Intestinal pseudo-obstruction
| Intestinal pseudo-obstruction | |
|---|---|
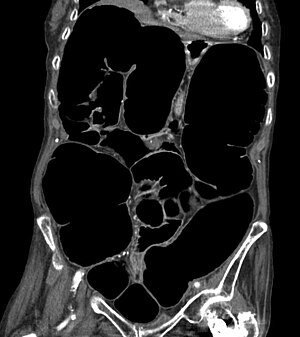 | |
| CT-scan showing a coronal section of the abdomen of an elderly women with an IPO. | |
| Pronunciation |
|
| Specialty | Gastroenterology |
| Symptoms | Abdominal pain, nausea, distention, vomiting, dysphagia, and constipation |
| Complications | Intestinal failure, malabsorption, nutrient deficiencies, small intestinal bacterial overgrowth |
| Duration | Varies according to etiology of disease. < 6 months is considered acute |
| Causes | Idiopathic, Kawasaki Disease, Parkinson's disease, Chaga's disease, Hirschsprung's disease, intestinal hypogangliosis, collagen vascular disease, mitochondrial disease, endocrine disorders, medication side effects |
| Diagnostic method | Signs and symptoms consistent with a mechanical intestinal obstruction with no identifying lesion. |
| Differential diagnosis | Intestinal obstruction, Crohn's Disease, ovarian torsion, ovarian cyst, neoplasm, infection (parasitic) |
| Treatment | Aimed at management of complications (eg - nutrition, hydration, pain relief). |
| Prognosis | 10-25% mortality rate in chronic cases |
| Frequency | Unknown |
Intestinal pseudo-obstruction (IPO) is a syndrome of severe impairment in the ability of the intestines to push food through. Symptoms include intestinal obstruction without any lesion in the intestinal lumen.[1] It appears similar to mechanical intestinal obstructions and can include abdominal pain, nausea, abdominal distension, vomiting, dysphagia and constipation[2][3] depending upon the part of the gastrointestinal tract involved.
It is a difficult condition to diagnose, requiring exclusion of any other mechanical cause of obstruction.[4] Many patients are diagnosed late in the course of disease after additional symptoms are seen. Mortality is also difficult to accurately determine. One retrospective study estimated mortality to be between 10-25% for chronic intestinal pseudo-obstruction (CIPO) and to vary greatly depending on the etiology of the condition.[5] When present for less than six months, it is diagnosed as acute IPO[6] or Ogilvie's Syndrome.[4] Longer than this is considered chronic.[7] Owing to the difficulty of diagnosis, few studies are available which have attempted to estimate its prevalence.[8]
The condition can begin at any age. Most studies describing CIPO are in children.[9][10][4] It can be a primary condition (idiopathic or inherited) or caused by another disease (secondary).[11] It can be a result of myriad of etiologies including infectious, parasitic, autoimmune, genetic, congenital, neurologic, toxic, endocrinological, or anatomical pathology.
Treatment targets nutritional support, improving intestinal motility, and minimizing surgical intervention.[4] Bacterial overgrowth of the small intestine can occur in chronic cases - presenting as malabsorption, diarrhea, and nutrient deficiencies[12] - which may require the use of antibiotics.
Signs and symptoms
Features of IPO can include abdominal pain, nausea, abdominal distension, vomiting, dysphagia, and constipation. Symptoms depend on the portion of the gastrointestinal tract involved[2] and the duration of symptoms. Symptoms may occur intermittently and over a prolonged period of time. It is not unusual for patients to present several times owing to the nonspecific nature of the symptoms.[4] Conditions and onset will vary if the disease is primary vs secondary and the underlying disease (if a secondary manifestation) and its management.
Symptoms indicative of advanced disease and possible intestinal failure include diarrhea, loss of appetite, sepsis, bloating, fatigue, signs of low volume status, and malabsorption including nutritional deficiencies and foul-smelling stools.[13][14]
Causes
In primary CIPO (the majority of chronic cases) the condition results from disruption of the intestine's ability to move food. These can be broadly classified as myopathic (affecting the smooth muscle), mesenchymopathic (affecting the interstitial cells of Cajal), or neuropathic (of the nervous system) of the gastrointestinal tract.[15]
In some cases there appears to be a genetic association.[16] One form has been associated with DXYS154.[17]
Secondary chronic intestinal pseudo-obstruction can occur as a consequence of a number of other conditions including:
- Hirschsprung's disease[18] - the absence of colonic nerve cells
- Chagas' disease - a chronic parasitic infection of the colon leading to loss of nerve endings
- Kawasaki disease[19][20] - a rare presentation for this particular autoimmune disorder of the vasculature
- Parkinson's disease[21] - related to the neurodegeneration of gastrointestinal tract
- Autoimmune conditions - conditions including systemic lupus erythematosus and scleroderma lead to collagen vascular deposition[22] and gastrointestinal motility disruption
- Mitochondrial disease[23] - IPO is a known presentation for mitochondrial disease
- Endocrine disorders[4]
- Certain medications.[15]
The term may be used synonymously with enteric neuropathy if a neurological cause is suspected.
Diagnosis

The symptoms of IPO are nonspecific. It is not unusual for patients to present repeatedly and to undergo numerous tests.[4] Mechanical causes of intestinal obstruction must be excluded to reach a diagnosis of pseudo-obstruction. Attempts must also be made to determine whether the IPO is the result of a primary or secondary condition.[15] A diagnostic work-up may include:[14]
- Gastric motility studies
- Imaging studies:
- X-rays - may show intestinal air fluid levels (seen with true mechanical intestinal obstruction)
- CT scans
- Barium enema
- Blood tests
- Upper and lower endoscopies
- Manometry - used to measure pressure of esophagus and stomach
Treatment
Treatment for IPO (acute or chronic) is aimed at removing the disease process and/or managing the complications present. Focus is placed on management of pain, gastrointestinal symptoms, nutritional deficiencies, fluid status, infection control, and improving quality of life. When CIPO is secondary to another disease, treatment is addressed towards the underlying condition. Surgery is sometimes required in severe cases of CIPO.
Medical
Prucalopride,[24][25] pyridostigmine,[11] metoclopramide, cisapride, erythromycin[9] and octreotide[9][26][27] are medications that aim to enhance intestinal motility.
Intestinal stasis, which may lead to bacterial overgrowth and subsequently, diarrhea or malabsorption, is treated with antibiotics.
Nutritional deficiencies are treated by encouraging patients to avoid foods that increase distention and are difficult to digest (eg - those high in fat and fibre), consuming small frequent meals (5–6 per day), focusing on liquids and soft food. Reducing intake of poorly absorbed sugar alcohols may be of benefit. Referral to an accredited dietitian is recommended. If dietary changes are unsuccessful in meeting nutritional requirements and energy needs, enteral nutrition is used. Many patients eventually require parenteral nutrition.[15]
Total parenteral nutrition (TPN) is a form of long-term nutritional treatment reserved for patients that have severe pseudo-obstruction. TPN dependent patients require frequent checkups to monitor catheter function, check liver enzyme levels, and evaluate for signs of blood infections. TPN format is typically changed depending on loss/gain of weight and bloodwork results, and is specially formulated to meet each individual patient's needs.[28]
Procedures
Intestinal decompression by tube placement in a small stoma can also be used to reduce distension and pressure within the gut. The stoma may be a gastrostomy, jejunostomy, ileostomy or cecostomy. These may be used for feed (eg - gastrostomy and jejunostomy) or to flush the intestines.
Colostomy or ileostomy can bypass affected parts if they are distal to (come after) the stoma. For instance, if only the colon is affected, an ileostomy may be helpful. Either of these ostomies are typically placed at or a few centimeters below the patient's navel per doctor recommendation based on the affected area of the intestines as well as concerns for patient comfort and future physical growth for children.[28]
The total removal of the colon, called a colectomy or resection of affected parts of the colon may be needed if part of the gut dies (for instance toxic megacolon), or if there is a localized area of dysmotility.
Gastric and colonic pacemakers have been tried. These are strips placed along the colon or stomach which create an electric discharge intended to cause the muscle to contract in a controlled manner.
A potential solution, albeit radical, is intestinal transplantation. This is only appropriate in the case of intestinal failure. These procedures are most frequently described in pediatric cases of CIPO.[29][30] One operation involving multi-organ transplant of the pancreas, stomach, duodenum, small intestine, and liver, and was performed by Doctor Kareem Abu-Elmagd on Gretchen Miller.[31]
Research
Further research is necessary into other treatments which may alleviate symptoms. These include stem-cell transplantation[9][32][33] and fecal microbiota transplantation.[9] Cannabis[34][35][unreliable source?] has not been studied with regards to CIPO. Any claims to its efficacy for use in CIPO are speculative.
See also
- Ogilvie syndrome: acute pseudoobstruction of the colon in severely ill debilitated patients.
- Hirschsprung's disease: enlargement of the colon due to lack of development of autonomic ganglia.
- Intestinal neuronal dysplasia: a disease of motor neurons leading to the bowels.
- Bowel obstruction: mechanical or functional obstruction of the bowel, most commonly due to adhesions, hernias or neoplasms.
- Enteric neuropathy: alternative name sometimes used for diagnosis in UK
References
- ↑ Stanghellini V, Cogliandro RF, De Giorgio R, et al. (May 2005). "Natural history of chronic idiopathic intestinal pseudo-obstruction in adults: a single center study". Clinical Gastroenterology and Hepatology. 3 (5): 449–58. doi:10.1016/S1542-3565(04)00675-5. PMID 15880314.
- ↑ 2.0 2.1 De Giorgio R, Sarnelli G, Corinaldesi R, Stanghellini V (November 2004). "Advances in our understanding of the pathology of chronic intestinal pseudo-obstruction". Gut. 53 (11): 1549–52. doi:10.1136/gut.2004.043968. PMC 1774265. PMID 15479666.
- ↑ Robbins basic pathology. Vinay Kumar, Abul K. Abbas, Jon C. Aster, James A. Perkins (10th ed.). Philadelphia, Pa.: Elsevier. 2018. pp. Chapter 5: intestinal obstruction. ISBN 978-0-323-39413-0. OCLC 972900144.
{{cite book}}: CS1 maint: others (link) - ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 El-Chammas, Khalil; Sood, Manu R. (March 2018). "Chronic Intestinal Pseudo-obstruction". Clinics in Colon and Rectal Surgery. 31 (2): 99–107. doi:10.1055/s-0037-1609024. ISSN 1531-0043. PMC 5825855. PMID 29487492.
- ↑ Ko, Dayoung; Yang, Hee-Beom; Youn, Joong; Kim, Hyun-Young (2021-05-28). "Clinical Outcomes of Pediatric Chronic Intestinal Pseudo-Obstruction". Journal of Clinical Medicine. 10 (11): 2376. doi:10.3390/jcm10112376. ISSN 2077-0383. PMC 8198288. PMID 34071279.
- ↑ Saunders MD (October 2004). "Acute colonic pseudoobstruction". Current Gastroenterology Reports. 6 (5): 410–6. doi:10.1007/s11894-004-0059-5. PMID 15341719. S2CID 27281556.
- ↑ Sutton DH, Harrell SP, Wo JM (February 2006). "Diagnosis and management of adult patients with chronic intestinal pseudoobstruction". Nutrition in Clinical Practice. 21 (1): 16–22. doi:10.1177/011542650602100116. PMID 16439766.
{{cite journal}}: CS1 maint: url-status (link) - ↑ Iida, Hiroshi; Ohkubo, Hidenori; Inamori, Masahiko; Nakajima, Atsushi; Sato, Hajime (2013). "Epidemiology and clinical experience of chronic intestinal pseudo-obstruction in Japan: a nationwide epidemiologic survey". Journal of Epidemiology. 23 (4): 288–294. doi:10.2188/jea.je20120173. ISSN 1349-9092. PMC 3709546. PMID 23831693.
- ↑ 9.0 9.1 9.2 9.3 9.4 Zenzeri, Letizia; Tambucci, Renato; Quitadamo, Paolo; Giorgio, Valentina; De Giorgio, Roberto; Di Nardo, Giovanni (May 2020). "Update on chronic intestinal pseudo-obstruction". Current Opinion in Gastroenterology. 36 (3): 230–237. doi:10.1097/MOG.0000000000000630. ISSN 1531-7056. PMID 32073506. S2CID 211193582. Archived from the original on 2022-02-09. Retrieved 2022-01-05.
- ↑ Downes, Thomas J.; Cheruvu, Manikandar S.; Karunaratne, Tennekoon B.; De Giorgio, Roberto; Farmer, Adam D. (July 2018). "Pathophysiology, Diagnosis, and Management of Chronic Intestinal Pseudo-Obstruction". Journal of Clinical Gastroenterology. 52 (6): 477–489. doi:10.1097/MCG.0000000000001047. ISSN 1539-2031. PMID 29877952. S2CID 46960493. Archived from the original on 2022-02-09. Retrieved 2022-01-05.
- ↑ 11.0 11.1 Antonucci A, Fronzoni L, Cogliandro L, et al. (May 2008). "Chronic intestinal pseudo-obstruction". World Journal of Gastroenterology. 14 (19): 2953–61. doi:10.3748/wjg.14.2953. PMC 2712158. PMID 18494042. Archived from the original on 2019-10-31. Retrieved 2022-01-05.
- ↑ Cucchiara, Salvatore; Borrelli, Osvaldo (April 2009). "Nutritional challenge in pseudo-obstruction: the bridge between motility and nutrition". Journal of Pediatric Gastroenterology and Nutrition. 48 Suppl 2: S83–85. doi:10.1097/MPG.0b013e3181a15bfe. ISSN 1536-4801. PMID 19300134. S2CID 11393186. Archived from the original on 2021-11-06. Retrieved 2022-01-05.
- ↑ "Pediatric Intestinal Failure". Children's National. Archived from the original on 11 April 2021. Retrieved 8 November 2021.
- ↑ 14.0 14.1 "Intestinal Failure". Top Doctors United Kingdom. Archived from the original on 8 November 2021. Retrieved 8 November 2021.
- ↑ 15.0 15.1 15.2 15.3 Gabbard SL, Lacy BE (June 2013). "Chronic intestinal pseudo-obstruction". Nutrition in Clinical Practice. 28 (3): 307–16. doi:10.1177/0884533613485904. PMID 23612903.
- ↑ Guzé CD, Hyman PE, Payne VJ (January 1999). "Family studies of infantile visceral myopathy: a congenital myopathic pseudo-obstruction syndrome". American Journal of Medical Genetics. 82 (2): 114–22. doi:10.1002/(SICI)1096-8628(19990115)82:2<114::AID-AJMG3>3.0.CO;2-H. PMID 9934973.
- ↑ Auricchio A, Brancolini V, Casari G, et al. (April 1996). "The locus for a novel syndromic form of neuronal intestinal pseudoobstruction maps to Xq28". American Journal of Human Genetics. 58 (4): 743–8. PMC 1914695. PMID 8644737.
- ↑ "Hirschsprung disease". GARD: Genetic and Rare Diseases Information Center. 4 September 2017. Archived from the original on 24 November 2018. Retrieved 8 November 2021.
- ↑ Akikusa JD, Laxer RM, Friedman JN (May 2004). "Intestinal pseudoobstruction in Kawasaki disease". Pediatrics. 113 (5): e504–6. doi:10.1542/peds.113.5.e504. PMID 15121996.
- ↑ Colomba, Claudia; La Placa, Simona; Saporito, Laura; Corsello, Giovanni; Ciccia, Francesco; Medaglia, Alice; Romanin, Benedetta; Serra, Nicola; Di Carlo, Paola; Cascio, Antonio (November 2018). "Intestinal Involvement in Kawasaki Disease". The Journal of Pediatrics. 202: 186–193. doi:10.1016/j.jpeds.2018.06.034. ISSN 1097-6833. PMID 30029859. S2CID 51704336. Archived from the original on 2021-11-09. Retrieved 2022-01-05.
- ↑ Salari, Mehri; Fayyazi, Emad; Mirmosayyeb, Omid (2016). "Gastrointestinal dysfunction in idiopathic Parkinsonism: A narrative review". Journal of Research in Medical Sciences. 21: 126. doi:10.4103/1735-1995.196608. ISSN 1735-1995. PMC 5348835. PMID 28331512.
- ↑ Takahashi, Hiroki; Ohara, Mikiko; Imai, Kohzoh (June 2004). "[Collagen diseases with gastrointestinal manifestations]". Nihon Rinsho Men'eki Gakkai Kaishi = Japanese Journal of Clinical Immunology. 27 (3): 145–155. doi:10.2177/jsci.27.145. ISSN 0911-4300. PMID 15291251. Archived from the original on 2021-11-09. Retrieved 2022-01-05.
- ↑ Finsterer, Josef; Frank, Marlies (January 2017). "Gastrointestinal manifestations of mitochondrial disorders: a systematic review". Therapeutic Advances in Gastroenterology. 10 (1): 142–154. doi:10.1177/1756283X16666806. ISSN 1756-283X. PMC 5330602. PMID 28286566.
- ↑ Briejer MR, Prins NH, Schuurkes JA (October 2001). "Effects of the enterokinetic prucalopride (R093877) on colonic motility in fasted dogs". Neurogastroenterology and Motility. 13 (5): 465–72. doi:10.1046/j.1365-2982.2001.00280.x. PMID 11696108. S2CID 13610558.
- ↑ Oustamanolakis P, Tack J (February 2012). "Prucalopride for chronic intestinal pseudo-obstruction". Alimentary Pharmacology & Therapeutics. 35 (3): 398–9. doi:10.1111/j.1365-2036.2011.04947.x. PMID 22221087.
- ↑ Sharma S, Ghoshal UC, Bhat G, Choudhuri G (November 2006). "Gastric adenocarcinoma presenting with intestinal pseudoobstruction, successfully treated with octreotide". Indian Journal of Medical Sciences. 60 (11): 467–70. doi:10.4103/0019-5359.27974. PMID 17090868.
- ↑ Sørhaug S, Steinshamn SL, Waldum HL (April 2005). "Octreotide treatment for paraneoplastic intestinal pseudo-obstruction complicating SCLC". Lung Cancer. 48 (1): 137–40. doi:10.1016/j.lungcan.2004.09.008. PMID 15777981.
- ↑ 28.0 28.1 Heneyke S, Smith VV, Spitz L, Milla PJ (July 1999). "Chronic intestinal pseudo-obstruction: treatment and long term follow up of 44 patients". Archives of Disease in Childhood. 81 (1): 21–7. doi:10.1136/adc.81.1.21. PMC 1717974. PMID 10373127.
- ↑ Mousa, Hayat; Hyman, Paul E.; Cocjin, Jose; Flores, Alejandro F.; Di Lorenzo, Carlo (October 2002). "Long-term outcome of congenital intestinal pseudoobstruction". Digestive Diseases and Sciences. 47 (10): 2298–2305. doi:10.1023/a:1020199614102. ISSN 0163-2116. PMID 12395903. S2CID 25029477. Archived from the original on 2021-11-09. Retrieved 2022-01-05.
- ↑ Bond, Geoffrey J.; Reyes, Jorge D. (November 2004). "Intestinal transplantation for total/near-total aganglionosis and intestinal pseudo-obstruction". Seminars in Pediatric Surgery. 13 (4): 286–292. doi:10.1053/j.sempedsurg.2004.10.016. ISSN 1055-8586. PMID 15660322. Archived from the original on 2022-01-21. Retrieved 2022-01-05.
- ↑ "Discovery Channel - Multiorgan transplant". Archived from the original on 2007-01-29. Retrieved 2022-01-05.
- ↑ Westfal, Maggie L.; Goldstein, Allan M. (June 2017). "Pediatric enteric neuropathies: diagnosis and current management". Current Opinion in Pediatrics. 29 (3): 347–353. doi:10.1097/MOP.0000000000000486. ISSN 1531-698X. PMC 5475271. PMID 28319561.
- ↑ Halter, Joerg P.; Michael, W.; Schüpbach, M.; Mandel, Hanna; Casali, Carlo; Orchard, Kim; Collin, Matthew; Valcarcel, David; Rovelli, Attilio; Filosto, Massimiliano; Dotti, Maria T. (October 2015). "Allogeneic haematopoietic stem cell transplantation for mitochondrial neurogastrointestinal encephalomyopathy". Brain: A Journal of Neurology. 138 (Pt 10): 2847–2858. doi:10.1093/brain/awv226. ISSN 1460-2156. PMC 4836400. PMID 26264513.
- ↑ Lin XH, Wang YQ, Wang HC, Ren XQ, Li YY (August 2013). "Role of endogenous cannabinoid system in the gut" (PDF). Sheng Li Xue Bao. 65 (4): 451–60. PMID 23963077. Archived (PDF) from the original on 2013-12-13. Retrieved 2022-01-05.
- ↑ Gastrointestinal Disorders Archived 2019-11-09 at the Wayback Machine.
External links
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- CS1 maint: others
- CS1 maint: url-status
- CS1: long volume value
- Webarchive template wayback links
- All articles lacking reliable references
- Articles lacking reliable references from May 2014
- Articles with invalid date parameter in template
- Portal templates with all redlinked portals
- Diseases of intestines