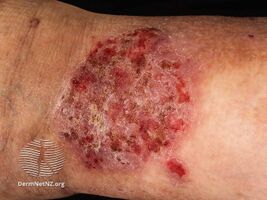
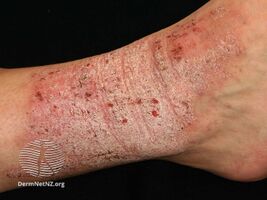
Lichen simplex chronicus
| Lichen simplex chronicus | |
|---|---|
| Other names: Neurodermatitis[1] | |
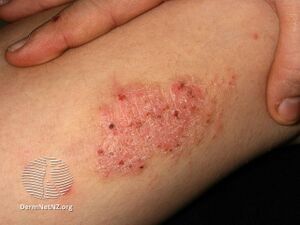 | |
| Symptoms | Thick leathery skin, exaggerated skin markings, small bumps, patches, scratch marks, scale[1] |
| Usual onset | Gradual[1] |
| Causes | Excessive rubbing and scratching[1] |
| Frequency | Females>males |
Lichen simplex chronicus (LSC) is thick, leathery skin with exaggerated skin markings caused by sudden itching and excessive rubbing and scratching.[1] It generally results in small bumps, patches, scratch marks, scale and prominence of the normal skin markings.[1] It typically affects the neck, scalp, upper eyelids, ears, palms, soles, ankles, wrists, genital areas and bottom.[1] It typically develops gradually and the scratching becomes a habit.[1]
Risk factors include psychological stressors, and atopy.[2]
Treatment includes persuading the person to stop scratching.[1] Applying a corticosteroid cream may help at the beginning.[1] It may be used in a tape form to provide occlusion.[1] Other options include applying doxepin, capsaicin, pimecrolimus or tacrolimus.[1] Injection of triamcinolone at 2.5-5mg/ml may help and injecting Botox may cure it.[1]
LSC is more common between ages 35 and 50 and is seen approximately twice as often in women compared to men.[2]
Signs and symptoms
People burdened with LSC report pruritus, followed by uncontrollable scratching of the same body region, excessively.[3] Most common sites of LSC are the sides of the neck, the scalp, ankles, vulva, pubis, scrotum, and extensor sides of the forearms.[2] However, due to the stigma associated with chronic scratching, some patients will not admit to chronic rubbing or abrasion. The skin may become thickened and hyperpigmented (lichenified) as a direct result of chronic excoriation.[2] Typically this period of increased scratching is associated with stressors.
-
Neurodermatitis
-
Neurodermatitis
Causes
This is a skin disorder characterized by a self-perpetuating scratch-itch cycle:[4]
- It may begin with something that rubs, irritates, or scratches the skin, such as clothing.
- This causes the person to rub or scratch the affected area. Constant scratching causes the skin to thicken.
- The thickened skin itches, causing more scratching, causing more thickening.
- Affected area may spread rapidly through the rest of the body.
Many hypothesize LSC has a psychosomatic origin.[2] Those predisposed to itch as a response to emotional tensions may be more susceptible to the itch-scratch cycle. It may also be associated with nervousness, anxiety, depression, and other psychological disorders.[5][6] Many people with LSC are aware of the scratching they do during the day, but they might not be aware of the scratching they do in their sleep.[3] LSC is also associated with atopy, or atopic dermatitis (eczema) and an increase of histamine levels.[3]
Diagnosis
LSC is typically diagnosed by careful observation and history taking.[2] It is easily recognized (see signs and symptoms, and gallery).[3] Biopsies are sometimes necessary to confirm the diagnosis and differentiate it from other similar appearing lesions.
Treatment
Treatment includes persuading the person to stop scratching.[1] Applying a corticosteroid cream may help at the beginning.[1] It may be used in a tape form to provide occlusion.[1] Other options include applying doxepin, capsaicin, pimecrolimus or tacrolimus.[1] Injection of triamcinolone at 2.5-5mg/ml may help and injecting Botox may cure it.[1] Night-time scratching can be reduced with sedatives and antihistamines.[3]
Gallery
See also
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 James, William D.; Elston, Dirk; Treat, James R.; Rosenbach, Misha A.; Neuhaus, Isaac (2020). "4. Pruritus and neurocutaneous dermatoses". Andrews' Diseases of the Skin: Clinical Dermatology (13th ed.). Elsevier. pp. 53–54. ISBN 978-0-323-54753-6. Archived from the original on 2023-04-29. Retrieved 2023-04-29.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 Lotti, Torello; Buggiani, Gionata; Prignano, Francesca (2008-01-01). "Prurigo nodularis and lichen simplex chronicus". Dermatologic Therapy. 21 (1): 42–46. doi:10.1111/j.1529-8019.2008.00168.x. ISSN 1529-8019. PMID 18318884.
- ↑ 3.0 3.1 3.2 3.3 3.4 Lynch, Peter J. (2004-01-01). "Lichen simplex chronicus (atopic/neurodermatitis) of the anogenital region". Dermatologic Therapy. 17 (1): 8–19. doi:10.1111/j.1396-0296.2004.04002.x. ISSN 1396-0296. PMID 14756886.
- ↑ Lee, Michael R.; Shumack, Stephen (2005-11-01). "Prurigo nodularis: a review". The Australasian Journal of Dermatology. 46 (4): 211–218, quiz 219–220. doi:10.1111/j.1440-0960.2005.00187.x. ISSN 0004-8380. PMID 16197418.
- ↑ Konuk, Numan; Koca, Rafet; Atik, Levent; Muhtar, Sennur; Atasoy, Nuray; Bostanci, Bora (2007-05-01). "Psychopathology, depression and dissociative experiences in patients with lichen simplex chronicus". General Hospital Psychiatry. 29 (3): 232–235. doi:10.1016/j.genhosppsych.2007.01.006. ISSN 0163-8343. PMID 17484940.
{{cite journal}}: CS1 maint: url-status (link) - ↑ Krishnan, Anjeli; Koo, John (2005-07-01). "Psyche, opioids, and itch: therapeutic consequences". Dermatologic Therapy. 18 (4): 314–322. doi:10.1111/j.1529-8019.2005.00038.x. ISSN 1396-0296. PMID 16297003.
External links
| Classification | |
|---|---|
| External resources |