Tinea incognita
| Tinea incognita | |
|---|---|
| Other names: Tinea incognito, tinea atypia, steroid-modified tinea[1] | |
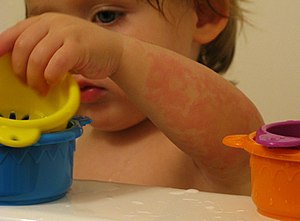 | |
| Tinea incognita in the forearm of a child being treated for contact dermatitis | |
| Specialty | Infectious diseases, dermatology |
| Causes | Steroid cream[2] |
| Treatment | Antifungals, stop steroid application[2] |
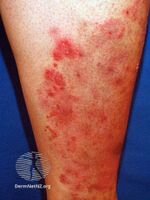
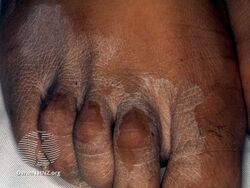
Tinea incognita, also spelled tinea incognito, is a fungal infection of the skin that generally looks odd for a typical tinea infection.[2][3][lower-alpha 1] The border of the skin lesion is usually blurred and it appears to have florid growth.[2] The border of the skin lesion is usually blurred and it appears to have florid growth.[1][2]
It generally occurs following the application of a steroid cream to what at first is thought to be eczema.[2] Continued application results in expansion of the fungal infection which appears unrecognisable.[1] Occasionally, secondary infection with bacteria occurs with concurrent pustules and impetigo.[5]
Tinea incognita was first described by Adrian Ive and Ronnie Marks in 1968.[4]
Signs and symptoms
-
Tinea incognita
-
Tinea incognita
-
Tinea incognita
-
Tinea incognita
-
Tinea incognita
-
Tinea incognita
-
Tinea incognita
Cause
The use of a topical steroid is the most common cause.[2] Frequently, a combination topical steroid and antifungal cream is prescribed by a physician. These combinations include betamethasone dipropionate and clotrimazole (trade name Lotrisone) and triamcinolone acetonide and clotrimazole. In areas of open skin, these combinations are acceptable in treating fungal infection of the skin. In areas where the skin is occluded (groin, buttock crease, armpit), the immunosuppression by the topical steroid might be significant enough to cause tinea incognita to occur even in the presence of an effective antifungal.
Diagnosis
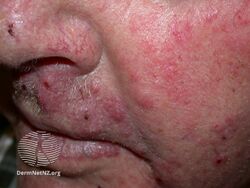
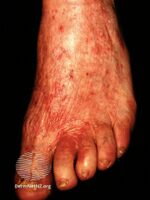
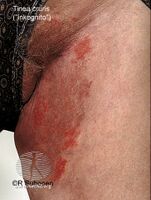
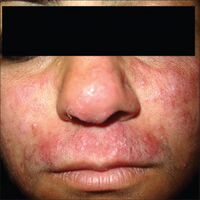
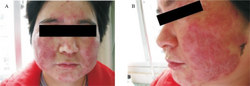
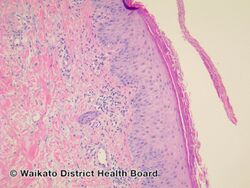
Suspicion arises especially if the eruption is on the face, ankle, legs, or groin. A history of topical steroid or immunosuppressive agent is noted. Confirmation is with a skin scraping and either fungal culture or microscopic exam with potassium hydroxide solution. Characteristic hyphae are seen running through the squamous epithelial cells.
-
Tinea incognita
-
Tinea incognita
Treatment
The removal of the offending topical steroid or immunosuppressive agent and treatment with a topical antifungal is often adequate. If the tinea incognita is extensive or involves hair bearing areas, treatment with a systemic antifungal may be indicated.[citation needed]
History
The condition was first described by Adrian Ive and Ronnie Marks in 1968.[4]
References
- ↑ 1.0 1.1 1.2 1.3 "What is tinea incognita?". DermNet NZ. Archived from the original on 2019-04-30. Retrieved 2021-04-25.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 Chander, Jagdish (2018). Textbook of Medical Mycology (4th ed.). New Delhi: Jaypee Brothers Medical Publishers Ltd. p. 172. ISBN 978-93-86261-83-0. Archived from the original on 2021-08-29. Retrieved 2021-08-27.
- ↑ James, William D.; Elston, Dirk; Treat, James R.; Rosenbach, Misha A.; Neuhaus, Isaac (2020). "15. Diseases resulting from fungi and yeasts". Andrews' Diseases of the Skin: Clinical Dermatology (13th ed.). Elsevier. p. 296. ISBN 978-0-323-54753-6. Archived from the original on 2021-08-29. Retrieved 2021-08-27.
- ↑ 4.0 4.1 4.2 Verma, SB (March 2017). "A Closer Look at the Term "Tinea Incognito:" A Factual as Well as Grammatical Inaccuracy". Indian journal of dermatology. 62 (2): 219–220. doi:10.4103/ijd.IJD_84_17. PMID 28400650.
- ↑ Habif, T. P. (1995) Clinical Dermatology. Mosby, 3rd ed.; pp. 41-42.