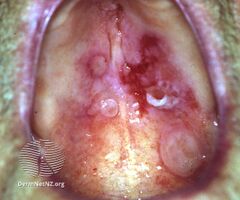
Mucous membrane pemphigoid
| Mucous membrane pemphigoid | |
|---|---|
| Other names: Cicatricial pemphigoid; MMP, Benign mucosal pemphigoid, Benign mucous membrane pemphigoid,[1] Ocular pemphigoid,[2] and Scarring pemphigoid[1]) | |
 | |
| Cicatricial pemphigoid | |
| Symptoms | Blisters in eyes, mouth, skin[3] |
| Complications | Scarring and blindness.[4] |
| Frequency | Elderly females[4] |
Mucous membrane pemphigoid is a rare longterm autoimmune blistering skin disease characterized by erosions in the eyes, mouth and skin.[3][5] It tends to cause scarring and blindness.[4]
It has a tendency to affect elderly females.[4]
Signs and symptoms
The autoimmune reaction most commonly affects the oral mucosa in the mouth, causing lesions in the gums (gingiva), known as desquamative gingivitis. More severe cases can also affect areas of mucous membrane elsewhere in the body, such as the sinuses, genitals, anus, and cornea.[6] When the cornea of the eye is affected, repeated scarring may result in blindness.
Brunsting–Perry cicatricial pemphigoid is a rare variant of mucous membrane pemphigoid involving the scalp and the neck without mucosal involvement. It is proposed by some authors that this be called a variant of epidermolysis bullosa acquisita.[7] [1]
Nikolsky's sign (gentle lateral pressure) on unaffected mucosa or skin raises a bulla. If no lesions are present on examination it may be useful way of demonstrating reduced epithelial adhesion. In contrast, in Pemphigus, the epithelium tends to disintegrate rather than form a bulla.
Nikolsky's sign is present in pemphigus and mucous membrane pemphigoid, but not in bullous pemphigoid.
-
Cicatricial pemphigoid
-
Cicatricial pemphigoid
Pathophysiology
In mucous membrane pemphigoid, the autoimmune reaction occurs in the skin, specifically at the level of the basement membrane, which connects the lower skin layer (dermis) to the upper skin layer (epidermis) and keeps it attached to the body.
When the condition is active, the basement membrane is dissolved by the antibodies produced, and areas of skin lift away at the base, causing hard blisters which scar if they burst. In other words, this is a desquamating/blistering disease in which the epithelium "unzips" from the underlying connective tissue, allowing fluid to gather that subsequently manifest as bullae, or blisters.
Diagnosis
Diagnostic techniques:
- antibodies (IgG) precipitate complement (C3) in the lamina lucida of the basement membrane.
- Circulating auto-antibodies to BP-1 antigen (located in hemidesmosome). 50% have BP-2.
- Positive Nikolsky sign.
- IgG, C3 deposition at BM creating smooth line in immunofluorescent analysis.
Management
The management depends upon the severity of the condition. For example, where there are lesions in the mouth alone, systemic drugs are less likely to be used. Where the condition is not limited to the mouth, or where there is poor response to Topical treatments, systemic drugs are more likely to be used.[8]
Conservative
Simple measures that can be taken include avoidance of hard, sharp or rough foods, and taking care when eating. Good oral hygiene is also usually advised, and professional oral hygiene measures such as dental scaling.[8]
Medications
Topical and intralesional (injected into the affected areas) corticosteroid drugs may be used, such as fluocinonide, clobetasol propionate or triamcinolone acetonide. Oral candidiasis may develop with long term topical steroid use, and sometimes antimycotics such as miconazole gel or chlorhexidine mouthwash are used to prevent this. Topical ciclosporin is sometimes used.
Dapsone is sometimes used as a steroid sparing agent. The dose is often increased very slowly in order to minimize side effects. Systemic steroids, such as prednisone or prednisolone may be needed in severe cases. Many other drugs have been used to treat mucous membrane pemphoid, including azathioprine, cyclophosphamide, methotrexate, thalidomide, mycophenolate mofetil, leflunomide, sulphasalazine, sulphapuridine, sulphamethoxypiridazine, tetracyclines (e.g. minocycline, doxycycline) and nicotinamide.[8]
Other treatments
Plasmapheresis appears to help some cases. Sometimes surgical procedures are required to repair scars, prevent complications such as blindness, upper airway stenosis or esophageal stricture.[8]
See also
- List of cutaneous conditions
- List of target antigens in pemphigoid
- List of immunofluorescence findings for autoimmune bullous conditions
References
- ↑ 1.0 1.1 1.2 Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. ISBN 978-1-4160-2999-1.
- ↑ "Pemphigoid, Benign Mucous Membrane". MeSH. 2019. Archived from the original on 10 January 2021. Retrieved 22 July 2019.
- ↑ 3.0 3.1 James, William D.; Elston, Dirk; Treat, James R.; Rosenbach, Misha A.; Neuhaus, Isaac (2020). "21. Chronic blistering dermatoses". Andrews' Diseases of the Skin: Clinical Dermatology (13th ed.). Edinburgh: Elsevier. p. 466-468. ISBN 978-0-323-54753-6. Archived from the original on 2022-03-22. Retrieved 2022-03-22.
- ↑ 4.0 4.1 4.2 4.3 Johnstone, Ronald B. (2017). "6. Vesiculobullous reaction pattern". Weedon's Skin Pathology Essentials (2nd ed.). Elsevier. p. 127. ISBN 978-0-7020-6830-0. Archived from the original on 2021-05-25. Retrieved 2022-03-22.
- ↑ Holtsche, MM; Zillikens, D; Schmidt, E (January 2018). "[Mucous membrane pemphigoid]". Der Hautarzt; Zeitschrift für Dermatologie, Venerologie, und verwandte Gebiete. 69 (1): 67–83. doi:10.1007/s00105-017-4089-y. PMID 29242962.
- ↑ "Mucous Membrane Pemphigoid". British Skin Foundation. Archived from the original on 2020-06-11. Retrieved 2020-12-27.
- ↑ Chen, Peggy. "Brunsting-Perry cicatricial pemphigoid". dermnetz.org. Archived from the original on 22 July 2019. Retrieved 21 July 2019.
- ↑ 8.0 8.1 8.2 8.3 Scully, Crispian; Lo Muzio, Lorenzo (30 June 2008). "Oral mucosal diseases: Mucous membrane pemphigoid". British Journal of Oral and Maxillofacial Surgery. 46 (5): 358–366. doi:10.1016/j.bjoms.2007.07.200. PMID 17804127.
External links
| Classification |
|---|