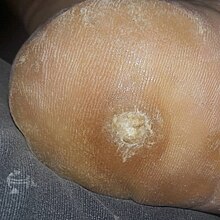
Plantar wart
| Plantar wart | |
|---|---|
| Other names: Verruca, myrmecia, verruca plantaris[1] | |
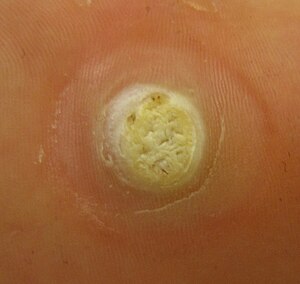 | |
| Close up image of a large plantar wart | |
| Specialty | Dermatology |
| Symptoms | Skin colored lesion, may be painful[2] |
| Complications | Trouble walking[2] |
| Duration | Two years[2] |
| Causes | Human papillomavirus (HPV)[2] |
| Risk factors | Communal showers, prior warts, poor immune function[2][3] |
| Diagnostic method | Based on symptoms[3] |
| Differential diagnosis | Callus, molluscum contagiosum, squamous cell carcinoma[2] |
| Treatment | Salicylic acid, cryotherapy, surgical removal[2] |
| Frequency | Common[4] |
A plantar wart is a wart occurring on the bottom of the foot or toes.[4] Their color is typically similar to that of the skin.[2] Small black dots often occur on the surface.[4] One or more may occur in an area.[2] They may result in pain with pressure such that walking is difficult.[2]
They are caused by the human papillomavirus (HPV).[2] A break in the skin is required for infection to occur.[2] Risk factors include use of communal showers, having had prior warts, and poor immune function.[2][3] Diagnosis is typically based on symptoms.[3]
Treatment is only needed if it is causing symptoms.[3] This may include salicylic acid, cryotherapy, or surgical removal.[2] The skin over-top the lesion should generally be removed before treatment.[2] In about a third to two thirds of cases they go away without specific treatment, however this may take a couple of years.[2] Plantar warts are common.[4] Children and young adults are most often affected.[3]
Signs and symptoms
Their color is typically similar to that of the skin.[2] Small black dots may occur on the surface.[4] One or more may occur in an area.[2] They may result in pain with pressure such that walking may be difficult.[2]
-
A plantar wart: striae (fingerprints) go around the lesion.
-
Mosaic wart cluster
-
Young plantar warts
-
Deep, painful plantar warts
-
Deep plantar wart on heel
Cause
Plantar warts are benign epithelial tumors generally caused by infection by human papillomavirus types 1, 2, 4, 60, or 63,[5] but have also been caused by types 57,[6] 65,[7] 66,[8] and 156.[9] These types are classified as clinical (visible symptoms). The virus attacks compromised skin through direct contact, possibly entering through tiny cuts and abrasions in the stratum corneum (outermost layer of skin). After infection, warts may not become visible for several weeks or months. Because of pressure on the sole of the foot or finger, the wart is pushed inward and a layer of hard skin may form over the wart. A plantar wart can be painful if left untreated.[10][11]
Warts may spread through autoinoculation, by infecting nearby skin or by infected walking surfaces. They may fuse or develop into clusters called mosaic warts.[5]
Diagnosis
A plantar wart is a small lesion that appears on the surface of the skin and typically resembles a cauliflower, with tiny black petechiae (tiny hemorrhages under the skin) in the center. Pinpoint bleeding may occur when these are scratched. Plantar warts occur on the soles of feet and toes. They may be painful when standing or walking.
Plantar warts are often similar to calluses or corns, but can be differentiated by close observation of skin striations. Feet are covered in friction ridges, which are akin to fingerprints of the feet. Friction ridges are dirupted by plantar warts; if the lesion is not a plantar wart, the striations continue across the top layer of the skin. Plantar warts tend to be painful on application of pressure from either side of the lesion rather than direct pressure, unlike calluses (which tend to be painful on direct pressure instead).
Prevention
HPV is spread by direct and indirect contact from an infected host. Avoiding direct contact with infected surfaces such as communal changing rooms and shower floors and benches, avoiding sharing of shoes and socks and avoiding contact with warts on other parts of the body and on the bodies of others may help reduce the spread of infection. Infection is less common among adults than children.[11]
As all warts are contagious, precautions should be taken to avoid spreading them. Recommendations include:
- cover them with an adhesive bandage while swimming
- wear flip-flops when using communal showers
- do not share towels.[12]
Plantar warts are not prevented by inoculation with HPV vaccines because the warts are caused by different strains of HPV. Gardasil protects against strains 6, 11, 16, and 18, and Cervarix protects against 16 and 18, whereas plantar warts are caused by strains 1, 2, 4, and 63.
Treatment
| First-line therapy | Over-the-counter salicylic acid |
| Second-line therapy | Cryosurgery, intralesional immunotherapy, or pulsed dye laser therapy |
| Third-line therapy | Bleomycin, surgical excision |
A number of treatments have been found to be effective.[13] A 2012 review concluded modest benefit from salicylic acid and cryotherapy appears similar to salicylic acid.[14]
Medications
Salicylic acid — the treatment of warts by keratolysis involves the peeling away of dead surface skin cells with keratolytic chemicals such as salicylic acid or trichloroacetic acid. These are available in over-the-counter products or, in higher concentrations, may need to be prescribed by a physician. A 12-week daily treatment with salicylic acid has been shown to lead to a complete clearance of warts in 10–15% of the cases.[15]
Formic acid — Topical formic acid is a common treatment for plantar warts, which works by being applied over a period of time causing the body to reject the wart.[16]
Immunotherapy — Intralesional injection of antigens (mumps, candida or trichophytin antigens USP) is a new wart treatment which may trigger a host immune response to the wart virus, resulting in wart resolution. It is now recommended as a second-line therapy.[17]
Surgery

Liquid nitrogen — This, and similar cryosurgery methods, is a common surgical treatment which acts by freezing the external cell structure of the warts, destroying the live tissue.
Electrodesiccation and surgical excision, which may produce scarring.
Laser surgery — This is generally a last resort treatment, as it is expensive and painful, but may be necessary for large, hard-to-cure warts.[18]
Cauterization — This may be effective as a prolonged treatment. As a short-term treatment, cauterization of the base with anesthetic can be effective, but this method risks scarring or keloids. Subsequent surgical removal if necessary, also risks keloids and/or recurrence in the operative scar.[19]
References
- ↑ James, William D.; Berger, Timothy G.; et al. (2006). Andrews' Diseases of the Skin: clinical Dermatology. Saunders Elsevier. p. 405. ISBN 978-0-7216-2921-6.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 2.17 2.18 Vlahovic, TC; Khan, MT (July 2016). "The Human Papillomavirus and Its Role in Plantar Warts: A Comprehensive Review of Diagnosis and Management". Clinics in Podiatric Medicine and Surgery. 33 (3): 337–53. doi:10.1016/j.cpm.2016.02.003. PMID 27215155.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 Ferri, Fred F. (2017). Ferri's Clinical Advisor 2018 E-Book: 5 Books in 1. Elsevier Health Sciences. p. 1375. ISBN 9780323529570. Archived from the original on 2017-11-11. Retrieved 2017-11-11.
- ↑ 4.0 4.1 4.2 4.3 4.4 "Plantar Warts". AOFAS. Archived from the original on 11 November 2017. Retrieved 11 November 2017.
- ↑ 5.0 5.1 Human Papillomavirus at eMedicine
- ↑ Egawa K, Kitasato H, Honda Y, Kawai S, Mizushima Y, Ono T (1998). "Human papillomavirus 57 identified in a plantar epidermoid cyst". Br. J. Dermatol. 138 (3): 510–4. doi:10.1046/j.1365-2133.1998.02135.x. PMID 9580810.
- ↑ "Human Papillomaviruses Compendium" (PDF). Los Alamos National Laboratory. Archived (PDF) from the original on 2010-05-27. Retrieved 2013-02-05.
- ↑ Davis MD, Gostout BS, McGovern RM, Persing DH, Schut RL, Pittelkow MR (2000). "Large plantar wart caused by human papillomavirus-66 and resolution by topical cidofovir therapy". J. Am. Acad. Dermatol. 43 (2 Pt 2): 340–3. doi:10.1067/mjd.2000.100534. PMID 10901717.
- ↑ Chouhy D, Bolatti EM, Piccirilli G, Sánchez A, Fernandez Bussy R, Giri AA (2013). "Identification of human papillomavirus type 156, the prototype of a new human gammapapillomavirus species, by a generic and highly sensitive PCR strategy for long DNA fragments". J. Gen. Virol. 94 (Pt 3): 524–33. doi:10.1099/vir.0.048157-0. PMID 23136368.
- ↑ Warts, Plantar at eMedicine
- ↑ 11.0 11.1 "Understanding Plantar Warts". Health Plan of New York. Archived from the original on 2009-03-21. Retrieved 2007-12-07.
- ↑ "Clinical Knowledge Summaries: Previous version – Warts (including verrucas)" (PDF). National Health Service. January 2007. p. 2. Archived from the original (PDF) on 2011-06-01. Retrieved 2010-12-05.
- ↑ Bacelieri R, Johnson SM (2005). "Cutaneous warts: an evidence-based approach to therapy". Am Fam Physician. 72 (4): 647–52. PMID 16127954. Archived from the original on 2008-07-09. Retrieved 2008-02-27.
- ↑ Kwok, Chun Shing; Gibbs, Sam; Bennett, Cathy; Holland, Richard; Abbott, Rachel (12 September 2012). "Topical treatments for cutaneous warts". The Cochrane Database of Systematic Reviews (9): CD001781. doi:10.1002/14651858.CD001781.pub3. ISSN 1469-493X. PMID 22972052.
- ↑ Cockayne S, Curran M, Denby G, Hashmi F, Hewitt C, Hicks K, Jayakody S, Kang'ombe A, McIntosh C, McLarnon N, Stamuli E, Thomas K, Turner G, Torgerson D, Watt I (2011). "EVerT: Cryotherapy versus salicylic acid for the treatment of verrucae--a randomised controlled trial". Health Technology Assessment (Winchester, England). 15 (32): 1–170. doi:10.3310/hta15320. PMID 21899812.
- ↑ Bhat, RM; Vidya, K; Kamath, G (June 2001). "Topical formic acid puncture technique for the treatment of common warts". International Journal of Dermatology. 40 (6): 415–9. doi:10.1046/j.1365-4362.2001.01242.x. PMID 11589750.
- ↑ Bacelieri R, Johnson SM (2005). "Cutaneous warts: An evidence-based approach to therapy". American Family Physician. 72 (4): 647–652. PMID 16127954. Archived from the original on 2014-04-21. Retrieved 2014-05-31.
- ↑ "Laser Surgery for Warts" Archived 2012-06-02 at the Wayback Machine, webmd.com
- ↑ Kunnamo, Ilkka (2005). Evidence-based Medicine Guidelines. John Wiley and Sons. p. 422. ISBN 978-0-470-01184-3. Archived from the original on 2018-06-17. Retrieved 2016-09-24.
External links
| Classification |
|---|
- Plantar warts Archived 2006-04-27 at the Wayback Machine at the Mayo Clinic website
- Warts Archived 2012-04-10 at the Wayback Machine at The Merck Manual