Keratosis pilaris
| Keratosis pilaris | |
|---|---|
| Other names: Follicular keratosis, lichen pilaris, chicken skin[1] | |
 | |
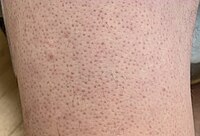
| Keratosis pilaris as seen on the calf | |
| Specialty | Dermatology |
| Symptoms | Painless red bumpy skinref name=Weedon2017.15/> |
| Usual onset | Early childhood[2] |
| Duration | Long term[3] |
| Risk factors | Obesity, atopic dermatitis, ichthyosis vulgaris, pregnancy, diabetes[1] |
| Diagnostic method | Based on symptoms and examination[2] |
| Differential diagnosis | Acne, folliculitis, atopic dermatitis, milia, scurvy[2] |
| Treatment | Moisturizers, creams that include lactic acid or salicylic acid, phototherapy[1][2] |
| Prognosis | Not serious[2] |
| Frequency | Common (female>male)[3] |
Keratosis pilaris (KP) is a skin condition that results in multiple small red bumps in skin.[4] It is generally not itchy or painful.[2] The most commonly affected areas are the back of the upper arms, thighs, and buttocks.[2] Less frequently the face, chest, or forearms may be involved.[2] Often it gets better during the summer and worse during the winter.[2] It may be associated with other medical conditions and may result in psychological distress.[2]
KP has an autosomal dominant genetic inheritance.[2] It is associated with obesity, atopic dermatitis, ichthyosis vulgaris, pregnancy, diabetes, and rarely cancer.[1] It may also be associated with a number of genetic syndromes.[1] The underlying mechanism is not completely understood.[2] Proposals include that it is an abnormality in the process of depositing the keratin in hair follicles, abnormalities in the hair shaft, or both.[1] Diagnosis is usually based on the skin's appearance; however, dermoscopy may be useful in unclear cases.[1][2]
There is no cure; though, the condition often improves with time.[2] Treatments may improve the appearance.[2] This may include applying moisturizers and medications such as lactic acid, salicylic acid, urea, or retinoids to the skin.[1] Fractional carbon dioxide lasers and Nd:YAG laser therapies may also be tried.[1] The condition is common.[3] Onset is often in later childhood with up to 80% affected, with it still present in about 40% of adults.[2] Though others report rates of 0.8% to 34% of the population.[1]
Signs and symptoms
KP results in small, rough bumps on the surface of the skin. They are skin-colored bumps the size of a grain of sand, many of which are surrounded by a slight pink color in light skinned people and dark spots in dark skinned people.[5] Most people with KP do not have symptoms, but the bumps in the skin can occasionally be itchy.[6] Irritation due to scratching KP bumps can result in redness and inflammation.
Though people with KP experience the condition year-round, the problem can become exacerbated, with the bumps likely to look and feel more pronounced in color and texture, during the colder months when moisture levels in the air are lower.[7] The symptoms may also worsen during pregnancy or after childbirth.[8]
Hairless skin (like the palms or soles) is not involved.[9]
-
Keratosis pilaris on lower leg
-
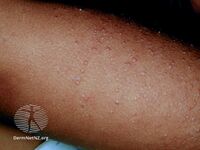
Keratosis pilaris on back of upper arm
-
Keratosis pilaris arm
-
Keratosis pilaris in darker skin
-
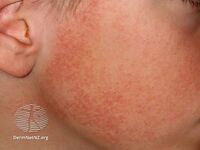
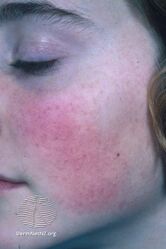
Keratosis pilaris face
-
Keratosis pilaris face
-
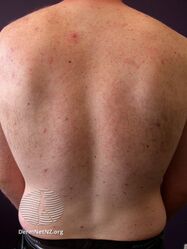
Keratosis pilaris back
Pathophysiology
KP occurs when the human body produces excess amounts of the skin protein keratin, resulting in the formation of small, raised bumps in the skin often with surrounding redness.[6] The excess keratin, which is the same color of the person's natural skin tone, surrounds and entraps the hair follicles in the pore. This causes the formation of hard plugs (process known as hyperkeratinization).[5] Many KP bumps contain an ingrown hair that has coiled.[10] This is a result of the keratinized skin's "capping off" the hair follicle, preventing the hair from exiting. The hair grows encapsulated inside the follicle. KP is more common in patients affected by atopic diseases such as allergic rhinitis and atopic dermatitis.
KP subtypes are occasionally part of genetically inherited syndromes associated with intellectual disability, neuro-cardio-facial-cutaneous syndromes, RASopathies, ectodermal dysplasias, and certain myopathies.[1]
Diagnosis
Physicians can often diagnose KP simply by examining the skin without specialized tests.[5] However, a dermatologist can use dermoscopy to confirm the diagnosis and assess if a person with KP is responding to treatment.[10] Physicians will often consider family history and the presence of symptoms when making the diagnosis.[11] Those with this condition are generally encouraged to contact a physician if the bumps are bothersome and do not improve with over-the-counter lotions.[5]
Classification
There are several different types of KP. Variations of KP include KP rubra (red, inflamed bumps which can be on arms, head, legs), KP alba (rough, bumpy skin with no irritation), KP rubra faceii (reddish rash on the cheeks), KP atrophicans, keratosis follicularis spinulosa decalvans, atrophoderma vermiculatum, KP atrophicans faciei, erythromelanosis follicularis faciei et colli, and papular profuse precocious KP.[1][6]
KP is commonly described in association with other dry skin conditions, such as ichthyosis vulgaris, dry skin and atopic dermatitis, including those of asthma and allergies.[1]
KP does not bear any known, long-term health implications, nor is it associated with increased mortality or morbidity.[12] It is not related to goose bumps, which results from muscle contractions, except that both occur in the area where the hair shaft exits the skin.
Differential diagnosis
Several medications can cause a skin eruption similar to KP. Medications known to produce this type of skin eruption include cyclosporine, BRAF inhibitors, and tyrosine kinase inhibitors.[1]
Treatment
KP is medically harmless,[10] but many individuals may seek treatment as the condition can cause emotional distress.[8] Topical creams and lotions are currently the most commonly used treatment for KP, specifically those consisting of moisturizing or keratolytic treatments, including urea, lactic acid, glycolic acid, salicylic acid, vitamin D, fish oil, or topical retinoids such as tretinoin.[13] Improvement of the skin often takes months and the bumps are likely to return. Limiting time in the shower and using gentle exfoliation to unplug pores can help.[8][14] Many products are available that apply abrasive materials to and alpha or beta hydroxy acids to assist with exfoliation.
Some cases of KP have been successfully treated with laser therapy, which involves passing intense bursts of light into targeted areas of the skin.[15] Depending on the body's response to the treatment, multiple sessions over the course of a few months may be necessary.
Epidemiology
Worldwide, KP affects an estimated 30 to 50% of the adult population and approximately 50 to 80% of all adolescents. It is more common in women than in men, and it is often present in otherwise healthy individuals.[13] The skin condition is prevalent in persons of all ethnicities, and no particular ethnicity is at higher risk for developing KP. Although KP may manifest in persons of any age, it usually appears within the first decade of life and is more common in young children.[12] In most cases, the condition gradually improves before age 30; however, it can persist longer.[8]
See also
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 Wang, JF; Orlow, SJ (July 2018). "Keratosis Pilaris and its Subtypes: Associations, New Molecular and Pharmacologic Etiologies, and Therapeutic Options". American Journal of Clinical Dermatology. 19 (5): 733–757. doi:10.1007/s40257-018-0368-3. PMID 30043128.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 Pennycook, KB; McCready, TA (January 2020). "Keratosis Pilaris". PMID 31536314.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ 3.0 3.1 3.2 James, William D.; Elston, Dirk; Treat, James R.; Rosenbach, Misha A.; Neuhaus, Isaac (2020). "27. Genodermatoses and congenital anomalies". Andrews' Diseases of the Skin: Clinical Dermatology (13th ed.). Elsevier. p. 585. ISBN 978-0-323-54753-6. Archived from the original on 2021-10-17. Retrieved 2021-10-16.
- ↑ Johnstone, Ronald B. (2017). "15. Diseases of cutaneous appendages". Weedon's Skin Pathology Essentials (2nd ed.). Elsevier. p. 324. ISBN 978-0-7020-6830-0. Archived from the original on 2021-05-25. Retrieved 2021-09-25.
- ↑ 5.0 5.1 5.2 5.3 Berman, Kevin. "Keratosis pilaris". MedlinePlus. Archived from the original on 2016-07-04. Retrieved 2008-06-19.
- ↑ 6.0 6.1 6.2 Hwang S, Schwartz RA (September 2008). "Keratosis pilaris: a common follicular hyperkeratosis". Cutis. 82 (3): 177–80. PMID 18856156.
- ↑ "Keratosis pilaris ("chicken skin")". NHS Choices. 2017-10-24. Archived from the original on 2013-07-07. Retrieved 2013-06-30.
- ↑ 8.0 8.1 8.2 8.3 "Keratosis pilaris: Self-management". Mayo Clinic. Archived from the original on 2016-04-03. Retrieved 2016-04-11.
- ↑ Alai, Nili. "Keratosis Pilaris (KP)". MedicineNet. Archived from the original on 2018-06-18. Retrieved 2008-10-06.
- ↑ 10.0 10.1 10.2 Panchaprateep R, Tanus A, Tosti A (March 2015). "Clinical, dermoscopic, and histopathologic features of body hair disorders". Journal of the American Academy of Dermatology. 72 (5): 890–900. doi:10.1016/j.jaad.2015.01.024. PMID 25748313.
- ↑ Mayo Clinic Staff. "Tests and Diagnosis". Mayo Clinic. Retrieved 2013-10-31
- ↑ 12.0 12.1 Alai, Nili; Arash Michael Saemi; Raul Del Rosario. "Keratosis Pilaris". eMedicine. Medscape (WebMD). Archived from the original on 2000-10-01. Retrieved 2008-10-20. and "Pathophysiology". Medscape (WebMD). Archived from the original on October 1, 2000. Retrieved February 5, 2018.
- ↑ 13.0 13.1 Yosipovitch G, DeVore A, Dawn A (June 2007). "Obesity and the skin: skin physiology and skin manifestations of obesity". Journal of the American Academy of Dermatology. 56 (6): 901–16. doi:10.1016/j.jaad.2006.12.004. PMID 17504714.
- ↑ Mayo Clinic Staff (5 January 2016). "Self-management - Keratosis Pilaris". mayoclinic.org. Mayo Foundation. Archived from the original on 3 April 2016. Retrieved 11 April 2016.
- ↑ Schoch, Jennifer J.; Tollefson, Megha M.; Witman, Patricia; Davis, Dawn M. R. (July 2016). "Successful Treatment of Keratosis Pilaris Rubra with Pulsed Dye Laser". Pediatric Dermatology. 33 (4): 443–446. doi:10.1111/pde.12892. ISSN 1525-1470. PMID 27282957.
External links
| Classification | |
|---|---|
| External resources |
- The American Academy of Dermatology Archived 2016-11-25 at the Wayback Machine
- The American Osteopathic College of Dermatology Archived 2010-07-21 at the Wayback Machine - Article on keratosis pilaris