Impetigo
| Impetigo | |
|---|---|
| Other names: School sores,[1] impetigo contagiosa | |
 | |
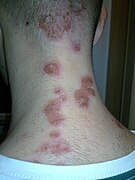
| A case of impetigo on the chin | |
| Pronunciation | |
| Specialty | Dermatology |
| Symptoms | Yellowish skin crusts, painful[2] |
| Complications | Cellulitis, poststreptococcal glomerulonephritis[3] |
| Usual onset | Young children[3] |
| Duration | Less than 3 weeks[3] |
| Types | Bullous impetigo, ecthyma |
| Causes | Staphylococcus aureus or Streptococcus pyogenes which spreads by direct contact[4] |
| Risk factors | Day care, crowding, poor nutrition, diabetes mellitus, contact sports, breaks in the skin[3][5] |
| Prevention | Hand washing, avoiding infected people, cleaning injuries[3] |
| Treatment | Based on symptoms[3] |
| Medication | Antibiotics (mupirocin, fusidic acid, cephalexin)[3][6] |
| Prognosis | Good[4] |
| Frequency | 140 million (2010)[7] |
Impetigo is a bacterial infection that involves the superficial skin.[2] It typically presents as yellowish crusts on reddened skin, most frequently of the face, arms, or legs.[2] Less commonly there may be large blisters which affect the groin or armpits.[8] The lesions may be painful or itchy.[3] Fever is uncommon.[3] Healing generally occurs without scarring.[4]
Half of cases are typically due to Staphylococcus aureus, with or withoutStreptococcus pyogenes.[4] Risk factors include attending day care, crowding, poor nutrition, diabetes mellitus, contact sports, and breaks in the skin such as from mosquito bites, eczema, scabies, or herpes.[3][5] With contact it can spread around or between people.[4] Diagnosis is typically based on the symptoms and appearance.[4]
Prevention is by hand washing, avoiding people who are infected, and cleaning injuries.[4] Treatment is typically with antibiotic creams, such as mupirocin 2% applied for 5-days.[9] An alternative is fusidic acid cream.[3][6] Antibiotics by mouth, such as cephalexin, may be used if large areas are affected.[3] Antibiotic-resistant forms have been found.[3]
Impetigo affected about 140 million people (2% of the world population) in 2010.[7] It can occur at any age, but is most common in young children.[3] Without treatment people typically get better within three weeks.[3] Recurring infections can occur due to colonization of the nose by the bacteria.[10][11] Complications may include cellulitis or poststreptococcal glomerulonephritis.[3] The name is from the Latin impetere meaning "attack".[12]
Signs and symptoms
Contagious impetigo
This most common form of impetigo, also called nonbullous impetigo, most often begins as a red sore near the nose or mouth which soon breaks, leaking pus or fluid, and forms a honey-colored scab,[13] followed by a red mark which heals without leaving a scar. Sores are not painful, but they may be itchy. Lymph nodes in the affected area may be swollen, but fever is rare. Touching or scratching the sores may easily spread the infection to other parts of the body.[14]
Skin ulcers with redness and scarring also may result from scratching or abrading the skin.[citation needed]
Bullous impetigo

Bullous impetigo, mainly seen in children younger than 2 years, involves painless, fluid-filled blisters, mostly on the arms, legs, and trunk, surrounded by red and itchy (but not sore) skin. The blisters may be large or small. After they break, they form yellow scabs.[14]
Ecthyma
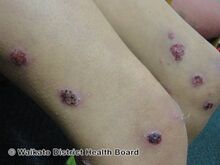
Ecthyma, the nonbullous form of impetigo, produces painful fluid- or pus-filled sores with redness of skin, usually on the arms and legs, become ulcers that penetrate deeper into the dermis.[4] After they break open, they form hard, thick, gray-yellow scabs, which sometimes leave scars. Ecthyma may be accompanied by swollen lymph nodes in the affected area.[14]
Causes
Impetigo is primarily caused by Staphylococcus aureus, and sometimes by Streptococcus pyogenes.[15] Both bullous and nonbullous are primarily caused by S. aureus, with Streptococcus also commonly being involved in the nonbullous form.[16]
Predisposing factors
Impetigo is more likely to infect children ages 2–5, especially those that attend school or day care.[3][17] 70% of cases are the nonbullous form and 30% are the bullous form.[3] Other factors can increase the risk of contracting impetigo such as diabetes mellitus, dermatitis, immunodeficiency disorders, and other irritable skin disorders.[18] Impetigo occurs more frequently among people who live in warm climates.[19]
Transmission
The infection is spread by direct contact with lesions or with nasal carriers. The incubation period is 1–3 days after exposure to Streptococcus and 4–10 days for Staphylococcus.[20] Dried streptococci in the air are not infectious to intact skin. Scratching may spread the lesions.[citation needed]
Diagnosis
Impetigo is usually diagnosed based on its appearance. It generally appears as honey-colored scabs formed from dried serum, and is often found on the arms, legs, or face.[15] If a visual diagnosis is unclear a culture may be done to test for resistant bacteria.[21]
Differential diagnosis
Other conditions that can result in symptoms similar to the common form include contact dermatitis, herpes simplex virus, discoid lupus, and scabies.[3]
Other conditions that can result in symptoms similar to the blistering form include other bullous skin diseases, burns, and necrotizing fasciitis.[3]
Prevention
To prevent the spread of impetigo the skin and any open wounds should be kept clean and covered. Care should be taken to keep fluids from an infected person away from the skin of a non-infected person. Washing hands, linens, and affected areas will lower the likelihood of contact with infected fluids. Scratching can spread the sores; keeping nails short will reduce the chances of spreading. Infected people should avoid contact with others and eliminate sharing of clothing or linens.[22]Children with impetigo can return to school 24 hours after starting antibiotic therapy as long as their draining lesions are covered.[23]
Treatment
Antibiotics, either as a cream or by mouth, are usually prescribed. Mild cases may be treated with mupirocin ointments. In 95% of cases, a single 7-day antibiotic course results in resolution in children.[23][24] It has been advocated that topical antiseptics are inferior to topical antibiotics, and therefore should not be used as a replacement.[3] However, the National Institute for Health and Care Excellence (NICE) as of February 2020 recommends a hydrogen peroxide 1% cream antiseptic rather than topical antibiotics for localised non-bullous impetigo in otherwise well individuals.[25] This recommendation is part of an effort to reduce the overuse of antimicrobials that may contribute to the development of resistant organisms[26] such as MRSA.
More severe cases require antibiotics by mouth, such as dicloxacillin, flucloxacillin, or erythromycin. Alternatively, clavulanate, cephalosporins (first-generation) and others may be used. Alternatives for people who are seriously allergic to penicillin or infections with methicillin-resistant Staphococcus aureus include doxycycline, clindamycin, and trimethoprim-sulphamethoxazole, although doxycycline should not be used in children under the age of eight due to the risk of drug-induced tooth discolouration.[23] When streptococci alone are the cause, penicillin is the drug of choice.
When the condition presents with ulcers, valacyclovir, an antiviral, may be given in case a viral infection is causing the ulcer.
Alternative medicine
There is not enough evidence to recommend alternative medicine such as tea tree oil or honey.[3]
Prognosis
Without treatment, individuals with impetigo typically get better within three weeks.[3] Complications may include cellulitis or poststreptococcal glomerulonephritis.[3] Rheumatic fever does not appear to be related.[3]
Epidemiology
Globally, impetigo affects more than 162 million children in low to middle income countries.[27] The rates are highest in countries with low available resources and is especially prevalent in the region of Oceania.[27] The tropical climate and high population in lower socioeconomic regions contribute to these high rates.[28] Children under the age of 4 in the United Kingdom are 2.8% more likely than average to contract impetigo; this decreases to 1.6% for children up to 15-years-old.[29] As age increases, the rate of impetigo declines, but all ages are still susceptible.[28]
History
Impetigo was originally described and differentiated by William Tilbury Fox.[30] The word "impetigo" is the generic Latin word for "skin eruption", and stems from the verb impetere, "to attack" (as in "impetus").[31] Before the discovery of antibiotics, the disease was treated with an application of the antiseptic gentian violet, which was an effective treatment.[32]
References
- ↑ "Impetigo (school sores, skin infections): Images, Causes, and Symptoms — DermNet". dermnetnz.org. Archived from the original on 7 June 2023. Retrieved 13 December 2023.
- ↑ 2.0 2.1 2.2 James, William D.; Elston, Dirk; Treat, James R.; Rosenbach, Misha A.; Neuhaus, Isaac (2020). "14. Bacterial infections". Andrews' Diseases of the Skin: Clinical Dermatology (13th ed.). Elsevier. pp. 252–254. ISBN 978-0-323-54753-6. Archived from the original on 2023-07-01. Retrieved 2023-12-13.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 3.14 3.15 3.16 3.17 3.18 3.19 3.20 3.21 3.22 3.23 3.24 Hartman-Adams, H; Banvard, C; Juckett, G (15 August 2014). "Impetigo: diagnosis and treatment". American Family Physician. 90 (4): 229–35. PMID 25250996.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 Stevens, Daniel L. (2022). "18. Impetigo". In Jong, Elaine C.; Stevens, Dennis L. (eds.). Netter's Infectious Diseases (2nd ed.). Philadelphia: Elsevier. pp. 78–80. ISBN 978-0-323-71159-3. Archived from the original on 2023-12-16. Retrieved 2023-12-15.
- ↑ 5.0 5.1 Adams, BB (2002). "Dermatologic disorders of the athlete". Sports Medicine. 32 (5): 309–21. doi:10.2165/00007256-200232050-00003. PMID 11929358. S2CID 34948265.
- ↑ 6.0 6.1 Koning, S; van der Sande, R; Verhagen, AP; van Suijlekom-Smit, LW; Morris, AD; Butler, CC; Berger, M; van der Wouden, JC (18 January 2012). "Interventions for impetigo". The Cochrane Database of Systematic Reviews. 1: CD003261. doi:10.1002/14651858.CD003261.pub3. PMC 7025440. PMID 22258953.
- ↑ 7.0 7.1 Vos, T (Dec 15, 2012). "Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries 1990-2010: a systematic analysis for the Global Burden of Disease Study 2010". Lancet. 380 (9859): 2163–96. doi:10.1016/S0140-6736(12)61729-2. PMC 6350784. PMID 23245607. Archived from the original on January 12, 2019. Retrieved April 20, 2018.
- ↑ Ibrahim, F; Khan, T; Pujalte, GG (December 2015). "Bacterial Skin Infections". Primary Care. 42 (4): 485–99. doi:10.1016/j.pop.2015.08.001. PMID 26612370.
- ↑ The WHO AWaRe (Access, Watch, Reserve) antibiotic book. World Health Organization. 2022. p. 197. Archived from the original on 13 August 2023. Retrieved 4 December 2023.
- ↑ "Impetigo symptoms and treatments". www.nhsinform.scot. Archived from the original on 2020-04-30. Retrieved 2020-05-26.
- ↑ "Impetigo and Ecthyma - Skin Disorders". Merck Manuals Consumer Version. Archived from the original on 2020-05-27. Retrieved 2020-05-26.
- ↑ Limited, Wordsworth Editions (1993). Concise English Dictionary. Wordsworth Editions. p. 452. ISBN 9781840224979. Archived from the original on 2016-10-03.
- ↑ Cole C, Gazewood J (2007). "Diagnosis and treatment of impetigo". Am Fam Physician. 75 (6): 859–64. ISSN 0002-838X. PMID 17390597. Archived from the original on 2015-04-30.
- ↑ 14.0 14.1 14.2 Mayo Clinic staff (5 October 2010). "Impetigo". Mayo Clinic Health Information. Mayo Clinic. Archived from the original on 28 November 2012. Retrieved 25 August 2012.
- ↑ 15.0 15.1 Kumar, Vinay; Abbas, Abul K.; Fausto, Nelson; & Mitchell, Richard N. (2007). Robbins Basic Pathology (8th ed.). Saunders Elsevier. pp. 843 ISBN 978-1-4160-2973-1
- ↑ Stulberg DL, Penrod MA, Blatny RA (2002). "Common bacterial skin infections". American Family Physician. 66 (1): 119–24. PMID 12126026. Archived from the original on 2007-09-29.
- ↑ "Impetigo (school sores)". www.health.govt.nz. Ministry of Health. Archived from the original on 14 September 2017. Retrieved 14 September 2017.
- ↑ "Impetigo". Healthline. Archived from the original on 7 October 2016. Retrieved 7 October 2016.
- ↑ Tamparo, Carol; Lewis, Marcia (2011). Diseases of the Human Body. Philadelphia, PA: F.A. Davis Company. p. 194. ISBN 9780803625051.
- ↑ "ISDH: Impetigo". state.in.us. Archived from the original on 11 December 2014. Retrieved 11 December 2014.
- ↑ "Impetigo: MedlinePlus Medical Encyclopedia". medlineplus.gov. Archived from the original on 2016-11-07.
- ↑ "Self-management - Impetigo - Mayo Clinic". www.mayoclinic.org. Archived from the original on 16 October 2016. Retrieved 7 October 2016.
- ↑ 23.0 23.1 23.2 Baddour, Larry. "Impetigo". UpToDate. Archived from the original on 2018-08-16. Retrieved 2018-08-15.
- ↑ Fleisher, Gary R.; Ludwig, Stephen (2010-01-01). Textbook of Pediatric Emergency Medicine. Lippincott Williams & Wilkins. p. 925. ISBN 9781605471594. Archived from the original on 2017-09-08.
- ↑ "Impetigo: antimicrobial prescribing - NICE guideline [NG153]". www.nice.org.uk. Archived from the original on 2020-08-07. Retrieved 2020-05-26.
- ↑ Mahase, Elisabeth (15 August 2019). "Doctors should treat impetigo with antiseptics not antibiotics, says NICE". BMJ. 366: l5162. doi:10.1136/bmj.l5162. ISSN 1756-1833. PMID 31416810. S2CID 201018620. Archived from the original on 15 August 2019. Retrieved 26 May 2020.
- ↑ 27.0 27.1 Bowen, Asha; Mahe, Antoine; Hay, Roderick; Andrews, Ross; Steer, Andrew; Tong, Steven; Carapetis, Jonathan (2015). "The Global Epidemiology of Impetigo: A Systematic Review of the Population Prevalence of Impetigo and Pyoderma". PLOS ONE. 10 (8): e0136789. Bibcode:2015PLoSO..1036789B. doi:10.1371/journal.pone.0136789. PMC 4552802. PMID 26317533.
- ↑ 28.0 28.1 Romani, Lucia; Steer, Andrew; Whitfeld, Margot; Kaldor, John (2015). "Prevalence of scabies and impetigo worldwide: a systematic review". The Lancet Infectious Diseases. 15 (8): 960–7. doi:10.1016/S1473-3099(15)00132-2. PMID 26088526.
- ↑ George, Ajay; Rubin, Greg (2003). "A systematic review and meta-analysis of treatments for impetigo". British Journal of General Practice. 53 (491): 480–7. PMC 1314624. PMID 12939895.
- ↑ "Impetigo". The British Medical Journal. 1 (4185): 448. 1941. doi:10.1136/bmj.1.4185.445-a. JSTOR 20319413. S2CID 214846855.
- ↑ The Barnhart Concise Dictionary of Etymology. Harper Collins. 1995. ISBN 978-0-06-270084-1.
- ↑ MacDonald RS (October 2004). "Treatment of impetigo: Paint it blue". BMJ. 329 (7472): 979. doi:10.1136/bmj.329.7472.979. PMC 524121. PMID 15499130.
External links
- Impetigo at Curlie
- Impetigo and Ecthyma at Merck Manual of Diagnosis and Therapy Professional Edition
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- Articles with hatnote templates targeting a nonexistent page
- All articles with unsourced statements
- Articles with unsourced statements from May 2020
- Articles with invalid date parameter in template
- Articles with Curlie links
- Bacterium-related cutaneous conditions
- Pediatrics
- RTT
- RTTEM