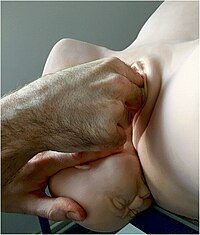
Shoulder dystocia
| Shoulder dystocia | |
|---|---|
 | |
| Suprapubic pressure being used in a shoulder dystocia | |
| Specialty | Obstetrics |
| Symptoms | Retraction of the babies head back into the vagina[1] |
| Complications | Baby: Brachial plexus injury, clavicle fracture[2] Mother: Vaginal or perineal tears, postpartum bleeding[3] |
| Risk factors | Gestational diabetes, previous history of the condition, operative vaginal delivery, obesity in the mother, an overly large baby, epidural anesthesia[2] |
| Diagnostic method | Body fails to deliver within one minute of the head[2] |
| Treatment | Pushing the mothers legs outward and upward, pushing on the abdomen above the pubic bone, manually rotate the babies shoulders, placing the women on all fours[3][2] |
| Frequency | ~ 1% of vaginal births[2] |
Shoulder dystocia is when, after vaginal delivery of the head, the baby's anterior shoulder gets caught above the mother's pubic bone.[3][1] Signs include retraction of the baby's head back into the vagina, known as "turtle sign".[1] Complications for the baby may include brachial plexus injury, or clavicle fracture.[2][1] Complications for the mother may include vaginal or perineal tears, postpartum bleeding, or uterine rupture.[3][1]
Risk factors include gestational diabetes, previous history of the condition, operative vaginal delivery, obesity in the mother, an overly large baby, and epidural anesthesia.[2] It is diagnosed when the body fails to deliver within one minute of delivery of the baby's head.[2] It is a type of obstructed labour.[4]
Shoulder dystocia is an obstetric emergency.[3] Initial efforts to release a shoulder typically include: with a woman on her back pushing the legs outward and upward, pushing on the abdomen above the pubic bone, and making a cut in the vagina.[3] If these are not effective, efforts to manually rotate the baby's shoulders or placing the women on all fours may be tried.[3][2] Shoulder dystocia occurs in approximately 0.4% to 1.4% of vaginal births.[2] Death as a result of shoulder dystocia is very uncommon.[1]
Signs and symptoms
One characteristic of a minority of shoulder dystocia deliveries is the turtle sign, which involves the appearance and retraction of the baby's head (analogous to a turtle withdrawing into its shell), and a red, puffy face. This occurs when the baby's shoulder is obstructed by the maternal pelvis.
Complications
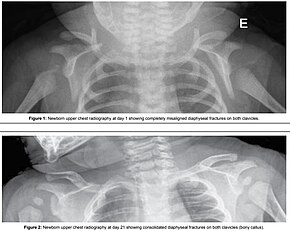
One complication of shoulder dystocia is damage to the upper brachial plexus nerves. These supply the sensory and motor components of the shoulder, arm, and hands. The ventral roots (motor pathway) are most prone to injury. The cause of injury to the baby is debated, but a probable mechanism is manual stretching of the nerves, which in itself can cause injury. Excess tension may physically tear the nerve roots out from the neonatal spinal column, resulting in total dysfunction.
Possible complications include:
- Neonatal complications:
- Maternal complications:[5]
- Postpartum bleeding (11%)
- Perineal lacerations that extend into the anal sphincter
- Pubic symphysis separation
- Neuropathy of lateral femoral cutaneous nerve
- Uterine rupture
Risk factors
About 16% of deliveries where shoulder dystocia occurs have conventional risk factors.[citation needed] These include diabetes,[6] fetal macrosomia, and maternal obesity.[7][8]
Risk factors:[9]
- Age >35
- Short in stature
- Small or abnormal pelvis
- More than 42 weeks gestation
- Estimated fetal weight >4,500 g
- Maternal diabetes (2–4 fold increase in risk)
Factors which increase the risk/are warning signs:[citation needed]
- Need for oxytocics
- Prolonged first or second stage of labour
- Turtle sign (head bobbing in the second stage)
- Failure to restitute
- No shoulder rotation or descent
- Instrumental delivery
For women with a previous shoulder dystocia, the risk of recurrence is at least 10%.[5]
Management
The steps to treating a shoulder dystocia are outlined by the mnemonic ALARMER:[10]
- Ask for help.[2] This involves asking for the help of an obstetrician, anesthesia, and for pediatrics for subsequent resuscitation of the infant that may be needed if the methods below fail;
- Leg hyperflexion and abduction at the hips (McRoberts maneuver);[2]
- Anterior shoulder disimpaction (suprapubic pressure);[10]
- Rotation of the shoulder (Rubin maneuver);[10]
- Manual delivery of posterior arm;[10]
- Episiotomy;[10]
- Roll over on all fours.[10]
Typically the procedures are performed in the order listed and the sequence ends whenever a technique is successful.[10] Intentional fracturing of the clavicle is another possibility at non-operative vaginal delivery prior to Zavanelli's maneuver or symphysiotomy, both of which are considered extraordinary treatment measures. Pushing on the fundus is not recommended.[1]
Simulation training of health care providers to prevent delays in delivery when a shoulder dystocia prevents is useful.[11]
Procedures
A number of labor positions and maneuvers are sequentially performed in attempt to facilitate delivery. These include:[10]
- McRoberts maneuver;[12][13] involves hyperflexing the mother's legs tightly to her abdomen. This widens the pelvis, and flattens the spine in the lower back (lumbar spine). If this maneuver does not succeed, an assistant applies pressure on the lower abdomen (suprapubic pressure), and the delivered head is also gently pulled. The technique is effective in about 42% of cases;
- Suprapubic pressure (or Rubin I);[14]
- Rubin II or posterior pressure on the anterior shoulder, which would bring the baby into an oblique position with the head somewhat towards the vagina;[15]
- Active delivery of the anterior arm
-
Step 1: Index and middle fingers insertion with the hand opposite the baby's face
-
Step 2: Baby's head slightly tilted downward with the free hand
-
Step 3: Two fingers are placed on the humerus like a splint
-
Step 4: Baby's hand appears under the maternal pubic symphysis, allowing the anterior arm to be delivered
- Wood's screw maneuver which leads to turning the anterior shoulder to the posterior and vice versa (somewhat the opposite of Rubin II maneuver);[16]
- Jacquemier's maneuver (also called Barnum's maneuver), or delivery of the posterior shoulder first, in which the forearm and hand are identified in the birth canal, and gently pulled;
- Gaskin maneuver involves moving the mother to an all fours position with the back arched, widening the pelvic outlet.[17][18]
More drastic maneuvers include:
- Zavanelli's maneuver, which involves pushing the baby's head back in (internal cephalic replacement) followed by a cesarean section;[19]
- Intentional causing clavicular fractures, which reduces the diameter of the shoulders that requires to pass through the birth canal;[2]
- Maternal symphysiotomy, which makes the opening of the birth canal laxer by breaking the connective tissue between the two pubes bones;[2]
- Abdominal rescue, described by O'Shaughnessy, where a hysterotomy facilitates vaginal delivery of the impacted shoulder.[20]
Epidemiology
Shoulder dystocia occurs in about 0.15% to 4% of term vaginal births.[21]
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 Gherman, Robert B.; Gonik, Bernard (2009). "Shoulder Dystocia". The Global Library of Women's Medicine. doi:10.3843/GLOWM.10137.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 Dahlke, JD; Bhalwal, A; Chauhan, SP (June 2017). "Obstetric Emergencies: Shoulder Dystocia and Postpartum Hemorrhage". Obstetrics and Gynecology Clinics of North America. 44 (2): 231–243. doi:10.1016/j.ogc.2017.02.003. PMID 28499533.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 "Shoulder dystocia" (PDF). Royal College of Obstetricians and Gynaecologists. 2013. Archived (PDF) from the original on 24 October 2020. Retrieved 3 October 2018.
- ↑ Buck, Carol J. (2016). 2017 ICD-10-CM Standard Edition - E-Book. Elsevier Health Sciences. p. 108. ISBN 9780323484572. Archived from the original on 2021-04-30. Retrieved 2018-10-03.
- ↑ 5.0 5.1 "Practice Bulletin No. 178 Summary: Shoulder Dystocia". Obstetrics & Gynecology. 129 (5): 961–962. 2017-05-01. doi:10.1097/AOG.0000000000002039. ISSN 0029-7844. Archived from the original on 2020-10-27. Retrieved 2020-04-20.
- ↑ Jouatte F, Aitken B, Dufour P, et al. (December 1999). "Diabète antérieur à la grossesse, à propos de 143 observations" [Diabetes before pregnancy, apropos of 143 cases]. Contracept Fertil Sex (in French). 27 (12): 845–52. PMID 10676041.
{{cite journal}}: CS1 maint: unrecognized language (link) - ↑ Breeze AC, Lees CC (2004). "Managing shoulder dystocia". Lancet. 364 (9452): 2160–1. doi:10.1016/S0140-6736(04)17607-1. PMID 15610787.
- ↑ Murray; McKinney (2006). "Intrapartum Complications Chapter 27)". Foundations of Maternal-Newborn and Women's Health Nursing (Fifth ed.). Saunders Elsevier. p. 697. ISBN 978-1-4377-0259-0.
- ↑ Royal College of Obstetricians and Gynaecologists (March 2012). "Shoulder Dystocia" (PDF). Archived (PDF) from the original on 2017-09-18. Retrieved 2017-12-06.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ 10.0 10.1 10.2 10.3 10.4 10.5 10.6 10.7 "Obstetrical Emergencies - Shoulder Dystocia" (PDF). PSBC. 2011. Archived (PDF) from the original on 13 July 2019. Retrieved 3 October 2018.
- ↑ Gilstrop, M; Hoffman, MK (December 2016). "An Update on the Acute Management of Shoulder Dystocia". Clinical Obstetrics and Gynecology. 59 (4): 813–819. doi:10.1097/GRF.0000000000000240. PMID 27681692.
- ↑ Stallard TC, Burns B (August 2003). "Emergency delivery and perimortem C-section". Emerg. Med. Clin. North Am. 21 (3): 679–93. doi:10.1016/S0733-8627(03)00042-7. PMID 12962353.
- ↑ Kish & Collea 2003, p. 382
- ↑ "Shoulder Dystocia Management". Archived from the original on 2007-10-08. Retrieved 2007-11-28.
- ↑ Baxley EG, Gobbo RW (April 2004). "Shoulder dystocia". Am Fam Physician. 69 (7): 1707–14. PMID 15086043. Archived from the original on 2021-08-29. Retrieved 2013-03-29.
- ↑ "Fetal Dystocia: Abnormalities and Complications of Labor and Delivery: Merck Manual Professional". Archived from the original on 2007-12-02. Retrieved 2007-11-28.
- ↑ Murray, Michelle; Huelsmann, Gayle (2008-12-15). Labor and Delivery Nursing: Guide to Evidence-Based Practice. Springer Publishing Company. pp. 143–144. ISBN 978-0-8261-1803-5.
- ↑ Murray, Michelle; Huelsmann, Gayle (2008-12-15). Labor and Delivery Nursing. Labor and Delivery Nursing: A Guide to Evidence-Based Practice. Springer Publishing. ISBN 978-0-8261-1803-5. Retrieved 2009-02-01.
- ↑ Fernandez H, Papiernik E (1990). "Manoeuvre de Zavanelli : application à la rétention de tête dernière au détroit supérieur : à propos d'une observation" [The Zavanelli maneuver: use during breech retention of the head in the birth canal. Apropos of a case]. J Gynecol Obstet Biol Reprod (Paris) (in French). 19 (4): 483–5. PMID 2380511.
{{cite journal}}: CS1 maint: unrecognized language (link) - ↑ O'Shaughnessy MJ (October 1998). "Hysterotomy facilitation of the vaginal delivery of the posterior arm in a case of severe shoulder dystocia". Obstet Gynecol. 92 (4 Pt 2): 693–5. doi:10.1016/S0029-7844(98)00153-7. PMID 9764668.
- ↑ "Shoulder Dystocia: Overview, Indications, Contraindications". 21 June 2017. Archived from the original on 1 April 2019. Retrieved 2 April 2019.
{{cite journal}}: Cite journal requires|journal=(help)
External links
| Classification |
|---|
- GLOWM video showing management of shoulder dystocia Archived 2021-01-26 at the Wayback Machine
- Pages with script errors
- CS1 maint: unrecognized language
- CS1 errors: missing periodical
- Harv and Sfn no-target errors
- All articles with unsourced statements
- Articles with unsourced statements from January 2020
- Articles with invalid date parameter in template
- Webarchive template wayback links
- Complications of labour and delivery
- Medical mnemonics
- RTT
- WHRTT