Lobomycosis
| Lobomycosis | |
|---|---|
| Other names: Lobo disease,[1] Jorge Lobo's disease,[2] Lacaziosis,[3] keloidal blastomycosis[4] | |
 | |
| Lobomycosis | |
| Specialty | Infectious diseases |
| Symptoms | Nodules, keloid[1] |
| Causes | Lacazia loboi[4] |
| Diagnostic method | Skin biopsy |
| Treatment | Surgical excision, cryosurgery[5] |
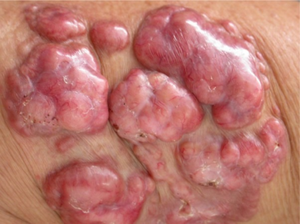
Lobomycosis is a fungal infection of the skin.[4] It usually presents with bumps in the skin, firm swellings, deep skin lesions, or malignant tumors.[1]
It is caused by Lacazia loboi (formerly named Loboa loboi).[4] Transmission is generally by direct contact with contaminated water, soil, vegetation, or by direct contact with an infected dolphin.[1]
Diagnosis is by identifying Lacazia laboi in a lesion.[1]
This disease has been reported in humans and bottlenose dolphins, with the possible risk of transmission from one species to the other.[6]
The condition was first described in 1931 by Brazilian dermatologist Jorge Lobo.[6]
Signs and symptoms
Infection most commonly develops after minor scratches or insect bites, but many people cannot recall any skin trauma. Human-to-human transmission does not occur, and the disease is only acquired from the environment.[7] The disease manifests as chronic keloidal nodular lesions on the face, ears, or extremities.[citation needed]
-
Nodular plaques covered by smooth and shiny skin
-
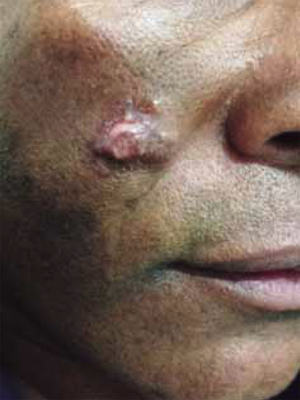
Multiple ill-defined, smooth, shiny, elastic nodules
Diagnosis

Diagnosis of Lobo's disease is made by taking a sample of the infected skin (skin biopsy) and examining it under the microscope.[4] Lacazia loboi is characterized by "lemon-shaped" fungi, a "sieve-like" appearance due to unstained fungi, and long chains of spherical cells interconnected by tubules.[4]
The cells appear to be yeast-like with a diameter of 5 to 12 μm. Attempts to culture L. loboi have so far been unsuccessful.[citation needed]
Differential diagnosis
The disease is often misdiagnosed as Blastomyces dermatitidis or Paracoccidiodes brasiliensis due to its similar morphology.[citation needed]
Treatment
Surgical excision or cryosurgery is the treatment of choice.[5] Treatment with antifungals has been considered ineffective, but the use of clofazimine and dapsone in patients with leprosy and lobomycosis has been found to improve the latter. This treatment regimen, with concomitant itraconazole, has been used to prevent recurrence after surgery.[8]
Epidemiology

The disease is endemic in rural regions in South America and Central America.[7]
Other animals
Lesions in dolphins occur on the dorsal fin, head, flukes, and peduncle. In January 2006, a potential epidemic of lobomycosis was reported in dolphins of the Indian River Lagoon in Florida.[9]
-
Lobomycosis lesions on the skin of a bottlenosed dolphin
-
Infected dorsal fin of wild bottle-nosed dolphin, Gulfo Dulce, Costa Rica
History
The condition was first described in 1931 by Brazilian dermatologist Jorge Lobo.[6] Other names which were given to the disease are: keloidal blastomycosis', Amazonian blastomycosis, blastomycoid granuloma, miraip and piraip. These last two names were given by natives of the Amazon and mean that which burns.
See also
References
- ↑ 1.0 1.1 1.2 1.3 1.4 "ICD-11 - ICD-11 for Mortality and Morbidity Statistics". icd.who.int. Archived from the original on 1 August 2018. Retrieved 4 July 2021.
- ↑ Talhari C, Oliveira CB, de Souza Santos MN, Ferreira LC, Talhari S (June 2008). "Disseminated lobomycosis". Int. J. Dermatol. 47 (6): 582–3. doi:10.1111/j.1365-4632.2008.03678.x. PMID 18477148.
- ↑ Xavier MB, Libonati RM, Unger D, et al. (February 2008). "Macrophage and TGF-beta immunohistochemical expression in Jorge Lobo's disease". Hum. Pathol. 39 (2): 269–74. doi:10.1016/j.humpath.2007.06.016. PMID 17959227.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 Johnstone, Ronald B. (2017). "25. Mycoses and Algal infections". Weedon's Skin Pathology Essentials (2nd ed.). Elsevier. p. 464. ISBN 978-0-7020-6830-0. Archived from the original on 2023-07-01. Retrieved 2023-06-16.
- ↑ 5.0 5.1 Sobera JO, Elewski BE (2007). "Fungal diseases". In Bolognia JL (ed.). Dermatology. St. Louis: Mosby. p. 1150. ISBN 978-1-4160-2999-1.
- ↑ 6.0 6.1 6.2 Francesconi, Valeska Albuquerque; Klein, Ana Paula; Santos, Ana Paula Botelho Gualda; Ramasawmy, Rajendranath; Francesconi, Fábio (2014). "Lobomycosis: epidemiology, clinical presentation, and management options". Therapeutics and Clinical Risk Management. 10: 851–860. doi:10.2147/TCRM.S46251. ISSN 1176-6336. PMID 25328400. Archived from the original on 2020-11-01. Retrieved 2020-12-06.
- ↑ 7.0 7.1 Baruzzi RG, Lacaz CS, Souza FA (1979). "História natural da doença de Jorge Lobo. Ocorrência entre os índios Caibi (Brasil Central)". Rev Inst Med Trop Sao Paulo. 21: 302–338.
- ↑ Rosa PS, Soares CT, Belone AF, et al. (2009). "Accidental Jorge Lobo's disease in a worker dealing with Lacazia loboi infected mice: a case report". Journal of Medical Case Reports. 3: 67. doi:10.1186/1752-1947-3-67. PMC 2647936. PMID 19220901.
- ↑ Reif JS, Mazzoil MS, McCulloch SD, et al. (January 2006). "Lobomycosis in Atlantic bottlenose dolphins from the Indian River Lagoon, Florida". J Am Vet Med Assoc. 228 (1): 104–8. doi:10.2460/javma.228.1.104. PMID 16426180.
External links
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- All articles with unsourced statements
- Articles with unsourced statements from May 2017
- Articles with invalid date parameter in template
- Articles with unsourced statements
- Articles with unsourced statements from July 2020
- Tropical diseases
- Animal fungal diseases
- Mycosis-related cutaneous conditions