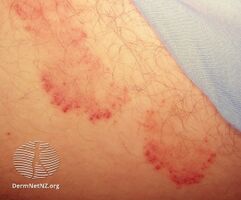
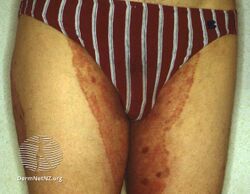
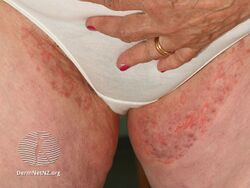
Tinea cruris
| Tinea cruris | |
|---|---|
| Other names: Ringworm of the groin,[1] eczema marginatum,[1] crotch itch, crotch rot, dhobi itch, gym itch, jock itch, jock rot, scrot rot[2][3] | |
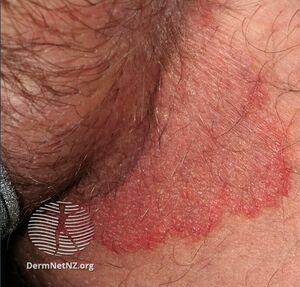 | |
| Case of tinea cruris[4] | |
| Specialty | Dermatology |
| Symptoms | Itchy and red groin rash[5] |
| Duration | Prolonged[1] |
| Causes | Dermatophytes[6] |
| Risk factors | Excessive sweating, tight fighting clothing, contact sports, diabetes, poverty[6] |
| Diagnostic method | Microscopy, culture[4] |
| Differential diagnosis | Candidal intertrigo, erythrasma, inverse psoriasis, seborrhoeic dermatitis[4] |
| Prevention | Treat other fungal infections, keep groin dry, avoid tight clothing, losing weight if obese[7] |
| Medication | Antifungal medication[1] |
| Frequency | Common[5] |
Tinea cruris, also known as jock itch, is a type of fungal infection of the skin of the groin region.[3][6] Symptoms typically include an itchy, red, and raised rash with a scaly and well-defined curved border.[1][5] Most commonly this occurs over the upper inner thighs.[5]
It is cause by a group of fungi known as dermatophytes.[6] Risk factors include excessive sweating, tight fighting clothing, contact sports, diabetes, and poverty.[6] It may spread to the groin from athletes foot, a fungal nail infection, or an infected towel or other clothing.[1][5] Diagnosis may be confirmed by microscopy or culturing of skin scrapings.[4] Similar conditions include candidal intertrigo, erythrasma, inverse psoriasis and seborrhoeic dermatitis.[4] It is a type of dermatophytosis.[6]
Treatment is typically with antifungal creams which are particularly effective if started soon after symptoms onset.[1] In more significant cases antifungals, such as terbinafine, by mouth may be used.[1] Steroid cream may speed symptom improvement.[4] Prevention of recurrences include treating other fungal infections and taking measures to avoid moisture build-up by keeping the groin dry, avoiding tight clothing, and losing weight if obese.[7]
Tinea cruris is common.[5] Males are affected more often than females and it occurs more commonly in hot-humid climates.[6] Children; however, are rarely affected.[5] Tinea was first described in 30 AD by Aulus Cornelius Celsus.[8]
Signs and symptoms
Typically, over the upper inner thighs, there is a red raised rash with a scaly well-defined border. There may be some blistering and weeping, and the rash can reach near to the anus.[9] The distribution is usually on both sides of the groin and the centre may be lighter in colour.[7] The rash may appear reddish, tan, or brown, with flaking, rippling, peeling, iridescence, or cracking skin.[10]
If the person is hairy, hair follicles can become inflamed resulting in some bumps (papules, nodules and pustules) within the plaque. The plaque may reach the scrotum in men and the labia majora and mons pubis in women. The penis is usually unaffected unless there is immunodeficiency or there has been use of steroids.[5]
Affected people usually experience intense itching in the groin which can extend to the anus.[9][5]
-
Tinea cruris in a female
-
Tinea cruris in a male
-
Tinea cruris
-
Tinea cruris
Causes

Tinea cruris is a common type of superficial fungal infection of the groin region, which is contagious.[1][5]
Tinea cruris is often associated with athletes foot and fungal nail infections.[1][5] Rubbing from clothing, excessive sweating, diabetes and obesity are risk factors.[7][11] It is contagious and can be transmitted person-to-person by skin-to-skin contact or by contact with contaminated sports clothing and sharing towels.[1][9]
The type of fungus involved may vary in different parts of the world; for example, Trichophyton rubrum and Epidermophyton floccosum are common in New Zealand.[4] Less commonly Trichophyton mentagrophytes and Trichophyton verrucosum are involved.[7] Trichophyton interdigitale has also been implicated.[1]
Diagnosis
Tests are usually not needed to make a diagnosis, but if required, may include microscopy and culture of skin scrapings, a KOH examination to check for fungus or skin biopsy.[9][4]
Differential diagnosis
The symptoms of tinea cruris may be similar to other causes of itch in the groin.[9] Its appearance may be similar to some other rashes that occur in skin folds including candidal intertrigo, erythrasma, inverse psoriasis and seborrhoeic dermatitis.[4]
Prevention
To prevent recurrences of tinea cruris, concurrent fungal infections such as athlete's foot need to be treated. Also advised are measures to avoid moisture build-up including keeping the groin region dry, avoiding tight clothing and losing weight if obese.[7] People with athletes foot or tinea cruris can prevent spread by not lending their towels to others.[1]
Treatment

Tinea cruris is treated with by applying antifungal medications of the allylamine or azole type to the groin region. Allylamines (naftifine and terbinafine) appear quicker but more expensive compared to azoles (clotrimazole, econazole, ketoconazole, oxiconazole, miconazole, sulconazole).[11] If the symptoms have been present for long or the condition worsens despite applying creams, terbinafine or itraconazole can be given by mouth.[1]
The benefits of the use of topical steroids in addition to an antifungal is unclear.[12] There might be a greater cure rate but no guidelines currently recommend their addition.[12] The effect of Whitfield's ointment is also unclear,[12] but when given, it is prescribed at half strength.[1]
Wearing cotton underwear and socks, in addition to keeping the groin dry and using antifungal powders are helpful.[13]
Prognosis
Tinea cruris is not life threatening and treatment is effective, particularly if the symptoms have not been present for long.[1] However, recurrence may occur. The intense itch may lead to lichenification and secondary bacterial infection. Irritant and allergic contact dermatitis may be caused by applied medications.[7]
Epidemiology
Tinea cruris is common in hot-humid climates and is the second most common clinical presentation for dermatophytosis.[7] It occurs predominantly but not exclusively in men. It is uncommon in children.[5]
Names
Other names include jock rot,[14] dhobi itch,[15] crotch itch,[16] scrot rot,[17] gym itch, ringworm of groin and eczema marginatum.[18]
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 Hay, Roderick J.; Morris-Jones, Rachel; Bleiker, Tanya O. (2016). "32. Fungal Infections". In Griffiths, Christopher; Barker, Jonathan; Bleiker, Tanya O.; Chalmers, Robert; Creamer, Daniel (eds.). Rook's Textbook of Dermatology, 4 Volume Set. John Wiley & Sons. p. 47. ISBN 978-1-118-44119-0. Archived from the original on 2021-08-29. Retrieved 2020-11-15.
- ↑ Rapini, R. P.; Bolognia, J. L.; Jorizzo, J. L. (2007). Dermatology. St. Louis: Mosby. ISBN 978-1-4160-2999-1.
- ↑ 3.0 3.1 James, William D.; Elston, Dirk; Treat, James R.; Rosenbach, Misha A.; Neuhaus, Isaac (2020). "15. Diseases resulting from fungi and yeasts". Andrews' Diseases of the Skin: Clinical Dermatology (13th ed.). Elsevier. p. 297. ISBN 978-0-323-54753-6. Archived from the original on 2023-04-19. Retrieved 2023-04-19.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 4.8 "Tinea cruris | DermNet NZ". dermnetnz.org. 2003. Archived from the original on 11 November 2020. Retrieved 15 November 2020.
- ↑ 5.00 5.01 5.02 5.03 5.04 5.05 5.06 5.07 5.08 5.09 5.10 5.11 Libby Edwards; Peter J. Lynch (2010). Genital Dermatology Atlas. Lippincott Williams & Wilkins. p. 67. ISBN 978-1-60831-079-1. Archived from the original on 2021-08-29. Retrieved 2020-11-13.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 6.6 Pippin, MM; Madden, ML (January 2020). "Tinea Cruris". PMID 32119489.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ 7.0 7.1 7.2 7.3 7.4 7.5 7.6 7.7 Wiederkehr, Michael (11 September 2020). "Tinea Cruris". Medscape. Archived from the original on 23 July 2017. Retrieved 1 December 2020.
- ↑ Cox, Rebecca A. (1989). Immunology of the Fungal Diseases. CRC Press. p. PR5-IA1. ISBN 978-1-000-14184-9. Archived from the original on 2021-08-29. Retrieved 2020-12-01.
- ↑ 9.0 9.1 9.2 9.3 9.4 Lehrer, Michael (16 April 2019). "Jock itch". MedlinePlus. NLM / NIH. Archived from the original on 9 June 2016.
- ↑ "Jock itch". NYU Langone Medical Center. Archived from the original on 2007-10-13.
- ↑ 11.0 11.1 Nadalo, Dana; Montoya, Cathy; Hunter-Smith, Dan (March 2006). "What is the best way to treat tinea cruris?". The Journal of Family Practice. 55 (3): 256–258. ISSN 0094-3509. PMID 16510062. Archived from the original on 2017-09-18. Retrieved 2020-11-14.
- ↑ 12.0 12.1 12.2 El-Gohary, M; van Zuuren, EJ; Fedorowicz, Z; Burgess, H; Doney, L; Stuart, B; Moore, M; Little, P (Aug 4, 2014). "Topical antifungal treatments for tinea cruris and tinea corporis". The Cochrane Database of Systematic Reviews. 8 (8): CD009992. doi:10.1002/14651858.CD009992.pub2. PMID 25090020.
- ↑ Ellen F. Crain; Jeffrey C. Gershel (2010). Clinical Manual of Emergency Pediatrics. Cambridge University Press. p. 131. ISBN 978-1-139-49286-7. Archived from the original on 2021-08-29. Retrieved 2020-11-29.
- ↑ Paul Bedson (2005). The Complete Family Guide to Natural Healing. Penton Overseas, Inc. p. 71. ISBN 978-1-74121-597-7. Archived from the original on 2021-08-29. Retrieved 2020-11-14.
- ↑ Eric Partridge (2006). The New Partridge Dictionary of Slang and Unconventional English: A-I. Taylor & Francis. p. 580. ISBN 0-415-25937-1. Archived from the original on 2021-08-29. Retrieved 2020-11-14.
- ↑ Thomas C. Rosenthal; Mark E. Williams; Bruce J. Naughton (2006). Office Care Geriatrics. Lippincott Williams & Wilkins. p. 501. ISBN 0-7817-6196-4. Archived from the original on 2021-08-29. Retrieved 2020-12-01.
- ↑ Christian Jessen (2010). Can I Just Ask?. Hay House, Inc. p. 43. ISBN 978-1-84850-246-8. Archived from the original on 2021-08-29. Retrieved 2020-12-01.
- ↑ Reutter, Jason C. (2019). "56. Dermatophytosis". In Marisa R. Nucci (ed.). Diagnostic Pathology: Gynecological E-Book. Esther Oliva. Elsevier. p. 56. ISBN 978-0-323-54815-1. Archived from the original on 2021-08-29. Retrieved 2020-11-14.
External links
| Classification | |
|---|---|
| External resources |