Paricalcitol
 | |
 | |
| Names | |
|---|---|
| Trade names | Zemplar |
| Other names | 19-nor-1,25-(OH)2-vitamin D2 |
| |
| Clinical data | |
| Drug class | Vitamin D[1] |
| Main uses | Hyperparathyroidism due to chronic kidney disease[2] |
| Side effects | Diarrhea, allergic reactions, nausea, headache, trouble sleeping[1] |
| Pregnancy category |
|
| Routes of use | By mouth, intravenous |
| External links | |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a682335 |
| Legal | |
| Legal status | |
| Pharmacokinetics | |
| Bioavailability | 72%[3] |
| Protein binding | 99.8%[3] |
| Metabolism | Hepatic[3] |
| Elimination half-life | 14-20 hours[3] |
| Excretion | Faeces (74%), urine (16%)[3] |
| Chemical and physical data | |
| Formula | C27H44O3 |
| Molar mass | 416.646 g·mol−1 |
| |
Paricalcitol, sold under the trade name Zemplar, is a medication used to prevent and treat hyperparathyroidism due to chronic kidney disease.[2] It is taken by mouth.[2]
Common side effects include diarrhea, allergic reactions, nausea, headache, and trouble sleeping.[1] Other side effects may include high calcium and aluminum toxicity.[1] There are concerns with use in pregancy.[2] It is a form of calcitriol, an active type of vitamin D.[1]
Paricalcitol was patented in 1989 and approved for medical use in 1998.[4] It is available as a generic medication.[1] In the United Kingdom 28 doses of 1 microgram costs the NHS about £70 as of 2021.[2] This amount in the United States is about 100 USD.[5]
Medical uses
Its primary use in medicine is in the treatment of secondary hyperparathyroidism associated with chronic kidney disease.[6] However current evidence is not sufficient to demonstrate an advantage of paricalcitol over non-selective vitamin D derivatives for this indication.[7]
Dosage
The dose used is based on the intact parathyroid hormone levels.[1]
Side effects
By frequency:[3][6][8][9]
Very common (>10% frequency):
- Nausea
Common (1-10% frequency):
- Diarrhoea†
- Oedema
- Allergic reaction
- Arthritis
- Dizziness†
- Stomach discomfort‡
- Gastroesophageal reflux disease†
- Acne†
- Hypercalcaemia†
- Hypocalcaemia†
- Hyperphosphataemia
- Decreased appetite†
- Headache
- Breast tenderness†
- Taste changes
- Hypoparathyroidism
- Vertigo
- Rash‡
Uncommon (0.1-1% frequency):
- Abnormal hepatic enzymes‡
- Constipation‡
- Dry mouth‡
- Itchiness‡
- Hives
- Hypersensitivity‡
- Muscle spasms‡
- Bleeding time prolonged
- Aspartate aminotransferase increased
- Laboratory test abnormal
- Weight loss
- Elevated blood creatinine
- Cardiac arrest
- Arrhythmia
- Atrial flutter
- Anaemia
- Leucopenia
- Lymphadenopathy
- Coma
- Stroke
- Transient ischemic attack
- Fainting
- Myoclonus
- Hypoaesthesia
- Paraesthesia
- Glaucoma
- Conjunctivitis
- Ear disorder
- Pulmonary oedema
- Asthma
- Shortness of breath
- Nose bleed
- Cough
- Rectal haemhorrhage
- Colitis
- Gastritis
- Indigestion
- Difficulty swallowing
- Gastrointestinal disorder
- Gastrointestinal haemorrhage
- Bullous dermatitis
- Hair loss
- Hirsutism
- Hyperhidrosis
- Joint pain
- Joint stiffness
- Back pain
- Muscle twitching
- Muscle aches
- Hyperparathyroidism
- Hyperkalaemia
- Hypocalcemia
- Breast cancer
- Sepsis
- Pneumonia
- Infection
- Pharyngitis
- Vaginal infection
- Influenza
- High blood pressure
- Hypotension
- Gait disturbance
- Injection site pain
- Fever
- Chest pain
- Condition aggravated
- Muscle weakness
- Malaise
- Thirst
- Breast pain
- Impotence
- Confusional state
- Delirium
- Depersonalization
- Agitation
- Insomnia
- Nervousness
‡ These are adverse effects only seen in patients with grade 3 or 4 chronic kidney disease. † These are adverse effects only seen in patients with grade 5 chronic kidney disease.
Contraindications
Contraindications include:[9]
- Vitamin D intoxication
- Hypercalcaemia
- Hypersensitivity to paricalcitol or any of its excipients
whereas cautions include:[3]
- Impaired liver function
- It is also advised that physicians regularly monitor their patients' calcium and phosphorus levels.
Interactions
Drugs that may interact with paricalcitol include:[3][9]
- Ketoconazole, as it may interfere with paricalcitol's metabolism in the liver.
- Digitoxin, hypercalcaemia due to any cause can exacerbate the toxicity of digitoxin.
- Thiazide diuretics or calcium supplements as hypercalcaemia may be induced by this combination
- Magnesium-containing products such as antacids may increase the risk of hypermagnesemia.
- Aluminium-containing products such as antacids may increase the risk of aluminium toxicity.
- Drugs that interfere with the absorption of fat-soluble vitamins, such as cholestyramine may interfere with the absorption of paricalcitol.
Overdose
Electrolyte abnormalities (e.g. hypercalcaemia and hyperphosphataemia) are common overdose symptoms.[9] Treatment is mostly supportive, with particular attention being paid to correcting electrolyte anomalies and reducing intake of calcium in both the form of supplementation and diet.[9] As it is so heavily bound to plasma proteins haemodialysis is unlikely to be helpful in cases of overdose.[9]
Early symptoms of overdose can include:[9]
- Weakness
- Headache
- Somnolence
- Nausea
- Vomiting
- Dry mouth
- Constipation
- Muscle pain
- Bone pain
- Metallic taste in the mouth.
It is worth noting, however, that may of these symptoms are also indicative of kidney failure and hence may be masked by the patient's condition.[9]
Late symptoms of overdose include:
- Loss of appetite
- Weight loss
- Conjunctivitis (calcific)
- Pancreatitis
- Photophobia
- Rhinorrhoea
- Pruritus
- Hyperthermia
- Decreased libido
- Elevated BUN
- Hypercholesterolaemia
- Elevated AST and ALT
- Ectopic calcification
- Hypertension
- Cardiac arrhythmias
- Somnolence
- Death
- Psychosis (rare)
Mechanism of action
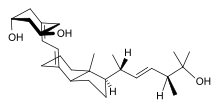
Like 1,25-dihydroxyergocalciferol, paricalcitol acts as an agonist at the vitamin D receptor and thereby lowers parathyroid hormone levels in the blood.[3]
Pharmacokinetics
The plasma concentration of paricalcitol decreases rapidly and log-linearly within two hours after initial intravenous administration. Therefore, it is not expected to accumulate with multiple dosing, since paricalcitol is usually given no more frequently than every other day (3 times per week).[10]
Chemistry
It may also be known as (1R,3S)-5-[2-[(1R,3aR,7aS)-1-[(2R,5S)-6-hydroxy-5,6-dimethyl-3E-hepten-2-yl]-7a-methyl-2,3,3a,5,6,7-hexahydro-1H-inden-4-ylidene]ethylidene]-cyclohexane-1,3-diol.
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 "Paricalcitol Monograph for Professionals". Drugs.com. Archived from the original on 27 February 2021. Retrieved 26 October 2021.
- ↑ 2.0 2.1 2.2 2.3 2.4 BNF 81: March-September 2021. BMJ Group and the Pharmaceutical Press. 2021. p. 1137. ISBN 978-0857114105.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 3.8 "Zemplar (paricalcitol) dosing, indications, interactions, adverse effects, and more". Medscape Reference. WebMD. Archived from the original on 2 February 2014. Retrieved 26 January 2014.
- ↑ Fischer J, Ganellin CR (2006). Analogue-based Drug Discovery. John Wiley & Sons. p. 452. ISBN 9783527607495. Archived from the original on 2021-01-22. Retrieved 2021-03-18.
- ↑ "Paricalcitol Prices, Coupons & Patient Assistance Programs". Drugs.com. Archived from the original on 10 August 2020. Retrieved 26 October 2021.
- ↑ 6.0 6.1 Rossi S, ed. (2013). Australian Medicines Handbook (2013 ed.). Adelaide: The Australian Medicines Handbook Unit Trust. ISBN 978-0-9805790-9-3.
- ↑ Cai P, Tang X, Qin W, Ji L, Li Z (April 2016). "Comparison between paricalcitol and active non-selective vitamin D receptor activator for secondary hyperparathyroidism in chronic kidney disease: a systematic review and meta-analysis of randomized controlled trials". International Urology and Nephrology. 48 (4): 571–84. doi:10.1007/s11255-015-1195-6. PMID 26748501. S2CID 10633197.
- ↑ "PARICALCITOL capsule, liquid filled [Teva Pharmaceuticals USA Inc]" (PDF). DailyMed. Teva Pharmaceuticals USA Inc. September 2013. Archived from the original on 2 February 2014. Retrieved 26 January 2014.
- ↑ 9.0 9.1 9.2 9.3 9.4 9.5 9.6 9.7 "Zemplar Soft Capsules 1 mcg - Summary of Product Characteristics". electronic Medicines Compendium. AbbVie Limited. 15 April 2013. Archived from the original on 1 February 2014. Retrieved 26 January 2014.
- ↑ Rxlist: Zemplar Archived 2021-01-19 at the Wayback Machine
External links
| Identifiers: |
|
|---|
- Pages using duplicate arguments in template calls
- Webarchive template wayback links
- Chemical articles with unknown parameter in Infobox drug
- Chemical articles without CAS registry number
- Articles without EBI source
- Chemical pages without ChemSpiderID
- Chemical pages without DrugBank identifier
- Articles without KEGG source
- Articles without UNII source
- Drugs missing an ATC code
- Drugboxes which contain changes to verified fields
- Drugboxes which contain changes to watched fields
- Articles with changed DrugBank identifier
- Articles with changed KEGG identifier
- Secosteroids
- Vitamin D
- AbbVie brands
- RTT