Sunitinib
 | |
 | |
| Names | |
|---|---|
| Trade names | Sutent, others |
| Other names | SU11248 |
| |
| Clinical data | |
| Drug class | Receptor tyrosine kinase (RTK) inhibitor[1] |
| Main uses | Renal cell carcinoma (RCC), gastrointestinal stromal tumor (GIST), pancreatic neuroendocrine tumor (pNET)[2] |
| Side effects | Tiredness, fever, nausea, diarrhea, inflammation of the mouth, abdominal pain, swelling, rash, pain, bleeding, shortness of breath[1] |
| Pregnancy category |
|
| Routes of use | By mouth |
| Typical dose | 50 mg OD[2] |
| External links | |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a607052 |
| Legal | |
| License data | |
| Legal status | |
| Pharmacokinetics | |
| Bioavailability | Unaffected by food |
| Protein binding | 95% |
| Metabolism | Liver (CYP3A4-mediated) |
| Elimination half-life | 40 to 60 hours (sunitinib) 80 to 110 hours (metabolite) |
| Excretion | Fecal (61%) and Kidney (16%) |
| Chemical and physical data | |
| Formula | C22H27FN4O2 |
| Molar mass | 398.482 g·mol−1 |
| 3D model (JSmol) | |
| |
| |
Sunitinib, sold under the brand name Sutent, is a medication used to treat cancer, specifically renal cell carcinoma (RCC), gastrointestinal stromal tumor (GIST), and pancreatic neuroendocrine tumor (pNET).[2] It is taken by mouth.[2]
Common side effects include tiredness, fever, nausea, diarrhea, inflammation of the mouth, abdominal pain, swelling, rash, pain, bleeding, and shortness of breath.[1] Other side effects may include liver problems, osteonecrosis of the jaw, and prolonged QT.[1] Use during pregnancy may harm the baby.[1] It is a receptor tyrosine kinase (RTK) inhibitor.[1]
Sunitinib was approved for medical use in the United States and Europe in 2006.[1][3] In the United Kingdom 4 weeks of medication costs the NHS about £3,100 as of 2021.[4] In the United States this amount costs about 4,900 USD.[5]
Medical uses
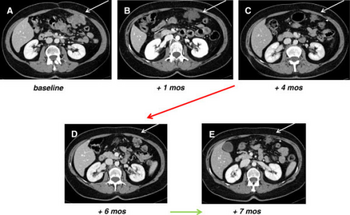
Gastrointestinal stromal tumor
Like RCC, GIST does not generally respond to standard chemotherapy or radiation. Imatinib was the first cancer agent proven effective for metastatic GIST and represented a major development in the treatment of this rare but challenging disease. However, approximately 20% of patients do not respond to imatinib (early or primary resistance), and among those who do respond initially, 50% develop secondary imatinib resistance and disease progression within two years. Prior to sunitinib, patients had no therapeutic option once they became resistant to imatinib.[6]
Pancreatic neuroendocrine tumors
In 2010, it gained approval from the European Commission for the treatment of 'unresectable or metastatic, well-differentiated pancreatic neuroendocrine tumors with disease progression in adults'.[7] In May 2011, the USFDA approved sunitinib for treating people with 'progressive neuroendocrine cancerous tumors located in the pancreas that cannot be removed by surgery or that have spread to other parts of the body (metastatic)'.[8]
Renal cell carcinoma
Sunitinib is approved for treatment of metastatic RCC. Other therapeutic options in this setting are pazopanib, sorafenib, temsirolimus, interleukin-2, everolimus, bevacizumab, and aldesleukin.
RCC is generally resistant to chemotherapy or radiation. Prior to RTKs, metastatic disease could only be treated with the cytokines interferon alpha (IFNα) or interleukin-2. However, these agents demonstrated low rates of efficacy (5%-20%).
In a phase III study, median progression-free survival was significantly longer in the sunitinib group (11 months) than in the IFNα group (five months), a hazard ratio of 0.42.[2][9] In the secondary endpoints, 28% had significant tumor shrinkage with sunitinib compared to 5% with IFNα. Patients receiving sunitinib had a better quality of life than IFNα. An update in 2008 showed that the primary endpoint of median progression-free survival (PFS) remained superior with sunitinib: 11 months versus 5 months for IFNα, P<.000001. Objective response rate also remained superior: 39-47% for sunitinib versus 8-12% with IFNα, P<.000001.[10][11]
Sunitinib treatment trended towards a slightly longer overall survival, although this was not statistically significant.
- Median overall survivability was 26 months with sunitinib vs 22 months for IFNα regardless of stratification (P-value ranges from .051 to .0132, depending on statistical analysis).
- The first analysis includes 25 patients initially randomized to IFNα who crossed over to sunitinib therapy, which may have confounded the results; in an exploratory analysis that excluded these patients, the difference becomes more robust: 26 vs 20 months, P=.0081.
- Patients in the study were allowed to receive other therapies once they had progressed on their study treatment. For a "pure" analysis of the difference between the two agents, an analysis was done using only patients who did not receive any post-study treatment. This analysis demonstrated the greatest advantage for sunitinib: 28 months vs 14 months for IFNα, P=.0033. The number of patients in this analysis was small and this does not reflect actual clinical practice and is therefore not meaningful.
Dosage
It is typically taken at a dose of 50 mg per day for GIST and RCC.[2] A dose of 37.5 mg per day is used in pNET.[2]
Side effects
Sunitinib adverse events are considered somewhat manageable and the incidence of serious adverse events low.[6][9]
The most common side effects are fatigue, diarrhea, nausea, anorexia, hypertension, a yellow skin discoloration, hand-foot skin reaction, and stomatitis.[12] In the placebo-controlled Phase III GIST study, adverse events which occurred more often with sunitinib than placebo included diarrhea, anorexia, skin discoloration, mucositis/stomatitis, asthenia, altered taste, and constipation.[2][6]
Dose reductions were required in 50% of the patients studied in RCC in order to manage the significant toxicities of this agent.
Serious (grade 3 or 4) adverse events occur in ≤10% of patients and include hypertension, fatigue, asthenia, diarrhea, and chemotherapy-induced acral erythema. Lab abnormalities associated with sunitinib therapy include lipase, amylase, neutrophils, lymphocytes, and platelets. Hypothyroidism and reversible erythrocytosis have also been associated with sunitinib.[2][13]
Most adverse events can be managed through supportive care, dose interruption, or dose reduction.[6][9]
Sunitinib was relatively well tolerated. About 83% of sunitinib patients experienced a treatment-related adverse event of any severity, as did 59% of patients who received placebo. Serious adverse events were reported in 20% of sunitinib patients and 5% of placebo patients. Adverse events were generally moderate and easily managed by dose reduction, dose interruption, or other treatment. Nine percent of sunitinib patients and 8% of placebo patients discontinued therapy due to an adverse event.[6]
Fatigue is the adverse event most commonly associated with sunitinib therapy. In this study, 34% of sunitinib patients reported any grade of fatigue, compared with 22% for placebo. The incidence of grade 3 (severe) fatigue was similar between the two groups, and no grade 4 fatigue was reported.[6]
Interactions
Epigallocatechin-3-gallate, a major constituent of green tea, may reduce the bioavailability of sunitinib when they are taken together.[14]
Mechanism of action
Sunitinib inhibits cellular signaling by targeting multiple receptor tyrosine kinases (RTKs).
These include all receptors for platelet-derived growth factor (PDGF-Rs) and vascular endothelial growth factor receptors (VEGFRs), which play a role in both tumor angiogenesis and tumor cell proliferation. The simultaneous inhibition of these targets therefore reduces tumor vascularization and triggers cancer cell apoptosis and thus results in tumor shrinkage.
Sunitinib also inhibits CD117 (c-KIT),[15] the receptor tyrosine kinase that (when improperly activated by mutation) drives the majority of gastrointestinal stromal cell tumors.[16] It has been recommended as a second-line therapy for patients whose tumors develop mutations in c-KIT that make them resistant to imatinib, or who the cannot tolerate the drug.[17][18]
In addition, sunitinib binds other receptors.[2] These include:
The fact that sunitinib targets many different receptors, leads to many of its side effects such as the classic hand-foot syndrome, stomatitis, and other dermatologic toxicities.
History
The drug was discovered at SUGEN, a biotechnology company which pioneered protein kinase inhibitors. It was the third in a series of compounds including SU5416 and SU6668. The concept was of an ATP mimic that would compete with ATP for binding to the catalytic site of receptor tyrosine kinases. This concept led to the invention of many small-molecule tyrosine kinase inhibitors, including Gleevec, Sutent, Tarceva and many others.[citation needed]
Sunitinib was the first cancer drug simultaneously approved for two different indications.[19]
Society and culture
Economics
Sunitinib is marketed by Pfizer as Sutent, and is subject to patents and market exclusivity as a new chemical entity until February 15, 2021.[20][21] Sutent has been cited in financial news as a potential revenue source to replace royalties lost from Lipitor following the expiration of the latter drug's patent expiration in November 2011.[22][23] Sutent is one of the most expensive drugs widely marketed.[citation needed] Doctors and editorials have criticized the high cost for a drug that does not cure cancer, but only prolongs life.
US
In the U.S., the insurance companies[which?] have refused to pay for all or part of the costs of Sutent. Because it is an oral therapy, the copay associated with this therapy can be very substantial. If a patient's secondary insurance does not cover this, the cost burden to the patient can be extreme. Particularly challenging is the Medicare Part D coverage gap. Patients have to spend thousands of dollars out-of-pocket during the gap in coverage. If this is done at the end of a calendar year, it has to be paid again at the beginning of the next calendar year, which may be burdensome financially.
UK
In the UK, NICE refused (late 2008) to recommend sunitinib for late-stage renal cancer (kidney cancer) due to the high cost per QALY, estimated by NICE at £72,000/QALY and by Pfizer at £29,000/QALY.[24][25] This was overturned in February 2009 after pricing changes and public responses.[26] Therefore, Sunitinib is recommended as a first-line treatment option for people with advanced and/or metastatic renal cell carcinoma who are suitable for immunotherapy and have an ECOG performance status of 0 or 1 (i.e. completely ambulatory).[27]
AU
Sunitinib is available in Australia and is subsidized by the Pharmaceutical Benefits Scheme for Stage IV Renal Cell Carcinoma (RCC). The cost to the patient who meets the clinical criteria of Stage IV RCC is AUD $35.40 for 28 capsules, regardless of dose. Manufacturer pricing for Sunitinib ranges from AUD $1,834.30 to AUD $6897.54, depending on dose (12.5 mg to 50 mg).[28]
Research
Other solid tumors
The efficacy of sunitinib is currently being evaluated in a broad range of solid tumors, including breast, lung, thyroid and colorectal cancers. Early studies have shown single-agent efficacy in a number of different areas. Sunitinib blocks the tyrosine kinase activities of KIT, PDGFR, VEGFR2 and other tyrosine kinases involved in the development of tumours.
- A Phase II study in previously treated patients with metastatic breast cancer found sunitinib “has significant single agent activity”.[29]
- A Phase II study of refractory non-small-cell lung cancer found “Sunitinib has provocative single-agent activity in previously treated pts with recurrent and advanced NSCLC, with the level of activity similar to currently approved agents.” [30]
- In a Phase II study of patients with nonresectable neuroendocrine tumors, 91% of patients responded to sunitinib (9% partial response + 82% stable disease).[31]
Leukemia
Sunitinib was used to treat the leukemia of a Washington University in St. Louis leukemia researcher who developed the disease himself. His team used genetic sequencing and noticed that the FLT3 gene was hyperactive in his leukemia cells and used sunitinib as a treatment.[32]
Unsuccessful trials
Between April 2009 and May 2011 Pfizer has reported unsuccessful late-stage trials in breast cancer, metastatic colorectal cancer, advanced non-small-cell lung cancer, and castration-resistant prostate cancer.[33]
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 "SUNItinib Monograph for Professionals". Drugs.com. Archived from the original on 23 January 2021. Retrieved 15 October 2021.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 "Sutent- sunitinib malate capsule". DailyMed. Archived from the original on 23 March 2021. Retrieved 7 April 2021.
- ↑ "Sutent". Archived from the original on 12 July 2021. Retrieved 15 October 2021.
- ↑ BNF (80 ed.). BMJ Group and the Pharmaceutical Press. September 2020 – March 2021. p. 1058. ISBN 978-0-85711-369-6.
{{cite book}}: CS1 maint: date format (link) - ↑ "Sunitinib Prices, Coupons & Savings Tips - GoodRx". GoodRx. Retrieved 15 October 2021.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 Demetri GD, et al. (2006). "Efficacy and safety of sunitinib in patients with advanced gastrointestinal stromal tumour after failure of imatinib: a randomised controlled trial". Lancet. 368 (9544): 1329–1338. doi:10.1016/S0140-6736(06)69446-4. PMID 17046465. S2CID 25931515.
- ↑ "Pfizer Scores New Approval for Sutent in Europe". 2 Dec 2010. Archived from the original on 24 September 2015. Retrieved 6 July 2021.
- ↑ FDA approves Sutent for rare type of pancreatic cancer
- ↑ 9.0 9.1 9.2 Motzer RJ, et al. (2007). "Sunitinib versus interferon alfa in metastatic renal-cell carcinoma". N Engl J Med. 356 (2): 115–124. doi:10.1056/NEJMoa065044. PMID 17215529.
- ↑ Figlin RA, et al. "Overall survival with sunitinib versus interferon alfa (IFN-α) as first-line treatment of metastatic renal cell carcinoma (mRCC). Abstract no. 5024". Presented at ASCO 2008. Available at: http://www.asco.org/ASCO/Abstracts+%26+Virtual+Meeting/Abstracts?&vmview=abst_detail_view&confID=55&abstractID=32895.
- ↑ Motzer RJ, Hutson TE, Tomczak P, et al. (August 2009). "Overall survival and updated results for sunitinib compared with interferon alfa in patients with metastatic renal cell carcinoma". J. Clin. Oncol. 27 (22): 3584–90. doi:10.1200/JCO.2008.20.1293. PMC 3646307. PMID 19487381.
- ↑ Dasanu CA, et al. (2007-03-01). "Yellow skin discoloration associated with sorafenib use for treatment of metastatic renal cell carcinoma". Southern Medical Journal. 100 (3): 328–330. doi:10.1097/smj.0b013e31802f01a9. PMID 17396743. Archived from the original on 2016-03-03. Retrieved 2021-07-06.
- ↑ Alexandrescu DT, McClure R, Farzanmehr H, Dasanu CA (2008). "Secondary erythrocytosis produced by the tyrosine kinase inhibitors sunitinib and sorafenib". Journal of Clinical Oncology. 26 (24): 4047–8. doi:10.1200/jco.2008.18.3525. PMID 18711201.
- ↑ Ge J, Tan BX, Chen Y, Yang L, Peng XC, Li HZ, Lin HJ, Zhao Y, Wei M, et al. (Jun 2011). "Interaction of green tea polyphenol epigallocatechin-3-gallate with sunitinib: potential risk of diminished sunitinib bioavailability". J Mol Med (Berl). 89 (6): 595–602. doi:10.1007/s00109-011-0737-3. PMID 21331509. S2CID 8334011.
- ↑ Hartmann JT, Kanz L (November 2008). "Sunitinib and periodic hair depigmentation due to temporary c-KIT inhibition". Arch Dermatol. 144 (11): 1525–6. doi:10.1001/archderm.144.11.1525. PMID 19015436. Archived from the original on 2011-07-25.
- ↑ Quek R, George S (February 2009). "Gastrointestinal stromal tumor: a clinical overview". Hematol. Oncol. Clin. North Am. 23 (1): 69–78, viii. doi:10.1016/j.hoc.2008.11.006. PMID 19248971.
- ↑ Blay JY, Reichardt P (June 2009). "Advanced gastrointestinal stromal tumor in Europe: a review of updated treatment recommendations". Expert Rev Anticancer Ther. 9 (6): 831–8. doi:10.1586/era.09.34. PMID 19496720. S2CID 23601578.
- ↑ Gan HK, Seruga B, Knox JJ (June 2009). "Sunitinib in solid tumors". Expert Opin Investig Drugs. 18 (6): 821–34. doi:10.1517/13543780902980171. PMID 19453268. S2CID 25353839.
- ↑ "FDA approves new treatment for gastrointestinal and kidney cancer". U.S. Food and Drug Administration (FDA). 2006. Archived from the original on 2006-02-03.
- ↑ "Patent and Exclusivity Search Results from query on Appl No 021938 Product 003 in the OB_Rx list". U.S. Food and Drug Administration (FDA). Archived from the original on 2011-09-17. Retrieved 2009-06-05. Sutent is subject to US patent 7211600 (expires Dec 22 2020), 7125905 and 6573293 (expire Feb 15 2021). Note that this information does not include or predict patent extensions.
- ↑ "Details for Generic 'SUNITINIB MALATE'". DrugPatentWatch. Archived from the original on 2021-04-10. Retrieved 2021-07-06.
- ↑ Jamie Dlugosch (2009-03-13). "Will biologics and Sutent save Pfizer?". InvestorPlace. Archived from the original on 2016-03-04. Retrieved 2021-07-06.
- ↑ Zacks Investment Research (2007-03-22). "Pfizer's a Sell: Shrinking Top Line, No Blockbusters In the Pipeline". SeekingAlpha. Archived from the original on 2016-03-03. Retrieved 2021-07-06.
- ↑ BMJ 31-Jan-2009 "NICE and the challenge of cancer drugs" p271
- ↑ "BBC news - Aug 2008 - 'We'll sell our house for this drug'". Archived from the original on 2009-06-11. Retrieved 2021-07-06.
- ↑ Daily Telegraph, Feb 4, 2009
- ↑ "Renal cancer - NICE Pathways". pathways.nice.org.uk. Archived from the original on 2017-03-15. Retrieved 2017-03-14.
- ↑ "Australian Pharmaceutical Benefits Scheme - Sutent". Archived from the original on 2021-04-28. Retrieved 2021-07-06.
- ↑ Miller KD, et al. "Phase II study of SU11248, a multi-targeted tyrosine kinase inhibitor in patients with previously treated metastatic breast cancer". Presented at ASCO 2005. Available at: http://www.asco.org/portal/site/ASCO/menuitem.34d60f5624ba07fd506fe310ee37a01d/?vgnextoid=76f8201eb61a7010VgnVCM100000ed730ad1RCRD&vmview=abst_detail_view&confID=34&abstractID=31881.
- ↑ Socinski MA, et al. (2006). "Efficacy and safety of sunitinib in previously treated, advanced non-small cell lung cancer (NSCLC): preliminary results of a multicenter phase II trial". Journal of Clinical Oncology, 2006 ASCO Annual Meeting Proceedings Part I. 24 (18S (June 20 suppl)). Available at: http://www.asco.org/portal/site/ASCO/menuitem.34d60f5624ba07fd506fe310ee37a01d/?vgnextoid=76f8201eb61a7010VgnVCM100000ed730ad1RCRD&vmview=abst_detail_view&confID=40&abstractID=34252.
- ↑ Kulke MH, et al. "A Phase 2 Study to Evaluate the Efficacy of SU11248 in Patients with Unresectable Neuroendocrine Tumors". Presented at ASCO 2005. Available at: http://www.asco.org/portal/site/ASCO/menuitem.34d60f5624ba07fd506fe310ee37a01d/?vgnextoid=76f8201eb61a7010VgnVCM100000ed730ad1RCRD&vmview=abst_detail_view&confID=34&abstractID=33268.
- ↑ "In Gene Sequencing Treatment for Leukemia, Glimpses of the Future". Archived from the original on 2021-04-28. Retrieved 2021-07-06.
- ↑ "GEN | News Highlights: FDA Expands Sutent Label to Include Pancreatic Neuroendocrine Tumors". Archived from the original on 2016-03-04. Retrieved 2021-07-06.
External links
| External sites: | |
|---|---|
| Identifiers: |
- "Sunitinib". National Cancer Institute. Archived from the original on 2020-10-15. Retrieved 2021-07-06.
- Pages using duplicate arguments in template calls
- CS1 maint: date format
- Drugs with non-standard legal status
- Chemical articles with unknown parameter in Infobox drug
- Chemical articles without CAS registry number
- Articles without EBI source
- Chemical pages without ChemSpiderID
- Chemical pages without DrugBank identifier
- Articles without KEGG source
- Articles without UNII source
- Multiple chemicals in Infobox drug
- Chemicals using indexlabels
- Drugs missing an ATC code
- Drug has EMA link
- Drugboxes which contain changes to verified fields
- Drugboxes which contain changes to watched fields
- All articles with unsourced statements
- Articles with unsourced statements from October 2015
- Articles with invalid date parameter in template
- Articles with unsourced statements from September 2017
- All articles with specifically marked weasel-worded phrases
- Articles with specifically marked weasel-worded phrases from September 2017
- Receptor tyrosine kinase inhibitors
- Pfizer brands
- Fluoroarenes
- Indoles
- Pyrroles
- Diethylamino compounds
- RTT