Noma (disease)
| Noma | |
|---|---|
| Other names: Fusospirochetal gangrene, necrotizing ulcerative stomatitis, stomatitis gangrenosa[1] | |
 | |
| A man afflicted with noma | |
| Symptoms | Rapidly progressive gangrene of the mouth and face[2] |
| Usual onset | Age 2 years to 7 years[2] |
| Causes | Malnutrition[2] |
| Risk factors | Pre-term births, low birth weight, Measles, malaria, HIV, poor oral hygiene[2] |
| Prevention | Adequate nutrition, measles vaccination, prevention of malaria and HIV[2] |
| Treatment | Antibiotics, surgery[2] |
| Frequency | 30,000–40,000 cases per year (globally)[2] |
| Deaths | 85%[2] |
Noma, also known as cancrum oris, is a rapidly progressive neglected tropical disease that presents with gangrene of the mouth and face resulting in significant facial disfigurement.[2][3]
The cause is opportunistic infection by normal oral flora, on a background of poverty and malnutrition and in association with other diseases including measles, malaria, HIV, and poor oral hygiene.[2] The death rate is around 85%.[2] Prevention requires adequate nutrition, measles vaccination, and prevention of malaria and HIV.[2] Treatment is with antibiotics, and surgery.[2]
Worldwide, the incidence is 30,000–40,000 cases per year.[2] It is generally seen in children age 2-years to 7-years living in sub-Saharan Africa.[2] The condition has been recognised for centuries.[2]
Signs and symptoms
The mucous membranes of the mouth develop ulcers, and rapid, painful tissue degeneration ensues, which can degrade tissues of the bones in the face.[4]
-
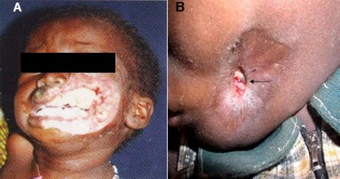
a. Rapidly destructive and fulminatingdisease requiring lengthy antibiotic treatment prior to surgery. b. Arrested advanced disease requiring short course of antibioticsbefore surgical reconstruction (arrow indicates sequestrumformation)
-
Noma (sketch from 1836)
Causes
Noma affects extremely impoverished and malnourished children in sub-Saharan countries and other tropical regions; while some bacterial organisms are often found in affected children, these same bacteria are widespread. The underlying causes for this disease are primarily poor sanitation and malnutrition.[2][3]
Fusobacterium necrophorum and Prevotella intermedia are important bacterial pathogens in this disease process, interacting with one or more other bacterial organisms (such as Borrelia vincentii, Porphyromonas gingivalis, Tannerella forsythia, Treponema denticola, Staphylococcus aureus, and certain species of nonhemolytic Streptococcus).[5] Treatment of these organisms can help arrest the infection, but does not restore already-missing or disfigured tissue.
It is often reported as a sequela to acute necrotising ulcerative gingivitis. Predisposing factors include:[3][6][7]
- malnutrition (particularly Vitamin-A and Vitamin-B) or dehydration
- poor hygiene, particularly oral
- unsafe drinking water
- proximity to unkempt livestock
- recent illness
- an immunodeficiency disease, including AIDS
- measles
- smoking
Diagnosis
The diagnosis of this condition in an affected individual is based on physical exam which will show mouth ulcers, and skin ulcers.[8]
Treatment
Known in antiquity to such physicians as Hippocrates and Galen, noma was once reported around the world, including Europe and the United States. With improvements in hygiene and nutrition, noma has disappeared from industrialized countries since the 20th century, except during World War II when it was endemic to Auschwitz and Belsen concentration camps.[9] The disease and treatments were studied by Berthold Epstein, a Czech physician and forced-labor prisoner who had recommended the study under Josef Mengele's direction.[9]
The progression of the disease can be halted with the use of antibiotics and improved nutrition; however, its physical effects are permanent and may require oral and maxillofacial surgery or reconstructive plastic surgery to repair. Reconstruction is usually very challenging and should be delayed until full recovery (usually about one year following initial intervention).[10]
Epidemiology
The disease is associated with high morbidity and mortality.[2] It affects mainly children in the poorest countries of Africa. Children in Asia and some countries of South America are also highly affected. Most children who get the disease are between the ages of two and six years old.[11] The WHO estimates that 500,000 people are affected, and that 140,000 new cases are reported each year.[12] The mortality rate is approximately 90 per cent.[1]
Society and culture
Children and other noma survivors in Africa are helped by a few international charitable organizations, such as Facing Africa, a UK registered charity that helps affected Ethiopian, and Swiss charity Winds of Hope.[13] There is one dedicated noma hospital in Nigeria, the Noma Children Hospital Sokoto, staffed by resident and visiting medical teams supported by Médecins Sans Frontières.[14] In other countries, such as Ethiopia, international charities work in collaboration with the local health care system to provide complex reconstructive surgery which can give back facial functions such as eating, speaking and smiling. Teams of volunteer medics coming from abroad are often needed to support the local capacity to address the most severe cases, which can be extremely challenging even for senior maxillofacial surgeons.[15] On 10 June 2010 the work of such volunteer surgeons was featured in a UK BBC Two documentary presented by Ben Fogle, Make Me a New Face: Hope for Africa's Hidden Children. Recently a case was reported from Nepal where the 19-year-old girl received free surgical treatment in Chitwan Medical College, Bharatpur; the team of surgeons was led by Sushil Subedi, Oral and Maxillofacial surgeon and the head of Department.[16][17]
References
- ↑ 1.0 1.1 Marck KW (April 2003). "A history of noma, the 'Face of Poverty'". Plastic and Reconstructive Surgery. 111 (5): 1702–7. doi:10.1097/01.PRS.0000055445.84307.3C. PMID 12655218. Archived from the original on 2019-04-04. Retrieved 2021-07-15.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 2.17 Srour, ML; Marck, K; Baratti-Mayer, D (8 February 2017). "Noma: Overview of a Neglected Disease and Human Rights Violation". The American journal of tropical medicine and hygiene. 96 (2): 268–274. doi:10.4269/ajtmh.16-0718. PMID 28093536. Archived from the original on 14 August 2022. Retrieved 21 April 2023.
- ↑ 3.0 3.1 3.2 Enwonwu CO, Falkler WA, Phillips RS (July 8, 2006). "Noma (cancrum oris)". The Lancet. 368 (9530): 147–56. doi:10.1016/S0140-6736(06)69004-1. PMID 16829299. S2CID 10647321.
- ↑ "AllRefer Health - Noma (Cancrum Oris, Gangrenous Stomatitis)". Archived from the original on 2007-05-28. Retrieved 2007-07-12.
- ↑ Neville, Brad. Oral and Maxillofacial Pathology (3rd ed.). Saunders Book Company. pp. 062008. 5.11.
- ↑ Auluck A, Pai KM (2005). "Noma: Life Cycle of a Devastating Sore - Case Report and Literature Review" (PDF). Journal of the Canadian Dental Association. 71 (10): 757–757c. PMID 16324228. Archived (PDF) from the original on 2021-08-12. Retrieved 2021-07-15.
- ↑ Enwonwu CO (2006). "Noma--the ulcer of extreme poverty". The New England Journal of Medicine. 354 (3): 221–4. doi:10.1056/NEJMp058193. PMID 16421362.
- ↑ "Noma: MedlinePlus Medical Encyclopedia". medlineplus.gov. Archived from the original on 31 August 2021. Retrieved 14 September 2021.
- ↑ 9.0 9.1 Lifton RJ (1986). The Nazi Doctors: Medical Killing and Psychological Genocide. Basic Books. p. 361. ISBN 978-0-465-04905-9.
- ↑ Neville, Brad. Oral and Maxillofacial Pathology, 3rd Ed. Saunders Book Company, 062008. 5.11.2
- ↑ "The European Noma-Network". Archived from the original on 2016-03-14. Retrieved 2007-07-12.
- ↑ Bourgeois DM, Leclercq MH (1999). "The World Health Organization initiative on noma". Oral Dis. 5 (2): 172–174. doi:10.1111/j.1601-0825.1999.tb00085.x. PMID 10522217.
- ↑ "Winds of Hope". www.windsofhope.org. Archived from the original on 2021-01-26. Retrieved 2021-05-14.
- ↑ "Noma - a neglected disease". Noma. Archived from the original on 2021-06-12. Retrieved 2021-06-12.
- ↑ Medical care Archived 2009-04-28 at the Wayback Machine at Project Harar
- ↑ "Make Me a New Face: Hope for Africa's Hidden Children". BBC. June 2010. Archived from the original on April 8, 2019. Retrieved January 13, 2016.
- ↑ Fogle, Ben (July 6, 2010). "Ben's Documentary on Noma - BBC2". BenFogle.com. Archived from the original on April 11, 2018. Retrieved January 13, 2010.
External links
| Classification | |
|---|---|
| External resources |