Postpartum thyroiditis
| Postpartum thyroiditis | |
|---|---|
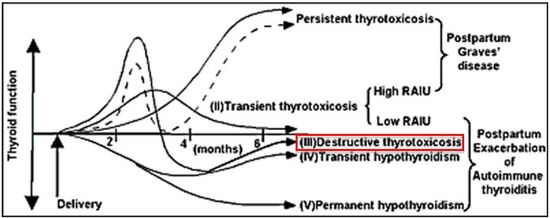 | |
| Postpartum thyroiditis-various clinical courses of thyroid dysfunction after delivery[1] | |
| Specialty | Endocrinology |
Postpartum thyroiditis refers to thyroid dysfunction occurring in the first 12 months after pregnancy[2] and may involve hyperthyroidism, hypothyroidism or the two sequentially. According to the National Institute of Health, postpartum thyroiditis affects about 8% of pregnancies.[3] There are, however, different rates reported globally. This is likely due to the differing amounts of average postpartum follow times around the world, and due to humans' own innate differences. For example, in Bangkok, Thailand the rate is 1.1%, but in Brazil it is 13.3%.[3] The first phase is typically hyperthyroidism. Then, the thyroid either returns to normal or a woman develops hypothyroidism. Of those women who experience hypothyroidism associated with postpartum thyroiditis, one in five will develop permanent hypothyroidism requiring lifelong treatment.
Postpartum thyroiditis is believed to result from the modifications to the immune system necessary in pregnancy, and histologically is a subacute lymphocytic thyroiditis. The process is normally self-limiting, but when conventional antibodies are found there is a high chance of this proceeding to permanent hypothyroidism. Postpartum thyroiditis is a member of the group of thyroiditis conditions known as resolving thyroiditis.
Signs and symptoms
The initial phase of hyperthyroid symptoms occurs transiently about two to six months postpartum.[4] Typical symptoms include irritability, nervousness, palpitations, and heat intolerance. Hormonal disturbances during this phase tend to occur with lower intensity compared with the hypothyroid phase.[4] As a result, the hyperthyroid phase may pass undetected. The second phase of hypothyroid symptoms is also transient and can occur anytime within the three- to twelve-month period postpartum.[4] Women in this phase experience low energy, poor memory, impaired concentration, carelessness, dry skin, cold intolerance, and general aches and pains. After one year postpartum, euthyroid function resumes. Any case with hypothyroid symptoms extending beyond one year postpartum is not considered postpartum thyroiditis.[4]
Women who test positive for thyroid antibodies may be at increased risk of developing symptoms associated with postpartum depression than women without thyroid antibodies.[5]
Cause
During pregnancy, immunologic suppression occurs which induces tolerance to the presence of the fetus.[6] Without this suppression, the fetus would be rejected causing miscarriage.[6] As a result, following delivery, the immune system rebounds causing levels of thyroids antibodies to rise in susceptible women.[7]
Specifically, the immunohistological features of susceptible women are indicated by:[6]
- antibodies to thyroglobulin (TgAb)
- antibodies to thyroid peroxidase (TPOAb)
- increase in TPOAb subclasses IgG1-IgG3
- lymphocyte infiltration and follicle formation within thyroid gland (Hashimoto's thyroiditis)
- T-cell changes (increased CD4:CD8 ratio)
- TSH-receptor antibodies (TSH-R Abs)
Diagnosis
This condition is commonly undiagnosed by physicians due to either unfamiliarity with the disease, the subtlety of symptoms, or the attribution of the symptoms to the stresses of having a newborn.[7] Usual screening begins with assessing the thyroid stimulating hormone (TSH) level. A suppressed TSH could represent the hyperthyroid phase, but warrants further testing to investigate for possible Graves' disease.[7] A normal TSH with persistent symptoms could represent the shift between phases and requires repeat testing 4–6 weeks later; an elevated TSH at this time could indicate the hypothyroid phase.[7]
Treatment
For most women, the hyperthyroid phase presents with very mild symptoms or is asymptomatic; intervention is usually not required. If symptomatic cases require treatment, a short course of beta-blockers would be effective.[4]
Assessing treatment for the hypothyroid is more complex. Women with symptoms or a very high TSH level, or both, are usually prescribed a course of levothyroxine.[4] Asymptomatic women with slightly elevated TSH levels who are planning subsequent pregnancies, should consider a course of treatment until completion of the family to avoid possible developmental complications in future children.[4] Otherwise, treatment could be discontinued after one year postpartum.[citation needed]
Prevalence
Women with type I diabetes mellitus have a threefold increase in the prevalence of postpartum thyroiditis than non-diabetic women in the same region.[4]
According to Johns Hopkins, 3 in 100 women develop postpartum thyroiditis. Some risk factors include antithyroid antibodies, type 1 diabetes, history of thyroid problems, and family history of thyroid problems. According to the National Institute of Health, postpartum thyroiditis is especially common in Pakistan because it is an iodine-deficient country.[citation needed]
References
- ↑ Inaba, Hidefumi; Akamizu, Takashi (2000). "Postpartum Thyroiditis". Endotext. MDText.com, Inc. Archived from the original on 8 August 2023. Retrieved 5 August 2023.
- ↑ Muller AF, Drexhage HA, Berghout A (October 2001). "Postpartum thyroiditis and autoimmune thyroiditis in women of childbearing age: recent insights and consequences for antenatal and postnatal care". Endocr. Rev. 22 (5): 605–30. doi:10.1210/edrv.22.5.0441. PMID 11588143.
{{cite journal}}: CS1 maint: url-status (link) - ↑ 3.0 3.1 Keely, Erin Joanne (March 2011). "Postpartum thyroiditis: an autoimmune thyroid disorder which predicts future thyroid health". Obstetric Medicine. 4 (1): 7–11. doi:10.1258/om.2010.100041. ISSN 1753-495X. PMC 4989649. PMID 27579088.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 Stagnaro-Green, A. (2004). "Postpartum thyroiditis". Best Practice & Research Clinical Endocrinology & Metabolism. 18 (2): 303–316. doi:10.1016/j.beem.2004.03.008. PMID 15157842. Archived from the original on 2018-05-11. Retrieved 2022-07-10.
- ↑ Bokhari, R.; Bhatara, V.S.; Bandettini, F.; McMillan, J.M. (1998). "Postpartum psychosis and postpartum thyroiditis". Psychoneuroendocrinology. 23 (6): 643–650. doi:10.1016/S0306-4530(98)00034-1. PMID 9802134. S2CID 28530447.
- ↑ 6.0 6.1 6.2 Premawardhana, L.D.K.E., Parkes, A.B., & Lazarus, J.H. (2004). Thyroiditis, postpartum. In Editor-in-Chief: Luciano Martini (Ed.), Encyclopedia of endocrine diseases (pp. 509–514). New York: Elsevier. doi:10.1016/B0-12-475570-4/01299-3
- ↑ 7.0 7.1 7.2 7.3 Stagnaro-Green, A. (2000). Recognizing, understanding, and treating postpartum thyroiditis. Endocrinology & Metabolism Clinics of North America, 29(2), 417–430. doi:10.1016/S0889-8529(05)70140-7
Further reading
- "Postpartum Thyroiditis." Johns Hopkins Medicine, www.hopkinsmedicine.org/health/conditions-and-diseases/postpartum-thyroiditis. Afzal, Rafia. "Thyroid disorders in pregnancy: An overview of literature from Pakistan." Indian journal of endocrinology and metabolism vol. 17,5 (2013): 943–5. doi:10.4103/2230-8210.117202
| Classification |
|---|