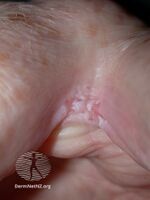
Intertrigo
| Intertrigo | |
|---|---|
 | |
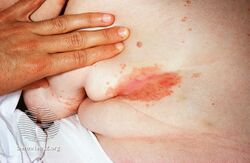
| Intertrigo under the breasts | |
| Pronunciation | |
Intertrigo is an inflammation of skin that occurs where two skin surfaces rub each other.[1]
These areas are more susceptible to irritation and subsequent infection due to factors that promote skin breakdown such as moisture, friction, and exposure to bodily secretions such as sweat, urine, or feces.[2] Areas of the body which are more likely to be affected by intertrigo include the inframammary fold, intergluteal cleft, armpits, and spaces between the fingers or toes. Skin affected by intertrigo is more prone to infection than intact skin.[2] Intertrigo occurs more often in warm and humid conditions. Generally, intertrigo is more common in people with a weakened immune system including children, the elderly, and immunocompromised people.[2] The condition is also more common in people who experience urinary incontinence and decreased ability to move.[2]
Definition
The term "intertrigo" commonly refers to a secondary infection with bacteria (such as Corynebacterium minutissimum), fungi (such as Candida albicans), or viruses. A frequent manifestation is candidal intertrigo.
Signs and symptoms
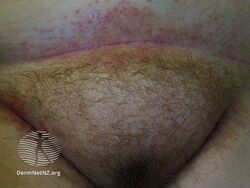
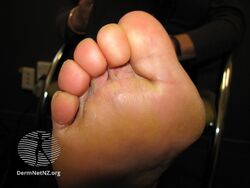
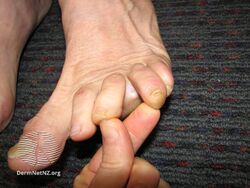
Interigo may be caused by a candidiasis, a fungal infection of the skin by Candida albicans.[1]
-
Candida intertrigo
-
Candida intertrigo
-
Candida intertrigo
-
Candida intertrigo
-
Candida intertrigo
-
Candida intertrigo
Cause
An intertrigo usually develops from the chafing of warm, moist skin in the areas of the inner thighs and genitalia, the armpits, under the breasts, the underside of the belly, behind the ears, and the web spaces between the toes and fingers. An intertrigo usually appears red and raw-looking, and may also itch, ooze, and be sore. Intertrigos occur more often among overweight individuals, those with diabetes, those restricted to bed rest or diaper use, and those who use medical devices, like artificial limbs, that trap moisture against the skin. Also, there are several skin diseases that can cause an intertrigo to develop, such as dermatitis or inverse psoriasis.[citation needed]
Bacterial
Bacterial intertrigo can be caused by Streptococci and Corynebacterium minutissimum.[2][3]
Diagnosis
Intertrigo can be diagnosed clinically by a medical professional after taking a thorough history and performing a detailed physical examination. Many other skin conditions can mimic intertrigo's appearance including erythrasma, inverse psoriasis, scabies, pyoderma, atopic dermatitis, candidiasis, seborrheic dermatitis, and fungal infections of the superficial skin caused by Tinea versicolor or Tinea corporis.[2]
Treatment
Intertrigo is treated by addressing associated infections, by removing moisture from the site, and by using substances at the site to help maintain skin integrity. If the individual is overweight, losing weight may also help. Relapses of intertrigo are common.[citation needed]
Keeping the area of the intertrigo dry and exposed to the air can help prevent recurrences, as can removing moisture from the area using absorbent fabrics or body powders, including plain cornstarch and judiciously used antiperspirants.[citation needed]
Greases, oils, and barrier ointments [4] may help by protecting skin from moisture and from friction.[5] Antifungal powders, most commonly clotrimazole 1%, may also be used in conjunction with a barrier ointment. Diaper rash ointment can also help.[citation needed]
Fungal infections associated with intertrigo may be treated with prescription antifungals applied directly to the skin (in most cases) or systemic antifungals, including fluconazole, nystatin, and griseofulvin.[citation needed]
Intertrigo is also a known symptom of vitamin B6 deficiency.[6]
See also
References
- ↑ 1.0 1.1 James, William D.; Elston, Dirk; Treat, James R.; Rosenbach, Misha A.; Neuhaus, Isaac (2020). "14. Bacterial infections". Andrews' Diseases of the Skin: Clinical Dermatology (13th ed.). Edinburgh: Elsevier. p. 266-267. ISBN 978-0-323-54753-6. Archived from the original on 2022-07-10. Retrieved 2022-06-21.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 Kalra, MG; Higgins, KE; Kinney, BS (April 2014). "Intertrigo and secondary skin infections". American Family Physician. 89 (7): 569–73. PMID 24695603. Archived from the original on 2022-03-23. Retrieved 2022-03-18.
- ↑ Tüzün, Y; Wolf, R; Engin, B; Keçici, AS; Kutlubay, Z (July–August 2015). "Bacterial infections of the folds (intertriginous areas)". Clinics in Dermatology (Review). 33 (4): 420–8. doi:10.1016/j.clindermatol.2015.04.003. PMID 26051056.
- ↑ Bodkhe RB, Shrestha SB, Unertl K, Fetzik J, McNulty AK. Comparing the physical performance of liquid barrier films. Skin Res Technol. 2021 Mar 24. doi: 10.1111/srt.13038. Online ahead of print. PMID 33760305
- ↑ Alison Parnham, Dale Copson, Tanya Loban. Moisture-associated skin damage: causes and an overview of assessment, classification and management. Br J Nurs. 2020 Jun 25;29(12):S30-S37. doi: 10.12968/bjon.2020.29.12.S30. PMID 32579457
- ↑ Tong, Y (2014). "Seizures caused by pyridoxine (vitamin B6) deficiency in adults: A case report and literature review". Intractable Rare Dis Res. 3 (2): 52–6. doi:10.5582/irdr.2014.01005. PMC 4204538. PMID 25343127.
External links
| Classification | |
|---|---|
| External resources |