Drug rash with eosinophilia and systemic symptoms
| Drug rash with eosinophilia and systemic symptoms | |
|---|---|
| Other names: Drug reaction with eosinophilia and systemic symptoms, drug-induced hypersensitivity syndrome (DIHS), drug hypersensitivity syndrome (DHS), drug-induced delayed multiorgan hypersensitivity syndrome (DIDMOHS), drug-induced pseudolymphoma | |
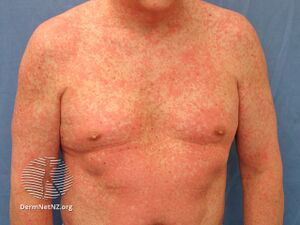 | |
| A medication induced rash[1] | |
| Specialty | Critical care, dermatology |
| Symptoms | Rash, fever, swollen lymph nodes, blood abnormalities (high eosinophils, atypical lymphocytes), organ inflammation[2] |
| Complications | Reactivation of human herpes viruses, autoimmune diseases[2] |
| Usual onset | 2 to 3 weeks after exposure[2] |
| Duration | Weeks[2] |
| Causes | Allopurinol, anticonvulsants, sulfonamides, antibiotics, others[2][1] |
| Risk factors | Genetics[1] |
| Diagnostic method | Based on symptoms, supported by laboratory tests[1] |
| Treatment | Stopping the offending medication, supportive care[1] |
| Prognosis | 10% risk of death[3] |
| Frequency | 1 in 100,000 per year[2] |
Drug rash with eosinophilia and systemic symptoms (DRESS) is a type of severe reaction to certain medications.[2] Symptoms may include a rash, fever, swollen lymph nodes, blood abnormalities (high eosinophils, atypical lymphocytes), and organ inflammation.[2] Onset is typically two to three weeks after medication exposure and symptoms generally last for weeks.[2] Complications may include reactivation of human herpes viruses and autoimmune diseases.[2]
Medications that may result in this condition include allopurinol, anticonvulsants, sulfonamides, and antibiotics.[2] Occasionally other medications may be involved and in some cases the cause remains unclear.[1] Risk factors include genetics.[1] Diagnosis is based on symptoms and supported by laboratory tests.[1] It is a form of severe cutaneous adverse reactions (SCARs), along with Stevens–Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), and acute generalized exanthematous pustulosis (AGEP).[1]
Screening of populations at high risk of a certain HLA type is recommended before using carbamazapine, with such use avoided if they test positive to prevent DRESS.[4] Treatment consists of stopping the offending medication and providing supportive care.[1] While systemic corticosteroids may be used in significant disease; there is a lack of high quality evidence for such use.[1] While most fully recover over weeks to months, the risk of death is about 10%.[1][3]
DRESS syndrome is rare, affecting about 1 in 100,000 people a year.[2] Of those who take an anticonvulsant, about 1 in 10,000 are affected.[1] Males and females are affected with similar frequency.[1] The current term came into use in 1996; though the condition was known by various other names since first described in the 1940s.[3]
Signs and symptoms
The symptoms of DRESS usually begin 2 to 6 weeks but uncommonly up to 8–16 weeks after exposure to an offending drug. Symptoms generally include fever, an often itchy rash which may be morbilliform or consist mainly of macules or plaques, facial edema (i.e. swelling, which is a hallmark of the disease), enlarged and sometimes painful lymph nodes, and other symptoms due to inflammation-based internal organ involvement, most commonly liver, less commonly kidney, lung, and heart, and rarely pancreas or other organs.[5][6] Laboratory findings include increased blood eosinophil and atypical lymphocyte counts, elevated blood markers for systemic inflammation (e.g. erythrocyte sedimentation rate, C-reactive protein), and evidence of internal organ involvement. Liver involvement is detected by measuring blood levels of alanine aminotransferase (ALT), a marker of hepatocyte injury, and alkaline phosphatase (ALP), a marker of bile duct injury, to define three types of injury: hepatocellular (elevated ALP, high ALT/ALP ratio of greater than 5), cholestatic (high ALP, low ALT/ALP ratio of less than 2), and mixed (elevated ALT and ALP, ALT/ALP ratio between 2 and 5, the cutoff values for cholestatic and hepatocellular injury, respectively). Renal involvement is more prone to occur in older individuals and in those with prior kidney or cardiovascular disease; it may take the form of severe interstitial nephritis, acute tubular necrosis, or vasculitis and may lead to kidney failure and, uncommonly, be lethal. Lung involvement takes the form of interstitial pneumonitis, pleuritis, or the acute respiratory distress syndrome; minocycline and abacavir are the main culprit drugs causing severe lung involvement. However, lung involvement in this disorder typically resolves. Cardiac involvement usually presents with evidence of left ventricular dysfunction and ECG changes; it occurs more often in individuals taking minocycline, ampicillin, or sulfonamides, and is either a cardiac hypersensitivity reaction classified as an eosinophilic myocarditis which generally resolves or a far more serious acute necrotizing eosinophilic myocarditis which has a mortality rate of more than 50%. Neurological manifestations of the DRESS syndrome include headache, seizure, coma, and motor dysfunction due to meningitis or encephalitis. Rare manifestations of the disorder include inflammation of the pancreas, gastrointestinal tract, and spleen.[5][7]
The following table gives the percentages for organ involvement and blood abnormalities found in individuals with the DRESS syndrome based on various studies. There are large variations in the percentages found in different studies and populations.[8][5][9][10][11]
| Organ | Percentage involvement | Comment | Blood abnormality | Percentage involvement | Comment | |
|---|---|---|---|---|---|---|
| Liver | 59-100% | >90% if based on high blood levels of ALT | Eosinophilia | 30-95% | usually seen in >66% of cases | |
| Kidney | 8-40% | >40% if based on high levels of BUN or creatinine | Atypical blood lymphocytosis | 27-67% | - | |
| Lung | 5-33% | usually resolves | Lymphocytosis | ~3% | - | |
| Heart (hypersensitivity reaction) | 2-15% | generally not life-threatening | Leukocytosis | up to 100% | due to eosinophilia and/or lymphocytosis | |
| Heart (necrotizing eosinophilic myocarditis) | 2-15% | mortality> 50% | Thrombocytopenia | 3% | Thrombocytopenia may precede and not be due to DRESS syndrome[12] | |
| Nervous system | ~5% | usually resolves | Elevated ESR | ~60-70% | marker of systemic inflammation | |
| Pancreas | ~5% | may result in diabetes | Elevated C-reactive protein | ~60% | marker of systemic inflammation |
No gold standard exists for diagnosis, and at least two diagnostic criteria have been proposed viz., the RegiSCAR criteria [13] and the Japanese consensus group criteria.[14] These two sets of criteria are detailed in the following table.
| RegiSCAR inclusion criteria for DRESS syndrome: 3 of the 4 starred criteria are required for diagnosis | Japanese consensus group diagnostic criteria for DIHS: 7 criteria are needed for diagnosis of DIHS or the first 5 criteria required for diagnosis of atypical DIHS. |
|---|---|
| Hospitalization | pruritic, macular erythema containing papules, pustules or vesicles (generally a Maculopapular rash), developing >3 weeks after starting suspected drug |
| Reaction suspected to be drug-related | Prolonged clinical symptoms 2 weeks after discontinuation of the suspected drug |
| Acute Rash* | Fever > 38 °C |
| Fever > 38 °C* | Liver abnormalities (ALT > 100 U/L) or other organ involvement |
| Lymphadenopathy in at least two sites* | Leukocyte abnormalities |
| Involvement of at least one internal organ* | Leukocytosis ( > 11 x 109/l) |
| Blood count abnormalities (lymphopenia or lymphocytosis*, eosinophilia*, thrombocytopenia*) | Atypical lymphocytosis (>5%) |
| Severe nerve pain | Lymphadenopathy |
| Human herpesvirus 6 reactivation |
Causes
Medications
Drugs that may induce DRESS arranged according to clinical action:[5][15][16][17][18][19][20]
- Anticonvulsants: Carbamazepine, lamotrigine, phenobarbital, phenytoin, oxcarbazepine, gabapentin, primidone
- Antibacterial: Amoxicillin, ampicillin, azithromycin, levofloxacin, minocycline, piperacillin/tazobactam combination, vancomycin, streptomycin
- Anti-tubercular: Ethambutol, isoniazid, pyrazinamide, rifampin
- Anti-retroviral: Abacavir, nevirapine
- Anti-hepatitis C: Boceprevir, telaprevir
- Anti-inflammatory: Acetaminophen, diclofenac, celecoxib, ibuprofen
- Sulfa drugs: Dapsone, sulfamethoxazole-trimethoprim combination, sulfasalazine
- Anticancer drugs: Sorafenib, vismodegib, vemurafenib, imatinib,
- Other drugs: Allopurinol (inhibits uric acid production; treatment for gout), mexiletine (treatment for heart arrhythmias), omeprazole (treatment for gastroesophageal reflux and peptic ulcer), Strontium ranelate (osteoporosis treatment), Chinese herbal medicine.
Medications associated with the development of DRESS are often popular, widely used, or important for the control of certain diseases. This is evident in the most commonly cited medications that cause the DRESS viz., allopurinol, sulfasalazine, and minocycline, as well as in prominent but less commonly cited causes of the disorder such as strontium ranelate, leflunomide, dapsone, and nonsteroidal anti-inflammatory drugs (diclofenac, celecoxib, ibuprofen, and phenylbutazone).[8]
Genetics
Certain populations that express particular serotypes (i.e. alleles) of HLA-A, HLA-B, and/or HLA-C have an increased risk of developing the DRESS syndrome in response to specific medications. These associations include the following:[5][21]
- Carbamazepine: Chinese, Koreans, Japanese, and European individuals who express the HLA serotype (i.e. allele) termed HLA-A31:01 have a low (~1%) but far higher risk of developing the syndrome in response to carbamazepine than those not expressing it. Japanese expressing the serotypes HLA-A11 or HLA-B51 also have increased risks of developing it in response to Carbamazepine.
- Phenytoin: Han Chinese individuals expressing HLA-B13:01, HLA-B51:01, HLA-B15:02, HLA-Cw*08:01, or HLA-DRB1*16:02 serotypes have higher risks of developing the syndrome in response to phenytoin.
- Dapsone: Han Chinese individuals expressing the HLA-B13:01 serotype have a higher risk (7.8%) of developing the DRESS syndrome in response to dapsone.
- Allopurinol: Han Chinese, Korean, Thai, and European individuals expressing the HLA-B58:01 serotype have a higher incidence of developing the syndrome in response to allopurinol.
- Nevirapine: Africans, Asians, and Europeans expressing HLA-DRB1:01:01 or HLA-DRB1:01:02, or HLA-Cw4 serotypes, Asians expressing the HLA-B35 serotype and Australians and Europeans expressing the HLA-C04 serotype have higher incidences of developing the syndrome in response to nevirapine.[22]
- Abacavir: European and African individuals expressing the HLA-B57:01 serotype have a higher incidence (55%) of developing the syndrome in response to abacavir.[23]
- Vancomycin: European individuals carrying HLA-A*32:01 have an approximately 20% chance of developing DRESS syndrome after ≥ 2 weeks of vancomycin [24]
Pathophysiology
Human leukocyte antigens
Like other drug-induced SCARs disorders, the DRESS syndrome is a type IV hypersensitivity reaction in which a drug or its metabolite stimulates cytotoxic T cells (i.e. CD8+ T cells) or T helper cells (i.e. CD4+ T cells) to initiate autoimmune reactions that attack self tissues. DRESS syndrome is a SCARs type IV, subtype IVb reaction. This contrasts with SJS, SJS/TEN, and TEN which are type IV, subtype IVc reactions and AGEP which is a type IV subtype IVd reaction. DRESS syndrome therefore differs from the other SCARs disorders in that it involves the tissue-injuring action of CD4+ cells and the cell- and tissue-injuring action of eosinophils as well as the release of the following cytokines: Interleukins 5 and 13 which simulate the growth, longevity, and activation of eosinophils; Interleukin 4 which promotes the differentiation of naive helper T cells into Th2 helper cells that then serve to activate eosinophils as well as other types of pro-inflammatory cells; IFNγ which activates macrophages and induces the expression of Class II MHC molecules; and TNFα which promotes inflammation but also has cell-killing actions.[25][26][27]
Like other SCARs-inducing drugs, DRESS syndrome-inducing drugs or their metabolites stimulate CD8+ T or CD4+ T cells to initiate autoimmune responses. Studies indicate that the mechanism by which a drug or its metabolites accomplishes this stimulation involves subverting the antigen presentation pathways of the innate immune system. The drug or metabolite covalently binds with a host protein to form a non-self, drug-related epitope. An antigen-presenting cell (APC) takes up these alter proteins; digests them into small peptides; places the peptides in a groove on the human leukocyte antigen (i.e. HLA) component of their major histocompatibility complex (i.e. MHC); and presents the MHC-associated peptides to the T-cell receptor on CD8+ T or CD4+ T cells. Those peptides expressing a drug-related, non-self epitope on their HLA-A, HLA-B, HLA-C, HLA-DM, HLA-DO, HLA-DP, HLA-DQ, or HLA-DR proteins may bind to a T-cell receptor to stimulate the receptor-bearing parent T cell to initiate attacks on self tissues. Alternatively, a drug or metabolite may stimulate these T cells by inserting into the groove on a HLA protein to serve as a non-self epitope or bind outside of this groove to alter a HLA protein so that it forms a non-self epitope. Importantly, however, non-self epitopes must bind to specific HLA serotypes in order to stimulate T cells. Since the human population expresses some 13,000 different HLA serotypes while an individual expresses only a fraction of them and since a DRESSs-inducing drug or metabolite interacts with only one or a few HLA serotypes, a drug's ability to induce SCARs is limited to those individuals who express HLA serotypes targeted by the drug or its metabolite.[27][28] Thus, only rare individuals are predisposed to develop SCARs in response to a particular drug on the basis of their expression of HLA serotypes.[29] Studies have identified several HLA serotypes associated with development of the DRESS syndrome in response to certain drugs, have developed tests to identify individuals who express some of these serotypes, and thereby have identified individuals who should avoid certain DRESS syndrome-inducing drugs.[25][30]
T-cell receptors
A drug or its metabolite may also stimulate CD8+ T or CD4+ T cells to initiate autoimmune responses by directly binding to the T-cell receptors on these T cells. Again, this binding appears to develop only on certain T-cell receptors. Since the genes for these receptors are highly edited, i.e. altered to encode proteins with different amino acid sequences, and since the human population may express more than 100 trillion different (i.e. different amino acid sequences) T-cell receptors while an individual express only a fraction of these, a drug's or its metabolite's ability to induce the DRESS syndrome by interacting with a T-cell receptor is limited to those individuals whose T cells express a T-cell receptor(s) that can interact with drug or its metabolite.[27][21] Thus, only rare individuals are predisposed to develop a SCARs disorder in response to a particular drug on the basis of their expression of specific cell receptor types.[29] While the evidence supporting these ideas is limited, one study identified the preferential presence of the TCR-V-b and complementarity-determining region 3 in T-cell receptors found on the T cells in the blisters of patients with allopurinol-induced DRESS syndrome. This finding is compatible with the notion that specific types of T-cell receptors are involved in the development of specific drug-induced SCARs.[30]
ADME
Variations in ADME, i.e. an individual's efficiency in absorpting, distributing, metabolizing, and excreting a drug has been found to occur in cases of the DRESS syndrome. These variations influence the levels and duration of a drug or drug metabolite in tissues and thereby impact the drug's or drug metabolite's ability to evoke the DRESS syndrome.[4] For example, the CYP2C9 gene codes for CYP2C9, a cytochrome P450 enzyme which metabolizes various substances including phenytoin. The CYP2CP*3 variant of CYP29C has reduced catalytic activity; individuals expressing this variant show an increased incidence of developing the DRESS syndrome when taking phenytoin apparently due to increases in the drug's blood and tissue levels. In a second example of a genetically based ADME defect causing SCARs, Japanese individuals bearing slow acetylating variants of the N-acetyltransferase 2 gene, (NAT2), viz., NAT2*6A and NAT2*7B, acetylate sulfasalazine more slowly than individuals homozygous for the wild type gene. Individuals expressing the NAT2*6A and NAT2*7 variants have an increased risk for developing DRESS syndrome-like reactions to this anti-inflammatory drug.[8] None-genetic ADME factors are also associated with increased risks of developing the DRESS syndrome. Allopurinol is metabolized to oxipurinol, a product with a far slower renal excretion rate than its parent compound. Renal impairment is associated with abnormally high blood levels of oxipurinol and an increased risk of developing the DRESS syndrome, particularly the more severe forms of this disorder. Dysfunction of the kidney and liver are also suggested to promote this disorder in response to other drugs due to the accumulation of SCARs-inducing drugs or metabolites in blood and tissues.[4][31][32] Currently, it is suspected that the expression of particular HLA proteins and T-cell receptors interact with ADME factors to promote SCARs particularly in their more serious forms.[4]
Viral reactivation
During the progression of the DRESS syndrome certain viruses that previously infected an individual and then became latent are reactivated and proliferate. Viruses known to do so include certain members of the Herpesviridae family of Herpes viruses viz., Epstein–Barr virus, human herpesvirus 6, human herpesvirus 7, and cytomegalovirus. Individuals with DRESS syndrome may exhibit sequential reactivation of these four viruses, typically in the order just given. Reactivation of these viruses is associated with a flare-up in symptoms, a prolonged course, and increased disease severity which includes significant organ involvement and the development of certain autoimmune diseases viz., systemic lupus erythematosus, autoimmune thyroiditis, and type 1 diabetes mellitus. While these viral reactivations, particularly of human herpes virus 6, have been suggested to be an important factor in the pathogenesis of the DRESS syndrome, studies to date have not clearly determined if they are a cause or merely a consequence of T cell-mediated tissue injury.[4][5]
Prevention
Screening individuals from populations at high risk for the expression of certain HLA alleles before starting treatment with DRESS-inducing drugs is recommended.[33] Individuals expressing the HLA allele associated with sensitivity to an indicated drug should not be treated with the drug. These recommendations include:[4][34]
- Allopurinol: The American College of Rheumatology guidelines for the management of gout recommend HLA-B*58:01 screening before allopurinol treatment. This is provided in many medical centers in Taiwan, Hong Kong, Thailand, and Mainland China.
- Abacavir: The USA Food and Drug Administration recommends screening for HLA-B*57:01 in the treatment of HIV with abacovir in Caucasian populations. This screening is widely implemented. It has also been suggested that all individuals with this HLA serotype avoid treatment with abacovir.
Current trials are underway to evaluate the ability of genetic screening to prevent the DRESS syndrome for dapsone and HLA-B*13:01 in China and Indonesia. Similar trials are underway in Taiwan to prevent phenytoin-induced DRESS syndrome in individuals expressing the CYP2C9*3 allele of CYP2C9 as well as a series of HLA alleles.[34]
Treatment
Immediate discontinuance of the offending medication is the first and critical step in treating any SCARs disorder. In the past, the mainstay treatment of severe cases of DRESS syndrome was the use, often at high-dosage, of systemic glucocorticoids, relying on the anti-inflammatory actions of these drugs to suppress the eosinophil- and T cell-induced tissue damage caused by the disorder. However, there have been no randomized control trials systemic treatment. Rather, there are suggestions that systemic glucocorticoids is associated with a higher rate of relapse compared to topical glucocorticoid and may be associated with a higher rate of opportunistic infection. Accordingly, less severe cases may be better treated conservatively with general support and, where needed, topical glucocorticoids. Severer cases, particularly those involving significant internal organ involvement, may require systemic corticosteroids and efforts to support heart, kidney, lung, or other organ dysfunctions.[5][27]
Terminology
DRESS syndrome is one of several terms that have been used to describe a severe idiosyncratic reaction to a drug that is characterized by a long latency of onset after exposure to the offending medication, a rash, involvement of internal organs, hematologic abnormalities, and systemic illness. Other synonymous names and acronyms include drug-induced hypersensitivity syndrome (DIHS or DHiS), anticonvulsant hypersensitivity syndrome, drug-induced delayed multiorgan hypersensitivity syndrome, drug-induced pseudolymphoma, anticonvulsant hypersensitivity syndrome, allopurinol hypersensitivity syndrome, dapsone syndrome, and dapsone hypersensitivity syndrome.[3][5][35][36]
See also
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 "Drug hypersensitivity syndrome. DRESS | DermNet". dermnetnz.org. Archived from the original on 3 February 2023. Retrieved 13 June 2023.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 Cardones, Adela R. (November 2020). "Drug reaction with eosinophilia and systemic symptoms (DRESS) syndrome". Clinics in Dermatology. 38 (6): 702–711. doi:10.1016/j.clindermatol.2020.06.008. PMID 33341203.
- ↑ 3.0 3.1 3.2 3.3 Walsh SA, Creamer D (January 2011). "Drug reaction with eosinophilia and systemic symptoms (DRESS): a clinical update and review of current thinking". Clinical and Experimental Dermatology. 36 (1): 6–11. doi:10.1111/j.1365-2230.2010.03967.x. PMID 21143513. S2CID 16048518.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 Adler NR, Aung AK, Ergen EN, Trubiano J, Goh MS, Phillips EJ (2017). "Recent advances in the understanding of severe cutaneous adverse reactions". The British Journal of Dermatology. 177 (5): 1234–1247. doi:10.1111/bjd.15423. PMC 5582023. PMID 28256714.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 5.7 Cho YT, Yang CW, Chu CY (2017). "Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS): An Interplay among Drugs, Viruses, and Immune System". International Journal of Molecular Sciences. 18 (6): 1243. doi:10.3390/ijms18061243. PMC 5486066. PMID 28598363.
- ↑ Corneli HM (2017). "DRESS Syndrome: Drug Reaction With Eosinophilia and Systemic Symptoms". Pediatric Emergency Care. 33 (7): 499–502. doi:10.1097/PEC.0000000000001188. PMID 28665896.
- ↑ Thongsri T, Chularojanamontri L, Pichler WJ (March 2017). "Cardiac involvement in DRESS syndrome". Asian Pacific Journal of Allergy and Immunology. 35 (1): 3–10. doi:10.12932/AP0847. PMID 27996289.
- ↑ 8.0 8.1 8.2 Adwan MH (2017). "Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) Syndrome and the Rheumatologist". Current Rheumatology Reports. 19 (1): 3. doi:10.1007/s11926-017-0626-z. PMID 28138822. S2CID 10549742.
- ↑ Chen, YC; Chiu, HC; Chu, CY (2010). "Drug reaction with eosinophilia and systemic symptoms: A retrospective study of 60 cases". Arch Dermatol. 146 (12): 1373–9. doi:10.1001/archdermatol.2010.198. PMID 20713773.
- ↑ Spriet S, Banks TA (2015). "Drug reaction with eosinophilia and systemic symptoms syndrome". Allergy and Asthma Proceedings. 36 (6): 501–5. doi:10.2500/aap.2015.36.3903. PMID 26534757.
- ↑ Nam YH, Park MR, Nam HJ, Lee SK, Kim KH, Roh MS, Um SJ, Son CH (2015). "Drug reaction with eosinophilia and systemic symptoms syndrome is not uncommon and shows better clinical outcome than generally recognised". Allergologia et Immunopathologia. 43 (1): 19–24. doi:10.1016/j.aller.2013.08.003. PMID 24388810.
- ↑ Sauvetre G, MahÉvas M, Limal N, Guillaud C, Khellaf M, Bierling P, Languille L, Delbos F, Noizat-Pirenne F, Michel M, Godeau B (October 2015). "Cutaneous rash and dapsone-induced hypersensitivity syndrome a common manifestation in adult immune thrombocytopenia. Presentation and outcome in 16 cases". American Journal of Hematology. 90 (10): E201–2. doi:10.1002/ajh.24068. PMID 26120067.
- ↑ Kardaun SH, Sidoroff A, Valeyrie-Allanore L, et al. (2007). "Variability in the clinical pattern of cutaneous side-effects of drugs with systemic symptoms: does a DRESS syndrome really exist?". Response Br J Dermatol. 156 (3): 609–610. doi:10.1111/j.1365-2133.2006.07704.x. PMID 17300272. S2CID 32299525.
- ↑ Shiohara T, Iijima M, Ikezawa Z, Hashimoto K (2007). "The diagnosis of DRESS syndrome has been sufficiently established on the basis of typical clinical features and viral reactivations". Response Br J Dermatol. 156 (5): 1045–92. doi:10.1111/j.1365-2133.2007.07807.x. PMID 17381452. S2CID 33786375.
- ↑ Allam, JP; Paus T; Reichel C; et al. (Sep–Oct 2004). "DRESS syndrome associated with carbamazepine and phenytoin". European Journal of Dermatology. 14 (5): 339–342. PMID 15358574. Archived from the original on 2009-06-23. Retrieved 2023-03-31.
- ↑ "Tetracycline (doxycycline, minocycline)". Archived from the original on 2016-08-02. Retrieved 2023-03-31.
- ↑ Markel, A (October 2005). "Allopurinol-induced DRESS syndrome" (PDF). Israel Medical Association Journal. 7 (10): 656–660. PMID 16259349. Archived from the original (PDF) on 2020-11-28. Retrieved 2009-02-03.
- ↑ "Ziprasidone (Marketed as Geodon and Generics): Drug Safety Communication - Rare But Potentially Fatal Skin Reactions". Food and Drug Administration. 11 December 2014. Archived from the original on 6 April 2017. Retrieved 31 March 2023.
- ↑ Blumenthal, Kimberly G.; Patil, Sarita U.; Long, Aidan A. (2012-04-01). "The importance of vancomycin in drug rash with eosinophilia and systemic symptoms (DRESS) syndrome". Allergy and Asthma Proceedings. 33 (2): 165–171. doi:10.2500/aap.2012.33.3498. ISSN 1539-6304. PMID 22525393.
- ↑ "Olanzapine: Drug Safety Communication - FDA Warns About Rare But Serious Skin Reactions". Food and Drug Administration. 10 May 2016. Archived from the original on 26 January 2018. Retrieved 31 March 2023.
- ↑ 21.0 21.1 Garon SL, Pavlos RK, White KD, Brown NJ, Stone CA, Phillips EJ (September 2017). "Pharmacogenomics of off-target adverse drug reactions". British Journal of Clinical Pharmacology. 83 (9): 1896–1911. doi:10.1111/bcp.13294. PMC 5555876. PMID 28345177.
- ↑ Pavlos R, Mckinnon E, Ostrov D, Peters B, Buus S, Koelle D, Chopra A, Schutte R, Rive C, Redwood A, Restrepo S, Bracey A, Kaever T, Myers P, Speers E, Malaker S, Shabanowitz J, Yuan J, Gaudieri S, Hunt D, Carrington M, Haas D, Mallal S, Phillips E (2017). "Shared peptide binding of HLA class I and II alleles associate with cutaneous nevirapine hypersensitivity and identify novel risk alleles". Scientific Reports. 7 (1): 8653. Bibcode:2017NatSR...7.8653P. doi:10.1038/s41598-017-08876-0. PMC 5561238. PMID 28819312.
- ↑ Mallal S, Phillips E, Carosi G, et al. (2008). "for the PREDICT-1 Study Team. HLA-B*5701 screening for abacavir hypersensitivity". N Engl J Med. 358 (6): 568–579. doi:10.1056/nejmoa0706135. PMID 18256392. Archived from the original on 2021-01-22. Retrieved 2023-03-31.
- ↑ Konvinse KC, Trubiano JA, Pavlos R, James I, Shaffer CM, Bejan CA, Schutte RJ, Ostrov DA, Pilkinton MA, Rosenbach M, Zwerner JP, Williams KB, Bourke J, Martinez P, Rawandamuriye F, Chopra A, Watson M, Redwood AJ, White KD, Mallal SA, Phillips EJ (2019). "HLA-A*32:01 is strongly associated with vancomycin-induced drug reaction with eosinophilia and systemic symptoms". J Allergy Clin Immunol. 144 (1): 183–192. doi:10.1016/j.jaci.2019.01.045. PMC 6612297. PMID 30776417.
- ↑ 25.0 25.1 Hoetzenecker W, Nägeli M, Mehra ET, Jensen AN, Saulite I, Schmid-Grendelmeier P, Guenova E, Cozzio A, French LE (2016). "Adverse cutaneous drug eruptions: current understanding". Seminars in Immunopathology. 38 (1): 75–86. doi:10.1007/s00281-015-0540-2. PMID 26553194. S2CID 333724.
- ↑ Feldmeyer L, Heidemeyer K, Yawalkar N (2016). "Acute Generalized Exanthematous Pustulosis: Pathogenesis, Genetic Background, Clinical Variants and Therapy". International Journal of Molecular Sciences. 17 (8): 1214. doi:10.3390/ijms17081214. PMC 5000612. PMID 27472323.
- ↑ 27.0 27.1 27.2 27.3 Duong TA, Valeyrie-Allanore L, Wolkenstein P, Chosidow O (2017). "Severe cutaneous adverse reactions to drugs". Lancet. 390 (10106): 1996–2011. doi:10.1016/S0140-6736(16)30378-6. PMID 28476287. S2CID 9506967.
- ↑ Bachelez H (January 2018). "Pustular psoriasis and related pustular skin diseases". The British Journal of Dermatology. 178 (3): 614–618. doi:10.1111/bjd.16232. PMID 29333670. S2CID 4436573.
- ↑ 29.0 29.1 Pichler WJ, Hausmann O (2016). "Classification of Drug Hypersensitivity into Allergic, p-i, and Pseudo-Allergic Forms". International Archives of Allergy and Immunology. 171 (3–4): 166–179. doi:10.1159/000453265. PMID 27960170.
- ↑ 30.0 30.1 Wang CW, Dao RL, Chung WH (2016). "Immunopathogenesis and risk factors for allopurinol severe cutaneous adverse reactions". Current Opinion in Allergy and Clinical Immunology. 16 (4): 339–45. doi:10.1097/ACI.0000000000000286. PMID 27362322. S2CID 9183824.
- ↑ Chung WH, Wang CW, Dao RL (2016). "Severe cutaneous adverse drug reactions". The Journal of Dermatology. 43 (7): 758–66. doi:10.1111/1346-8138.13430. PMID 27154258. S2CID 45524211.
- ↑ Lerch M, Mainetti C, Terziroli Beretta-Piccoli B, Harr T (2017). "Current Perspectives on Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis". Clinical Reviews in Allergy & Immunology. 54 (1): 147–176. doi:10.1007/s12016-017-8654-z. PMID 29188475. S2CID 46796285.
- ↑ Chong HY, Mohamed Z, Tan LL, Wu DB, Shabaruddin FH, Dahlui M, Apalasamy YD, Snyder SR, Williams MS, Hao J, Cavallari LH, Chaiyakunapruk N (2017). "Is universal HLA-B*15:02 screening a cost-effective option in an ethnically diverse population? A case study of Malaysia". The British Journal of Dermatology. 177 (4): 1102–1112. doi:10.1111/bjd.15498. PMC 5617756. PMID 28346659.
- ↑ 34.0 34.1 Su SC, Hung SI, Fan WL, Dao RL, Chung WH (2016). "Severe Cutaneous Adverse Reactions: The Pharmacogenomics from Research to Clinical Implementation". International Journal of Molecular Sciences. 17 (11): 1890. doi:10.3390/ijms17111890. PMC 5133889. PMID 27854302.
- ↑ Bocquet H, Bagot M, Roujeau JC (December 1996). "Drug-induced pseudolymphoma and drug hypersensitivity syndrome (Drug Rash with Eosinophilia and Systemic Symptoms: DRESS)". Semin Cutan Med Surg. 15 (4): 250–7. doi:10.1016/S1085-5629(96)80038-1. PMID 9069593.
- ↑ Saltzstein SL, Ackerman LV (1959). "Lymphadenopathy induced by anticonvulsant drugs and mimicking clinically pathologically malignant lymphomas". Cancer. 12 (1): 164–82. doi:10.1002/1097-0142(195901/02)12:1<164::AID-CNCR2820120122>3.0.CO;2-Y. PMID 13618867. S2CID 27319054.
Further reading
- eMedicine Article Archived 2008-12-05 at the Wayback Machine