Fifth disease
| fifth disease | |
|---|---|
| Other names: Erythema infectiosum, human erythrovirus infection, slapped cheek syndrome, slapcheek, slap face, slapped face[1][2][3] | |
 | |
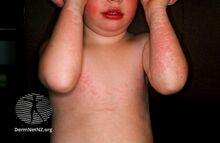
| 16-month-old with the typical rash | |
| Specialty | Infectious disease |
| Symptoms | None, fever, rash, runny nose[4][5][6] |
| Complications | Aplastic anemia, pain in multiple joints, hydrops fetalis[4] |
| Usual onset | 4 days to 2 wks after exposure;[7][5] 5 to 15 years old[4] |
| Duration | 6 weeks[3] |
| Causes | Parvovirus B19[4] |
| Diagnostic method | Based on symptoms,[3] detection of parvovirus IgM or DNA[6] |
| Differential diagnosis | Measles, rubella, roseola, scarlet fever[4] |
| Medication | Paracetamol (acetaminophen), NSAIDs[4] |
| Frequency | Common in school children[6] |
Fifth disease, also known as erythema infectiosum, is a type of viral infection that most commonly occurs in children.[4] The most common symptoms are a low grade fever and rash.[4] Other symptoms may include joint pain, diarrhea, runny nose, vomiting, and headache.[4][5] The rash generally starts in the latter part of the infection, involves the cheeks and spreads to chest and arms.[4] One in five have no symptoms.[6] Complications may include aplastic anemia, pain in multiple joints, and during pregnancy hydrops fetalis.[4]
It is caused by infection by parvovirus B19.[8] It is typically spread via the respiratory route, though may also spread from mother to child during pregnancy and via blood transfusions.[4] Diagnosis is usually based on the symptoms, though it may be confirmed with blood tests.[3]
Treatment is symptomatic and supportive which may include paracetamol (acetaminophen) and NSAIDs.[4] Symptoms generally last for 1 to 3 weeks.[9][7] After recovery people generally do not get the disease again.[5]
Fifth disease is common and typically occurs in those between the ages of 5 and 15.[3][4] Early descriptions of the disease data from at least 1889 by Tschamer and maybe as early as 1799 by Robert Willan.[10][11] In 1905 it was classified as the "fifth rash disease" in the standard list of rash-causing childhood diseases.[5][11]
Signs and symptoms
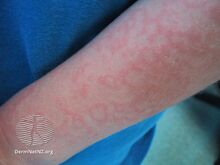
Fifth disease starts with a low-grade fever, headache, rash, and cold-like symptoms, such as a runny or stuffy nose.[4] These symptoms pass, then a few days later, the rash appears. The bright red rash most commonly appears in the face, particularly the cheeks. This is a defining symptom of the infection in children (hence the name "slapped cheek disease"). Occasionally, the rash will extend over the bridge of the nose or around the mouth. In addition to red cheeks, children often develop a red, lacy rash on the rest of the body, with the upper arms, torso, and legs being the most common locations. The rash typically lasts a few days and may itch; some cases have been known to last for several weeks. Patients are usually no longer infectious once the rash has appeared.[1][2] The rash usually may be itchy especially on the bottom of the feet.[5]
Onset of symptoms is generally within two weeks of exposure.[5]
Teenagers and adults may present with a self-limited arthritis. It manifests in painful swelling of the joints that feels similar to arthritis. Older children and adults with fifth disease may have difficulty in walking and in bending joints such as wrists, knees, ankles, fingers, and shoulders.[1][2]
Complications
The disease is usually mild,[13] but in certain risk groups, it can have serious consequences:
- In pregnant women, infection in the first trimester has been linked to hydrops fetalis, causing spontaneous miscarriage.
- In people with sickle-cell disease or other forms of chronic hemolytic anemia such as hereditary spherocytosis, infection can precipitate an aplastic crisis.[1][2]
- Those who are immunocompromised (HIV/AIDS, chemotherapy) may be at risk for complications if exposed.[14]
Causes
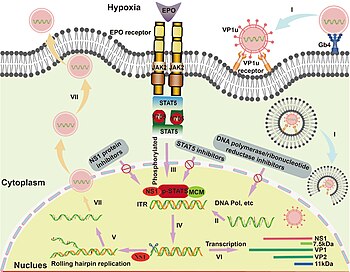
Fifth disease is caused by parvovirus B19, which only infects humans.[17]
Parvovirus B19 (B19V) is a small, single-stranded, non-enveloped DNA virus. Binding of B19V capsid to the cellular receptor globoside (Gb4Cer) results in a cascade of structural changes and subsequent signal transduction processes facilitating the entry of parvovirus B19 into the host cell. After gaining access to the host cell, B19V binds to glycosphingolipid globoside (blood group P antigen) targeting erythroid lineage in the bone marrow. Replication of viral genome and release of virus from infected cells lead to various complex effects on host's cellular environment such as induction of DNA damage, hijack of cell cycle and apoptosis (killing of infected cells).[18][19]
B19V DNA has been found in a wide range of tissues in healthy and diseased individuals indicates the persistence of B19V infection. According to a clinical microbiology review published by Jianming Qiu "Persistence of viral DNA has been detected in up to 50% of biopsy specimens of the spleen, lymph nodes, tonsils, liver, heart, synovial tissues, skin, brain, and testes, for decades after infection."[20]
Recovery from parvovirus B19 infection is achieved by production of IgM antibodies which are specific for virus and are generated 10–12 days after infection.[19]
Spread
Fifth disease is transmitted primarily by respiratory secretions (saliva, mucus, etc.), but can also be spread by contact with infected blood. The incubation period is usually between 4 and 21 days. Individuals with fifth disease are most infectious before the onset of symptoms ( school children, day-care workers, teachers, and parents are most likely to be exposed to the virus). When symptoms are evident, the risk of transmission is small; therefore, symptomatic individuals do not need to be isolated.[1][2]
Individuals with aplastic anemia, have a very high viral load[21]
Diagnosis
In terms of the diagnosis for Fifth disease, we find this can be obtained via bloodwork for specific antibodies[21]
Prevention
There is no vaccine or medicine that can prevent the disease.[5] The risk of disease can be reduced by washing hands, covering the mouth when you cough, not touching their eyes, nose, or mouth, avoiding close contact with people who are sick, and staying home when you are sick.[5]
Treatment
Treatment is supportive, and the infection is generally self-limiting. Medications that may decrease symptoms include NSAIDs and paracetamol (acetaminophen).
Epidemiology
Any age may be affected, although it is most common in children aged 5 to 15 years.[22] By the time adulthood is reached, about half the population will have become immune following infection at some time in their past.[1][2] Outbreaks can arise especially in nursery schools, preschools, and elementary schools. Infection is an occupational risk for school and day-care personnel.[23] No vaccine is available for human parvovirus B19,[2] though attempts have been made to develop one.[24]
History
A possible description of the condition by Robert Willan occurred in 1799 and was named "rubeola, sine catarrho".[10] It was better defined by Anton Tschamer in 1889 as a rubella variant (Ortliche Rotheln), identified as a distinct condition in 1896 by Theodor Escherich, and given the name "erythema infectiosum" in 1899.[25] The term "Fifth disease" was coined in 1905 by the Russian-French physician Léon Cheinisse (1871-1924), who proposed a numbered classification of the six most common childhood exanthems.[26][10][27][28][29]
The name "fifth disease" is not typically capitalized, since the name derives from its historical classification as the fifth of the classical childhood skin rashes. They are 1) measles 2) scarlet fever 3) rubella 4) Dukes' disease 5) fifth disease (erythema infectiosum) 6) roseola.
The virus was first described in 1957 at the University of Pennsylvania by Werner, Brachman et al.[30]
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Sabella C, Goldfarb J (October 1999). "Parvovirus B19 infections". Am Fam Physician. 60 (5): 1455–60. PMID 10524489. Archived from the original on 2008-05-14. Retrieved 2009-11-06.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 Servey JT, Reamy BV, Hodge J (February 2007). "Clinical presentations of parvovirus B19 infection". Am Fam Physician. 75 (3): 373–6. PMID 17304869. Archived from the original on 2008-08-21. Retrieved 2009-11-06.
- ↑ 3.0 3.1 3.2 3.3 3.4 "Erythema infectiosum | DermNet NZ". dermnetnz.org. Archived from the original on 29 October 2020. Retrieved 22 October 2020.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 4.12 4.13 4.14 Kostolansky, S; Waymack, JR (January 2020). "Erythema Infectiosum (Fifth Disease)". PMID 30020681.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 5.7 5.8 "Parvovirus B19 | About Fifth Disease | CDC". www.cdc.gov. 26 November 2019. Archived from the original on 19 October 2020. Retrieved 23 October 2020.
- ↑ 6.0 6.1 6.2 6.3 Barlow, Gavin; Irving, William L.; Moss, Peter J. (2020). "20. Infectious disease". In Feather, Adam; Randall, David; Waterhouse, Mona (eds.). Kumar and Clark's Clinical Medicine (10th ed.). Elsevier. p. 519. ISBN 978-0-7020-7870-5. Archived from the original on 2022-04-30. Retrieved 2022-05-05.
- ↑ 7.0 7.1 "Fifth Disease". familydoctor.org. 1 June 2023. Archived from the original on 22 June 2023. Retrieved 26 June 2023.
- ↑ Weir E (March 2005). "Parvovirus B19 infection: fifth disease and more". CMAJ. 172 (6): 743. doi:10.1503/cmaj.045293. PMC 552884. PMID 15767606.
- ↑ "Fifth disease (Erythema Infectiosum)". caringforkids.cps.ca. Archived from the original on 7 May 2023. Retrieved 26 June 2023.
- ↑ 10.0 10.1 10.2 Morens, David M. (6 August 1982). "Fifth Disease: Still Hazy After All These Years". JAMA: The Journal of the American Medical Association. 248 (5): 553. doi:10.1001/jama.1982.03330050035026.
- ↑ 11.0 11.1 Zuckerman, Arie J.; Banatvala, Jangu E.; Pattison, John R.; Griffiths, Paul; Schoub, Barry (2004). Principles and Practice of Clinical Virology. John Wiley & Sons. p. 710. ISBN 978-0-470-02096-8. Archived from the original on 2021-08-28. Retrieved 2020-10-23.
- ↑ "Erythema infectiosum images | DermNet NZ". www.dermnetnz.org. Archived from the original on 28 August 2021. Retrieved 22 October 2020.
- ↑ Mankuta D, Bar-Oz B, Koren G (March 1999). "Erythema infectiosum (fifth disease) and pregnancy". Can Fam Physician. 45: 603–5. PMC 2328398. PMID 10099795.
- ↑ Yoto Y; et al. (2003). "Retrospective study on the influence of human parvovirus B19 infection among children with malignant diseases". Acta Haematol. 90 (1): 8–12. doi:10.1159/000204365. PMID 8237278.
- ↑ Hu, Xi; Jia, Chen; Wu, Jianyong; Zhang, Jian; Jiang, Zhijie; Ma, Kuifen (2022). "Towards the Antiviral Agents and Nanotechnology-Enabled Approaches Against Parvovirus B19". Frontiers in Cellular and Infection Microbiology. 12. doi:10.3389/fcimb.2022.916012/full. ISSN 2235-2988. Retrieved 16 February 2024.
- ↑ Luo, Yong; Qiu, Jianming (2015). "Human parvovirus B19: a mechanistic overview of infection and DNA replication". Future virology. 10 (2): 155–167. doi:10.2217/fvl.14.103. ISSN 1746-0794.
- ↑ Macri A, Crane JS (2021). "Parvoviruses". StatPearls. Treasure Island (FL): StatPearls Publishing. PMID 29489222. Archived from the original on 2021-08-28. Retrieved 2021-07-30.
- ↑ Manaresi E, Gallinella G (July 2019). "Advances in the Development of Antiviral Strategies against Parvovirus B19". Viruses. 11 (7): 659. doi:10.3390/v11070659. PMC 6669595. PMID 31323869.
- ↑ 19.0 19.1 Rogo LD, Mokhtari-Azad T, Kabir MH, Rezaei F (2014). "Human parvovirus B19: a review". Acta Virologica. 58 (3): 199–213. doi:10.4149/av_2014_03_199. PMID 25283854.
- ↑ Qiu J, Söderlund-Venermo M, Young NS (January 2017). "Human Parvoviruses". Clinical Microbiology Reviews. 30 (1): 43–113. doi:10.1128/CMR.00040-16. PMC 5217800. PMID 27806994.
- ↑ 21.0 21.1 Kostolansky, Sean; Waymack, James R. (2024). "Erythema Infectiosum". StatPearls. StatPearls Publishing. Archived from the original on 27 September 2023. Retrieved 16 February 2024.
- ↑ Kwon, Kenneth T (March 19, 2009). "Pediatrics, Fifth Disease or Erythema Infectiosum". eMedicine. Archived from the original on December 7, 2008. Retrieved November 7, 2009.
- ↑ Gillespie, S. M.; Cartter, M. L.; Asch, S; Rokos, J. B.; Gary, G. W.; Tsou, C. J.; Hall, D. B.; Anderson, L. J.; Hurwitz, E. S. (1990). "Occupational risk of human parvovirus B19 infection for school and day-care personnel during an outbreak of erythema infectiosum". JAMA. 263 (15): 2061–5. doi:10.1001/jama.1990.03440150069028. PMID 2157074.
- ↑ Ballou WR, Reed JL, Noble W, Young NS, Koenig S (2003). "Safety and immunogenicity of a recombinant parvovirus B19 vaccine formulated with MF59C.1". J Infect Dis. 187 (4): 675–8. doi:10.1086/368382. PMID 12599085.
- ↑ Altman, Lawrence K (November 30, 1982). "THE DOCTOR'S WORLD". The New York Times. Archived from the original on April 12, 2018. Retrieved November 7, 2009.
- ↑ "Robert R. Briney. Primary Cutaneous Actinomycosis". Archived from the original on 2019-10-03. Retrieved 2019-10-06.
- ↑ "Dictionary of Virology". Archived from the original on 2021-08-28. Retrieved 2019-10-06.
- ↑ "St. Louis Courier of Medicine (1906)". Archived from the original on 2021-08-28. Retrieved 2019-10-06.
- ↑ "Principles and Practice of Clinical Virology". Archived from the original on 2021-08-28. Retrieved 2019-10-06.
- ↑ Werner, Georges H.; Brachman, Philip S.; Ketler, Albert; Scully, John; Rake, Geoffrey (1957). "A new viral agent associated with Erythema Infectiosum". Viruses in Search of Disease. Annals of the New York Academy of Sciences. Vol. 67. pp. 338–345. doi:10.1111/j.1749-6632.1957.tb46058.x. PMID 13411972.
External links
- Parvovirus B19 and fifth disease Archived 2020-10-19 at the Wayback Machine at the Centers for Disease Control and Prevention
| Classification | |
|---|---|
| External resources |