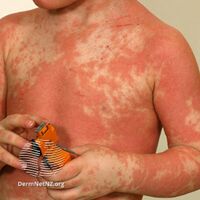
Pityriasis rubra pilaris
| Pityriasis rubra pilaris | |
|---|---|
| Other names: Devergie's disease,[1] lichen ruber acuminatus,[1] and lichen ruber pilaris[1] | |
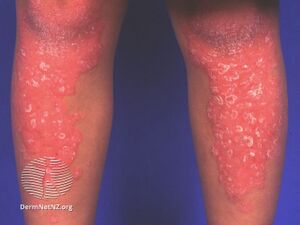 | |
| Pityriasis rubra pilaris | |
| Specialty | Dermatology |
| Symptoms | Tiny horny bumps that feel like nutmeg grater, pink-to-orange/red scaly well defined plaques merging to cause widespread redness with islands of sparing,[2] thickened nails, thinning hair[3] |
| Usual onset | Child or adult[3] |
| Duration | Varies[3] |
| Types | I-VI[3] |
| Causes | Mostly unknown, some hereditary[3] |
| Treatment | Applying moisturisers, Retinoids by mouth, and/or immunosuppressants[3] |
| Prognosis | Varies, but normalise expectancy[3] |
| Frequency | Rare,[3] males=females[4] |
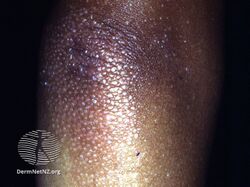
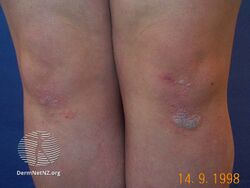
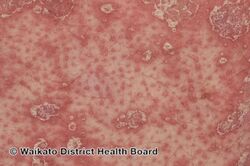
Pityriasis rubra pilaris refers to a group of longterm skin conditions characterized by localised or widespread reddish orange, scaling plaques and horny pinpoint bumps, generally divided into juvenile onset and adult onset.[3] The bumps may feel like a nutmeg grater, and the plaques typically merge to form widespread redness with islands of sparing.[2] There may be uncomfortable itching, thickening of the skin on the feet and hands, thickened bumps around hair follicles, thickened nails and thinning hair.[3] There is currently no known cause or cure for PRP.[3]
Males and females are affected equally.[4] It was first described by Marie-Guillaume-Alphonse Devergie in 1856.[5]
Signs and symptoms
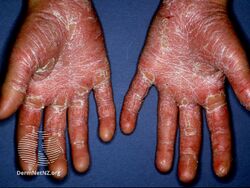
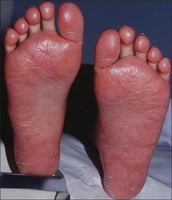
The presentation includes scaling of the skin/scalp, thickening of the skin on palms and shedding of the nails.[3] For some, early symptoms may also include generalized swelling of the legs, feet and other parts of the body. PRP has a varied clinical progression and a varied rate of improvement.
-
Pityriasis rubra pilaris
-
Pityriasis rubra pilaris
-
Pityriasis rubra pilaris
-
Pityriasis rubra pilaris
-
Pityriasis rubra pilaris
-
Keratodermic sandals
Diagnosis
Classification
W.A.D. Griffiths, from Great Britain, classified six forms of PRP in the early 1980s.[6] At this time, the causes of PRP are still unknown and symptoms can be difficult to diagnose. Frequently, more than one medical professional will be consulted before an accurate PRP diagnosis is made.[citation needed]
Dermatologists have identified both an acquired form and an inherited form (familial) of PRP and have described them in medical journals. The acquired form usually shows a spontaneous or gradual remission of symptoms within several years although long-term symptoms may continue for years. The inherited form starts early in childhood with persistent long-term symptoms into adulthood.[citation needed]
Although most people who develop PRP are over age 50, individuals of any age, race, and nationality can be affected. Women and men seem to be equally affected.[7]
Treatment
Treatment with emollients is used to relieve symptoms of cracking and dryness. Application of lubricants under plastic occlusion before bedtime appears to aid removal of scales on hands and feet. Other topical options include: topical corticosteroids alone, or combined with keratolytics, such as urea and vitamin D3 analogues. The most effective therapy is long term use of oral retinoids, such as acitretin and isotretinoin. Other effective systemic approaches include: methotrexate, cyclosporin and corticosteroids. There are also reports that the monoclonal Ab ustekinumab (blocks IL-23/ IL-12) may be effective.
See also
Footnotes
- ↑ 1.0 1.1 1.2 Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. ISBN 978-1-4160-2999-1.
- ↑ 2.0 2.1 Allen, Herbert B. (2010). "1. Papulosquamous diseases". Dermatology Terminology. Philadelphia: Springer. pp. 13–14. ISBN 978-1-84882-839-1. Archived from the original on 2021-09-23. Retrieved 2022-04-23.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 "Pityriasis rubra pilaris | Genetic and Rare Diseases Information Center (GARD) – an NCATS Program". rarediseases.info.nih.gov. Archived from the original on 19 April 2021. Retrieved 14 May 2021.
- ↑ 4.0 4.1 Lim, Henry W. (2020). "409. Eczemas, photodermatoses, papulomatoses, papulosquamous (including fungal) diseases, and figurate erythema: Pityriasis rubra pilaris". In Goldman, Lee; Schafer, Andrew I. (eds.). Goldman-Cecil Medicine. Vol. 2 (26th ed.). Philadelphia: Elsevier. pp. 2616–2617. ISBN 978-0-323-53266-2. Archived from the original on 2023-04-28. Retrieved 2023-04-28.
- ↑ M. G. A. Devergie and the eponymous named Devergie's disease at Who Named It?
- ↑ "Pityriasis rubra pilaris". DermNZ (New Zealand Dermatological Society). 26 December 2006. Archived from the original on 2007-05-02. Retrieved 2007-05-08. - describes the various forms
- ↑ Allison DS, El-Azhary RA, Calobrisi SD, Dicken CH (2002). "Pityriasis rubra pilaris in children". Journal of the American Academy of Dermatology. 47 (3): 386–389. doi:10.1067/mjd.2002.124619. PMID 12196748.
Further reading
- Dr. Griffith (June 1998). "Pityriasis rubra pilaris". In Champion R.H.; Burton J.L.; Burns D.A.; Breathnach S.M. (eds.). Textbook of Dermatology. Vol. 2 (6th ed.). pp. 1539–1545. ISBN 0-632-05064-0.
External links
| Classification | |
|---|---|
| External resources |