Amniotic fluid embolism
| Amniotic fluid embolism | |
|---|---|
| Other names: Anaphylactoid syndrome of pregnancy[1] | |
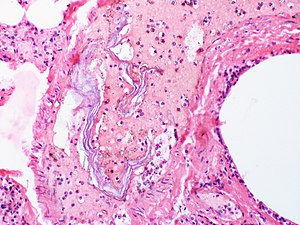 | |
| Skin cells are present in the blood vessels of this case of amniotic fluid embolism. | |
| Specialty | Obstetrics, anesthesiology |
| Symptoms | Headache, chest pain, nausea, shortness of breath[2] |
| Complications | Bleeding problems, coma, cardiac arrest[2] |
| Usual onset | Sudden[2] |
| Causes | Allergic reaction to fetal tissue that has entered the mother's blood stream[2] |
| Risk factors | Unclear[2] |
| Diagnostic method | Based on symptoms, after ruling out other causes[2] |
| Differential diagnosis | Eclampsia, pulmonary embolism, placental abruption, peripartum cardiomyopathy, air embolism, hemorrhagic shock[2][1] |
| Treatment | Supportive care, rapid delivery[2][3] |
| Frequency | 1 in 40,000 deliveries[3] |
| Deaths | ~40% risk of death[3] |
Amniotic fluid embolism (AFE) is a complication around childbirth in which fetal tissue enters the blood stream of the mother resulting in health problems.[2][4] Onset is rapid.[2] Initial symptoms may include headache, chest pain, nausea, and shortness of breath.[2] This may be followed by bleeding problems, coma, or cardiac arrest.[2]
Risk factors are unclear; though those affected may more commonly have allergies.[1][2] The underlying mechanism is believed to involve an allergic reaction to fetal tissue that has entered the mother's blood.[2] Diagnosis is based on symptoms, particularly low oxygen and low blood pressure, after ruling out other possible causes.[1][2]
Treatment is generally supportive care.[3] This may include oxygen therapy, intubation and ventilation, blood transfusions, or cardiopulmonary resuscitation (CPR).[2] If delivery has not yet occurred, rapid delivery may be required.[2] Of those who survive, some have brain damage while others return to normal.[2]
Amniotic fluid embolism occurs in about 1 in 40,000 deliveries.[3] Older mothers are more commonly affected.[1] Of those affected about 40% die.[3] It is a relatively common cause of death during pregnancy, representing about 7.5% of such deaths in the United States.[3][5] The condition was first described in 1926.[3]
Signs and symptoms
Symptoms often include sudden onset of low oxygen, low blood pressure, and profuse bleeding around the time of giving birth.[1] Though symptoms can be profound, they can also be variable.[6]
While usually occurring around the time of birth; rarely it may occur with amniocentesis or abortion procedures.[1]
Causes

The disorder occurs during the last stages of labor if amniotic fluid enters the circulatory system of the mother via tears in the placental membrane or uterine vein rupture.[7] Fetal cells are found in the maternal circulation. When the fetal cells and amniotic fluid enter the bloodstream, reactions occur that affect blood clotting. Disseminated intravascular coagulation occurs and results in serious bleeding.[8] The condition can also develop after elective abortion, amniocentesis, cesarean delivery, or trauma. Small lacerations in the lower reproductive tract are also associated with AFE.[6]
It is unclear if induction of labor affects the risk.[3] Mothers who are older are more commonly affected as are those carrying more than one baby.[3]
Diagnosis
AFE is diagnosed when other causes have been excluded. Fetal squamous cells or other fetal tissues, including meconium, have been found in the maternal circulation after the event. Diagnosis is also based upon symptoms.[6]
Treatment
Treatment is generally supportive care.[3] This may include oxygen therapy, intubation and ventilation, blood transfusions, or cardiopulmonary resuscitation (CPR).[2] If delivery has not yet occurred, rapid delivery may be required.[2]
After deliver, oxytocin should be used to promote contraction of the uterus.[1] Tranexamic acid may be used for bleeding.[1] Excessive intravenous normal saline should be avoided.[1]
Medications that improve blood pressure and decrease pulmonary pressure such as milrinone and dubutamine are commonly used.[1] Norepinephrine may also be used.[1] ECMO may also be an option.[1]
Prognosis
About 15 to 50% of women both survive and do well.[1] Death of the baby occurs in over half of cases with many of the babies who survive having neurological problems.[1]
Epidemiology
Amniotic fluid embolism occurs in about 1 in 40,000 deliveries.[3] Though rare, it comprises 10% of all maternal deaths.[6]
History
This rare complication has been recorded seventeen times prior to 1950. The complication was originally described in 1926 by J. R. Meyer at the University of Sao Paulo.[9][10] A 1941 case study of eight autopsies of pregnant women who died suddenly during childbirth by Clarence Lushbaugh and Paul Steiner enabled widespread recognition of the diagnosis within the medical community, and was eventually republished as a landmark paper in the Journal of the American Medical Association.[10][11]
The name "anaphylactoid syndrome of pregnancy" was suggested in 1995 as no significant embolism is believed to occur.[1] It is also believed to be unrelated to amniotic fluid.[4]
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 Coggins, Ashley S.; Gomez, Erin; Sheffield, Jeanne S. (September 2022). "Pulmonary Embolism and Amniotic Fluid Embolism". Obstetrics and Gynecology Clinics of North America. 49 (3): 439–460. doi:10.1016/j.ogc.2022.02.015. PMID 36122978.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 2.17 2.18 2.19 "Amniotic Fluid Embolism - Symptoms, Causes, Treatment | NORD". rarediseases.org. Archived from the original on 10 January 2023. Retrieved 29 June 2023.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 Shamshirsaz, AA; Clark, SL (December 2016). "Amniotic Fluid Embolism". Obstetrics and gynecology clinics of North America. 43 (4): 779–790. doi:10.1016/j.ogc.2016.07.001. PMID 27816160.
- ↑ 4.0 4.1 Combs, C. Andrew; Montgomery, Douglas M.; Toner, Lorraine E.; Dildy, Gary A. (April 2021). "Society for Maternal-Fetal Medicine Special Statement: Checklist for initial management of amniotic fluid embolism". American Journal of Obstetrics and Gynecology. 224 (4): B29–B32. doi:10.1016/j.ajog.2021.01.001.
- ↑ "Amniotic Fluid Embolism: Background, Pathophysiology, Etiology". Emedicine. 15 March 2023. Archived from the original on 13 March 2023. Retrieved 29 June 2023.
- ↑ 6.0 6.1 6.2 6.3 Stein, Paul (2016). Pulmonary embolism. Chichester, West Sussex, UK Hoboken, NJ: John Wiley & Sons Inc. ISBN 9781119039099.
- ↑ Vinay Kumar; Abul K. Abbas; Nelson Fausto; Jon C. Aster (2014-08-27). Robbins and Cotran Pathologic Basis of Disease, Professional Edition E-Book. Elsevier Health Sciences. pp. 129–. ISBN 978-0-323-29639-7. Archived from the original on 2023-06-30. Retrieved 2023-02-19.
- ↑ "Disseminated Intravascular Coagulation". The Lecturio Medical Concept Library. Archived from the original on 12 July 2021. Retrieved 12 July 2021.
- ↑ "CEArticlePrint". nursingcenter.com. Archived from the original on 2021-01-14. Retrieved 2021-02-25.
- ↑ 10.0 10.1 Caeiro, Ana Filipa Cabrita; Ramilo, Irina Dulce Tapadinhas Matos; Santos, Ana Paula; Ferreira, Elizabeth; Batalha, Isabel Santos (July 2017). "Amniotic Fluid Embolism. Is a New Pregnancy Possible? Case Report". Brazilian Journal of Gynecology and Obstetrics. 39 (7): 369–372. doi:10.1055/s-0037-1601428. PMID 28464190.
- ↑ Steiner, Paul E.; Lushbaugh, Clarence C. (October 11, 1941). "Landmark article, Oct. 1941: Maternal pulmonary embolism by amniotic fluid as a cause of obstetric shock and unexpected deaths in obstetrics". Journal of the American Medical Association. 255 (16): 2187–2303. doi:10.1001/jama.255.16.2187. PMID 3514978. Archived from the original on February 21, 2023. Retrieved February 19, 2023 – via PubMed.
External links
- Checklist for initial management of amniotic fluid embolism Archived 2023-06-30 at the Wayback Machine
| Classification | |
|---|---|
| External resources |