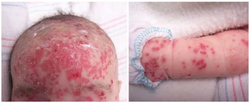
Eczema herpeticum
| Eczema herpeticum | |
|---|---|
| Other names: Kaposi varicelliform eruption, pustulosis varioliformis acute, Kaposi-Juliusberg dermatitis | |
 | |
| Specialty | Dermatology |
| Complications | Secondary bacterial infection, blindness[1][2] |
| Duration | Up to six weeks |
| Causes | Herpes simplex virus (HSV) type 1 or 2[1] |
| Risk factors | Atopic dermatitis (eczema), other forms of dermatitis, burns, ichthyoses[2] |
| Diagnostic method | Based on symptoms, confirmed by testing[1] |
| Differential diagnosis | Impetigo, hand-foot-and-mouth disease, disseminated herpes zoster, disseminated molluscum contagiosum, dermatitis herpetiformis, eczema vaccinatum[2] |
| Treatment | Acyclovir, valacyclovir, supportive care[2] |
| Frequency | Rare[3] |
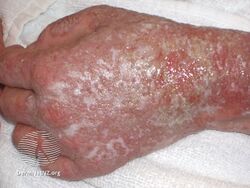
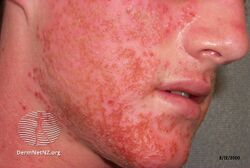
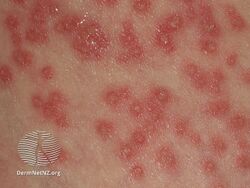
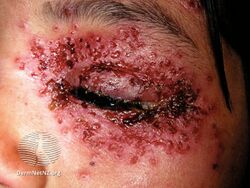
Eczema herpeticum is a widespread viral infection associated with small skin blisters.[1][2] The blisters generally begin in groups at the site of other skin problems and are painful.[2] They then break open to form small ulcers before developing a blood-stained crust.[2] Associated symptoms often include fever and swollen lymph nodes.[2] Healing generally occurs within six weeks.[2] Complications may include secondary bacterial infection and blindness.[1][2]
It is most commonly caused by a first episode of herpes simplex virus (HSV) type 1 or 2.[1] Those affected generally have atopic dermatitis (eczema); though it may also occur in other skin conditions such as other forms of dermatitis, burns, and ichthyoses.[2] Diagnosis is generally based on symptoms and may be confirmed by viral culture or PCR.[1] Coxsackievirus A16 or vaccinia virus (eczema vaccinatum) may produce a similar condition.[1]
Treatment should occur promptly with either acyclovir or valacyclovir.[2] Supportive care, including intravenous fluids, nutritional support, and pain medication may also be required.[2] Death is rare with appropriate treatment.[1][2] Some; however, are left with permanent loss of function.[2]
Eczema herpeticum affects about 3% of people with atopic dermatitis.[3] Children are more commonly affected than adults.[2] It was first described in 1887 by Moritz Kaposi.[1][3] Some use the term "eczema herpeticum" when it occurs in atopic dermatitis and "Kaposi varicelliform eruption" when it occurs in other skin conditions.[1]
Signs and symptoms
In addition to the skin, this infection affects multiple organs, including the eyes, brain, lung, and liver, and can be fatal.
-
Eczema herpeticum
-
Eczema herpeticum
-
Eczema herpeticum
-
Eczema herpeticum
-
Eczema herpeticum
Treatment
It can be treated with systemic antiviral drugs, such as aciclovir or valganciclovir.[4] Foscarnet may also be used for immunocompromised host with Herpes simplex and acyclovir-resistant Herpes simplex.
History
Eczema herpeticum was first described by Hungarian dermatologist Moriz Kaposi in 1887.[5] Fritz Juliusberg coined the term Pustulosis varioliformis acute in 1898.
Epidemiology
Even though the disease may develop at any age it is mostly present in childhood.[6] Those who are affected typically had pre-existing cutaneous condition like atopic dermatitis.[6]
See also
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 "Eczema herpeticum | DermNet NZ". dermnetnz.org. Archived from the original on 24 May 2022. Retrieved 20 June 2022.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 Xiao, A; Tsuchiya, A (January 2022). "Eczema Herpeticum". PMID 32809616.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ 3.0 3.1 3.2 Damour, Alexia; Garcia, Magali; Seneschal, Julien; Lévêque, Nicolas; Bodet, Charles (August 2020). "Eczema Herpeticum: Clinical and Pathophysiological Aspects". Clinical Reviews in Allergy & Immunology. 59 (1): 1–18. doi:10.1007/s12016-019-08768-3. ISSN 1559-0267. PMID 31836943.
- ↑ Xiao, Anny; Tsuchiya, Arline (2022). "Eczema Herpeticum". StatPearls. StatPearls Publishing. Archived from the original on 2022-11-06. Retrieved 2022-11-24.
- ↑ Reitamo, Sakari; Luger, Thomas A; Steinhoff, Martin (2008). Textbook of atopic dermatitis. Informa Healthcare. p. 70. ISBN 978-1841842462.
- ↑ 6.0 6.1 Liaw, Fang-Yih; Huang, Ching-Fu; Hsueh, Ju-Ting; Chiang, Chien-Ping (December 2012). "Eczema herpeticum". Canadian Family Physician. 58 (12): 1358–1361. ISSN 0008-350X. PMC 3520662. PMID 23242894. Archived from the original on 2021-01-26. Retrieved 2021-04-28.
External links
| Classification | |
|---|---|
| External resources |
- Eczema Herpeticum photo library at Dermnet Archived 2009-06-09 at the Wayback Machine