Levetiracetam
| |||
| Names | |||
|---|---|---|---|
| Pronunciation | /lɛvɪtɪˈræsɪtæm/ | ||
| Trade names | Keppra, Elepsia, other | ||
| |||
| Clinical data | |||
| Drug class | Anticonvulsant (racetam) | ||
| Main uses | Epilepsy[1] | ||
| Side effects | Sleepiness, dizziness, feeling tired, aggression[1] | ||
| Pregnancy category |
| ||
| Routes of use | By mouth, intravenous | ||
| Defined daily dose | 1.5 gram[2] | ||
| External links | |||
| AHFS/Drugs.com | Monograph | ||
| MedlinePlus | a699059 | ||
| Legal | |||
| License data |
| ||
| Legal status | |||
| Pharmacokinetics | |||
| Bioavailability | ~100% | ||
| Protein binding | <10% | ||
| Metabolism | Enzymatic hydrolysis of acetamide group | ||
| Elimination half-life | 6–8 hrs | ||
| Excretion | Urinary | ||
| Chemical and physical data | |||
| Formula | C8H14N2O2 | ||
| Molar mass | 170.212 g·mol−1 | ||
| 3D model (JSmol) | |||
| |||
| |||
Levetiracetam, marketed under the trade name Keppra among others, is a medication used to treat epilepsy.[1] It is used for partial onset, myoclonic, or tonic-clonic seizures.[1] It is taken by mouth as an immediate or extended release formulation or by injection into a vein.[1]
Common side effects include sleepiness, dizziness, feeling tired, and aggression.[1] Severe side effects may include psychosis, suicide, and allergic reactions such as Stevens–Johnson syndrome and anaphylaxis.[1] It is unclear if use is safe during pregnancy but appears to be safe for use when breastfeeding.[3] It is the S-enantiomer of etiracetam.[4] How it works is not clear.[1]
Approved for medical use in the United States in 1999,[1] It is on the World Health Organization's List of Essential Medicines.[5] It is available as a generic medication.[6] A month's supply in the United Kingdom costs the NHS about £19.31 as of 2019.[6] In the United States, the wholesale cost of this amount is about US$4.50.[7] In 2020, it was the 92nd most commonly prescribed medication in the United States, with more than 7 million prescriptions.[8][9]
Medical uses
Focal epilepsy
Levetiracetam is effective as single-drug treatment for newly diagnosed focal epilepsy in adults.[10] It reduces focal seizures by 50% or more as an add-on medication.[11]
Partial-complex epilepsy
Levetiracetam is effective as add-on treatment for partial (focal) epilepsy.[12]
Generalized epilepsy
Levetiracetam is effective for treatment of generalized tonic-clonic epilepsy.[13] It has been approved in the United States as add-on treatment for myoclonic, and tonic-clonic seizures.[14] Levetiracetam has been approved in the European Union as a monotherapy treatment for epilepsy in the case of partial seizures or as an adjunctive therapy for partial, myoclonic, and tonic-clonic seizures.[15]
Levetiracetam is sometimes used off label to treat status epilepticus.[16][17]
Prevention of seizures
Based on low-quality evidence, levetiracetam is about as effective as phenytoin for prevention of early seizures after traumatic brain injury.[18] It may be effective for prevention of seizures associated with subarachnoid hemorrhages.[19]
Other
Levetiracetam has not been found to be useful for treatment of neuropathic pain,[20] nor for treatment of essential tremors.[21] Levetiracetam has not been found to be useful for treating autism,[22][23] but is an effective treatment for partial, myoclonic, or tonic-clonic seizures associated with autism spectrum disorder.[24]
Levetiracetam may be safely used with caution in children over the age of 4. However, it has not been determined whether it can be safely given to children under the age of 4.[25]
Dosage
It is generally started at 500 mg twice per day in adults and may be increased up to 1.5 grams twice per day.[1]
For status epilepticus a dose of 60 mg/kg IV up to 4.5 grams may be used.[26] This is given over 15 minutes.[26]
The defined daily dose is 1.5 grams by mouth or by injection.[2]
Side effects

The most common side effects of levetiracetam treatment include CNS effects such as somnolence, decreased energy, headache, dizziness, mood swings and coordination difficulties. These adverse effects are most pronounced in the first month of therapy. About 4% of patients dropped out of pre-approval clinical trials due to these side effects.[27]
About 13% of people taking levetiracetam experience adverse neuropsychiatric symptoms, which are usually mild. These include agitation, hostility, apathy, anxiety, emotional lability, and depression. Serious psychiatric adverse side effects that are reversed by drug discontinuation occur in about 1%. These include hallucinations, suicidal thoughts, or psychosis. These occurred mostly within the first month of therapy, but they could develop at any time during treatment.[28]
Although rare, Stevens–Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN), which appears as a painful spreading rash with redness and blistering and/or peeling skin, have been reported in patients treated with levetiracetam.[29] The incidence of SJS following exposure to anti-epileptics such as levetiracetam is about 1 in 3,000.[30]
Levetiracetam should not be used in people who have previously shown hypersensitivity to levetiracetam or any of the inactive ingredients in the tablet or oral solution. Such hypersensitivity reactions include, but are not limited to, unexplained rash with redness or blistered skin, difficulty breathing, and tightness in the chest or airways.[27]
In a study, the incidence of decreased bone mineral density of patients on levetiracetam was significantly higher than those for other epileptic medications.[31]
Pregnancy and breastfeeding
Levetiracetam is a pregnancy category C drug. Studies in female pregnant rats have shown minor fetal skeletal abnormalities when given maximum recommended human doses of levetiracetam orally throughout pregnancy and lactation.[14]
Suicide
Levetiracetam, along with other anti-epileptic drugs, can increase the risk of suicidal behavior or thoughts. People taking levetiracetam should be monitored closely for signs of worsening depression, suicidal thoughts or tendencies, or any altered emotional or behavioral states.[14]
Kidney and liver
Kidney impairment decreases the rate of elimination of levetiracetam from the body. Individuals with reduced kidney function may require dose adjustments. Kidney function can be estimated from the rate of creatinine clearance.[27]
Dose adjustment of levetiracetam is not necessary in liver impairment.[27]
Interactions
No significant pharmacokinetic interactions were observed between levetiracetam or its major metabolite and concomitant medications.[32] The pharmacokinetic profile of levetiracetam is not influenced by phenytoin, phenobarbital, primidone, carbamazepine, valproic acid, lamotrigine, gabapentin, digoxin, ethinylestradiol, or warfarin.[33]
Mechanism of action

The exact mechanism by which levetiracetam acts to treat epilepsy is unknown. Levetiracetam does not exhibit pharmacologic actions similar to that of classical anticonvulsants. It does not inhibit voltage-dependent Na+ channels, does not affect GABAergic transmission, and does not bind to GABAergic or glutamatergic receptors.[35] However, the drug binds to SV2A,[36] a synaptic vesicle glycoprotein, and inhibits presynaptic calcium channels,[37] reducing neurotransmitter release and acting as a neuromodulator. This is believed to impede impulse conduction across synapses.[38]
Pharmacokinetics
Absorption
The absorption of levetiracetam tablets and oral solution is rapid and essentially complete. The bioavailability of levetiracetam is close to 100 percent, and the effect of food on absorption is minor.[27]
Distribution
The volume of distribution of levetiracetam is similar to total body water. Levetiracetam modestly binds to plasma proteins (less than 10%).[27]
Metabolism
Levetiracetam does not undergo extensive metabolism, and the metabolites formed are not active and do not exert pharmacological activity. Metabolism of levetiracetam is not by liver cytochrome P450 enzymes, but through other metabolic pathways such as hydrolysis and hydroxylation.[27]
Excretion
In persons with normal kidney function, levetiracetam is eliminated from the body primarily by the kidneys with about 66 percent of the original drug passed unchanged into urine. The plasma half-life of levetiracetam in adults is about 6 to 8 hours.[27]
Analogues
Brivaracetam, a chemical analogue to levetiracetam, is a racetam derivative with similar properties.
Society and culture
Levetiracetam is available as regular and extended release oral formulations and as intravenous formulations.[27][39]
The immediate release tablet has been available as a generic in the United States since 2008, and in the UK since 2011.[40][11] The patent for the extended release tablet will expire in 2028.[41]
The branded version Keppra is manufactured by UCB Pharmaceuticals Inc.[42]
In 2015 Aprecia's 3d-printed orally disintegrating tablet form of the drug was approved by the FDA, under the trade name Spritam.[43]
Cost
A month's supply in the United Kingdom costs the NHS about £19.31 as of 2019.[6] In the United States, the wholesale cost of this amount is about US$4.50.[7] In 2017, it was the 110th most commonly prescribed medication in the United States, with more than six million prescriptions.[44][45]
-
Levetiracetam costs (US)
-
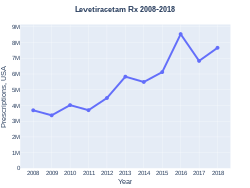
Levetiracetam prescriptions (US)
Legality
Levetiracetam is a schedule 4 substance in Australia under the Poisons Standard (February 2020).[46] A schedule 4 substance is classified as "Prescription Only Medicine, or Prescription Animal Remedy – Substances, the use or supply of which should be by or on the order of persons permitted by State or Territory legislation to prescribe and should be available from a pharmacist on prescription." [46]
Research
Levetiracetam is being looked at in psychiatric and neurologic conditions such as Tourette syndrome,[47] and anxiety disorder.[48] However, its most serious adverse effects are behavioral, and its benefit-risk ratio in these conditions is not well understood.[48]
Levetiracetam is being tested as a drug to reduce hyperactivity in the hippocampus in Alzheimer's disease.[49]
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 1.9 "Levetiracetam Monograph for Professionals". Drugs.com. AHFS. Archived from the original on 24 March 2019. Retrieved 14 January 2019.
- ↑ 2.0 2.1 "WHOCC - ATC/DDD Index". www.whocc.no. Archived from the original on 23 October 2020. Retrieved 6 September 2020.
- ↑ "Levetiracetam Use During Pregnancy". Drugs.com. Archived from the original on 6 March 2019. Retrieved 5 March 2019.
- ↑ Cavanna, Andrea E. (2018). Behavioural Neurology of Anti-Epileptic Drugs: A Practical Guide. Oxford University Press. p. 17. ISBN 9780198791577. Archived from the original on 6 March 2019. Retrieved 5 March 2019.
- ↑ World Health Organization (2023). The selection and use of essential medicines 2023: web annex A: World Health Organization model list of essential medicines: 23rd list (2023). Geneva: World Health Organization. hdl:10665/371090. WHO/MHP/HPS/EML/2023.02.
- ↑ 6.0 6.1 6.2 British national formulary: BNF 76 (76 ed.). Pharmaceutical Press. 2018. p. 319. ISBN 9780857113382.
- ↑ 7.0 7.1 "NADAC as of 2019-02-27". Centers for Medicare and Medicaid Services. Archived from the original on 6 March 2019. Retrieved 3 March 2019.
- ↑ "The Top 300 of 2020". ClinCalc. Archived from the original on 12 February 2021. Retrieved 7 October 2022.
- ↑ "Levetiracetam - Drug Usage Statistics". ClinCalc. Archived from the original on 28 February 2020. Retrieved 7 October 2022.
- ↑ Lattanzi S, Zaccara G, Giovannelli F, Grillo E, Nardone R, Silvestrini M, Trinka E, Brigo F (January 2019). "Antiepileptic monotherapy in newly diagnosed focal epilepsy. A network meta-analysis". Acta Neurol. Scand. 139 (1): 33–41. doi:10.1111/ane.13025. PMID 30194755.
- ↑ 11.0 11.1 Mbizvo, Gashirai K; Dixon, Pete; Hutton, Jane L; Marson, Anthony G (2012). "Levetiracetam add-on for drug-resistant focal epilepsy: An updated Cochrane Review". Cochrane Database of Systematic Reviews (9): CD001901. doi:10.1002/14651858.cd001901.pub2. PMC 7061650. PMID 22972056.
- ↑ Slater J, Chung S, Huynh L, Duh MS, Gorin B, McMicken C, Ziemann A, Isojarvi J (July 2018). "Efficacy of antiepileptic drugs in the adjunctive treatment of refractory partial-onset seizures: Meta-analysis of pivotal trials". Epilepsy Res. 143: 120–129. doi:10.1016/j.eplepsyres.2017.10.004. PMID 29784458.
- ↑ Nevitt SJ, Sudell M, Weston J, Tudur Smith C, Marson AG (December 2017). "Antiepileptic drug monotherapy for epilepsy: a network meta-analysis of individual participant data". Cochrane Database Syst Rev. 12: CD011412. doi:10.1002/14651858.CD011412.pub3. PMC 6486134. PMID 29243813.
- ↑ 14.0 14.1 "DailyMed - KEPPRA- levetiracetam tablet". dailymed.nlm.nih.gov. Archived from the original on 3 February 2015. Retrieved 2015-11-04.
- ↑ BNF 59. BMA & RPSGB. 2010.
- ↑ Brophy, Gretchen M.; Bell, Rodney; Claassen, Jan; Alldredge, Brian; Bleck, Thomas P.; Glauser, Tracy; Laroche, Suzette M.; Riviello, James J.; Shutter, Lori; Sperling, Michael R.; Treiman, David M.; Vespa, Paul M.; Neurocritical Care Society Status Epilepticus Guideline Writing Committee (2012). "Guidelines for the Evaluation and Management of Status Epilepticus". Neurocritical Care. 17 (1): 3–23. doi:10.1007/s12028-012-9695-z. PMID 22528274.
- ↑ Meierkord, H.; Boon, P.; Engelsen, B.; Göcke, K.; Shorvon, S.; Tinuper, P.; Holtkamp, M. (2010). "EFNS guideline on the management of status epilepticus in adults". European Journal of Neurology. 17 (3): 348–55. doi:10.1111/j.1468-1331.2009.02917.x. PMID 20050893.
- ↑ Khan NR, VanLandingham MA, Fierst TM, Hymel C, Hoes K, Evans LT, Mayer R, Barker F, Klimo P (December 2016). "Should Levetiracetam or Phenytoin Be Used for Posttraumatic Seizure Prophylaxis? A Systematic Review of the Literature and Meta-analysis". Neurosurgery. 79 (6): 775–782. doi:10.1227/NEU.0000000000001445. PMID 27749510.
- ↑ Shah, Dharmen; Husain, Aatif M. (2009). "Utility of levetiracetam in patients with subarachnoid hemorrhage". Seizure. 18 (10): 676–9. doi:10.1016/j.seizure.2009.09.003. PMID 19864168.
- ↑ Crawford-Faucher, A; Huijon, R. M. (2015). "The Role of Levetiracetam in Treating Chronic Neuropathic Pain Symptoms". American Family Physician. 92 (1): 23–4. PMID 26132123. Archived from the original on 29 August 2021. Retrieved 1 September 2017.
- ↑ Zesiewicz, T. A.; Elble, R. J.; Louis, E. D.; Gronseth, G. S.; Ondo, W. G.; Dewey, R. B.; Okun, M. S.; Sullivan, K. L.; Weiner, W. J. (2011). "Evidence-based guideline update: Treatment of essential tremor: Report of the Quality Standards Subcommittee of the American Academy of Neurology". Neurology. 77 (19): 1752–5. doi:10.1212/WNL.0b013e318236f0fd. PMC 3208950. PMID 22013182.
- ↑ Volkmar, Fred; Siegel, Matthew; Woodbury-Smith, Marc; King, Bryan; McCracken, James; State, Matthew (2014). "Practice Parameter for the Assessment and Treatment of Children and Adolescents with Autism Spectrum Disorder". Journal of the American Academy of Child & Adolescent Psychiatry. 53 (2): 237–57. doi:10.1016/j.jaac.2013.10.013. PMID 24472258.
- ↑ Hirota, Tomoya; Veenstra-Vanderweele, Jeremy; Hollander, Eric; Kishi, Taro (2013). "Antiepileptic Medications in Autism Spectrum Disorder: A Systematic Review and Meta-Analysis". Journal of Autism and Developmental Disorders. 44 (4): 948–57. doi:10.1007/s10803-013-1952-2. PMID 24077782.
- ↑ Frye, Richard; Rossignol, Daniel; Casanova, Manuel F.; Brown, Gregory L.; Martin, Victoria; Edelson, Stephen; Coben, Robert; Lewine, Jeffrey; Slattery, John C. (2013). "A review of traditional and novel treatments for seizures in autism spectrum disorder: Findings from a systematic review and expert panel". Frontiers in Public Health. 1: 31. doi:10.3389/fpubh.2013.00031. PMC 3859980. PMID 24350200.
- ↑ "Advancements in the Treatment of Epilepsy" (PDF). harvard.edu. 1 January 2008. Archived (PDF) from the original on 28 April 2021. Retrieved 8 July 2017.
- ↑ 26.0 26.1 "GGC Medicines - Levetiracetam IV - dosage and administration advice in status epilepticus". GGC Medicines. Archived from the original on 13 March 2023. Retrieved 16 April 2024.
- ↑ 27.0 27.1 27.2 27.3 27.4 27.5 27.6 27.7 27.8 "Keppra (levetiracetam) Prescribing Information" (PDF). Archived (PDF) from the original on 7 August 2015.
- ↑ Gambardella, Antonio (2008). "Monotherapy for partial epilepsy: Focus on levetiracetam". Neuropsychiatric Disease and Treatment. 4 (1): 33–8. doi:10.2147/NDT.S1655. PMC 2515905. PMID 18728811.
- ↑ Zou, Li-Ping; Ding, Chang-Hong; Song, Zhen-Jiang; Li, Xiao-Feng (2012). "Stevens–Johnson syndrome induced by levetiracetam". Seizure. 21 (10): 823–5. doi:10.1016/j.seizure.2012.09.005. PMID 23036769.
- ↑ Griebel, May L. (1998). "Acute Management of Hypersensitivity Reactions and Seizures". Epilepsia. 39: S17–21. doi:10.1111/j.1528-1157.1998.tb01680.x. PMID 9798757.
- ↑ Beniczky, Simona Alexandra; Viken, Janina; Jensen, Lars Thorbjørn; Andersen, Noémi Becser (2012). "Bone mineral density in adult patients treated with various antiepileptic drugs". Seizure. 21 (6): 471–2. doi:10.1016/j.seizure.2012.04.002. PMID 22541979.
- ↑ Browne, T. R.; Szabo, G. K.; Leppik, I. E.; Josephs, E.; Paz, J.; Baltes, E.; Jensen, C. M. (2000). "Absence of Pharmacokinetic Drug Interaction of Levetiracetam with Phenytoin in Patients with Epilepsy Determined by New Technique". The Journal of Clinical Pharmacology. 40 (6): 590–5. doi:10.1002/j.1552-4604.2000.tb05984.x. PMID 10868309.
- ↑ Gidal, Barry E.; Baltès, Eugène; Otoul, Christian; Perucca, Emilio (2005). "Effect of levetiracetam on the pharmacokinetics of adjunctive antiepileptic drugs: A pooled analysis of data from randomized clinical trials". Epilepsy Research. 64 (1–2): 1–11. doi:10.1016/j.eplepsyres.2005.01.005. PMID 15823510.
- ↑ Contreras-García, Itzel Jatziri; Cárdenas-Rodríguez, Noemí; Romo-Mancillas, Antonio; Bandala, Cindy; Zamudio, Sergio R.; Gómez-Manzo, Saúl; Hernández-Ochoa, Beatriz; Mendoza-Torreblanca, Julieta Griselda; Pichardo-Macías, Luz Adriana (13 April 2022). "Levetiracetam Mechanisms of Action: From Molecules to Systems". Pharmaceuticals (Basel, Switzerland). 15 (4): 475. doi:10.3390/ph15040475. ISSN 1424-8247.
- ↑ Deshpande LS, Delorenzo RJ (2014). "Mechanisms of levetiracetam in the control of status epilepticus and epilepsy". Front Neurol. 5: 11. doi:10.3389/fneur.2014.00011. PMC 3907711. PMID 24550884.
- ↑ Lynch BA, Lambeng N, Nocka K, et al. (June 2004). "The synaptic vesicle protein SV2A is the binding site for the antiepileptic drug levetiracetam". Proc Natl Acad Sci USA. 101 (26): 9861–6. Bibcode:2004PNAS..101.9861L. doi:10.1073/pnas.0308208101. PMC 470764. PMID 15210974.
- ↑ Vogl C, Mochida S, Wolff C, et al. (August 2012). "The Synaptic Vesicle Glycoprotein 2A Ligand Levetiracetam Inhibits Presynaptic Ca2+ Channels through an Intracellular Pathway". Mol. Pharmacol. 82 (2): 199–208. doi:10.1124/mol.111.076687. PMID 22554805.
- ↑ Rogawski, MA (June 2006). "Diverse mechanisms of antiepileptic drugs in the development pipeline". Epilepsy Research. 69 (3): 273–94. doi:10.1016/j.eplepsyres.2006.02.004. PMC 1562526. PMID 16621450.
- ↑ "Levetiracetam Injection Prescribing Information" (PDF). Archived (PDF) from the original on 1 November 2018.
- ↑ Branch Website Management. "Patent Terms Extended Under 35 USC §156". www.uspto.gov. Archived from the original on 15 November 2015. Retrieved 2015-11-05.
- ↑ Webber, Keith (12 September 2011). "FDA Access Data" (PDF). ANDA 091291. Department of Health and Human Services. Archived (PDF) from the original on 4 March 2016. Retrieved 4 November 2015.
- ↑ "Products | UCB". www.ucb-usa.com. Archived from the original on 25 September 2017. Retrieved 2015-11-05.
- ↑ "FDA approves the first 3D-printed drug product | KurzweilAI". www.kurzweilai.net. 13 October 2015. Archived from the original on 16 October 2015. Retrieved 2015-10-14.
- ↑ Cite error: Invalid
<ref>tag; no text was provided for refs namedref - ↑ Cite error: Invalid
<ref>tag; no text was provided for refs namedref1 - ↑ 46.0 46.1 Poisons Standard February 2020 Archived 2 March 2020 at the Wayback Machine. comlaw.gov.au
- ↑ Martínez-Granero, M. A.; García-Pérez, A; Montañes, F (2010). "Levetiracetam as an alternative therapy for Tourette syndrome". Neuropsychiatric Disease and Treatment. 6: 309–16. PMC 2898169. PMID 20628631.
- ↑ 48.0 48.1 Farooq MU, Bhatt A, Majid A, Gupta R, Khasnis A, Kassab MY (2009). "Levetiracetam for managing neurologic and psychiatric disorders". Am J Health Syst Pharm. 66 (6): 541–61. doi:10.2146/ajhp070607. PMID 19265183.
{{cite journal}}: CS1 maint: uses authors parameter (link) - ↑ Haberman, RP; Branch, A; Gallagher, M (July 2017). "Targeting Neural Hyperactivity as a Treatment to Stem Progression of Late-Onset Alzheimer's Disease". Neurotherapeutics : the journal of the American Society for Experimental NeuroTherapeutics. 14 (3): 662–676. doi:10.1007/s13311-017-0541-z. PMID 28560709.
External links
| External sites: | |
|---|---|
| Identifiers: |
|
- Pages using duplicate arguments in template calls
- Pages with reference errors
- Webarchive template wayback links
- CS1 maint: uses authors parameter
- Drugs with non-standard legal status
- Chemical articles with unknown parameter in Infobox drug
- Chemical articles without CAS registry number
- Articles without EBI source
- Chemical pages without ChemSpiderID
- Chemical pages without DrugBank identifier
- Articles without KEGG source
- Articles without UNII source
- Drugs missing an ATC code
- Drug has EMA link
- Drugboxes which contain changes to verified fields
- Drugboxes which contain changes to watched fields
- Articles with changed DrugBank identifier
- Anticonvulsants
- Belgian inventions
- Butyramides
- Drugs with unknown mechanisms of action
- Enantiopure drugs
- Racetams
- RTT
- World Health Organization essential medicines