Bevacizumab
| Monoclonal antibody | |
|---|---|
| Type | Whole antibody |
| Source | Humanized (from mouse) |
| Target | VEGF-A |
| Names | |
| Pronunciation | /ˌbɛvəˈsɪzjʊmæb/[1] |
| Trade names | Avastin, Zirabev, Mvasi, others[2] |
| Other names | bevacizumab-awwb,[3] bevacizumab-bvzr[4] |
| Clinical data | |
| Drug class | Anti–VEGF[5] |
| Main uses | Cancer, age-related macular degeneration[5][6] |
| Side effects | Nose bleeds, headache, high blood pressure, rash[5] |
| Pregnancy category | |
| Routes of use | intravenous, intravitreal |
| Defined daily dose | not established[8] |
| External links | |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a607001 |
| Legal | |
| License data |
|
| Legal status | |
| Pharmacokinetics | |
| Bioavailability | 100% (IV only) |
| Elimination half-life | 20 days (range: 11–50 days) |
| Chemical and physical data | |
| Formula | C6638H10160N1720O2108S44 |
| Molar mass | 149198.87 g·mol−1 |
Bevacizumab, sold under the brand name Avastin, is a medication used to treat a number of types of cancers and a specific eye disease.[5][6] For cancer it is given by slow injection into a vein and used for colon cancer, lung cancer, glioblastoma, and renal-cell carcinoma.[5][6] For age-related macular degeneration it is given by injection into the eye.[5]
Common side effects when used for cancer include nose bleeds, headache, high blood pressure, and rash.[5] Other severe side effects include gastrointestinal perforation, bleeding, allergic reactions, blood clots, and an increased risk of infection.[5] When used for eye disease side effects can include vision loss and retinal detachment.[5] Bevacizumab is a monoclonal antibody that functions as an angiogenesis inhibitor.[5] It works by slowing the growth of new blood vessels by inhibiting vascular endothelial growth factor A (VEGF-A), in other words anti–VEGF therapy.[5]
Bevacizumab was approved for medical use in the United States in 2004.[5] It is on the World Health Organization's List of Essential Medicines.[9] It is listed for its use in treating eye disease.[9] The wholesale cost in the developing world is about US$638.54 per vial.[10] This dose in the United Kingdom cost the NHS about £243 in 2015.[11]
Medical uses
Colorectal cancer
Bevacizumab was approved in the United States in February 2004, for use in metastatic colorectal cancer when used with standard chemotherapy treatment (as first-line treatment) and with 5-fluorouracil-based therapy for second-line metastatic colorectal cancer.[citation needed]
It was approved by the European Medicines Agency (EMA) in January 2005, for use in colorectal cancer.[12][13]
Bevacizumab has also been examined as an add on to other chemotherapy drugs in people with non-metastatic colon cancer. The data from two large randomized studies showed no benefit in preventing the cancer from returning and a potential to cause harm in this setting.[14]
Lung cancer
In 2006, the U.S. Food and Drug Administration (FDA) approved bevacizumab for use in first-line advanced nonsquamous non-small cell lung cancer in combination with carboplatin/paclitaxel chemotherapy. The approval was based on the pivotal study E4599 (conducted by the Eastern Cooperative Oncology Group), which demonstrated a two-month improvement in overall survival in patients treated with bevacizumab (Sandler, et al. NEJM 2004). A preplanned analysis of histology in E4599 demonstrated a four-month median survival benefit with bevacizumab for people with adenocarcinoma (Sandler, et al. JTO 2010); adenocarcinoma represents approximately 85% of all non-squamous cell carcinomas of the lung.
A subsequent European clinical trial, AVAiL, was first reported in 2009 and confirmed the significant improvement in progression-free survival shown in E4599 (Reck, et al. Ann. Oncol. 2010). An overall survival benefit was not demonstrated in patients treated with bevacizumab; however, this may be due to the more limited use of bevacizumab as maintenance treatment in AVAiL versus E4599 (this differential effect is also apparent in the European vs US trials of bevacizumab in colorectal cancer: Tyagi and Grothey, Clin Colorectal Cancer, 2006). As an anti-angiogenic agent, there is no mechanistic rationale for stopping bevacizumab before disease progression. Stated another way, the survival benefits achieved with bevacizumab can only be expected when used in accordance with the clinical evidence: continued until disease progression or treatment-limiting side effects.
Another large European-based clinical trial with bevacizumab in lung cancer, AVAPERL, was reported in October 2011 (Barlesi, et al. ECCM 2011). First-line patients were treated with bevacizumab plus cisplatin/pemetrexed for four cycles, and then randomized to receive maintenance treatment with either bevacizumab/pemetrexed or bevacizumab alone until disease progression. Maintenance treatment with bevacizumab/pemetrexed demonstrated a 50% reduction in risk of progression vs bevacizumab alone (median PFS: 10.2 vs 6.6 months). Maintenance treatment with bevacizumab/pemetrexed did not confer a significant increase in overall survival vs bevacizumab alone on follow up analysis.[15]
The National Comprehensive Cancer Network recommends bevacizumab as standard first-line treatment in combination with any platinum-based chemotherapy, followed by maintenance bevacizumab until disease progression.[medical citation needed] Higher doses are usually given with carboplatin-based chemotherapy, whereas the lower dose is usually given with cisplatin-based chemotherapy.[medical citation needed]
Breast cancer
In December 2010, the U.S. Food and Drug Administration (FDA) notified its intention to remove the breast cancer indication (approved in 2008) from bevacizumab, saying that it had not been shown to be safe and effective in breast cancer patients.[16][17] The combined data from four different clinical trials showed that bevacizumab neither prolonged overall survival nor slowed disease progression sufficiently to outweigh the risk it presents to patients. This only prevented Genentech from marketing bevacizumab for breast cancer. Doctors are free to prescribe bevacizumab off label, although insurance companies are less likely to approve off-label treatments.[18][19] In June 2011, an FDA panel unanimously rejected an appeal by Roche. A panel of cancer experts ruled for a second time that Avastin should no longer be used in breast cancer patients, clearing the way for the U.S. government to remove its endorsement from the drug. The June 2011 meeting of the FDA's oncologic drug advisory committee was the last step in an appeal by the drug's maker. The committee concluded that breast cancer clinical studies of patients taking Avastin have shown no advantage in survival rates, no improvement in quality of life, and significant side effects.[20]
On October 11, 2011, the U.S. Food and Drug Administration (FDA) announced that the agency was revoking the agency's approval of the breast cancer indication for bevacizumab after concluding that the drug had not been shown to be safe and effective for that use.[citation needed]
Renal cancers
In certain renal (kidney) cancers, bevacizumab improves the progression free survival time but not survival time. In 2009, the FDA approved bevacizumab for use in metastatic renal cell cancer (a form of kidney cancer).[21][22] following earlier reports of activity[23] EU approval was granted in 2007.[24]
Brain cancers
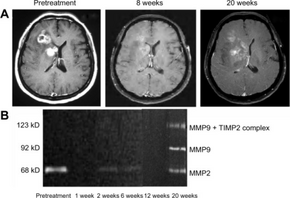
Bevacizumab slows tumor growth but does not affect overall survival in people with glioblastoma multiforme.[25] The FDA granted accelerated approval for the treatment of recurrent glioblastoma multiforme in May 2009.[26][27] A 2018 Cochrane review deemed there to not be good evidence for its use in recurrences either.[25]
Eye disease
Many diseases of the eye, such as age-related macular degeneration (AMD) and diabetic retinopathy, damage the retina and cause blindness when blood vessels around the retina grow abnormally and leak fluid, causing the layers of the retina to separate. This abnormal growth is caused by VEGF, so bevacizumab has been successfully used to inhibit VEGF and slow this growth.[medical citation needed]
Bevacizumab has recently[when?] been used by ophthalmologists in an off-label use as an intravitreal agent in the treatment of proliferative (neovascular) eye diseases, particularly for choroidal neovascular membrane (CNV) in AMD. Although not currently[when?] approved by the FDA for such use, the injection of 1.25–2.5 mg of bevacizumab into the vitreous cavity has been performed without significant intraocular toxicity.[28] Many retina specialists have noted impressive results in the setting of CNV, proliferative diabetic retinopathy, neovascular glaucoma, diabetic macular edema, retinopathy of prematurity[29] and macular edema secondary to retinal vein occlusions.[medical citation needed].
Some reviews conclude that similar results are obtained using either bevacizumab or ranibizumab.[30][31] Others found a higher rate of adverse events[32][33] such as thromboembolism with bevacizumab or were unable to reach firm conclusions based on the limited data available.[34]
Ovarian cancer
In 2018, the U.S. Food and Drug Administration (FDA) approved bevacizumab in combination with chemotherapy for stage III or IV of ovarian cancer after initial surgical operation, followed by single-agent bevacizumab. The approval was based on a study of the addition of bevacizumab to carboplatin and paclitaxel.[35] Progression-free survival was increased to 18 months from 13 months.[35]
Administration
Bevacizumab is usually given intravenously every 14 days. In colon cancer, it is given in combination with the chemotherapy drug 5-FU (5-fluorouracil), leucovorin, and oxaliplatin or irinotecan.[medical citation needed] For treatment of eye diseases it is injected intravitreously.
Dosage
The defined daily dose is not established.[8]
Side effects
Bevacizumab inhibits the growth of blood vessels, which is part of the body's normal healing and maintenance. The body grows new blood vessels in wound healing, and as collateral circulation around blocked or atherosclerotic blood vessels. One concern is that bevacizumab will interfere with these normal processes, and worsen conditions like coronary artery disease or peripheral artery disease.[36]
The main side effects are hypertension and heightened risk of bleeding. Bowel perforation has been reported.[37] Fatigue and infection are also common.[38] In advanced lung cancer, less than half of patients qualify for treatment.[39][40] Nasal septum perforation and renal thrombotic microangiopathy have been reported.[41] In December 2010, the FDA warned of the risk of developing perforations in the body, including in the nose, stomach, and intestines.
In 2013, Hoffmann-La Roche announced that the drug was associated with 52 cases of necrotizing fasciitis from 1997 to 2012, of which 17 patients died.[42] About 2/3 of cases involved patients with colorectal cancer, or patients with gastrointestinal perforations or fistulas.
These effects are largely avoided in ophthalmological use since the drug is introduced directly into the eye thus minimizing any effects on the rest of the body.[citation needed]
Neurological adverse events include reversible posterior encephalopathy syndrome. Ischemic and hemorrhagic strokes are also possible.[43]
Protein in the urine occurs in approximately 20% of people. This does not require permanent discontinuation of the drug. Nonetheless the presence of nephrotic syndrome necessitates permanent discontinue of bevacizumab.[44]
Mechanism of action
Bevacizumab is a recombinant humanized monoclonal antibody that blocks angiogenesis by inhibiting vascular endothelial growth factor A (VEGF-A).[45] VEGF-A is a growth factor protein that stimulates angiogenesis in a variety of diseases, especially in cancer. Bevacizumab was the first available angiogenesis inhibitor in the United States.[46]
Chemistry
Bevacizumab was originally derived from a mouse monoclonal antibody generated from mice immunized with the 165-residue- form of recombinant human vascular endothelial growth factor. It was humanized by retaining the binding region and replacing the rest with a human full light chain and a human truncated IgG1 heavy chain, with some other substitutions. The resulting plasmid was transfected into Chinese hamster ovary cells which are grown in industrial fermentation systems.[12]: 4
History
Bevacizumab is a recombinant humanized monoclonal antibody and in 2004, it became the first clinically used angiogenesis inhibitor.[47] Its development was based on the discovery of human vascular endothelial growth factor (VEGF), a protein that stimulated blood vessel growth, in the laboratory of Genentech scientist Napoleone Ferrara.[48][49][50] Ferrara later demonstrated that antibodies against VEGF inhibit tumor growth in mice.[51] His work validated the hypothesis of Judah Folkman, proposed in 1971, that stopping angiogenesis might be useful in controlling cancer growth.[50]
Approval
It received its first approval in the United States in 2004, for combination use with standard chemotherapy for metastatic colon cancer.[44] It has since been approved for use in certain lung cancers, renal cancers, ovarian cancers, and glioblastoma multiforme of the brain.[medical citation needed]
In 2008, bevacizumab was approved for breast cancer by the FDA, but the approval was revoked on 18 November 2011.[52][53][54] The approval for breast cancer was revoked because, although there was evidence that it slowed progression of metastatic breast cancer, there was no evidence that it extended life or improved quality of life, and it caused adverse effects including severe high blood pressure and hemorrhaging. In 2008, the FDA gave bevacizumab provisional approval for metastatic breast cancer, subject to further studies.
The FDA's advisory panel had recommended against approval.[55] In July 2010, after new studies failed to show a significant benefit, the FDA's advisory panel recommended against the indication for advanced breast cancer. Genentech requested a hearing, which was granted in June 2011. The FDA ruled to withdraw the breast cancer indication in November 2011. FDA approval is required for Genentech to market a drug for that indication. Doctors may sometimes prescribe it for that indication, although insurance companies are less likely to pay for it.[53]
The drug remains approved for breast cancer use in other countries including Australia.[56] It has been funded by the English NHS Cancer Drugs Fund but in January 2015 it was proposed to remove it from the approved list.[57]
Society and culture
Costs
In countries with national health care systems (such as the UK and Canada), many of those national health services have restricted bevacizumab on the basis of cost-benefit calculations; in the UK, for example, the National Institute for Health and Care Excellence has taken the position that bevacizumab should not be funded by the NHS because it costs nearly £21,000 per patient but only minimal benefit in many cancers.[58] In 2006, the Scottish Medicines Consortium recommended against the NHS funding Avastin for first-line treatment of metastatic carcinoma of the colon or rectum, due to estimated costs of £24,000 to £93,000 per quality-adjusted life year (QALY).[59]
The addition of bevacizumab to standard treatment can prolong the lives of lung cancer patients by several months, at a cost of $100,000 a year in the United States.[60] For colorectal cancer, Robert J. Mayer wrote in The New England Journal of Medicine that bevacizumab extended life by 4.7 months (20.3 months vs. 15.6 months) in the initial study, at a cost of $42,800 to $55,000.[61] Costs in other countries vary; in Canada it is reported to cost $40,000 CAD per year.[62]
In September 2018, claims from Bayer and Novartis Pharmaceuticals UK who argued that 12 clinical commissioning groups were acting illegally in using bevacizumab to treat people with wet age-related macular degeneration were rejected by the High Court of Justice.[63]
Specialty drug
On September 16, 2014, Genentech reclassified bevacizumab as a specialty drug which are only available through specialty pharmacies. "Specialty drugs usually fall under the FDA's Risk Evaluation and Mitigation Strategy (REMS) program, established for compounds like the testosterone... that may have unusual side effects; or for drugs that are unusually expensive."[64] This has caused concern to hospitals as the price increased.[64] According to IMS Health, the average price charged by hospitals for bevacizumab is approximately $9000 compared to approximately $2300 when administered in a doctor's office. As a result of the new distribution arrangement, many hospitals will no longer be eligible for the 51% discount to average wholesale price that was mandated by the Affordable Healthcare Act under the old distribution arrangement.[65]
Use for macular degeneration
When bevacizumab is used in the treatment of wet age-related macular degeneration (wet AMD), only tiny and relatively inexpensive doses (compared to amounts used in colon and other cancers) are required. Some investigators reported in 2010, that bevacizumab at a cost of around $42 a dose is as effective as ranibizumab at a cost of over $1,593 a dose.[66][67]
As of April 2015[update], there was a fierce debate in the UK and other European countries concerning the choice of prescribing bevacizumab or ranibizumab (Lucentis) for wet AMD.[68] In the UK, part of the tension was between on the one hand, both the European Medicines Agency and the Medicines and Healthcare products Regulatory Agency which had approved Lucentis but not Avastin for wet AMD, and their interest in ensuring that doctors to do not use medicines off-label when there are other, approved medications for the same indication, and on the other hand, NICE in the UK, which sets treatment guidelines, and has been unable so far to appraise Avastin as a first-line treatment, in order to save money for the National Health Service.[68] Novartis and Roche (which respectively have marketing rights and ownership rights for Avastin) had not conducted clinical trials to get approval for Avastin for wet AMD and had no intention of doing so.[68] Further, both companies lobbied against treatment guidelines that would make Avastin a first-line treatment, and when government-funded studies comparing the two drugs were published, they published papers emphasizing the risks of using Avastin for wet AMD.[68]
Breast cancer approval
On March 28, 2007, the European Commission approved bevacizumab in combination with paclitaxel for the first-line treatment of metastatic breast cancer.[69]
In 2008, the FDA approved bevacizumab for use in breast cancer. A panel of outside advisers voted 5 to 4 against approval, but their recommendations were overruled. The panel expressed concern that data from the clinical trial did not show any increase in quality of life or prolonging of life for patients—two important benchmarks for late-stage cancer treatments. The clinical trial did show that bevacizumab reduced tumor volumes and showed an increase in progression free survival time. It was based on this data that the FDA chose to overrule the recommendation of the panel of advisers. This decision was lauded by patient advocacy groups and some oncologists. Other oncologists felt that granting approval for late-stage cancer therapies that did not prolong or increase the quality of life for patients would give license to pharmaceutical companies to ignore these important benchmarks when developing new late-stage cancer therapies.[55]
In 2010, before the FDA announcement, The National Comprehensive Cancer Network (NCCN) updated the NCCN Clinical Practice Guidelines for Oncology (NCCN Guidelines) for Breast Cancer to affirm the recommendation regarding the use of bevacizumab in the treatment of metastatic breast cancer.[citation needed]
In 2011, the US Food and Drug Administration removed bevacizumab indication for metastatic breast cancer after concluding that the drug has not been shown to be safe and effective. The specific indication that was withdrawn was for the use of bevacizumab in metastatic breast cancer, with paclitaxel for the treatment of people who have not received chemotherapy for metastatic HER2-negative breast cancer.[citation needed]
Counterfeit
On Tuesday, February 14, 2012, Roche and its U.S. biotech unit Genentech announced that counterfeit Avastin had been distributed in the United States.[70] The investigation is ongoing, but differences in the outer packaging make identification of the bogus drugs simple for medical providers. Roche analyzed three bogus vials of Avastin and found they contained salt, starch, citrate, isopropanol, propanediol, t-butanol, benzoic acid, di-fluorinated benzene ring, acetone and phthalate moiety, but no active ingredients of the cancer drug. According to Roche, the levels of the chemicals were not consistent; whether the chemicals were at harmful concentrations could not therefore be determined. The counterfeit Avastin has been traced back to Egypt, and it entered legitimate supply chains via Europe to the United States.[71][72]
Biosimilars
In July 2014, two pharming companies, PlantForm and PharmaPraxis, announced plans to commercialize a biosimilar version of bevacizumab made using a tobacco expression system in collaboration with the Fraunhofer Center for Molecular Biology.[73]
In September 2017, the US FDA approved Amgen's biosimilar (generic name bevacizumab-awwb, product name Mvasi) for six cancer indications.[74]
In January 2018, Mvasi was approved for use in the European Union.[75]
In February 2019, Zirabev was approved for use in the European Union.[76]
In June 2020, the Committee for Medicinal Products for Human Use (CHMP) of the European Medicines Agency (EMA) recommended the approval of Aybintio.[77]
Research
A study released in April 2009, found that bevacizumab is not effective at preventing recurrences of non-metastatic colon cancer following surgery.[78]
Bevacizumab has been tested in ovarian cancer where it has shown improvement in progression-free survival but not in overall survival.[79] and glioblastoma multiforme where it failed to improve overall survival.[80][81]
Bevacizumab has been investigated as a possible treatment of pancreatic cancer, as an addition to chemotherapy, but studies have shown no improvement in survival.[82][83][84] It may also cause higher rates of high blood pressure, bleeding in the stomach and intestine, and intestinal perforations.[medical citation needed]
The drug has also undergone trials as an addition to established chemotherapy protocols and surgery in the treatment of pediatric osteosarcoma,[85] and other sarcomas, such as leiomyosarcoma.[86]
Bevacizumab has been studied as a treatment for cancers that grow from the nerve connecting the ear and the brain.[87]
As of 2012[update], clinical trials were underway to test an intra-arterial technique for delivering the drug directly to brain tumors, bypassing the blood–brain barrier.[88]
References
- ↑ "Bevacizumab Injection: MedlinePlus Drug Information". NLM.nih.gov. 28 February 2014. Archived from the original on 25 March 2014.
- ↑ "Bevacizumab - Drugs.com". www.drugs.com. Archived from the original on 28 December 2016. Retrieved 28 December 2016.
- ↑ "Mvasi- bevacizumab-awwb injection, solution". DailyMed. 25 June 2019. Archived from the original on 27 July 2020. Retrieved 18 March 2020.
- ↑ "Zirabev- bevacizumab-bvzr injection, solution". DailyMed. 27 January 2020. Archived from the original on 27 July 2020. Retrieved 18 March 2020.
- ↑ 5.00 5.01 5.02 5.03 5.04 5.05 5.06 5.07 5.08 5.09 5.10 5.11 "Bevacizumab". The American Society of Health-System Pharmacists. Archived from the original on 20 December 2016. Retrieved 8 December 2016.
- ↑ 6.0 6.1 6.2 "Avastin- bevacizumab injection, solution". DailyMed. 28 June 2019. Archived from the original on 27 July 2020. Retrieved 18 March 2020.
- ↑ 7.0 7.1 "Bevacizumab Use During Pregnancy". Drugs.com. 30 July 2019. Archived from the original on 18 March 2020. Retrieved 18 March 2020.
- ↑ 8.0 8.1 "Search Results By Name – International Medical Products Price Guide". mshpriceguide. Archived from the original on 28 August 2021. Retrieved 16 August 2020.
- ↑ 9.0 9.1 World Health Organization (2019). World Health Organization model list of essential medicines: 21st list 2019. Geneva: World Health Organization. hdl:10665/325771. WHO/MVP/EMP/IAU/2019.06. License: CC BY-NC-SA 3.0 IGO.
- ↑ "Bevacizumab". International Drug Price Indicator Guide. Archived from the original on 22 October 2018. Retrieved 8 December 2016.
- ↑ British national formulary : BNF 69 (69 ed.). British Medical Association. 2015. p. 597. ISBN 9780857111562.
- ↑ 12.0 12.1 European Medicines Agency. 2005 Bevacizumab Scientific DIscussion Archived 2015-09-24 at the Wayback Machine
- ↑ "Avastin EPAR". European Medicines Agency (EMA). 11 March 2020. Archived from the original on 18 March 2020. Retrieved 18 March 2020.
- ↑ Van Cutsem E, Lambrechts D, Prenen H, Jain RK, Carmeliet P (January 2011). "Lessons from the adjuvant bevacizumab trial on colon cancer: what next?". Journal of Clinical Oncology. 29 (1): 1–4. doi:10.1200/JCO.2010.32.2701. PMID 21115866.
- ↑ Barlesi F, Scherpereel A, Gorbunova V, Gervais R, Vikström A, Chouaid C, Chella A, Kim JH, Ahn MJ, Reck M, Pazzola A, Kim HT, Aerts JG, Morando C, Loundou A, Groen HJ, Rittmeyer A (May 2014). "Maintenance bevacizumab-pemetrexed after first-line cisplatin-pemetrexed-bevacizumab for advanced nonsquamous nonsmall-cell lung cancer: updated survival analysis of the AVAPERL (MO22089) randomized phase III trial". Annals of Oncology. 25 (5): 1044–52. doi:10.1093/annonc/mdu098. PMID 24585722.
- ↑ "Questions and Answers about Avastin". U.S. Food and Drug Administration (FDA). 16 December 2010. Archived from the original on 23 April 2020. Retrieved 22 April 2020.
- ↑ "Avastin (bevacizumab) Information". U.S. Food and Drug Administration (FDA). 29 June 2011. Archived from the original on 23 April 2020. Retrieved 22 April 2020.
- ↑ "FDA begins process to remove breast cancer indication from Avastin label" (Press release). U.S. Food and Drug Administration (FDA). 16 December 2010. Archived from the original on 16 December 2010. Retrieved 17 December 2010.
- ↑ Pollack, Andrew (16 December 2010). "F.D.A. Rejects Use of Drug in Cases of Breast Cancer". The New York Times. Archived from the original on 11 November 2012. Retrieved 16 December 2010.
- ↑ Couzin-Frankel J, Ogale Y (July 2011). "FDA. Once on 'fast track,' avastin now derailed". Science. 333 (6039): 143–4. doi:10.1126/science.333.6039.143. PMID 21737712.
- ↑ "FDA clears Genentech drug for kidney cancer". San Francisco Chronicle. 2 August 2009. Archived from the original on 30 September 2010.
- ↑ "FDA Gives Roche's Avastin the Go-Ahead for Metastatic Renal Carcinoma". GENNewsHighlights. Genetic Engineering & Biotechnology News. 3 August 2009. Archived from the original on 11 May 2020. Retrieved 13 August 2012.
- ↑ Rini BI (February 2007). "Vascular endothelial growth factor-targeted therapy in renal cell carcinoma: current status and future directions". Clinical Cancer Research. 13 (4): 1098–106. doi:10.1158/1078-0432.CCR-06-1989. PMID 17317817.
- ↑ European Medicines Agency (January 2008). "Avastin-H-C-582-II-0015 : EPAR - Assessment Report - Variation" (PDF). Archived (PDF) from the original on 30 January 2012.
- ↑ 25.0 25.1 Ameratunga M, Pavlakis N, Wheeler H, Grant R, Simes J, Khasraw M (November 2018). "Anti-angiogenic therapy for high-grade glioma". The Cochrane Database of Systematic Reviews. 11: CD008218. doi:10.1002/14651858.CD008218.pub4. PMC 6516839. PMID 30480778.
- ↑ Pazdur, Richard (May 2009). "FDA Approval for Bevacizumab". National Cancer Institute. Archived from the original on 10 January 2010. Retrieved 11 May 2010.
- ↑ "FDA Grants Accelerated Approval of Avastin for Brain Cancer (Glioblastoma) That Has Progressed Following Prior Therapy". Drugs.com. 5 May 2009. Archived from the original on 26 July 2020. Retrieved 22 April 2020.
- ↑ Arevalo JF, Fromow-Guerra J, Sanchez JG, Maia M, Berrocal MH, Wu L, Saravia MJ, Costa RA (2008). "Primary intravitreal bevacizumab for subfoveal choroidal neovascularization in age-related macular degeneration: results of the Pan-American Collaborative Retina Study Group at 12 months follow-up". Retina. 28 (10): 1387–94. doi:10.1097/IAE.0b013e3181884ff4. PMID 18827735.
- ↑ Azad R, Chandra P (2007). "Intravitreal bevacizumab in aggressive posterior retinopathy of prematurity". Indian Journal of Ophthalmology. 55 (4): 319, author reply 320. doi:10.4103/0301-4738.33057. PMID 17595491.
- ↑ Moja L, Lucenteforte E, Kwag KH, Bertele V, Campomori A, Chakravarthy U, D'Amico R, Dickersin K, Kodjikian L, Lindsley K, Loke Y, Maguire M, Martin DF, Mugelli A, Mühlbauer B, Püntmann I, Reeves B, Rogers C, Schmucker C, Subramanian ML, Virgili G (September 2014). Moja L (ed.). "Systemic safety of bevacizumab versus ranibizumab for neovascular age-related macular degeneration". The Cochrane Database of Systematic Reviews. 9 (9): CD011230. doi:10.1002/14651858.CD011230.pub2. PMC 4262120. PMID 25220133.
- ↑ Scott LJ, Chakravarthy U, Reeves BC, Rogers CA (March 2015). "Systemic safety of anti-VEGF drugs: a commentary". Expert Opinion on Drug Safety. 14 (3): 379–88. doi:10.1517/14740338.2015.991712. PMID 25489638.
- ↑ Chen G, Li W, Tzekov R, Jiang F, Mao S, Tong Y (February 2015). "Bevacizumab versus ranibizumab for neovascular age-related macular degeneration: a meta-analysis of randomized controlled trials". Retina. 35 (2): 187–93. doi:10.1097/IAE.0000000000000301. PMID 25105318.
- ↑ Kodjikian L, Decullier E, Souied EH, Girmens JF, Durand EE, Chapuis FR, Huot L (October 2014). "Bevacizumab and ranibizumab for neovascular age-related macular degeneration: an updated meta-analysis of randomised clinical trials". Graefe's Archive for Clinical and Experimental Ophthalmology = Albrecht von Graefes Archiv Fur Klinische und Experimentelle Ophthalmologie. 252 (10): 1529–37. doi:10.1007/s00417-014-2764-6. PMC 4180904. PMID 25142373.
- ↑ Wang W, Zhang X (2014). "Systemic adverse events after intravitreal bevacizumab versus ranibizumab for age-related macular degeneration: a meta-analysis". PLOS One. 9 (10): e109744. Bibcode:2014PLoSO...9j9744W. doi:10.1371/journal.pone.0109744. PMC 4199620. PMID 25330364.
- ↑ 35.0 35.1 "FDA approves bevacizumab in combination with chemotherapy for ovarian cancer". U.S. Food and Drug Administration (FDA). 13 June 2018. Archived from the original on 18 March 2020. Retrieved 4 August 2018.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain.
- ↑ Semenza GL (May 2008). "A new weapon for attacking tumor blood vessels". The New England Journal of Medicine. 358 (19): 2066–7. doi:10.1056/NEJMcibr0800272. PMID 18463385.
- ↑ Sliesoraitis S, Tawfik B (July 2011). "Bevacizumab-induced bowel perforation". The Journal of the American Osteopathic Association. 111 (7): 437–41. PMID 21803880.
- ↑ "AVASTIN (bevacizumab) injection, for intravenous use" (PDF). Genentech, Inc. Archived (PDF) from the original on 29 April 2016. Retrieved 2 June 2016.
- ↑ Velcheti V, Viswanathan A, Govindan R (June 2006). "The proportion of patients with metastatic non-small cell lung cancer potentially eligible for treatment with bevacizumab: a single institutional survey". Journal of Thoracic Oncology. 1 (5): 501. doi:10.1097/01243894-200606000-00023. PMID 17409907.
- ↑ Vaughn C, Zhang L, Schiff D (January 2008). "Reversible posterior leukoencephalopathy syndrome in cancer". Current Oncology Reports. 10 (1): 86–91. doi:10.1007/s11912-008-0013-z. PMID 18366965.
- ↑ Eremina V, Jefferson JA, Kowalewska J, Hochster H, Haas M, Weisstuch J, Richardson C, Kopp JB, Kabir MG, Backx PH, Gerber HP, Ferrara N, Barisoni L, Alpers CE, Quaggin SE (March 2008). "VEGF inhibition and renal thrombotic microangiopathy". The New England Journal of Medicine. 358 (11): 1129–36. doi:10.1056/NEJMoa0707330. PMC 3030578. PMID 18337603.
- ↑ "Cancer drug Avastin tied to 2 cases of flesh-eating disease in Canada". CBC News. 2 May 2013. Archived from the original on 2 May 2013. Retrieved 2 May 2013.
- ↑ Godfrey SE (May 1989). "Estrogen receptors". American Journal of Clinical Pathology. 91 (5): 629–30. doi:10.1215/15228517-2008-118. PMC 2718965. PMID 2718965.
- ↑ 44.0 44.1 "Avastin full Prescribing Information - Genentech" (PDF). Gene.com. 2011. Archived (PDF) from the original on 14 July 2011.
- ↑ Los M, Roodhart JM, Voest EE (April 2007). "Target practice: lessons from phase III trials with bevacizumab and vatalanib in the treatment of advanced colorectal cancer". The Oncologist. 12 (4): 443–50. doi:10.1634/theoncologist.12-4-443. PMID 17470687.
- ↑ Shih T, Lindley C (November 2006). "Bevacizumab: an angiogenesis inhibitor for the treatment of solid malignancies". Clinical Therapeutics. 28 (11): 1779–802. doi:10.1016/j.clinthera.2006.11.015. PMID 17212999.
- ↑ Andrew Pollack for The New York Times. February 27, 2004 F.D.A. Approves Cancer Drug From Genentech Archived 2016-10-24 at the Wayback Machine
- ↑ Palmer AM, Stephenson FA, Williams RJ (April 2007). "Society for Medicines Research: 40th anniversary symposium". Drug News & Perspectives. 20 (3): 191–6. PMID 17520096.
- ↑ Ferrara N (2009). "Anti-angiogenic drugs to treat human disease: an interview with Napoleone Ferrara by Kristin H. Kain". Disease Models & Mechanisms. 2 (7–8): 324–5. doi:10.1242/dmm.002972. PMID 19553691.
- ↑ 50.0 50.1 Ribatti D (2008). "Napoleone Ferrara and the saga of vascular endothelial growth factor". Endothelium. 15 (1): 1–8. doi:10.1080/10623320802092377. PMID 18568940.
- ↑ Ferrara N (2011). "From the discovery of vascular endothelial growth factor to the introduction of avastin in clinical trials - an interview with Napoleone Ferrara by Domenico Ribatti". The International Journal of Developmental Biology. 55 (4–5): 383–8. doi:10.1387/ijdb.103216dr. PMID 21858763.
- ↑ "Press Announcements - FDA Commissioner announces Avastin decision". U.S. Food and Drug Administration. 18 November 2011. Archived from the original on 15 December 2014. Retrieved 31 October 2014.
- ↑ 53.0 53.1 Pollack, Andrew (18 November 2011). "F.D.A. Revokes Approval of Avastin for Breast Cancer". The New York Times. Archived from the original on 21 November 2011.
- ↑ "Cancer drug Avastin loses US approval". BBC News Online. 18 November 2011. Archived from the original on 19 November 2011.
- ↑ 55.0 55.1 "F.D.A. Approves Drug's Use for Breast Cancer". The New York Times. 22 February 2008. Archived from the original on 2 February 2017.
- ↑ "Breast cancer drug 'still safe' for Aussie women". Australian Broadcasting Corporation. 22 July 2010. Archived from the original on 23 July 2010.
- ↑ "David Cameron's flagship Cancer Drugs Fund 'is a waste of NHS cash'". The Guardian. 10 January 2015. Archived from the original on 15 January 2015. Retrieved 11 January 2015.
- ↑ Briggs, Helen (24 August 2010). "Critics condemn bowel cancer drug rejection". Archived from the original on 24 August 2010. Retrieved 24 August 2010.
- ↑ "Bevacizumab" (PDF). Scottish Medicines. Archived from the original (PDF) on 24 April 2012. Retrieved 18 July 2012.
- ↑ Berenson, Alex (15 February 2006). "A Cancer Drug Shows Promise, at a Price That Many Can't Pay". The New York Times. Archived from the original on 18 November 2015.
- ↑ Mayer RJ (June 2004). "Two steps forward in the treatment of colorectal cancer". New England Journal of Medicine. 350 (23): 2406–8. doi:10.1056/NEJMe048098. PMID 15175443.
- ↑ "P.E.I. sole holdout on cancer drug". CBC News. 26 November 2009. Archived from the original on 16 September 2015.
- ↑ Cohen D (October 2018). "Bayer and Novartis appeal ruling that Avastin for wet AMD is lawful". BMJ. 363: k4586. doi:10.1136/bmj.k4586. PMID 30377211.
- ↑ 64.0 64.1 Saporito, Bill (27 October 2014). "Hospitals Furious at Cancer-Drug Price Hikes". Time. Archived from the original on 20 October 2015. Retrieved 26 October 2015.
- ↑ Johnson K, Blansett L, Mawrie R, Di Biase S. "Innovation in Cancer Care and Implications for Health Systems: Global Oncology Trend Report" (PDF). One IMS Drive, Plymouth Meeting, PA 19462, USA: IMS Institute for Health Care Informatics. Archived from the original on 13 October 2015.
{{cite web}}: CS1 maint: location (link) - ↑ Mundy, Alicia (17 June 2010). "Medicare Eye Study Finds Untapped Savings". Wall Street Journal. Archived from the original on 23 September 2013. Retrieved 3 August 2017.
- ↑ Tufail A, Patel PJ, Egan C, Hykin P, da Cruz L, Gregor Z, Dowler J, Majid MA, Bailey C, Mohamed Q, Johnston R, Bunce C, Xing W (June 2010). "Bevacizumab for neovascular age related macular degeneration (ABC Trial): multicentre randomised double masked study". BMJ. 340: c2459. doi:10.1136/bmj.c2459. PMID 20538634. Archived from the original on 17 June 2010. Retrieved 4 September 2019.
- ↑ 68.0 68.1 68.2 68.3 "Why have UK doctors been deterred from prescribing Avastin?". The British Medical Journal. 1 April 2015. Archived from the original on 4 April 2015. Retrieved 2 April 2015.
- ↑ Jasek W, ed. (2007). Austria-Codex (in German) (2007/2008 ed.). Vienna: Österreichischer Apothekerverlag. ISBN 978-3-85200-181-4.
{{cite book}}: CS1 maint: unrecognized language (link)[page needed] - ↑ "Counterfeits of cancer drug Avastin found in U.S". Reuters. 15 February 2012. Archived from the original on 24 September 2015.
- ↑ Berkrot, Bill (27 February 2012). "Fake Avastin had salt, starch, chemicals:Roche". Reuters. Archived from the original on 3 March 2012. Retrieved 28 February 2012.
- ↑ Staton, Tracy (28 February 2012). "Phony Avastin vials contained chemicals, but no drugs". FiercePharma. Archived from the original on 1 March 2012. Retrieved 28 February 2012.
- ↑ Brennan, Zachary (23 July 2014). "Brazilian JV to tap plant-based manufacturing system for biosimilars". BioPharma-Reporter. Archived from the original on 10 January 2016. Retrieved 18 March 2020.
- ↑ Gever, John (14 September 2017). "Avastin Clone OK'd — Biosimilar for bevacizumab approved for various cancers". MedPage Today. Archived from the original on 16 September 2017. Retrieved 18 March 2020.
- ↑ "Mvasi". European Medicines Agency (EMA). 17 September 2018. Archived from the original on 30 December 2019. Retrieved 2 April 2020.
- ↑ "Zirabev". European Medicines Agency (EMA). 11 December 2018. Archived from the original on 30 December 2019. Retrieved 2 April 2020.
- ↑ "Aybintio: Pending EC decision". European Medicines Agency (EMA). 25 June 2020. Archived from the original on 27 June 2020. Retrieved 26 June 2020.
- ↑ Reed, Katie (22 April 2009). "Roche drug Avastin fails cancer study, shares fall". Reuters. Archived from the original on 12 August 2009. Retrieved 22 April 2009.
- ↑ Rossi L, Verrico M, Zaccarelli E, Papa A, Colonna M, Strudel M, Vici P, Bianco V, Tomao F (February 2017). "Bevacizumab in ovarian cancer: A critical review of phase III studies". Oncotarget. 8 (7): 12389–12405. doi:10.18632/oncotarget.13310. PMC 5355353. PMID 27852039.
- ↑ Diaz RJ, Ali S, Qadir MG, De La Fuente MI, Ivan ME, Komotar RJ (July 2017). "The role of bevacizumab in the treatment of glioblastoma". Journal of Neuro-oncology. 133 (3): 455–467. doi:10.1007/s11060-017-2477-x. PMID 28527008.
- ↑ Kim MM, Umemura Y, Leung D (2018). "Bevacizumab and Glioblastoma: Past, Present, and Future Directions". Cancer Journal. Sudbury, Mass. 24 (4): 180–186. doi:10.1097/PPO.0000000000000326. PMID 30119081.
- ↑ Saif MW (July 2008). "New developments in the treatment of pancreatic cancer. Highlights from the "44th ASCO Annual Meeting". Chicago, IL, USA. May 30 - June 3, 2008". JOP. 9 (4): 391–7. PMID 18648128. Archived from the original on 31 January 2009.
- ↑ Rocha-Lima CM (June 2008). "New directions in the management of advanced pancreatic cancer: a review". Anti-Cancer Drugs. 19 (5): 435–46. doi:10.1097/CAD.0b013e3282fc9d11. PMID 18418211.
- ↑ Riess, Hanno (2008). "Antiangiogenic Strategies in Pancreatic Cancer". Pancreatic Cancer. Recent Results in Cancer Research. Vol. 177. pp. 123–9. doi:10.1007/978-3-540-71279-4_14. ISBN 978-3-540-71266-4. PMID 18084954.
- ↑ Navid F, Santana VM, Neel M, McCarville MB, Shulkin BL, Wu J, Billups CA, Mao S, Daryani VM, Stewart CF, Kunkel M, Smith W, Ward D, Pappo AS, Bahrami A, Loeb DM, Reikes Willert J, Rao BN, Daw NC (October 2017). "A phase II trial evaluating the feasibility of adding bevacizumab to standard osteosarcoma therapy". International Journal of Cancer. 141 (7): 1469–1477. doi:10.1002/ijc.30841. PMC 5812455. PMID 28631382.
- ↑ Bogani G, Ditto A, Martinelli F, Signorelli M, Chiappa V, Fonatella C, Sanfilippo R, Leone Roberti Maggiore U, Ferrero S, Lorusso D, Raspagliesi F (June 2018). "Role of bevacizumab in uterine leiomyosarcoma". Critical Reviews in Oncology/hematology. 126: 45–51. doi:10.1016/j.critrevonc.2018.03.019. PMID 29759566.
- ↑ Plotkin SR, Merker VL, Halpin C, Jennings D, McKenna MJ, Harris GJ, Barker FG (August 2012). "Bevacizumab for progressive vestibular schwannoma in neurofibromatosis type 2: a retrospective review of 31 patients". Otology & Neurotology. 33 (6): 1046–52. doi:10.1097/MAO.0b013e31825e73f5. PMID 22805104.
- ↑ Burkhardt JK, Riina H, Shin BJ, Christos P, Kesavabhotla K, Hofstetter CP, Tsiouris AJ, Boockvar JA (January 2012). "Intra-arterial delivery of bevacizumab after blood-brain barrier disruption for the treatment of recurrent glioblastoma: progression-free survival and overall survival". World Neurosurgery. 77 (1): 130–4. doi:10.1016/j.wneu.2011.05.056. PMC 3743246. PMID 22405392.
Further reading
- Berenson, Alex (15 February 2006). "A Cancer Drug Shows Promise, at a Price That Many Can't Pay". The New York Times. Archived from the original on 18 November 2015. Retrieved 18 February 2017.
- Sachdev JC, Jahanzeb M (October 2008). "Evolution of bevacizumab-based therapy in the management of breast cancer". Clinical Breast Cancer. 8 (5): 402–10. doi:10.3816/CBC.2008.n.048. PMID 18952553.
External links
| External sites: | |
|---|---|
| Identifiers: |
|
- "Bevacizumab". National Cancer Institute. Archived from the original on 10 April 2020. Retrieved 18 March 2020.
- "Bevacizumab". NCI Drug Dictionary. Archived from the original on 22 May 2020. Retrieved 23 April 2020.
- Pages using duplicate arguments in template calls
- Webarchive template wayback links
- Wikipedia articles incorporating the PD-notice template
- CS1 maint: location
- CS1 maint: unrecognized language
- Wikipedia articles needing page number citations from July 2011
- Articles with invalid date parameter in template
- Use dmy dates from April 2020
- Drugs with non-standard legal status
- Chemical articles with unknown parameter in Infobox drug
- Chemical articles without CAS registry number
- Articles without EBI source
- Chemical pages without ChemSpiderID
- Chemical pages without DrugBank identifier
- Articles without KEGG source
- Articles without InChI source
- Articles without UNII source
- Drugs missing an ATC code
- Drug has EMA link
- Drugboxes which contain changes to verified fields
- Drugboxes which contain changes to watched fields
- Drugs that are a monoclonal antibody
- All articles with unsourced statements
- Articles with unsourced statements from January 2020
- Articles with unsourced statements from March 2020
- All articles with vague or ambiguous time
- Vague or ambiguous time from January 2020
- Articles with unsourced statements from July 2011
- Articles containing potentially dated statements from April 2015
- All articles containing potentially dated statements
- Articles with hatnote templates targeting a nonexistent page
- Articles containing potentially dated statements from 2012
- Chemicals that do not have a ChemSpider ID assigned
- Articles with changed EBI identifier
- Angiogenesis inhibitors
- Genentech brands
- Hoffmann-La Roche brands
- Monoclonal antibodies for tumors
- Ophthalmology drugs
- Orphan drugs
- Specialty drugs
- World Health Organization essential medicines
- RTT