Pemphigoid gestationis
| Pemphigoid gestationis | |
|---|---|
| Other names: Gestational pemphigoid, herpes gestationis[1] | |
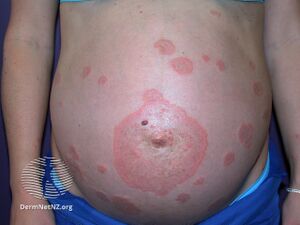 | |
| Pemphigoid gestationis | |
| Specialty | Dermatology. obstetrics |
| Symptoms | Blisters, itch, hives[1] |
| Complications | Baby: Premature delivery, blisters and hives,[1] bacterial infection[2] Mother: Grave's disease[1] |
| Usual onset | Mid pregnancy to shortly after birth[1] |
| Duration | Around 6-months[1] |
| Causes | Autoimmune[1] |
| Risk factors | Pregnancy, molar pregnancy, choriocarcinoma, birth control pill[1] |
| Diagnostic method | Appearance, skin biopsy with immunofluorescence[1] |
| Differential diagnosis | Pruritic urticarial papules and plaques of pregnancy, erythema multiforme, drug reactions, scabies[1] |
| Treatment | Corticosteroid applied to the skin or by mouth[1] |
| Medication | Prednisolone 40mg/day by mouth[1] |
| Frequency | 1 in 20,000 to 50,000 pregnancies[1] |
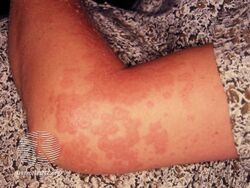
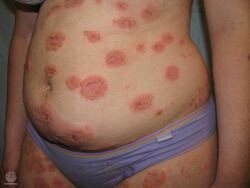
Pemphigoid gestationis (PG), also known as gestational pemphigoid, is an autoimmune variant of the skin disease bullous pemphigoid, that first appears in pregnancy.[3] Symptoms include blisters, small bumps, hives, and intense itching.[1] It usually starting around the belly button before spreading to the chest and limbs; with the head, face, and mouth being spared.[1][4] Onset is usually in mid-pregnancy to shortly after delivery.[1][5]
It is caused by antibodies against the mother's own skin, resulting in skin layers splitting and forming blisters.[4] It is possibly triggered by some placenta cells entering the mother's blood.[4] Risks include molar pregnancy and choriocarcinoma.[1] It does not spread between people and does not run in families.[4] It typically lasts six months and can reoccur in future pregnancies, menstrual periods, and from birth control pill.[1] In some people, it persists long-term.[1] Diagnosis is based on progression of symptoms, blood tests, and skin biopsy with immunofluorescence.[6][5] It can resemble pruritic urticarial papules and plaques of pregnancy (PUPP), erythema multiforme, drug reactions and blistering scabies.[1]
Treatment is generally with corticosteroids, either applied to the skin or taking prednisolone 40mg/day by mouth.[1] Other medicines that have been tried include pyridoxine, and tetracycline with nicotinamide.[1] Complications can include premature delivery of a small baby; or a baby born with blisters and hives, which generally resolves within six weeks.[4] The blisters can subsequently become infected with bacteria.[2] Around 10% of affected women develop Grave's disease.[1]
Pemphigoid gestationis affects around 1 in 20,000 to 50,000 pregnancies.[1] The condition was first described by London physician John Laws Milton in 1872.[7] It was originally called herpes gestationis because of the blistering appearance, although it is not associated with the herpes virus.[4]
Signs and symptoms
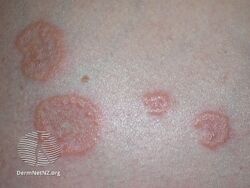
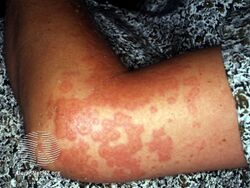
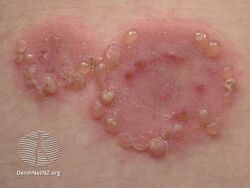
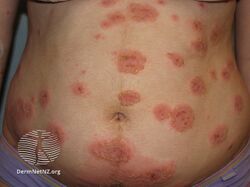
It presents with tense blisters, small bumps, hives and intense itching, usually starting around the belly button before spreading to chest and limbs in mid-pregnancy or shortly after delivery.[1] The head, face and mouth are not usually affected.[4]
-
Pemphigoid gestationis
-
Pemphigoid gestationis
-
Pemphigoid gestationis
-
Pemphigoid gestationis
-
Pemphigoid gestationis
-
Pemphigoid gestationis
-
Pemphigoid gestationis
Complications
In some people, it persists long-term.[1] It is associated with premature delivery of a small baby, a few who may be born with blisters and urticaria, which generally resolves within six weeks.[4] It does not spread from one person to another, and does not run in families.[4] Around 10% of affected people develop Grave's disease.[1]
Causes
Pemphigoid gestationis is an autoimmune variant of the skin disease bullous pemphigoid, and first appears in pregnancy.[3]
Circulating complement-fixing IgG antibodies attach to the lamina lucida resulting in the skin layers splitting and forming blisters, possibly triggered by some placenta cells entering into the mother's blood.[1] The triggering antigen, transmembrane collagen XVII, is part of the baby's membrane cells that encourage the movement of placental cytotrophoblastic cells.[1] The disease appears to be triggered by female hormones.[1] It can recur in subsequent pregnancies, menstrual periods and oral contraceptive pill.[1] A molar pregnancy and choriocarcinoma can provoke it.[1]
Diagnosis

Diagnosis is by its appearance and behaviour, blood test, biopsy and immunofluorescence.[6]
Differential diagnosis
Early in the disease, PG may appear similar to several other skin diseases.[4] Conditions that may appear similar include pruritic urticarial papules and plaques of pregnancy (PUPPP), erythema multiforme, drug reactions and blistering scabies.[1]
Treatment
The main aim of treatment is to relieve the itch, prevent further blistering, and treat any overlying infection.[4] PG is generally managed with the use of corticosteroids; prednisolone 40mg/day reducing to the lowest dose required to ease symptoms.[1] Milder cases may be managed with applying steroid creams to the skin.[1]
After the baby is born, if necessary, a more extensive range of immunosuppressive treatment may be administered for those unresponsive to corticosteroid treatments; pyridoxine, tetracycline with nicotinamide, cyclophosphamide, dapsone, rituximab, methotrexate, or intravenous immunoglobulin.[1]
Epidemiology
It is rare.[1] Around 1 in 20,000 to 50,000 pregnancies are affected.[1]
History
It was originally called herpes gestationis because of the blistering appearance, although it is not associated with the herpes virus.[4]
See also
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 1.19 1.20 1.21 1.22 1.23 1.24 1.25 1.26 1.27 1.28 1.29 1.30 1.31 1.32 1.33 1.34 1.35 1.36 1.37 James, William D.; Elston, Dirk; Treat, James R.; Rosenbach, Misha A.; Neuhaus, Isaac (2020). "21. Chronic blistering dermatoses". Andrews' Diseases of the Skin: Clinical Dermatology (13th ed.). Edinburgh: Elsevier. pp. 464–465. ISBN 978-0-323-54753-6. Archived from the original on 2023-06-30. Retrieved 2023-05-15.
- ↑ 2.0 2.1 "Pemphigoid gestationis | DermNet NZ". dermnetnz.org. Archived from the original on 9 March 2022. Retrieved 23 March 2022.
- ↑ 3.0 3.1 Wakelin, Sarah H. (2020). "22. Dermatology". In Feather, Adam; Randall, David; Waterhouse, Mona (eds.). Kumar and Clark's Clinical Medicine (10th ed.). Elsevier. pp. 686–687. ISBN 978-0-7020-7870-5.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 "Pemphigoid (herpes) gestationis". www.BAD.org.uk. British Association of Dermatologists. November 2020. Archived from the original on 2 February 2020. Retrieved 21 March 2022.
- ↑ 5.0 5.1 Roth, MM (1 February 2011). "Pregnancy dermatoses: diagnosis, management, and controversies". American journal of clinical dermatology. 12 (1): 25–41. doi:10.2165/11532010-000000000-00000. PMID 21110524.
- ↑ 6.0 6.1 Johnstone, Ronald B. (2017). "6. Vesiculobullous reaction pattern". Weedon's Skin Pathology Essentials (2nd ed.). Elsevier. p. 123. ISBN 978-0-7020-6830-0. Archived from the original on 2021-05-25. Retrieved 2022-03-21.
- ↑ Murrell, Dédée F. (28 April 2011). AutoImmune Blistering Disease Part I, An Issue of Dermatologic Clinics. Elsevier Health Sciences. p. 447. ISBN 978-1-4557-1247-2. Archived from the original on 19 December 2023. Retrieved 16 December 2023.
External links
| Classification | |
|---|---|
| External resources |