Melasma
| Melasma | |
|---|---|
| Other names: Chloasma faciei,[1] mask of pregnancy[2] | |
 | |
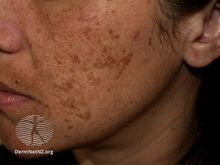
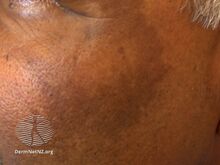
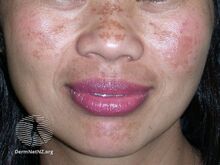
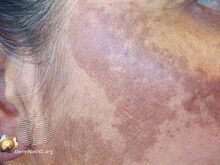
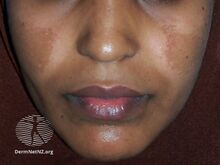
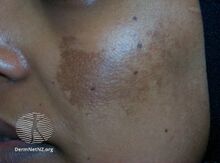
| Melasma on the cheek | |
| Specialty | Dermatology |
| Symptoms | Areas of brown or darker skin on the face[3] |
| Usual onset | 20 to 40 yr old[4] |
| Types | Epidermal, dermal, mixed[4] |
| Risk factors | Sun exposure, genetics, pregnancy, hormonal birth control, hormone replacement therapy[3][5] |
| Diagnostic method | Based on the appearance[4] |
| Differential diagnosis | Solar lentigo, drug induced hyperpigmentation, Nevus of Ota, post inflmmatory hyperpigmentation[4] |
| Treatment | Sunscreen[6] |
| Medication | Hydroquinone, tretinoin, steroid cream[7] |
| Prognosis | Generally good[7] |
| Frequency | Common[3] |
Melasma, also known as the mask of pregnancy,[8] generally presents with areas of brown or darker skin on both sides of the face.[3][4] Most commonly it occurs on the cheeks, chin, nose, or forehead.[3] Less commonly the forearms or neck may be involved.[6]
Causes may include sun exposure, genetics, pregnancy, hormonal birth control, hormone replacement therapy (HRT), or certain medications.[3][5] Occasionally thyroid disorders are implicated.[4] Diagnosis is generally by examination of the skin.[7] Occasionally a skin biopsy may be done to rule out other potential causes.[7]
Treatment generally involves avoiding the sun and wearing sunscreen.[6] Often it will resolve on its own when the trigger is not longer present.[7] Occasionally medications such as hydroquinone, tretinoin, or steroid cream may be used.[7] A number of other medications or procedures may also be used.[4] Outcomes are generally good; however, the condition can reoccur.[7][4]
Melasma is common affecting between 1.5% and 33% of people.[3] Women are affected about 10 times more often than men.[3][5] Onset is typically in the 20s and 30s.[4] People with darker skin are more commonly affected.[9] The term "melasma" means brown skin.[4]
Signs and symptoms
The symptoms of melasma are dark, irregular well demarcated hyperpigmented macules to patches. These patches often develop gradually over time. Melasma does not cause any other symptoms beyond the cosmetic discoloration.[10] Patches can vary in size from 0.5 cm to larger than 10 cm depending on the person. The location of melasma can be categorized as centrofacial, malar, or mandibular. The most common is centrofacial in which patches appear on the cheeks, nose, upper lip, forehead, and chin. The mandibular category accounts for patches on the bilateral rami, while the malar location accounts for patches only on the nose and checks.[11]
Cause
Melasma is thought to be the stimulation of melanocytes (cells in the dermal layer which transfer a pigment called melanin to the keratinocytes of skin) when the skin is exposed to ultraviolet light from the sun. Small amounts of sun exposure can make melasma return to the skin after it has faded, which is why people with melasma often get it repeatedly, particularly in the summer.[13]
Pregnant women often get melasma. Birth control pills and hormone replacement medicine can also be a trigger. The discoloration usually disappears spontaneously over a period of several months after giving birth or stopping the hormones.[13]
Genetic predisposition is also a major factor in determining whether someone will develop melasma. People with the Fitzpatrick skin type III or greater from African, Asian, or Hispanic descent are at a much higher risk than others.[11] In addition women with a light brown skin type who are living in regions with intense sun exposure are particularly susceptible to developing this condition.[14]
The rate of melasma also increases in thyroid disease.[15] It is thought that the overproduction of melanocyte-stimulating hormone (MSH) brought on by stress can cause outbreaks of this condition. Other rare causes of melasma include allergic reaction to medications and cosmetics.
Melasma suprarenale (Latin - above the kidneys) is a symptom of Addison's disease, particularly when caused by pressure or minor injury to the skin, as discovered by Dr. FJJ Schmidt of Rotterdam in 1859.
Diagnosis
There are two different kinds of melasma, epidermal and dermal. Epidermal melasma results from melanin pigment that is elevated in the suprabasal layers of the epidermis. Dermal melasma occurs when the dermal macrophages have an elevated melanin level.[16] Melasma is usually diagnosed visually or with assistance of a Wood's lamp (340 - 400 nm wavelength).[17] Under Wood's lamp, excess melanin in the epidermis can be distinguished from that of the dermis. This is done by looking at how dark the melasma appears, dermal melasma will appear darker than epidermal melasma under the Wood's lamp.[16]
Differential diagnosis
- Post inflammatory hyperpigmentation
- Actinic lichen planus
- Hydroquinone-induced exogenous ochronosis
Treatment

Treatments to hasten the fading of the discolored patches include:
- Topical depigmenting agents, such as hydroquinone (HQ) either in over-the-counter (2%) or prescription (4%) strength.[18] HQ is a chemical that inhibits tyrosinase, an enzyme involved in the production of melanin.
- Tretinoin,[19] an acid that increases skin cell (keratinocyte) turnover. This treatment is not used during pregnancy due to risk of harm to the fetus.
- Azelaic acid (20%), thought to decrease the activity of melanocytes.[13]
- Tranexamic acid by mouth has shown to provide rapid and sustained lightening in melasma by decreasing melanogenesis in epidermal melanocytes.
- Cysteamine hydrochloride (5%) over-the-counter.[20][21] Mechanism of action seems to involve inhibition of melanin synthesis pathway[22]
- Kojic acid (2%) over-the-counter.[11]
- Flutamide (1%)[23]
- Chemical peels[24]
- Microdermabrasion to dermabrasion (light to deep)[25]
- Galvanic or ultrasound facials with a combination of a topical crème/gel. Either in an aesthetician's office or as a home massager unit.
- Laser but not IPL (IPL can make the melasma darker)
Evidence-based reviews found that the most effective therapy for melasma includes a combination of topical agents.[19][18] Triple combination creams formulated with hydroquinone, tretinoin and a steroid component have shown to be more effective than dual combination therapy or hydroquinone alone.[26] More recently, a systematic review found that oral medications also have a role in melasma treatment, and have been shown to be efficacious with a minimal number and severity of adverse events. Oral medications and dietary supplements employed in the treatment of melasma include tranexamic acid, Polypodium leucotomos extract, beta‐carotenoid, melatonin, and procyanidin.[27] Oral procyanidin combined with vitamins A, C, and E shows promise as safe and effective for epidermal melasma. In an 8-week randomized, double-blind, placebo-controlled trial in 56 Filipino women, treatment was associated with significant improvements in the left and right malar regions, and was safe and well tolerated.[28]
In all of these treatments the effects are gradual and a strict avoidance of sunlight is required. The use of broad-spectrum sunscreens with physical blockers, such as titanium dioxide and zinc dioxide is preferred.[29] This is because UV-A, UV-B and visible lights are all capable of stimulating pigment production.
There are many negative side effects that go along with these treatments and many times treatments are unsatisfying overall. Things such as scarring, irritation, lighter patches of skin, and contact dermatitis are all commonly seen to occur.[16]
Patients should avoid other precipitants including hormonal triggers.
Cosmetic camouflage can also be used to hide melasma.
See also
References
- ↑ James, William; Berger, Timothy; Elston, Dirk (2005). Andrews' Diseases of the Skin: Clinical Dermatology. (10th ed.). Saunders. ISBN 0-7216-2921-0.: 854
- ↑ Tunzi, M; Gray, GR (January 2007). "Common skin conditions during pregnancy". Am Fam Physician. 75 (2): 211–18. PMID 17263216.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 Basit, H; Godse, KV; Al Aboud, AM (January 2020). "Melasma". PMID 29083744.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 4.8 4.9 "Melasma | DermNet NZ". www.dermnetnz.org. Archived from the original on 21 October 2020. Retrieved 22 October 2020.
- ↑ 5.0 5.1 5.2 "Melasma: Who gets and causes". www.aad.org. Archived from the original on 26 October 2020. Retrieved 22 October 2020.
- ↑ 6.0 6.1 6.2 "Melasma: Overview". www.aad.org. Archived from the original on 4 April 2013. Retrieved 22 October 2020.
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 7.6 "Melasma: Diagnosis and treatment". www.aad.org. Archived from the original on 19 October 2020. Retrieved 22 October 2020.
- ↑ Tunzi, M; Gray, GR (January 2007). "Common skin conditions during pregnancy". Am Fam Physician. 75 (2): 211–18. PMID 17263216.
- ↑ Onalaja, Amanda A.; Taylor, Susan C. (2021). "1. Defining skin color". In Li, Becky S.; Maibach, Howard I. (eds.). Ethnic Skin and Hair and Other Cultural Considerations. Switzerland: Springer. p. 12. ISBN 978-3-030-64829-9. Archived from the original on 2022-09-15. Retrieved 2022-08-29.
- ↑ "Melasma | American Academy of Dermatology". www.aad.org. Archived from the original on 2016-03-01. Retrieved 2016-02-25.
- ↑ 11.0 11.1 11.2 Arndt, Kenneth A., 1936- (2014-02-05). Manual of dermatologic therapeutics. Hsu, Jeffrey T. S. (Eighth ed.). [Place of publication not identified]. ISBN 978-1-4698-7200-1. OCLC 953864747.
{{cite book}}: CS1 maint: multiple names: authors list (link) - ↑ "Melasma images | DermNet NZ". www.dermnetnz.org. Archived from the original on 28 September 2020. Retrieved 22 October 2020.
- ↑ 13.0 13.1 13.2 "Melasma | American Academy of Dermatology". www.aad.org. Archived from the original on 2016-03-01. Retrieved 2016-02-25.
- ↑ "Melasma | American Academy of Dermatology". www.aad.org. Archived from the original on 2016-03-01. Retrieved 2016-02-25.
- ↑ Lutfi, R. J.; Fridmanis, M; Misiunas, A. L.; Pafume, O; Gonzalez, E. A.; Villemur, J. A.; Mazzini, M. A.; Niepomniszcze, H (1985). "Association of melasma with thyroid autoimmunity and other thyroidal abnormalities and their relationship to the origin of the melasma". The Journal of Clinical Endocrinology and Metabolism. 61 (1): 28–31. doi:10.1210/jcem-61-1-28. PMID 3923030.
- ↑ 16.0 16.1 16.2 Evidence-based dermatology. Williams, Hywel C.,, Bigby, Michael E. (Third ed.). Chichester, West Sussex. 2014-06-05. ISBN 978-1-118-35762-0. OCLC 867001321.
{{cite book}}: CS1 maint: others (link) - ↑ "Melasma | American Academy of Dermatology". www.aad.org. Archived from the original on 2016-03-01. Retrieved 2016-02-25.
- ↑ 18.0 18.1 Jutley, Gurpreet Singh; Rajaratnam, Ratna; Halpern, James; Salim, Asad; Emmett, Charis (2014-02-01). "Systematic review of randomized controlled trials on interventions for melasma: an abridged Cochrane review". Journal of the American Academy of Dermatology. 70 (2): 369–373. doi:10.1016/j.jaad.2013.07.044. ISSN 1097-6787. PMID 24438951.
- ↑ 19.0 19.1 Rivas, Shelly; Pandya, Amit G. (2013-10-01). "Treatment of melasma with topical agents, peels and lasers: an evidence-based review". American Journal of Clinical Dermatology. 14 (5): 359–376. doi:10.1007/s40257-013-0038-4. ISSN 1179-1888. PMID 23881551.
- ↑ Mansouri, P.; Farshi, S.; Hashemi, Z.; Kasraee, B. (2015-07-01). "Evaluation of the efficacy of cysteamine 5% cream in the treatment of epidermal melasma: a randomized double-blind placebo-controlled trial". British Journal of Dermatology. 173 (1): 209–217. doi:10.1111/bjd.13424. ISSN 1365-2133. PMID 25251767.
- ↑ Bleehen, S. S.; Pathak, M. A.; Hori, Y.; Fitzpatrick, T. B. (1968-02-01). "Depigmentation of skin with 4-isopropylcatechol, mercaptoamines, and other compounds". The Journal of Investigative Dermatology. 50 (2): 103–117. doi:10.1038/jid.1968.13. ISSN 0022-202X. PMID 5641641.
- ↑ Qiu, L.; Zhang, M.; Sturm, R. A.; Gardiner, B.; Tonks, I.; Kay, G.; Parsons, P. G. (2000-01-01). "Inhibition of melanin synthesis by cystamine in human melanoma cells". The Journal of Investigative Dermatology. 114 (1): 21–27. doi:10.1046/j.1523-1747.2000.00826.x. ISSN 0022-202X. PMID 10620110.
- ↑ Adalatkhah, Hassan; Sadeghi-Bazargani, Homayoun (2015-01-01). "The first clinical experience on efficacy of topical flutamide on melasma compared with topical hydroquinone: a randomized clinical trial". Drug Design, Development and Therapy. 9: 4219–4225. doi:10.2147/DDDT.S80713. ISSN 1177-8881. PMC 4531037. PMID 26345129.
- ↑ Chaudhary, Savita; Dayal, Surabhi (2013-10-01). "Efficacy of combination of glycolic acid peeling with topical regimen in treatment of melasma". Journal of Drugs in Dermatology. 12 (10): 1149–1153. ISSN 1545-9616. PMID 24085051. Archived from the original on 2020-08-08. Retrieved 2020-09-08.
- ↑ "Melasma: Diagnosis and treatment". www.aad.org. Archived from the original on 2020-10-19. Retrieved 2020-10-19.
- ↑ Rajaratnam, Ratna; Halpern, James; Salim, Asad; Emmett, Charis (2010-07-07). "Interventions for melasma". Cochrane Database of Systematic Reviews (7): CD003583. doi:10.1002/14651858.CD003583.pub2. ISSN 1465-1858. PMID 20614435. Archived from the original on 2018-06-13. Retrieved 2018-06-13.
- ↑ Zhou, Linghong Linda; Baibergenova, Akerke (2017-09-01). "Melasma: systematic review of the systemic treatments". International Journal of Dermatology. 56 (9): 902–908. doi:10.1111/ijd.13578. ISSN 1365-4632. PMID 28239840.
- ↑ Handog, Evangeline (2009-07-20). "A randomized, double-blind, placebo-controlled trial of oral procyanidin with Vitamins A, C, E for melasma among Filipino women". International Journal of Dermatology. 48 (8): 896–901. doi:10.1111/j.1365-4632.2009.04130.x. PMID 19659873.
- ↑ "Melasma: Tips for managing". www.aad.org. Archived from the original on 2020-10-19. Retrieved 2020-10-19.
External links
| Classification | |
|---|---|
| External resources |