavel (21 May 2020). "Effects of Drugs of Abuse on the Blood-Brain Barrier: A Brief Overview". Frontiers in Neuroscience. 14. doi:10.3389/fnins.2020.00513. PMC 7326150. PMID 32670001.
 This article incorporates text by Emely Pimentel, Kalaiselvi Sivalingam, Mayur Doke, and Thangavel Samikkannu available under the CC BY 4.0 license.
This article incorporates text by Emely Pimentel, Kalaiselvi Sivalingam, Mayur Doke, and Thangavel Samikkannu available under the CC BY 4.0 license.
- ↑ Nestler EJ, Barrot M, Self DW (September 2001). "DeltaFosB: a sustained molecular switch for addiction". Proceedings of the National Academy of Sciences of the United States of America. 98 (20): 11042–6. Bibcode:2001PNAS...9811042N. doi:10.1073/pnas.191352698. PMC 58680. PMID 11572966.
Although the ΔFosB signal is relatively long-lived, it is not permanent. ΔFosB degrades gradually and can no longer be detected in brain after 1–2 months of drug withdrawal ... Indeed, ΔFosB is the longest-lived adaptation known to occur in adult brain, not only in response to drugs of abuse, but to any other perturbation (that doesn't involve lesions) as well.
- ↑ Nestler EJ (December 2012). "Transcriptional mechanisms of drug addiction". Clinical Psychopharmacology and Neuroscience. 10 (3): 136–43. doi:10.9758/cpn.2012.10.3.136. PMC 3569166. PMID 23430970.
The 35–37 kD ΔFosB isoforms accumulate with chronic drug exposure due to their extraordinarily long half-lives. ... As a result of its stability, the ΔFosB protein persists in neurons for at least several weeks after cessation of drug exposure. ... ΔFosB overexpression in nucleus accumbens induces NFκB
- ↑ McNeill 2018, p. 54.
- ↑ 115.0 115.1 Walley, Susan C.; Wilson, Karen M.; Winickoff, Jonathan P.; Groner, Judith (2019). "A Public Health Crisis: Electronic Cigarettes, Vape, and JUUL". Pediatrics. 143 (6): e20182741. doi:10.1542/peds.2018-2741. ISSN 0031-4005. PMID 31122947.
- ↑ 116.0 116.1 McNeill 2018, p. 12, 62.
- ↑ McNeill 2018, p. 13, 62.
- ↑ MacDonald, K; Pappa, K (April 2016). "WHY NOT POT?: A Review of the Brain-based Risks of Cannabis". Innov Clin Neurosci. 13 (3–4): 13–22. PMC 4911936. PMID 27354924.
- ↑ Hayes, John E.; Baker, Allison N. (27 July 2022). "Flavor science in the context of research on electronic cigarettes". Frontiers in Neuroscience. 16. doi:10.3389/fnins.2022.918082. PMC 9365686. PMID 35968379.
 This article incorporates text by John E Hayes and Allison N Baker available under the CC BY 4.0 license.
This article incorporates text by John E Hayes and Allison N Baker available under the CC BY 4.0 license.
- ↑ 120.0 120.1 Kanithi, Manasa; Junapudi, Sunil; Shah, Syed Islamuddin; Matta Reddy, Alavala; Ullah, Ghanim; Chidipi, Bojjibabu (19 May 2022). "Alterations of Mitochondrial Network by Cigarette Smoking and E-Cigarette Vaping". Cells. 11 (10): 1688. doi:10.3390/cells11101688. PMC 9139349. PMID 35626724.
 This article incorporates text by Manasa Kanithi, Sunil Junapudi, Syed Islamuddin Shah, Alavala Matta Reddy, Ghanim Ullah,3 and Bojjibabu Chidipi available under the CC BY 4.0 license.
This article incorporates text by Manasa Kanithi, Sunil Junapudi, Syed Islamuddin Shah, Alavala Matta Reddy, Ghanim Ullah,3 and Bojjibabu Chidipi available under the CC BY 4.0 license.
- ↑ Das S, Prochaska JJ (October 2017). "Innovative approaches to support smoking cessation for individuals with mental illness and co-occurring substance use disorders". Expert Review of Respiratory Medicine. 11 (10): 841–850. doi:10.1080/17476348.2017.1361823. PMC 5790168. PMID 28756728.
- ↑ Heishman SJ, Kleykamp BA, Singleton EG (July 2010). "Meta-analysis of the acute effects of nicotine and smoking on human performance". Psychopharmacology. 210 (4): 453–69. doi:10.1007/s00213-010-1848-1. PMC 3151730. PMID 20414766.
The significant effects of nicotine on motor abilities, attention, and memory likely represent true performance enhancement because they are not confounded by withdrawal relief. The beneficial cognitive effects of nicotine have implications for initiation of smoking and maintenance of tobacco dependence.
- ↑ Baraona LK, Lovelace D, Daniels JL, McDaniel L (May 2017). "Tobacco Harms, Nicotine Pharmacology, and Pharmacologic Tobacco Cessation Interventions for Women". Journal of Midwifery & Women's Health. 62 (3): 253–269. doi:10.1111/jmwh.12616. PMID 28556464. S2CID 1267977.
- ↑ Dugas, En; Sylvestre, Mp; O'Loughlin, Ek; Brunet, J; Kakinami, L; Constantin, E; O'Loughlin, J (February 2017). "Nicotine dependence and sleep quality in young adults". Addictive Behaviors. 65: 154–160. doi:10.1016/j.addbeh.2016.10.020. PMID 27816041.
- ↑ Cohrs, Stefan; Rodenbeck, Andrea; Riemann, Dieter; Szagun, Bertram; Jaehne, Andreas; Brinkmeyer, Jürgen; Gründer, Gerhard; Wienker, Thomas; Diaz‐Lacava, Amalia; Mobascher, Arian; Dahmen, Norbert; Thuerauf, Norbert; Kornhuber, Johannes; Kiefer, Falk; Gallinat, Jürgen; Wagner, Michael; Kunz, Dieter; Grittner, Ulrike; Winterer, Georg (May 2014). "Impaired sleep quality and sleep duration in smokers-results from the German Multicenter Study on Nicotine Dependence". Addiction Biology. 19 (3): 486–96. doi:10.1111/j.1369-1600.2012.00487.x. hdl:11858/00-001M-0000-0025-BD0C-B. PMID 22913370. S2CID 1066283.
- ↑ Bruijnzeel AW (May 2012). "Tobacco addiction and the dysregulation of brain stress systems". Neuroscience and Biobehavioral Reviews. 36 (5): 1418–41. doi:10.1016/j.neubiorev.2012.02.015. PMC 3340450. PMID 22405889.
Discontinuation of smoking leads to negative affective symptoms such as depressed mood, increased anxiety, and impaired memory and attention...Smoking cessation leads to a relatively mild somatic withdrawal syndrome and a severe affective withdrawal syndrome that is characterized by a decrease in positive affect, an increase in negative affect, craving for tobacco, irritability, anxiety, difficulty concentrating, hyperphagia, restlessness, and a disruption of sleep. Smoking during the acute withdrawal phase reduces craving for cigarettes and returns cognitive abilities to pre-smoking cessation level
- ↑ 127.0 127.1 Nestler EJ (December 2013). "Cellular basis of memory for addiction". Dialogues in Clinical Neuroscience. 15 (4): 431–43. doi:10.31887/DCNS.2013.15.4/enestler. PMC 3898681. PMID 24459410.
- ↑ 128.0 128.1 Ruffle JK (November 2014). "Molecular neurobiology of addiction: what's all the (Δ)FosB about?". The American Journal of Drug and Alcohol Abuse. 40 (6): 428–37. doi:10.3109/00952990.2014.933840. PMID 25083822. S2CID 19157711.
The knowledge of ΔFosB induction in chronic drug exposure provides a novel method for the evaluation of substance addiction profiles (i.e. how addictive they are). Xiong et al. used this premise to evaluate the potential addictive profile of propofol (119). Propofol is a general anaesthetic, however its abuse for recreational purpose has been documented (120). Using control drugs implicated in both ΔFosB induction and addiction (ethanol and nicotine), ...
Conclusions
ΔFosB is an essential transcription factor implicated in the molecular and behavioral pathways of addiction following repeated drug exposure. The formation of ΔFosB in multiple brain regions, and the molecular pathway leading to the formation of AP-1 complexes is well understood. The establishment of a functional purpose for ΔFosB has allowed further determination as to some of the key aspects of its molecular cascades, involving effectors such as GluR2 (87,88), Cdk5 (93) and NFkB (100). Moreover, many of these molecular changes identified are now directly linked to the structural, physiological and behavioral changes observed following chronic drug exposure (60,95,97,102). New frontiers of research investigating the molecular roles of ΔFosB have been opened by epigenetic studies, and recent advances have illustrated the role of ΔFosB acting on DNA and histones, truly as a molecular switch (34). As a consequence of our improved understanding of ΔFosB in addiction, it is possible to evaluate the addictive potential of current medications (119), as well as use it as a biomarker for assessing the efficacy of therapeutic interventions (121,122,124). - ↑ Marttila K, Raattamaa H, Ahtee L (July 2006). "Effects of chronic nicotine administration and its withdrawal on striatal FosB/DeltaFosB and c-Fos expression in rats and mice". Neuropharmacology. 51 (1): 44–51. doi:10.1016/j.neuropharm.2006.02.014. PMID 16631212. S2CID 8551216.
- ↑ 130.00 130.01 130.02 130.03 130.04 130.05 130.06 130.07 130.08 130.09 130.10 130.11 130.12 130.13 130.14 130.15 130.16 130.17 130.18 130.19 130.20 Zhao, Yue (2016). "The Oncogenic Functions of Nicotinic Acetylcholine Receptors". Journal of Oncology. 2016: 1–9. doi:10.1155/2016/9650481. PMC 4769750. PMID 26981122.
 This article incorporates text by Yue Zhao available under the CC BY 4.0 license.
This article incorporates text by Yue Zhao available under the CC BY 4.0 license.
- ↑ Grando, Sergei A. (June 2014). "Connections of nicotine to cancer". Nature Reviews Cancer. 14 (6): 419–429. doi:10.1038/nrc3725. PMID 24827506.
- ↑ Dasgupta P (January 2009). "Nicotine induces cell proliferation, invasion and epithelial-mesenchymal transition in a variety of human cancer cell lines". International Journal of Cancer. The Journal of Clinical Endocrinology & Metabolism. 124 (1): 36–45. doi:10.1002/ijc.23894. PMC 2826200. PMID 18844224.
- ↑ Kothari AN, Mi Z, Zapf M, Kuo PC (2014). "Novel clinical therapeutics targeting the epithelial to mesenchymal transition". Clinical and Translational Medicine. 3: 35. doi:10.1186/s40169-014-0035-0. PMC 4198571. PMID 25343018.
- ↑ Taylor, Eve; Simonavičius, Erikas; McNeill, Ann; Brose, Leonie S; East, Katherine; Marczylo, Tim; Robson, Debbie (22 February 2024). "Exposure to Tobacco-Specific Nitrosamines Among People Who Vape, Smoke, or do Neither: A Systematic Review and Meta-Analysis". Nicotine and Tobacco Research. 26 (3): 257–269. doi:10.1093/ntr/ntad156. PMC 10882431. PMID 37619211.
{{cite journal}}: Check|pmc=value (help) This article incorporates text by Eve Taylor, Erikas Simonavičius, Ann McNeill, Leonie S Brose, Katherine East, Tim Marczylo, and Debbie Robson available under the CC BY 4.0 license.
This article incorporates text by Eve Taylor, Erikas Simonavičius, Ann McNeill, Leonie S Brose, Katherine East, Tim Marczylo, and Debbie Robson available under the CC BY 4.0 license.
- ↑ Knezevich A, Muzic J, Hatsukami DK, Hecht SS, Stepanov I (February 2013). "Nornicotine nitrosation in saliva and its relation to endogenous synthesis of N'-nitrosonornicotine in humans". Nicotine & Tobacco Research. 15 (2): 591–5. doi:10.1093/ntr/nts172. PMC 3611998. PMID 22923602.
- ↑ Birkett, Nicholas; Al-Zoughool, Mustafa; Bird, Michael; Baan, Robert A.; Zielinski, Jan; Krewski, Daniel (17 November 2019). "Overview of biological mechanisms of human carcinogens". Journal of Toxicology and Environmental Health, Part B. 22 (7–8): 288–359. doi:10.1080/10937404.2019.164353. PMID 31631808.
- ↑ 137.0 137.1 137.2 Bracken-Clarke, Dara; Kapoor, Dhruv; Baird, Anne Marie; Buchanan, Paul James; Gately, Kathy; Cuffe, Sinead; Finn, Stephen P. (2021). "Vaping and lung cancer – A review of current data and recommendations". Lung Cancer. 153: 11–20. doi:10.1016/j.lungcan.2020.12.030. ISSN 0169-5002. PMID 33429159.
- ↑ Schaal, Courtney; Chellappan, Srikumar P. (16 January 2014). "Nicotine-Mediated Cell Proliferation and Tumor Progression in Smoking-Related Cancers". Molecular Cancer Research. 12 (1): 14–23. doi:10.1158/1541-7786.MCR-13-0541. PMC 3915512. PMID 24398389.
- ↑ 139.0 139.1 Pucci, Susanna; Zoli, Michele; Clementi, Francesco; Gotti, Cecilia (21 January 2022). "α9-Containing Nicotinic Receptors in Cancer". Frontiers in Cellular Neuroscience. 15: 805123. doi:10.3389/fncel.2021.805123.
 This article incorporates text by Susanna Pucci, Michele Zoli, Francesco Clementi, and Cecilia Gotti available under the CC BY 4.0 license.
This article incorporates text by Susanna Pucci, Michele Zoli, Francesco Clementi, and Cecilia Gotti available under the CC BY 4.0 license.
- ↑ Hu, Zhiwei; Brooks, Samira A.; Dormoy, Valérian; Hsu, Chia-Wen; Hsu, Hsue-Yin; Lin, Liang-Tzung; Massfelder, Thierry; Rathmell, W.Kimryn; Xia, Menghang; Al-Mulla, Fahd; Al-Temaimi, Rabeah; Amedei, Amedeo; Brown, Dustin G.; Prudhomme, Kalan R.; Colacci, Anna Maria; Hamid, Roslida A.; Mondello, Chiara; Raju, Jayadev; Ryan, Elizabeth P.; Woodrick, Jordan; Scovassi, A.Ivana; Singh, Neetu; Vaccari, Monica; Roy, Rabindra; Forte, Stefano; Memeo, Lorenzo; Salem, Hosni K.; Lowe, Leroy; Jensen, Lasse; Bisson, William H.; Kleinstreuer, Nicole (June 2015). "Assessing the carcinogenic potential of low-dose exposures to chemical mixtures in the environment: focus on the cancer hallmark of tumor angiogenesis". Carcinogenesis. 36 (Suppl 1): S184–S202. doi:10.1093/carcin/bgv036. PMC 4492067. PMID 26106137.
- ↑ Cooke, John P.; Ghebremariam, Yohannes T. (October 2008). "Endothelial Nicotinic Acetylcholine Receptors and Angiogenesis". Trends in Cardiovascular Medicine. 18 (7): 247–253. doi:10.1016/j.tcm.2008.11.007. PMC 2673464. PMID 19232953.
- ↑ 142.0 142.1 142.2 142.3 142.4 Shalabi, Sharif; Belayachi, Ali; Larrivée, Bruno (5 February 2024). "Involvement of neuronal factors in tumor angiogenesis and the shaping of the cancer microenvironment". Frontiers in Immunology. 15. doi:10.3389/fimmu.2024.1284629. PMC 10875004. PMID 38375479.
{{cite journal}}: Check|pmc=value (help) This article incorporates text by Sharif Shalabi, Ali Belayachi, and Bruno Larrivée available under the CC BY 4.0 license.
This article incorporates text by Sharif Shalabi, Ali Belayachi, and Bruno Larrivée available under the CC BY 4.0 license.
- ↑ Iftikhar, Anem; Islam, Mohammad; Shepherd, Simon; Jones, Sarah; Ellis, Ian (6 January 2021). "Cancer and Stress: Does It Make a Difference to the Patient When These Two Challenges Collide?". Cancers. 13 (2): 163. doi:10.3390/cancers13020163. PMC 7825104. PMID 33418900.
 This article incorporates text by Anem Iftikhar, Mohammad Islam, Simon Shepherd, Sarah Jones, and Ian Ellis available under the CC BY 4.0 license.
This article incorporates text by Anem Iftikhar, Mohammad Islam, Simon Shepherd, Sarah Jones, and Ian Ellis available under the CC BY 4.0 license.
- ↑ 144.0 144.1 144.2 144.3 144.4 144.5 Kuol, Nyanbol; Stojanovska, Lily; Apostolopoulos, Vasso; Nurgali, Kulmira (December 2018). "Role of the nervous system in cancer metastasis". Journal of Experimental & Clinical Cancer Research. 37 (1). doi:10.1186/s13046-018-0674-x. PMC 5769535. PMID 29334991.
 This article incorporates text by Nyanbol Kuol, Lily Stojanovska, Vasso Apostolopoulos,, and Kulmira Nurgali available under the CC BY 4.0 license.
This article incorporates text by Nyanbol Kuol, Lily Stojanovska, Vasso Apostolopoulos,, and Kulmira Nurgali available under the CC BY 4.0 license.
- ↑ 145.0 145.1 145.2 145.3 Moccia, Francesco (11 January 2018). "Endothelial Ca2+ Signaling and the Resistance to Anticancer Treatments: Partners in Crime". International Journal of Molecular Sciences. 19 (1): 217. doi:10.3390/ijms19010217. PMC 5796166. PMID 29324706.
 This article incorporates text by Francesco Moccia available under the CC BY 4.0 license.
This article incorporates text by Francesco Moccia available under the CC BY 4.0 license.
- ↑ Ginzkey, Christian; Steussloff, Gudrun; Koehler, Christian; Burghartz, Marc; Scherzed, Agmal; Hackenberg, Stephan; Hagen, Rudolf; Kleinsasser, Norbert H. (2014). "Nicotine derived genotoxic effects in human primary parotid gland cells as assessed in vitro by comet assay, cytokinesis-block micronucleus test and chromosome aberrations test". Toxicology in vitro : an international journal published in association with BIBRA. Elsevier BV. 28 (5): 838–846. doi:10.1016/j.tiv.2014.03.012. ISSN 0887-2333. PMID 24698733.
- ↑ Ginzkey, Christian; Friehs, Gudrun; Koehler, Christian; Hackenberg, Stephan; Hagen, Rudolf; Kleinsasser, Norbert H. (18 February 2013). "Assessment of nicotine-induced DNA damage in a genotoxicological test battery". Mutation research. Elsevier BV. 751 (1): 34–39. doi:10.1016/j.mrgentox.2012.11.004. ISSN 1383-5718. PMID 23200805.
- ↑ Ginzkey, Christian; Stueber, Thomas; Friehs, Gudrun; Koehler, Christian; Hackenberg, Stephan; Richter, Elmar; Hagen, Rudolf; Kleinsasser, Norbert H. (5 January 2012). "Analysis of nicotine-induced DNA damage in cells of the human respiratory tract". Toxicology letters. Elsevier BV. 208 (1): 23–29. doi:10.1016/j.toxlet.2011.09.029. ISSN 0378-4274. PMID 22001448.
- ↑ "Electronic Cigarettes (E-cigarettes)". National Institute on Drug Abuse. March 2018.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ↑ Kumar, P.S.; Clark, P.; Brinkman, M.C.; Saxena, D. (2019). "Novel Nicotine Delivery Systems". Advances in Dental Research. 30 (1): 11–15. doi:10.1177/0022034519872475. ISSN 0895-9374. PMID 31538804.
- ↑ 151.0 151.1 151.2 Virgili, Fabrizio; Nenna, Raffaella; Ben David, Shira; Mancino, Enrica; Di Mattia, Greta; Matera, Luigi; Petrarca, Laura; Midulla, Fabio (December 2022). "E-cigarettes and youth: an unresolved Public Health concern". Italian Journal of Pediatrics. 48 (1): 97. doi:10.1186/s13052-022-01286-7. PMC 9194784. PMID 35701844.
 This article incorporates text by Fabrizio Virgili, Raffaella Nenna, Shira Ben David, Enrica Mancino, Greta Di Mattia, Luigi Matera, Laura Petrarca, and Fabio Midulla available under the CC BY 4.0 license.
This article incorporates text by Fabrizio Virgili, Raffaella Nenna, Shira Ben David, Enrica Mancino, Greta Di Mattia, Luigi Matera, Laura Petrarca, and Fabio Midulla available under the CC BY 4.0 license.
- ↑ 152.0 152.1 152.2 152.3 152.4 152.5 152.6 152.7 "Nicotine". United States National Library of Medicine – Toxicology Data Network. Hazardous Substances Data Bank. 20 August 2009.
- ↑ Behnke M, Smith VC (March 2013). "Prenatal substance abuse: short- and long-term effects on the exposed fetus". Pediatrics. 131 (3): e1009-24. doi:10.1542/peds.2012-3931. PMC 8194464. PMID 23439891.
- ↑ 154.0 154.1 "State Health Officer's Report on E-Cigarettes: A Community Health Threat" (PDF). California Department of Public Health. January 2015.
- ↑ Schraufnagel, Dean E.; Blasi, Francesco; Drummond, M. Bradley; Lam, David C. L.; Latif, Ehsan; Rosen, Mark J.; Sansores, Raul; Van Zyl-Smit, Richard (September 2014). "Electronic Cigarettes. A Position Statement of the Forum of International Respiratory Societies". American Journal of Respiratory and Critical Care Medicine. 190 (6): 611–618. doi:10.1164/rccm.201407-1198PP. ISSN 1073-449X. PMID 25006874. S2CID 43763340.
- ↑ Chatkin, José Miguel; Dullius, Cynthia Rocha (2016). "The management of asthmatic smokers". Asthma Research and Practice. 2 (1): 10. doi:10.1186/s40733-016-0025-7. ISSN 2054-7064. PMC 5142412. PMID 27965778.
 This article incorporates text available under the CC BY 4.0 license.
This article incorporates text available under the CC BY 4.0 license.
- ↑ Buck, Jordan M; Yu, Li; Knopik, Valerie S; Stitzel, Jerry A (14 September 2021). "DNA methylome perturbations: an epigenetic basis for the emergingly heritable neurodevelopmental abnormalities associated with maternal smoking and maternal nicotine exposure". Biology of Reproduction. 105 (3): 644–666. doi:10.1093/biolre/ioab138. PMC 8444709. PMID 34270696.
- ↑ "Tobacco Use". Centers for Disease Control and Prevention. 10 November 2022.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ↑ Barnes, Deborah E. (20 May 1998). "Why Review Articles on the Health Effects of Passive Smoking Reach Different Conclusions". JAMA. 279 (19): 1566. doi:10.1001/jama.279.19.1566. PMID 9605902.
- ↑ Schwartz, Ann G.; Cote, Michele L. (2016). "Epidemiology of Lung Cancer". Lung Cancer and Personalized Medicine. 893: 21–41. doi:10.1007/978-3-319-24223-1_2. PMID 26667337.
- ↑ Bhatt, Jayesh Mahendra; Ramphul, Manisha; Bush, Andrew (2020). "An update on controversies in e-cigarettes". Paediatric Respiratory Reviews. 36: 75–86. doi:10.1016/j.prrv.2020.09.003. ISSN 1526-0542. PMC 7518964. PMID 33071065.
- ↑ McGrath-Morrow, Sharon A.; Gorzkowski, Julie; Groner, Judith A.; Rule, Ana M.; Wilson, Karen; Tanski, Susanne E.; Collaco, Joseph M.; Klein, Jonathan D. (1 March 2020). "The Effects of Nicotine on Development". Pediatrics. 145 (3): e20191346. doi:10.1542/peds.2019-1346. PMC 7049940. PMID 32047098.
- ↑ Espinoza-Derout, Jorge; Shao, Xuesi M.; Lao, Candice J.; Hasan, Kamrul M.; Rivera, Juan Carlos; Jordan, Maria C.; Echeverria, Valentina; Roos, Kenneth P.; Sinha-Hikim, Amiya P.; Friedman, Theodore C. (7 April 2022). "Electronic Cigarette Use and the Risk of Cardiovascular Diseases". Frontiers in Cardiovascular Medicine. 9: 879726. doi:10.3389/fcvm.2022.879726. PMC 9021536. PMID 35463745.
 This article incorporates text by Jorge Espinoza-Derout, Xuesi M. Shao, Candice J. Lao, Kamrul M. Hasan, Juan Carlos Rivera, Maria C. Jordan, Valentina Echeverria, Kenneth P. Roos, Amiya P. Sinha-Hikim, and Theodore C. Friedman available under the CC BY 3.0 license.
This article incorporates text by Jorge Espinoza-Derout, Xuesi M. Shao, Candice J. Lao, Kamrul M. Hasan, Juan Carlos Rivera, Maria C. Jordan, Valentina Echeverria, Kenneth P. Roos, Amiya P. Sinha-Hikim, and Theodore C. Friedman available under the CC BY 3.0 license.
- ↑ 164.0 164.1 Szukalska, Marta; Szyfter, Krzysztof; Florek, Ewa; Rodrigo, Juan P.; Rinaldo, Alessandra; Mäkitie, Antti A.; Strojan, Primož; Takes, Robert P.; Suárez, Carlos; Saba, Nabil F.; Braakhuis, Boudewijn J.M.; Ferlito, Alfio (5 November 2020). "Electronic Cigarettes and Head and Neck Cancer Risk—Current State of Art". Cancers. 12 (11): 3274. doi:10.3390/cancers12113274.
 This article incorporates text by Marta Szukalska, Krzysztof Szyfter, Ewa Florek, Juan P. Rodrigo, Alessandra Rinaldo, Antti A. Mäkitie, Primož Strojan, Robert P. Takes, Carlos Suárez, Nabil F. Saba, Boudewijn J.M. Braakhuis, and Alfio Ferlito available under the CC BY 4.0 license.
This article incorporates text by Marta Szukalska, Krzysztof Szyfter, Ewa Florek, Juan P. Rodrigo, Alessandra Rinaldo, Antti A. Mäkitie, Primož Strojan, Robert P. Takes, Carlos Suárez, Nabil F. Saba, Boudewijn J.M. Braakhuis, and Alfio Ferlito available under the CC BY 4.0 license.
- ↑ 165.0 165.1 165.2 165.3 165.4 165.5 165.6 Drope, J; Chapman, S (1 August 2001). "Tobacco industry efforts at discrediting scientific knowledge of environmental tobacco smoke: a review of internal industry documents". Journal of Epidemiology & Community Health. 55 (8): 588–594. doi:10.1136/jech.55.8.588. PMC 1731959. PMID 11449018.
- ↑ "Consumer Updates: Nicotine Replacement Therapy Labels May Change". FDA. 1 April 2013.
- ↑ Toxicology and Applied Pharmacology. Vol. 44, Pg. 1, 1978.
- ↑ {{cite journal|last1=Quail|first1=M. Thomas|title=Nicotine toxicity|journal=Nursing|volume=50|issue=1|year=2020|pages=44–48|issn=0360-4039|doi=10.1097/01.NURSE.0000615084.47597.14}|pmid=31855987}
- ↑ 169.0 169.1 169.2 169.3 169.4 169.5 Aoki, Yayoi; Ikeda, Tomoya; Tani, Naoto; Shida, Alissa; Oritani, Shigeki; Ishikawa, Takaki (January 2020). "Evaluation of the distribution of nicotine intravenous injection: an adult autopsy case report with a review of literature". International Journal of Legal Medicine. 134 (1): 243–249. doi:10.1007/s00414-019-02035-y. PMC 6949309. PMID 30955048.
 This article incorporates text by Yayoi Aoki, Tomoya Ikeda, Naoto Tani, Alissa Shida, Shigeki Oritani, and Takaki Ishikawa available under the CC BY 4.0 license.
This article incorporates text by Yayoi Aoki, Tomoya Ikeda, Naoto Tani, Alissa Shida, Shigeki Oritani, and Takaki Ishikawa available under the CC BY 4.0 license.
- ↑ 170.0 170.1 Schep LJ, Slaughter RJ, Beasley DM (September 2009). "Nicotinic plant poisoning". Clinical Toxicology. 47 (8): 771–81. doi:10.1080/15563650903252186. PMID 19778187. S2CID 28312730.
- ↑ Smolinske SC, Spoerke DG, Spiller SK, Wruk KM, Kulig K, Rumack BH (January 1988). "Cigarette and nicotine chewing gum toxicity in children". Human Toxicology. 7 (1): 27–31. doi:10.1177/096032718800700105. PMID 3346035. S2CID 27707333.
- ↑ Furer V, Hersch M, Silvetzki N, Breuer GS, Zevin S (March 2011). "Nicotiana glauca (tree tobacco) intoxication--two cases in one family". Journal of Medical Toxicology. 7 (1): 47–51. doi:10.1007/s13181-010-0102-x. PMC 3614112. PMID 20652661.
- ↑ Gehlbach SH, Williams WA, Perry LD, Woodall JS (September 1974). "Green-tobacco sickness. An illness of tobacco harvesters". JAMA. 229 (14): 1880–3. doi:10.1001/jama.1974.03230520022024. PMID 4479133.
- ↑ "CDC – NIOSH Pocket Guide to Chemical Hazards – Nicotine". Centers for Disease Control and Prevention. 30 October 2019.
- ↑ Malenka RC, Nestler EJ, Hyman SE (2009). "Chapter 9: Autonomic Nervous System". In Sydor A, Brown RY (eds.). Molecular Neuropharmacology: A Foundation for Clinical Neuroscience (2nd ed.). New York: McGraw-Hill Medical. p. 234. ISBN =978-0-07-148127-4.
Nicotine ... is a natural alkaloid of the tobacco plant. Lobeline is a natural alkaloid of Indian tobacco. Both drugs are agonists are nicotinic cholinergic receptors ...
{{cite book}}: Check|isbn=value: invalid character (help)CS1 maint: extra punctuation (link) - ↑ Pomerleau OF, Pomerleau CS (1984). "Neuroregulators and the reinforcement of smoking: towards a biobehavioral explanation". Neuroscience and Biobehavioral Reviews. 8 (4): 503–13. doi:10.1016/0149-7634(84)90007-1. PMID 6151160. S2CID 23847303.
- ↑ Pomerleau OF, Rosecrans J (1989). "Neuroregulatory effects of nicotine". Psychoneuroendocrinology. 14 (6): 407–23. doi:10.1016/0306-4530(89)90040-1. hdl:2027.42/28190. PMID 2560221. S2CID 12080532.
- ↑ Katzung BG (2006). Basic and Clinical Pharmacology. New York: McGraw-Hill Medical. pp. 99–105.
- ↑ Xiu X, Puskar NL, Shanata JA, Lester HA, Dougherty DA (March 2009). "Nicotine binding to brain receptors requires a strong cation-pi interaction". Nature. 458 (7237): 534–7. Bibcode:2009Natur.458..534X. doi:10.1038/nature07768. PMC 2755585. PMID 19252481.
- ↑ Nesbitt P (1969). Smoking, physiological arousal, and emotional response. Unpublished doctoral dissertation, Columbia University.
- ↑ Parrott AC (January 1998). "Nesbitt's Paradox resolved? Stress and arousal modulation during cigarette smoking" (PDF). Addiction. 93 (1): 27–39. CiteSeerX 10.1.1.465.2496. doi:10.1046/j.1360-0443.1998.931274.x. PMID 9624709.
- ↑ Wadgave U, Nagesh L (July 2016). "Nicotine Replacement Therapy: An Overview". International Journal of Health Sciences. 10 (3): 425–35. doi:10.12816/0048737. PMC 5003586. PMID 27610066.
- ↑ Grizzell JA, Echeverria V (October 2015). "New Insights into the Mechanisms of Action of Cotinine and its Distinctive Effects from Nicotine". Neurochemical Research. 40 (10): 2032–46. doi:10.1007/s11064-014-1359-2. PMID 24970109. S2CID 9393548.
- ↑ 184.0 184.1 184.2 184.3 Malenka RC, Nestler EJ, Hyman SE (2009). Sydor A, Brown RY (eds.). Molecular Neuropharmacology: A Foundation for Clinical Neuroscience (2nd ed.). New York: McGraw-Hill Medical. pp. 369, 372–373. ISBN 978-0-07-148127-4.
- ↑ 185.0 185.1 Dickson SL, Egecioglu E, Landgren S, Skibicka KP, Engel JA, Jerlhag E (June 2011). "The role of the central ghrelin system in reward from food and chemical drugs" (PDF). Molecular and Cellular Endocrinology. 340 (1): 80–7. doi:10.1016/j.mce.2011.02.017. hdl:2077/26318. PMID 21354264. S2CID 206815322. Archived from the original (PDF) on 4 August 2020. Retrieved 23 September 2019.
This reward link comprises a dopamine projection from the ventral tegmental area (VTA) to the nucleus accumbens together with a cholinergic input, arising primarily from the laterodorsal tegmental area.
- ↑ 186.0 186.1 186.2 Picciotto MR, Mineur YS (January 2014). "Molecules and circuits involved in nicotine addiction: The many faces of smoking". Neuropharmacology (Review). 76 Pt B: 545–53. doi:10.1016/j.neuropharm.2013.04.028. PMC 3772953. PMID 23632083.
Rat studies have shown that nicotine administration can decrease food intake and body weight, with greater effects in female animals (Grunberg et al., 1987). A similar nicotine regimen also decreases body weight and fat mass in mice as a result of β4* nAChR-mediated activation of POMC neurons and subsequent activation of MC4 receptors on second order neurons in the paraventricular nucleus of the hypothalamus (Mineur et al., 2011).
- ↑ Levine, Amir; Huang, YanYou; Drisaldi, Bettina; Griffin, Edmund A.; Pollak, Daniela D.; Xu, Shiqin; Yin, Deqi; Schaffran, Christine; Kandel, Denise B.; Kandel, Eric R. (November 2011). "Molecular mechanism for a gateway drug: epigenetic changes initiated by nicotine prime gene expression by cocaine". Science Translational Medicine. 3 (107): 107ra109. doi:10.1126/scitranslmed.3003062. PMC 4042673. PMID 22049069.
- ↑ Volkow, Nora D. (November 2011). "Epigenetics of nicotine: another nail in the coughing". Science Translational Medicine. 3 (107): 107ps43. doi:10.1126/scitranslmed.3003278. PMC 3492949. PMID 22049068.
- ↑ Yoshida T, Sakane N, Umekawa T, Kondo M (January 1994). "Effect of nicotine on sympathetic nervous system activity of mice subjected to immobilization stress". Physiology & Behavior. 55 (1): 53–7. doi:10.1016/0031-9384(94)90009-4. PMID 8140174. S2CID 37754794.
- ↑ Marieb EN, Hoehn K (2007). Human Anatomy & Physiology (7th Ed.). Pearson. pp. ?. ISBN 978-0-8053-5909-1.[page needed]
- ↑ Henningfield JE, Calvento E, Pogun S (2009). Nicotine Psychopharmacology. Springer. pp. 35, 37. ISBN 978-3-540-69248-5.
- ↑ Le Houezec J (September 2003). "Role of nicotine pharmacokinetics in nicotine addiction and nicotine replacement therapy: a review". The International Journal of Tuberculosis and Lung Disease. 7 (9): 811–9. PMID 12971663.
- ↑ Benowitz NL, Jacob P, Jones RT, Rosenberg J (May 1982). "Interindividual variability in the metabolism and cardiovascular effects of nicotine in man". The Journal of Pharmacology and Experimental Therapeutics. 221 (2): 368–72. PMID 7077531.
- ↑ Russell MA, Jarvis M, Iyer R, Feyerabend C. Relation of nicotine yield of cigarettes to blood nicotine concentrations in smokers. Br Med J. 5 April 1980; 280(6219): 972–976.
- ↑ Bhalala O (Spring 2003). "Detection of Cotinine in Blood Plasma by HPLC MS/MS". MIT Undergraduate Research Journal. 8: 45–50. Archived from the original on 24 December 2013.
- ↑ Hukkanen J, Jacob P, Benowitz NL (March 2005). "Metabolism and disposition kinetics of nicotine". Pharmacological Reviews. 57 (1): 79–115. doi:10.1124/pr.57.1.3. PMID 15734728. S2CID 14374018.
- ↑ Petrick LM, Svidovsky A, Dubowski Y (January 2011). "Thirdhand smoke: heterogeneous oxidation of nicotine and secondary aerosol formation in the indoor environment". Environmental Science & Technology. 45 (1): 328–33. Bibcode:2011EnST...45..328P. doi:10.1021/es102060v. PMID 21141815. S2CID 206939025.
- ↑ "The danger of third-hand smoke: Plain language summary – Petrick et al., "Thirdhand smoke: heterogeneous oxidation of nicotine and secondary aerosol formation in the indoor environment" in Environmental Science & Technology". The Column. Vol. 7, no. 3. Chromatography Online. 22 February 2011.
- ↑ Benowitz NL, Herrera B, Jacob P (September 2004). "Mentholated cigarette smoking inhibits nicotine metabolism". The Journal of Pharmacology and Experimental Therapeutics. 310 (3): 1208–15. doi:10.1124/jpet.104.066902. PMID 15084646. S2CID 16044557.
- ↑ 200.0 200.1 200.2 200.3 Hu T, Yang Z, Li MD (December 2018). "Pharmacological Effects and Regulatory Mechanisms of Tobacco Smoking Effects on Food Intake and Weight Control". Journal of Neuroimmune Pharmacology. 13 (4): 453–466. doi:10.1007/s11481-018-9800-y. PMID 30054897. S2CID 51727199.
Nicotine's weight effects appear to result especially from the drug's stimulation of α3β4 nicotine acetylcholine receptors (nAChRs), which are located on pro-opiomelanocortin (POMC) neurons in the arcuate nucleus (ARC), leading to activation of the melanocortin circuit, which is associated with body weight. Further, α7- and α4β2-containing nAChRs have been implicated in weight control by nicotine.
- ↑ Seoane-Collazo, Patricia; Diéguez, Carlos; Nogueiras, Rubén; Rahmouni, Kamal; Fernández-Real, José Manuel; López, Miguel (March 2021). "Nicotine' actions on energy balance: Friend or foe?". Pharmacology & Therapeutics. 219: 107693. doi:10.1016/j.pharmthera.2020.107693. PMID 32987056.
- ↑ 202.0 202.1 202.2 Metcalf RL (2007), "Insect Control", Ullmann's Encyclopedia of Industrial Chemistry (7th ed.), Wiley, p. 9
- ↑ "L-Nicotine Material Safety Data Sheet". Sciencelab.com, Inc.
- ↑ 204.0 204.1 204.2 Henry TA (1949). The Plant Alkaloids (PDF) (4th ed.). Philadelphia, Toronto: The Blakiston Company. pp. 36–43.
- ↑ Gause GF (1941). "Chapter V: Analysis of various biological processes by the study of the differential action of optical isomers". In Luyet, B. J. (ed.). Optical Activity and Living Matter. A series of monographs on general physiology. Vol. 2. Normandy, Missouri: Biodynamica.
- ↑ 206.0 206.1 Zhang, Hongfei; Pang, Yongqiang; Luo, Yanbo; Li, Xiangyu; Chen, Huan; Han, Shulei; Jiang, Xingyi; Zhu, Fengpeng; Hou, Hongwei; Hu, Qingyuan (3 May 2018). "Enantiomeric composition of nicotine in tobacco leaf, cigarette, smokeless tobacco, and e-liquid by normal phase high-performance liquid chromatography". Chirality. 30 (7): 923–931. doi:10.1002/chir.22866. ISSN 0899-0042. PMID 29722457.
- ↑ Hellinghausen, Garrett; Lee, Jauh T.; Weatherly, Choyce A.; Lopez, Diego A.; Armstrong, Daniel W. (June 2017). "Evaluation of nicotine in tobacco-free-nicotine commercial products: Nicotine enantiomers in tobacco free nicotine". Drug Testing and Analysis. 9 (6): 944–948. doi:10.1002/dta.2145.
- ↑ Jenssen, Brian; Boykan, Rachel (February 2019). "Electronic Cigarettes and Youth in the United States: A Call to Action (at the Local, National and Global Levels)". Children. 6 (2): 30. doi:10.3390/children6020030. PMC 6406299. PMID 30791645.
 This article incorporates text by Brian P. Jenssen and Rachel Boykan available under the CC BY 4.0 license.
This article incorporates text by Brian P. Jenssen and Rachel Boykan available under the CC BY 4.0 license.
- ↑ "Tobacco (leaf tobacco)". Transportation Information Service.
- ↑ Baldwin, I. T. 2001. An Ecologically Motivated Analysis of Plant-Herbivore Interactions in Native Tobacco. Plant Physiology 127:1449–1458. American Society of Plant Biologists.
- ↑ N.d. Natural history-driven, plant-mediated RNAi-based study reveals CYP6B46's role in a nicotine-mediated antipredator herbivore defense | PNAS.
- ↑ Kessler, D., S. Bhattacharya, C. Diezel, E. Rothe, K. Gase, M. Schöttner, and I. T. Baldwin. 2012. Unpredictability of nectar nicotine promotes outcrossing by hummingbirds in Nicotiana attenuata. The Plant Journal 71:529–538.
- ↑ Domino EF, Hornbach E, Demana T (August 1993). "The nicotine content of common vegetables". The New England Journal of Medicine. 329 (6): 437. doi:10.1056/NEJM199308053290619. PMID 8326992.
- ↑ Mourino, Nerea; Ruano-Raviña, Alberto; Varela Lema, Leonor; Fernández, Esteve; López, María José; Santiago-Pérez, María Isolina; Rey-Brandariz, Julia; Giraldo-Osorio, Alexandra; Pérez-Ríos, Mónica (5 May 2022). "Serum cotinine cut-points for secondhand smoke exposure assessment in children under 5 years: A systemic review". PLOS ONE. 17 (5): e0267319. doi:10.1371/journal.pone.0267319. PMC 9070924. PMID 35511766.
 This article incorporates text by Nerea Mourino, Alberto Ruano-Raviña, Leonor Varela Lema, Esteve Fernández, María José López, María Isolina Santiago-Pérez, Julia Rey-Brandariz, Alexandra Giraldo-Osorio, and Mónica Pérez-Ríos available under the CC BY 4.0 license.
This article incorporates text by Nerea Mourino, Alberto Ruano-Raviña, Leonor Varela Lema, Esteve Fernández, María José López, María Isolina Santiago-Pérez, Julia Rey-Brandariz, Alexandra Giraldo-Osorio, and Mónica Pérez-Ríos available under the CC BY 4.0 license.
- ↑ Moldoveanu, Serban C.; Scott, Wayne A.; Lawson, Darlene M. (1 April 2016). "Nicotine Analysis in Several Non-Tobacco Plant Materials". Beiträge zur Tabakforschung International/Contributions to Tobacco Research. 27 (2): 54–59. doi:10.1515/cttr-2016-0008. ISSN 1612-9237.
- ↑ 216.0 216.1 216.2 Pictet A, Rotschy A (1904). "Synthese des Nicotins" [Synthesis of nicotine]. Berichte der Deutschen Chemischen Gesellschaft (in Deutsch). 37 (2): 1225–1235. doi:10.1002/cber.19040370206.
- ↑ Ho, Tse-Lok; Kuzakov, Eugene?V. (2004). "A New Approach to Nicotine: Symmetry Consideration for Synthesis Design". Helvetica Chimica Acta. 87 (10): 2712–2716. doi:10.1002/hlca.200490241.
- ↑ Ye, Xiaoping; Zhang, Yanxin; Song, Xiaoping; Liu, Qingchao (2022). "Research Progress in the Pharmacological Effects and Synthesis of Nicotine". ChemistrySelect. 7 (12). doi:10.1002/slct.202104425. S2CID 247687372.
- ↑ Lamberts BL, Dewey LJ, Byerrum RU (May 1959). "Ornithine as a precursor for the pyrrolidine ring of nicotine". Biochimica et Biophysica Acta. 33 (1): 22–6. doi:10.1016/0006-3002(59)90492-5. PMID 13651178.
- ↑ Dawson RF, Christman DR, d'Adamo A, Solt ML, Wolf AP (1960). "The Biosynthesis of Nicotine from Isotopically Labeled Nicotinic Acids". Journal of the American Chemical Society. 82 (10): 2628–2633. doi:10.1021/ja01495a059.
- ↑ Ashihara H, Crozier A, Komamine A, eds. (7 June 2011). Plant metabolism and biotechnology. Cambridge: Wiley. ISBN 978-0-470-74703-2.[page needed]
- ↑ Benowitz NL, Hukkanen J, Jacob P (1 January 2009). "Nicotine Chemistry, Metabolism, Kinetics and Biomarkers". Nicotine Psychopharmacology. Handbook of Experimental Pharmacology. Vol. 192. pp. 29–60. doi:10.1007/978-3-540-69248-5_2. ISBN 978-3-540-69246-1. PMC 2953858. PMID 19184645.
- ↑ Baselt RC (2014). Disposition of Toxic Drugs and Chemicals in Man (10th ed.). Biomedical Publications. pp. 1452–6. ISBN 978-0-9626523-9-4.
- ↑ Mündel T, Jones DA (July 2006). "Effect of transdermal nicotine administration on exercise endurance in men". Experimental Physiology. 91 (4): 705–13. doi:10.1113/expphysiol.2006.033373. PMID 16627574. S2CID 41954065.
- ↑ Hellinghausen G, Roy D, Wang Y, Lee JT, Lopez DA, Weatherly CA, Armstrong DW (May 2018). "A comprehensive methodology for the chiral separation of 40 tobacco alkaloids and their carcinogenic E/Z-(R,S)-tobacco-specific nitrosamine metabolites". Talanta. 181: 132–141. doi:10.1016/j.talanta.2017.12.060. PMID 29426492.
- ↑ Liu B, Chen Y, Ma X, Hu K (September 2019). "Site-specific peak intensity ratio (SPIR) from 1D 2H/1H NMR spectra for rapid distinction between natural and synthetic nicotine and detection of possible adulteration". Analytical and Bioanalytical Chemistry. 411 (24): 6427–6434. doi:10.1007/s00216-019-02023-6. PMID 31321470. S2CID 197593505.
- ↑ Cheetham AG, Plunkett S, Campbell P, Hilldrup J, Coffa BG, Gilliland S, Eckard S (14 April 2022). Greenlief CM (ed.). "Analysis and differentiation of tobacco-derived and synthetic nicotine products: Addressing an urgent regulatory issue". PLOS ONE. 17 (4): e0267049. Bibcode:2022PLoSO..1767049C. doi:10.1371/journal.pone.0267049. PMC 9009602. PMID 35421170.
- ↑ Henningfield JE, Zeller M (March 2006). "Nicotine psychopharmacology research contributions to United States and global tobacco regulation: a look back and a look forward". Psychopharmacology. 184 (3–4): 286–91. doi:10.1007/s00213-006-0308-4. PMID 16463054. S2CID 38290573.
- ↑ Posselt W, Reimann L (1828). "Chemische Untersuchung des Tabaks und Darstellung eines eigenthümlich wirksamen Prinzips dieser Pflanze" [Chemical investigation of tobacco and preparation of a characteristically active constituent of this plant]. Magazin für Pharmacie (in Deutsch). 6 (24): 138–161.
- ↑ Melsens L (1843). "Note sur la nicotine" [Note on nicotine]. Annales de Chimie et de Physique. third series (in français). 9: 465–479, see especially page 470. [Note: The empirical formula that Melsens provides is incorrect because at that time, chemists used the wrong atomic mass for carbon (6 instead of 12).]
- ↑ Pinner A, Wolffenstein R (1891). "Ueber Nicotin" [About nicotine]. Berichte der Deutschen Chemischen Gesellschaft (in Deutsch). 24: 1373–1377. doi:10.1002/cber.189102401242.
- ↑ Pinner A (1893). "Ueber Nicotin. Die Constitution des Alkaloïds" [About nicotine: The Constitution of the Alkaloids]. Berichte der Deutschen Chemischen Gesellschaft (in Deutsch). 26: 292–305. doi:10.1002/cber.18930260165.
- ↑ Pinner A (1893). "Ueber Nicotin. I. Mitteilung". Archiv der Pharmazie. 231 (5–6): 378–448. doi:10.1002/ardp.18932310508. S2CID 83703998.
- ↑ Zhang, Sarah. "E-Cigs Are Going Tobacco-Free With Synthetic Nicotine". Wired. ISSN 1059-1028. Retrieved 11 October 2022.
- ↑ 235.0 235.1 Dale MM, Ritter JM, Fowler RJ, Rang HP. Rang & Dale's Pharmacology (6th ed.). Churchill Livingstone. p. 598. ISBN 978-0-8089-2354-1.
- ↑ Sanchez-Ramos, Juan R. (2020). "The rise and fall of tobacco as a botanical medicine". Journal of Herbal Medicine. 22: 100374. doi:10.1016/j.hermed.2020.100374. ISSN 2210-8033.
- ↑ Connolly, G. N; Alpert, H. R; Wayne, G. F.; Koh, H. (October 2007). "Trends in nicotine yield in smoke and its relationship with design characteristics among popular US cigarette brands, 1997-2005". Tobacco Control. 16 (5): e5. doi:10.1136/tc.2006.019695. PMC 2598548. PMID 17897974.
- ↑ "Industry Documents Library". www.industrydocuments.ucsf.edu. Retrieved 11 October 2022.
- ↑ Jewett, Christina (8 March 2022). "The Loophole That's Fueling a Return to Teenage Vaping". The New York Times. ISSN 0362-4331. Retrieved 11 October 2022.
- ↑ Jewett, Christina (8 March 2022). "The Loophole That's Fueling a Return to Teenage Vaping". The New York Times. ISSN 0362-4331. Retrieved 11 October 2022.
- ↑ Jordt, Sven-Eric (7 September 2021). "Synthetic nicotine has arrived". Tobacco Control: tobaccocontrol–2021–056626. doi:10.1136/tobaccocontrol-2021-056626. ISSN 0964-4563. PMC 8898991. PMID 34493630.
- ↑ Bhalerao A, Sivandzade F, Archie SR, Cucullo L (August 2019). "Public Health Policies on E-Cigarettes". Current Cardiology Reports. 21 (10): 111. doi:10.1007/s11886-019-1204-y. PMC 6713696. PMID 31463564.
- ↑ "Tobacco 21". United States Food and Drug Administration. 1 September 2021.
- ↑ Bonner, Emily; Chang, Yvonne; Christie, Emerson; Colvin, Victoria; Cunningham, Brittany; Elson, Daniel; Ghetu, Christine; Huizenga, Juliana; Hutton, Sara J.; Kolluri, Siva K.; Maggio, Stephanie; Moran, Ian; Parker, Bethany; Rericha, Yvonne; Rivera, Brianna N.; Samon, Samantha; Schwichtenberg, Trever; Shankar, Prarthana; Simonich, Michael T.; Wilson, Lindsay B.; Tanguay, Robyn L. (September 2021). "The chemistry and toxicology of vaping". Pharmacology & Therapeutics. 225: 107837. doi:10.1016/j.pharmthera.2021.107837. ISSN 0163-7258. PMC 8263470. PMID 33753133.
- ↑ "21, 18, or 14: A look at the legal age for smoking around the world". Straits Times. 3 October 2017. Retrieved 1 March 2019.
- ↑ "The Tobacco Products and Nicotine Inhaling Products (Amendment) (EU Exit) Regulations 2020". legislation.gov.uk.
{{cite web}}: CS1 maint: url-status (link) - ↑ 247.0 247.1 247.2 Jacob, Micheal (1 March 1985). "Superman versus Nick O'Teen — a children's anti-smoking campaign". Health Education Journal. 44 (1): 15–18. doi:10.1177/001789698504400104. S2CID 71246970.
- ↑ Becker, Rachel (26 April 2019). "Why Big Tobacco and Big Vape love comparing nicotine to caffeine". The Verge.
- ↑ Mineur YS, Picciotto MR (December 2010). "Nicotine receptors and depression: revisiting and revising the cholinergic hypothesis". Trends in Pharmacological Sciences. 31 (12): 580–6. doi:10.1016/j.tips.2010.09.004. PMC 2991594. PMID 20965579.
- ↑ Peters, Ruth; Poulter, Ruth; Warner, James; Beckett, Nigel; Burch, Lisa; Bulpitt, Chris (December 2008). "Smoking, dementia and cognitive decline in the elderly, a systematic review". BMC Geriatrics. 8: 36. doi:10.1186/1471-2318-8-36. PMC 2642819. PMID 19105840.
- ↑ Henningfield JE, Zeller M (2009). "Nicotine Psychopharmacology: Policy and Regulatory". Nicotine Psychopharmacology. Handbook of Experimental Pharmacology. Vol. 192. pp. 511–34. doi:10.1007/978-3-540-69248-5_18. ISBN 978-3-540-69246-1. PMID 19184661.
- ↑ Quik M, O'Leary K, Tanner CM (September 2008). "Nicotine and Parkinson's disease: implications for therapy". Movement Disorders. 23 (12): 1641–52. doi:10.1002/mds.21900. PMC 4430096. PMID 18683238.
- ↑ 253.0 253.1 Fujii T, Mashimo M, Moriwaki Y, Misawa H, Ono S, Horiguchi K, Kawashima K (September 2017). "Expression and Function of the Cholinergic System in Immune Cells". Frontiers in Immunology. 8: 1085. doi:10.3389/fimmu.2017.01085. PMC 5592202. PMID 28932225.
- ↑ Banala, Sambashiva; Arvin, Matthew C; Bannon, Nicholas M; Jin, Xiao-Tao; Macklin, John J; Wang, Yong; Peng, Can; Zhao, Guiqing; Marshall, John J; Gee, Kyle R; Wokosin, David L; Kim, Veronica J; McIntosh, J Michael; Contractor, Anis; Lester, Henry A; Kozorovitskiy, Yevgenia; Drenan, Ryan M; Lavis, Luke D (May 2018). "Photoactivatable drugs for nicotinic optopharmacology". Nature Methods. 15 (5): 347–350. doi:10.1038/nmeth.4637. PMC 5923430. PMID 29578537.
- ↑ Holliday RS, Campbell J, Preshaw PM (July 2019). "Effect of nicotine on human gingival, periodontal ligament and oral epithelial cells. A systematic review of the literature". Journal of Dentistry. 86: 81–88. doi:10.1016/j.jdent.2019.05.030. PMID 31136818.
- ↑ Holliday R, Preshaw PM, Ryan V, Sniehotta FF, McDonald S, Bauld L, McColl E (4 June 2019). "A feasibility study with embedded pilot randomised controlled trial and process evaluation of electronic cigarettes for smoking cessation in patients with periodontitis". Pilot and Feasibility Studies. 5 (1): 74. doi:10.1186/s40814-019-0451-4. PMC 6547559. PMID 31171977.
External links
| Wikisource has the text of the 1911 Encyclopædia Britannica article Nicotine. |
- Pages using duplicate arguments in template calls
- Pages with reference errors
- Pages with broken file links
- Alkaloids found in Erythroxylum coca
- Alkaloids found in Nicotiana
- Anorectics
- Pfizer brands
- Drugs developed by GSK plc
- Anxiolytics
- Euphoriants
- Nicotinic agonists
- Nicotinic antagonists
- Plant toxin insecticides
- Pregnane X receptor agonists
- Pyridine alkaloids
- Pyrrolidine alkaloids
- Smoking
- Stimulants
- Teratogens
- 3-Pyridyl compounds





