Ogilvie syndrome
| Ogilvie syndrome | |
|---|---|
| Other names: Acute colonic pseudo-obstruction (ACPO) | |
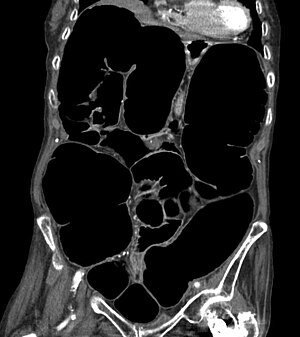 | |
| CT scan of the abdomen of an elderly woman with Ogilvie syndrome | |
| Symptoms | Bloating, abdominal pain, vomiting, constipation[1] |
| Complications | Bowel perforation, bowel ischemia[1] |
| Usual onset | Over a few days[1] |
| Risk factors | Significant health problems, recent surgery[2][1] |
| Diagnostic method | Based on symptoms after ruling out other potential causes[2][1] |
| Differential diagnosis | Chronic intestinal pseudo-obstruction, volvulus, bowel obstruction, gastroparesis[1][2] |
| Treatment | Watchful waiting, nasogastric tube, neostigmine, colonoscopy, surgery[3][1] |
| Frequency | Rare[1] |
| Deaths | 15% risk[2] |
Ogilvie syndrome (OS), also known as acute colonic pseudo-obstruction (ACPO), is the sudden dilatation of the colon in the absence of mechanical obstruction.[3] Symptoms may include bloating, abdominal pain, vomiting, and constipation.[1] Onset is typically over one or more days.[1] Complications can include bowel perforation and bowel ischemia.[1]
It generally occurs in those with significant health problems or following surgery.[2][1] While the underlying mechanism is unclear, it is believed to involve poor contraction of the colon.[3][1] Generally the cecum has a diameter of more than 10 cm and right colon is also dilated.[4] A CT scan or water-soluble enema is done to rule out a obstruction.[1]
Management may include watchful waiting, nasogastric tube, or the medication neostigmine.[3][1] Stopping opiates and anticholinergics may help.[1] In those with more severe cases efforts to remove the gas from the colon using a colonoscope or surgery may be required.[3][1] Prevention of reoccurrence may be by placing a colonic tube.[3] About 15% of people with the condition die as a result.[2]
Ogilvie syndrome is rare, affected about 1 per 1,000 people admitted to hospital.[1][2] It most commonly affects the older people.[2] Males and females are affected equally frequenctly.[1] The condition is named after the British surgeon William Heneage Ogilvie, who described it in 1948.[5][6]
Signs and symptoms
Usually the patient has abdominal distention, pain and altered bowel movements.[4][7] There may also be nausea and vomiting.[8]
Cause
Ogilvie syndrome may occur after surgery, especially following coronary artery bypass surgery and total joint replacement.[9] Drugs that disturb colonic motility (such as anticholinergics or opioid analgesics) contribute to the development of this condition.[4][7]
Pathophysiology
The exact mechanism is not known. The probable explanation is imbalance in the regulation of colonic motor activity by the autonomic nervous system.[10] It has been postulated that reactivation of varicella zoster virus (which causes chickenpox and shingles) in the enteric ganglia may be a cause of Ogilvie syndrome.[11]
Acute megacolon develops because of abnormal intestinal motility. Normal colonic motility requires integration of myogenic, neural, and hormonal influences. The enteric nervous system is independent but is connected to the central nervous system by sympathetic and parasympathetic nerves. The targets of the enteric neurons are muscle cells, secretory cells, endocrine cells, microvasculature, and inflammatory cells. The neurons in the enteric plexuses are stimulated by a food bolus, which both distends the gut and stimulates the mucosal surface, leading to the release of factors that stimulate interneurons. The stimulated interneurons transmit excitatory signals proximally, which cause contraction and inhibitory signals distally, and these in turn cause relaxation. These signals are transmitted by the neurotransmitters acetylcholine and serotonin, among others.[12]
Acute megacolon can also lead to ischemic necrosis in massively dilated intestinal segments. This is explained by Pascal's law and Laplaces's law. Pascal's principle states that a change in pressure at any point in an enclosed fluid at rest is transmitted undiminished to all points in the fluid; the pressure across all parts of the lumen is equal. Laplace's law states that:
where T=wall tension, p=pressure, r=radius, t=wall thickness. Since the wall tension is proportionate to the radius, a dilated intestinal segment has a greater wall tension than a nondilated segment; if the dilatation and tension are sufficiently great, blood flow may be obstructed and ischemia of the bowel will occur.[12] Ogilivie syndrome may precipitate volvulus.[citation needed]
Diagnosis
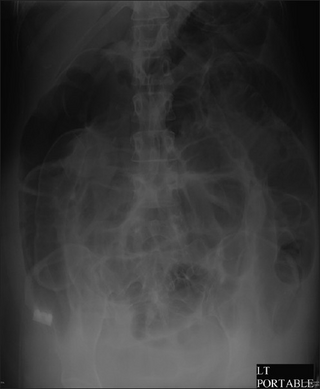
Diagnosis starts with physical exam, observation, and interview of the patient. Imaging to diagnose dilation of the colon involves one view abdominal xray or obstruction series (PA chest, erect abdomen, and supine abdomen images). If further imaging is needed CT may be ordered.[13]
Treatment
It usually resolves with conservative therapy stopping oral ingestions and employing a nasogastric tube,[4] but resolution may require colonoscopic decompression which is successful in 70% of the cases. Neostigmine may help decompressing the colon.[10] According to the American Society for Gastrointestinal Endoscopy (ASGE), it should be considered prior to colonoscopic decompression. The use of neostigmine is not without risk since it can induce bradyarrhythmia and bronchospasms.[7] Therefore, atropine should be within immediate reach when used.[10][4][14]
Prognosis
Ogilvie syndrome is a serious medical disorder. Its mortality rate can be as high as 30%.[7] The high rate is likely a measure that this syndrome is seen in critically ill patients, rather than this syndrome being in itself lethal, although it can also present in otherwise healthy individuals (especially if the disorder was induced by pharmacologic agents). Drug-induced megacolon (such as from clozapine) has been associated with mortality as high as 27.5%.[12]
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 "Ogilvie syndrome". NORD (National Organization for Rare Disorders). Archived from the original on 1 March 2022. Retrieved 30 March 2022.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 Conner, S; Nassereddin, A; Mitchell, C (January 2022). "Ogilvie Syndrome". PMID 30252358.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ 3.0 3.1 3.2 3.3 3.4 3.5 Pereira, P; Djeudji, F; Leduc, P; Fanget, F; Barth, X (April 2015). "Ogilvie's syndrome-acute colonic pseudo-obstruction". Journal of visceral surgery. 152 (2): 99–105. doi:10.1016/j.jviscsurg.2015.02.004. PMID 25770746.
- ↑ 4.0 4.1 4.2 4.3 4.4 Feldman, Mark; Friedman, Lawrence S.; Sleisenger, Marvin H. (July 2002). Sleisenger & Fordtran's Gastrointestinal and Liver Disease (7th ed.). Elsevier. ISBN 978-0-7216-8973-9.
- ↑ Ogilvie H (1948). "Large-intestine Colic due to Sympathetic Deprivation". Br Med J. 2 (4579): 671–673. doi:10.1136/bmj.2.4579.671. PMC 2091708. PMID 18886657. Reproduced in: Ogilvie WH (December 1987). "William Heneage Ogilvie 1887-1971. Large-intestine colic due to sympathetic deprivation. A new clinical syndrome". Dis. Colon Rectum. 30 (12): 984–7. doi:10.1007/BF02554291. PMID 3319452. S2CID 68079923.
- ↑ "Sir William Heneage Ogilvie". www.whonamedit.com. Archived from the original on 22 April 2021. Retrieved 30 March 2022.
- ↑ 7.0 7.1 7.2 7.3 Irwin, Richard S.; Rippe, James M. (January 2003). Intensive Care Medicine. LWW.com. Lippincott Williams & Wilkins, Philadelphia & London. ISBN 0-7817-3548-3. Archived from the original on 2005-11-07.
- ↑ Skeik N, Jabr FI (2009). "Ogilvie Syndrome". Consultant. 49 (2). Archived from the original on 2009-06-01. Retrieved 2021-11-12.
- ↑ Tenofsky PL, Beamer L, Smith RS (2000). "Ogilvie syndrome as a postoperative complication". Arch Surg. 135 (6): 682–6, discussion 686–7. doi:10.1001/archsurg.135.6.682. PMID 10843364.
- ↑ 10.0 10.1 10.2 Ponec RJ, Saunders MD, Kimmey MB (1999). "Neostigmine for the treatment of acute colonic pseudo-obstruction". N. Engl. J. Med. 341 (3): 137–41. doi:10.1056/NEJM199907153410301. PMID 10403850.
- ↑ Gershon, A. A. (2013). "Varicella zoster vaccines and their implications for development of HSV vaccines". Virology. 435 (1): 29–36. doi:10.1016/j.virol.2012.10.006. PMC 3595154. PMID 23217613.
- ↑ 12.0 12.1 12.2 Alam HB, Fricchione GL, Guimaraes AS, Zukerberg LR (October 2009). "Case records of the Massachusetts General Hospital. Case 31-2009. A 26-year-old man with abdominal distention and shock". N. Engl. J. Med. 361 (15): 1487–96. doi:10.1056/NEJMcpc0900643. PMID 19812406.
- ↑ Conner S, Nassereddin A, Mitchell C (2 July 2021). Ogilvie Syndrome. Treasure Island (FL): StatPearls Publishing [Internet]. Archived from the original on 1 October 2021. Retrieved 12 November 2021.
- ↑ Pratt DS, Epstein SK (2000). "Recent advances in critical care gastroenterology". Am. J. Respir. Crit. Care Med. 161 (5): 1417–20. doi:10.1164/ajrccm.161.5.16159. PMID 10806132. Archived from the original on 2011-09-27. Retrieved 2021-11-12.
External links
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- CS1 errors: missing periodical
- All articles with unsourced statements
- Articles with unsourced statements from December 2016
- Articles with invalid date parameter in template
- Diseases of intestines
- Varicella zoster virus-associated diseases
- Rare syndromes
- Syndromes affecting the gastrointestinal tract
- RTT
