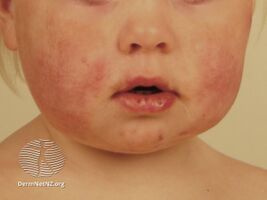
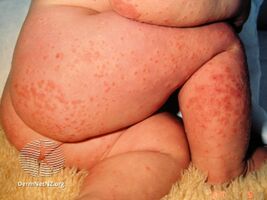
Gianotti–Crosti syndrome
| Gianotti–Crosti syndrome | |
|---|---|
| Other names: Papular acrodermatitis of childhood,[1] papulovesicular acrolocated syndrome[2]: 389 | |
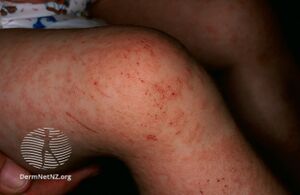 | |
| Gianotti–Crosti syndrome | |
| Pronunciation | |
| Specialty | Dermatology |
| Symptoms | Tiredness, large lymph glands, followed by multiple red small bumps[3] |
| Duration | < 6 weeks[3] |
| Causes | Hepatitis B virus, Epstein–Barr virus[3] |
| Risk factors | Under 14 years[3] |
| Medication | Steroid cream[3] |
Gianotti–Crosti syndrome, also known as infantile papular acrodermatitis, is a reaction of the skin to a viral infection.[1] It results in multiple red small bumps on the face, neck, limbs, bottom, palms and soles.[3][4] It may itch.[3] The rash is typically preceded by early symptoms of tiredness and large lymph glands.[3][5]
Hepatitis B virus and Epstein–Barr virus are the most frequently reported pathogens.[3] Other associated viruses include coxsackieviruses, echoviruses, parainfluenza viruses, cytomegalovirus and respiratory syncytial virus.[6] The time from exposure to onset of symptoms is not known.[3] Diagnosis is by symptoms, but a blood test may be requested.[3]
Applying a steroid cream may relieve the itch.[3] The bumps may become purple before resolving over 2 to 6 weeks.[3] Rarely, the glands and a large liver may persist for several months.[3]
It occurs most commonly in under-14 year olds.[3] It is named for Ferdinando Gianotti and Agostino Crosti.[7][8]
Signs and symptoms
Gianotti–Crosti syndrome mainly affects infants and young children. Children as young as 1.5 months and up to 12 years of age are reported to be affected.[9] It is generally recognized as a papular or papulovesicular skin rash occurring mainly on the face and distal aspects of the four limbs. Purpura is generally not seen but may develop upon tourniquet test. However, extensive purpura without any hemorrhagic disorder has been reported.[9] The presence of less florid lesions on the trunk does not exclude the diagnosis. Lymphadenopathy and hepatomegaly are sometimes noted. Raised AST and ALT levels with no rise in conjugated and unconjugated bilirubin levels are sometimes detectable, although the absence of such does not exclude the diagnosis. Spontaneous disappearance of the rash usually occurs after 15 to 60 days.
-
Gianotti–Crosti syndrome
-
Gianotti–Crosti syndrome
Cause
Hepatitis B virus and Epstein–Barr virus are the most frequently reported pathogens.[3] Other viruses implicated are hepatitis A virus, hepatitis C virus, cytomegalovirus,[10] coxsackievirus, adenovirus, enterovirus, rotavirus, rubella virus, HIV, and parainfluenza virus.[11]
Diagnosis
The diagnosis of Gianotti–Crosti syndrome is clinical. A validated diagnostic criteria[12][13][14] is as follows:
A patient is diagnosed as having Gianotti–Crosti syndrome if:
- On at least one occasion or clinical encounter, he/she exhibits all the positive clinical features,
- On all occasions or clinical encounters related to the rash, he/she does not exhibit any of the negative clinical features,
- None of the differential diagnoses is considered to be more likely than Gianotti–Crosti syndrome on clinical judgment, and
- If lesional biopsy is performed, the histopathological findings are consistent with Gianotti–Crosti syndrome.
The positive clinical features are:
- Monomorphous, flat-topped, pink-brown papules or papulovesicles 1-10mm in diameter.
- At least three of the following four sites involved – (1) cheeks, (2) buttocks, (3) extensor surfaces of forearms, and (4) extensor surfaces of legs.
- Being symmetrical, and
- Lasting for at least ten days.
The negative clinical features are:
- Extensive truncal lesions, and
- Scaly lesions.
Differential diagnosis
The differential diagnoses are: acrodermatitis enteropathica, erythema infectiosum, erythema multiforme, hand-foot-and-mouth disease, Henoch–Schönlein purpura, Kawasaki disease, lichen planus, papular urticaria, papular purpuric gloves and socks syndrome, and scabies.
Treatment
Gianotti-Crosti disease is a harmless and self-limiting condition, so no treatment may be required.[15] Treatment is mainly focused on controlling itching, symptomatic relief and to avoid any further complications. For symptomatic relief from itching, oral antihistamines or any soothing lotions like calamine lotion or zinc oxide may be used. If there are any associated conditions like streptococcal infections, antibiotics may be required.[12][13][14][15]
See also
References
- ↑ 1.0 1.1 Oakley, Amanda (2022). "2.3.6. Infections: infantile papular acrodermatitis". Dermatology Made Easy (2nd ed.). Scion Publishing Ltd. pp. 126–127. ISBN 978-1-914961-21-2. Archived from the original on 2023-07-01. Retrieved 2023-05-18.
- ↑ James, William D.; Berger, Timothy G.; et al. (2006). Andrews' Diseases of the Skin: clinical Dermatology. Saunders Elsevier. ISBN 0-7216-2921-0.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 3.14 3.15 Morris-Jones, Rachael (2019). "14. Viral infections". In Morris-Jones, Rachael (ed.). ABC of Dermatology (7th ed.). Hoboken: Wiley Blackwell. p. 120. ISBN 978-1-119-48899-6.
- ↑ "Gianotti-crosti syndrome, papulovesicular acrodermatitis. DermNet NZ". Archived from the original on 2016-07-11. Retrieved 2021-05-18.
- ↑ Snowden, Jessica; Rice, Ashley S.; O'Shea, Noreen E. (2023). "Papular Acrodermatitis". StatPearls. StatPearls Publishing. Archived from the original on 2023-05-17. Retrieved 2023-05-18.
- ↑ Michaels, Marian `G.; Williams, John V. (2023). "13. Infectious diseases". In Zitelli, Basil J.; McIntire, Sara C.; Nowalk, Andrew J.; Garrison, Jessica (eds.). Zitelli and Davis' Atlas of Pediatric Physical Diagnosis (8th ed.). Philadelphia: Elsevier. p. 468. ISBN 978-0-323-77788-9. Archived from the original on 2022-12-17. Retrieved 2022-12-18.
- ↑ synd/4051 at Who Named It?
- ↑ CROSTI A, GIANOTTI F (November 1957). "[Eruptive dermatosis of probable viral origin situated on the acra.]". Dermatologica (in français). 115 (5): 671–7. doi:10.1159/000256031. PMID 13500859.
- ↑ 9.0 9.1 Sarma, N; Sarkar UK (Jan–Mar 2013). "Hemorrhagic Gianotti-Crosti Syndrome in a One and Half Month old Infant: An Extremely Unusual Presentation". Indian J Dermatol. 58 (1): 65–67. doi:10.4103/0019-5154.105313. PMC 3555378. PMID 23372217. Archived from the original on 2016-09-10. Retrieved 2021-05-18.
- ↑ Haki M, Tsuchida M, Kotsuji M, et al. (October 1997). "Gianotti-Crosti syndrome associated with cytomegalovirus antigenemia after bone marrow transplantation". Bone Marrow Transplantation. 20 (8): 691–3. doi:10.1038/sj.bmt.1700945. PMID 9383234.
- ↑ Chandrasekaran M, Mukherjee S (September 2007). "Gianotti Crosti syndrome". Indian Pediatrics. 44 (9): 695. PMID 17921560.
- ↑ 12.0 12.1 Chuh, AA (September 2001). "Diagnostic criteria for Gianotti-Crosti syndrome: a prospective case-control study for validity assessment". Cutis; Cutaneous Medicine for the Practitioner. 68 (3): 207–13. PMID 11579787.
- ↑ 13.0 13.1 Chuh, Antonio; Lee, Albert; Zawar, Vijay (1 September 2004). "The Diagnostic Criteria of Gianotti-Crosti Syndrome: Are They Applicable to Children in India?". Pediatric Dermatology. 21 (5): 542–547. doi:10.1111/j.0736-8046.2004.21503.x. PMID 15461758.
- ↑ 14.0 14.1 Chuh, Antonio; Zawar, Vijay; Law, Michelle; Sciallis, Gabriel (2 January 2012). "Gianotti-Crosti syndrome, pityriasis rosea, asymmetrical periflexural exanthem, unilateral mediothoracic exanthem, eruptive pseudoangiomatosis and papular-purpuric gloves and socks syndrome: a brief review and arguments for diagnostic criteria". Infectious Disease Reports. 4 (1): 12. doi:10.4081/idr.2012.e12. PMC 3892651. PMID 24470919.
- ↑ 15.0 15.1 "Gianotti-crosti syndrome. Dermatalk". Archived from the original on 2018-03-11. Retrieved 2021-05-18.
Further reading
- Gianotti, F. (October 1976). "[Infantile papular acrodermatitis. Acrodermatitis papulosa and the infantile papulovesicular acrolocalized syndrome]". Der Hautarzt; Zeitschrift Fur Dermatologie, Venerologie, Und Verwandte Gebiete. 27 (10): 467–472. ISSN 0017-8470. PMID 993019. Archived from the original on 2023-07-01. Retrieved 2023-05-18.
External links
| Classification | |
|---|---|
| External resources |