Tinea manuum
| Tinea manuum | |
|---|---|
| Other names: Tinea manus[1] | |
 | |
| Tinea manuum hand | |
| Specialty | Dermatology, infectious diseases |
| Symptoms | Diffuse scaling, itch and prominent creases on palms[2] |
| Complications | Secondary bacterial infection[3] |
| Causes | Trichophyton rubrum[2] |
| Risk factors | Diabetes, high blood pressure, weak immune system, humid surroundings, excessive sweating, recurrent hand trauma and cracks, pet owners, farmworkers.[3] |
| Diagnostic method | Visualization, direct microscopy, culture[3] |
| Treatment | Topical or oral antifungals[3] |
| Medication | Terbinafine, itraconazole, clotrimazole, fluconazole, ketoconazole[3] |
| Frequency | Worldwide[3] |
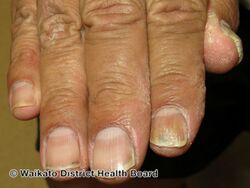
Tinea manuum is a type of fungal infection of the skin of the hand.[1][2] It is mostly a type of dermatophytosis, often part of two feet-one hand syndrome.[2] There is diffuse scaling on the palms or back of usually one hand and the palmer creases appear more prominent.[2] When both hands are affected, the rash looks different on each hand, with palmer creases appearing whitish if the infection has been present for a long time.[4] It can be itchy and look slightly raised.[4] Nails may also be affected.[4]
The most common cause is Trichophyton rubrum.[2] The infection can result from touching another area of the body with a fungal infection such as athletes foot or fungal infection of groin, contact with an infected person or animal, or from contact with soil or contaminated towels.[4] Risk factors include diabetes, high blood pressure, weak immune system, humid surroundings, excessive sweating, recurrent hand trauma and cracks in feet.[3] Pet owners and farmworkers are also at higher risk.[4] Machine operators, mechanics, gas/electricity workers and people who work with chemicals have also been reported to be at greater risk.[5]
Diagnosis is by visualization, direct microscopy and culture.[3] Psoriasis of the palms, pompholyx and contact dermatitis may appear similar.[3] Treatment is usually with long-term topical antifungal medications.[4] If not resolving, terbinafine or itraconazole taken by mouth might be options.[4]
It occurs worldwide.[3] One large study revealed around 84% of tinea manuum was associated with athletes foot, of which 80% admitted scratching their feet, and 60% were male,[5]
Signs and symptoms
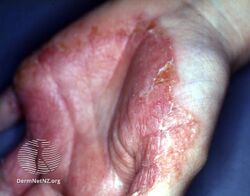
There is usually an itch, with generalised dry flaky thick skin of the palm of a hand.[3] Frequently, one hand is affected, but it can be in both.[3] If the back of the hand is affected, it may appear as reddish circles like in ringworm.[3] Sometimes there are no symptoms.[3] The feet may be affected as in two feet-one hand syndrome.[2]
-
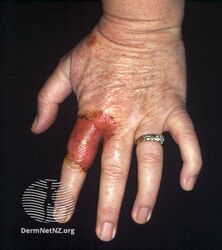
Tinea manuum finger
-
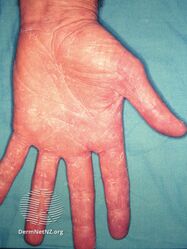
Tinea manuum palm
-
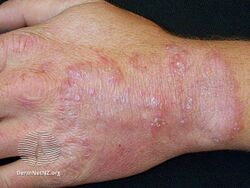
Tinea manuum back of hand
-
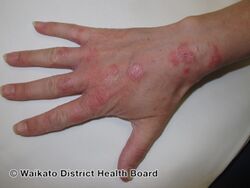
Longterm tinea manuum back of hand
-
Tinea manuum with infected nails
-
Tinea manuum due to Trichophyton erinacei
Cause and mechanism
The most common cause is Trichophyton rubrum.[2] Other causes include Trichophyton verrucosum (from cattle), Microsporum canis (from a cat or dog), Trichophyton erinacei (from a hedgehog), Trichophyton mentagrophytes, Epidermophyton floccosum, Trichophyton interdigitale, and more rarely Microsporum gypseum, Trichophyton eriotrephon, and Arhroderma benhamiae.[3][4]
Tinea manuum can result from touching another area of the body with a fungal infection such as athletes foot or tinea cruris, contact with an infected person or animal, or from contact with soil or contaminated towels.[4]
Risk factors
Diabetes, high blood pressure, weak immune system, humid surroundings, excessive sweating, recurrent hand trauma and cracks in feet are risk factors for tinea manuum.[3] Pet owners and farmworkers are also at higher risk.[3][4]
Diagnosis
Diagnosis is by visualization, direct microscopy and culture.[3]
Differential diagnosis
Psoriasis of the palms, pompholyx and contact dermatitis may appear similar.[3]
Treatment
Treatment is usually with long-term topical antifungal medications.[4] If not resolving, terbinafine or itraconazole by mouth might be options.[4] Other options include clotrimazole, fluconazole and ketoconazole.[3]
Prevention
Prevention is focussed on hygiene such as washing hands, avoiding scratching the feet or touching fungal toe infections.[3]
Epidemiology
Tinea manuum is most common in young adult males.[3] Dermatophyte infections occur in up to a quarter of the world's population, of which the hands and feet are most commonly involved.[3] It occurs worldwide.[3] One large study revealed around 84% of tinea manuum was associated with athletes foot, of which 80% admitted scratching their feet, and 60% were male, [5]
See also
References
- ↑ 1.0 1.1 Grossman, Sheila (2014). "61. Disorders of skin integrity and function". Porth's Pathophysiology: Concepts of Altered Health States (9th ed.). Lippincott Williams & Wilkins. p. 1545. ISBN 978-1-4511-4600-4. Archived from the original on 2023-04-19. Retrieved 2023-04-19.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 Johnstone, Ronald B. (2017). "25. Mycoses and Algal infections". Weedon's Skin Pathology Essentials (2nd ed.). Elsevier. p. 441. ISBN 978-0-7020-6830-0. Archived from the original on 2021-05-25. Retrieved 2021-05-25.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 3.14 3.15 3.16 3.17 3.18 3.19 3.20 3.21 3.22 3.23 Chamorro, Monica J.; House, Steven A. (10 August 2020). "Tinea Manuum". StatPearls. StatPearls Publishing. PMID 32644474. Archived from the original on 29 August 2021. Retrieved 15 October 2021.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 "Tinea manuum". dermnetnz.org. Archived from the original on 13 August 2021. Retrieved 27 September 2021.
- ↑ 5.0 5.1 5.2 McFadden, John; Puangpet, Pailin; Pongpairoj, Korbkarn; Thaiwat, Supitchaya; Lee, Shan Xian (2020). "8. Elimination or inclusion of non-allergic skin diseases". Common Contact Allergens: A Practical Guide to Detecting Contact Dermatitis. Hoboken: John Wiley & Sons. p. 104. ISBN 978-1-119-40571-9. Archived from the original on 2021-09-27. Retrieved 2021-09-27.
External links
| Classification |
|---|