Tinea faciei
| Tinea faciei | |
|---|---|
| Other names: Ringworm of the face[1] | |
 | |
| Tinea faciei | |
| Specialty | Dermatology, infectious diseases |
| Symptoms | Face: Red patches, small raised bumps,[2] weeping, crusting, fragile hairs.[3] |
| Complications | Tinea incognita[4] |
| Causes | T. rubrum, T. mentagrophytes, T. tonsurans, M. gypseum, M.canis[5][1] |
| Diagnostic method | Appearance, skin scraping for microscopy and culture,[3] biopsy[2] |
| Differential diagnosis | Lupus erythematosus, impetigo, eczema, herpes zoster[4] |
| Treatment | Antifungals[3] |
| Medication |
|
| Frequency | Uncommon[1] |
Tinea faciei is a type of fungal infection of the skin of the non-bearded part of the face.[6] It generally appears as a photosensitive, painless, red rash with small bumps and a raised edge appearing to grow outwards, usually over eyebrows or one side of the face.[2] It may feel wet or have some crusting, and overlying hairs may fall out easily.[3] There may be a mild itch or burning sensation.[6]
Tinea faciei can be caused by spread of fungal infections of the feet and nails, from pets such as cats and dogs, and from farm animals.[1] Causative organisms include T. rubrum, T. mentagrophytes, T. tonsurans, M. gypseum and M.canis.[5] Often misdiagnosed as an inflammatory condition, for which corticosteroids are applied, tinea faciei may be complicated by tinea incognita.[4]
Diagnosis is by the appearance of the rash and confirmed by taking a skin scraping for microscopy and culture,[3] or biopsy.[2] Differential diagnoses include lupus erythematosus, impetigo, eczema, herpes zoster,[4] seborrhoeic dermatitis, psoriasis, rosacea, actinic keratoses, perioral dermatitis and polymorphous light eruption.[1] Treatment is with topical antifungal medication; terbinafine, clotrimazole, miconazole and ketoconazole.[3] If the condition does not respond to topical treatment or is extensive, then oral terbinafine or itraconazole can be taken.[1]
The condition is uncommon.[1]
Signs and symptoms
It generally appears as a photosensitive painless red rash on the face, followed by patches of small, raised bumps.[2] It is considered distinct from fungal infection of the beard area.[3] The rash may weep or crust, and hairs may fall out easily. It is usually painless.[3]
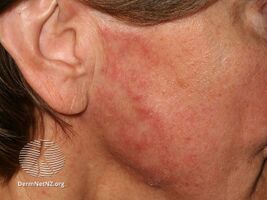
-
Tinea faciei: redness and small bumps
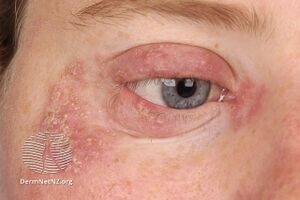
-
Tinea faciei: redness and scale
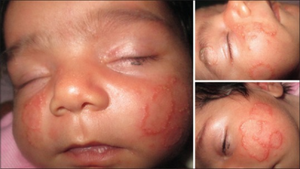
-
Tinea faciei on both cheeks
Causes
It is usually caused by T. rubrum, T. mentagrophytes, M. gypseum, T. tonsurans.[5]
Diagnosis
Diagnosis is by the appearance of the rash and confirmed by taking a skin scraping for microscopy.[3]
Treatment

Treatment is usually with topical antifungal medication such as terbinafine cream twice daily for 2 weeks, or miconazole twice daily for 2-4 weeks.[3][2] Extensive infection may require treatment with oral terbinafine for 2 weeks.[3]
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 "Tinea faciei". dermnetnz.org. Archived from the original on 13 August 2021. Retrieved 18 September 2021.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 James, William D.; Elston, Dirk; Treat, James R.; Rosenbach, Misha A.; Neuhaus, Isaac (2020). "15. Diseases resulting from fungi and yeasts". Andrews' Diseases of the Skin: Clinical Dermatology (13th ed.). Edinburgh: Elsevier. p. 295. ISBN 978-0-323-54753-6. Archived from the original on 2021-08-29. Retrieved 2021-05-21.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 "Tinea faciei (face) and barbae (beard)". www.pcds.org.uk. Archived from the original on 5 May 2020. Retrieved 21 May 2021.
- ↑ 4.0 4.1 4.2 4.3 Ginter-Hanselmayer, Gabriele; Nenoff, Pietro (2018). Presterl, Elisabeth (ed.). Clinically Relevant Mycoses: A Practical Approach. Springer. pp. 149–150. ISBN 978-3-319-92300-0. Archived from the original on 2021-09-22. Retrieved 2021-09-18.
- ↑ 5.0 5.1 5.2 Johnstone, Ronald B. (2017). "25. Mycoses and Algal infections". Weedon's Skin Pathology Essentials (2nd ed.). Elsevier. p. 441. ISBN 978-0-7020-6830-0. Archived from the original on 2021-05-25. Retrieved 2021-05-25.
- ↑ 6.0 6.1 Schachtel, April; DeNiro, Katherine L. (2021). "22. Superficial dermatophyte infections of the skin". In Jong, Elaine C.; Stevens, Dennis L. (eds.). Netter's Infectious Diseases (Second ed.). Philadelphia: Elsevier. pp. 101–102. ISBN 978-0-323-71159-3. Archived from the original on 2023-04-19. Retrieved 2023-04-19.
External links
| Classification |
|---|