Frey's syndrome
| Frey's syndrome | |
|---|---|
| Other names: Auriculotemporal syndrome, Baillarger's syndrome, Dupuy’s syndrome, Frey-Baillarger syndrome | |
 | |
| Redness associated with Frey's syndrome | |
| Symptoms | Redness and sweating of cheek area when salivating |
| Causes | Damage to auriculotemporal nerve |
| Diagnostic method | Starch-iodine test |
| Frequency | 30–50% (after parotidectomy) |
Frey's syndrome (also known as Baillarger's syndrome, Dupuy’s syndrome, auriculotemporal syndrome,[1] or Frey-Baillarger syndrome) is a rare neurological disorder resulting from damage to or near the parotid glands responsible for making saliva, and from damage to the auriculotemporal nerve often from surgery.[1][2]
The symptoms of Frey's syndrome are redness and sweating on the cheek area adjacent to the ear (see focal hyperhidrosis). They can appear when the affected person eats, sees, dreams, thinks about or talks about certain kinds of food which produce strong salivation.[3] Observing sweating in the region after eating a lemon wedge may be diagnostic.[2]
Signs and symptoms
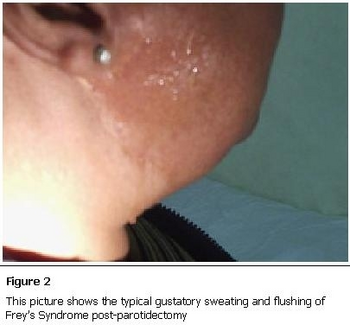
Signs and symptoms include erythema (redness or flushing) and sweating in the cutaneous distribution of the auriculotemporal nerve, usually in response to gustatory stimuli. There is sometimes pain in the same area, often burning in nature. Between attacks of pain there may be numbness or other altered sensations (anesthesia or paresthesia). This is sometimes termed "gustatory neuralgia".
Causes
Frey's syndrome often results as a complication of surgeries of or near the parotid gland or due to injury to the auriculotemporal nerve, which passes through the parotid gland in the early part of its course. The auriculotemporal branch of the mandibular branch (V3) of the trigeminal nerve carries parasympathetic fibers to the parotid salivary gland and sympathetic fibers to the sweat glands of the scalp. As a result of severance and inappropriate regeneration, the parasympathetic nerve fibers may switch course to a sympathetic response, resulting in "gustatory sweating" or sweating in the anticipation of eating, instead of the normal salivary response.[2] It is often seen with patients who have undergone endoscopic thoracic sympathectomy, a surgical procedure wherein part of the sympathetic trunk is cut or clamped to treat sweating of the hands or blushing. The subsequent regeneration or nerve sprouting leads to abnormal sweating and salivation. It can also include discharge from the nose when smelling certain food.
Rarely, Frey's syndrome can result from causes other than surgery, including accidental trauma, local infections, sympathetic dysfunction and pathologic lesions within the parotid gland.[4] An example of such rare trauma or localized infection can be seen in situations where a hair follicle has become ingrown, and is causing trauma or localized infection near or over one of the branches of the auriculotemporal nerve.
Diagnosis
Diagnosis is made based on clinical signs and symptoms and a starch-iodine test, also known as the Minor test. The affected area of the face is painted with iodine which is allowed to dry, then dry corn starch is applied to the face. The starch turns blue on exposure to iodine in the presence of sweat.[5]
Treatments
- Injection of botulinum toxin A[6]
- Surgical transection of the nerve fibers (a temporary treatment)[citation needed]
- Application of an ointment containing an anticholinergic drug such as scopolamine[citation needed]
Cochrane reviews of interventions to either prevent[7] or treat[8] Frey’s syndrome have found little or no evidence to support their effectiveness or safety, and conclude that further clinical trials are needed.
Epidemiology
The condition is rare, although the exact incidence is unknown.[9]
The disorder most often occurs as a complication of the surgical removal of a parotid gland (parotidectomy). The percentage of individuals who develop Frey syndrome after a parotidectomy is controversial and reported estimates range from 30–50 percent. In follow-up examinations, approximately 15 percent of affected individuals rated their symptoms as severe. Frey syndrome affects males and females in equal numbers.
History
It is named after Łucja Frey-Gottesman.[10] The disorder was first reported in medical literature by Baillarger in 1853. A neurologist from Poland, Dr. Lucja Frey, provided a detailed assessment of the disorder and coined the term "auriculotemporal syndrome" in 1923.[11]
References
- ↑ 1.0 1.1 "Frey's syndrome". Genetic and Rare Diseases Information Center (GARD). National Institutes of Health, U.S. Department of Health & Human Services. 2011. Archived from the original on 9 March 2013. Retrieved 17 December 2012.
- ↑ 2.0 2.1 2.2 Prattico F, Perfetti P (July 2006). "Images in clinical medicine. Frey's syndrome". The New England Journal of Medicine. 355 (1): 66. doi:10.1056/NEJMicm040462. PMID 16822997.
- ↑ "Frey's Syndrome Treatment: What You Need to Know". Parotid Tumor Surgery | Salivary Gland Surgery Los Angeles CA. Archived from the original on 2021-02-14. Retrieved 2021-02-07.
- ↑ Kragstrup TW, Christensen J, Fejerskov K, Wenzel A (August 2011). "Frey syndrome-an underreported complication to closed treatment of mandibular condyle fracture? Case report and literature review" (PDF). Journal of Oral and Maxillofacial Surgery. 69 (8): 2211–6. doi:10.1016/j.joms.2010.12.033. PMID 21496996. Archived (PDF) from the original on 2019-04-28. Retrieved 2021-08-09.
- ↑ Choi HG, Kwon SY, Won JY, Yoo SW, Lee MG, Kim SW, Park B (December 2013). "Comparisons of Three Indicators for Frey's Syndrome: Subjective Symptoms, Minor's Starch Iodine Test, and Infrared Thermography". Clinical and Experimental Otorhinolaryngology. 6 (4): 249–53. doi:10.3342/ceo.2013.6.4.249. PMC 3863675. PMID 24353866.
- ↑ "Onabotulinumtoxina (Injection Route, Intradermal Route, Intramuscular Route)". Mayo Clinic. 2011. Archived from the original on 27 January 2012. Retrieved 18 December 2012.
- ↑ Ye L, Cao Y, Yang W, Wu F, Lin J, Li L, Li C (October 2019). Cochrane ENT Group (ed.). "Graft interposition for preventing Frey's syndrome in patients undergoing parotidectomy". The Cochrane Database of Systematic Reviews. 10: CD012323. doi:10.1002/14651858.CD012323.pub2. PMC 6953270. PMID 31578708.
- ↑ Li C, Wu F, Zhang Q, Gao Q, Shi Z, Li L (March 2015). Cochrane ENT Group (ed.). "Interventions for the treatment of Frey's syndrome". The Cochrane Database of Systematic Reviews (3): CD009959. doi:10.1002/14651858.CD009959.pub2. PMID 25781421.
- ↑ "Frey Syndrome". NORD (National Organization for Rare Disorders). Archived from the original on 2018-01-27. Retrieved 2019-01-26.
- ↑ synd/390 at Who Named It?
- ↑ Frey L (1923). "Le syndrome du nerf auriculo-temporal" [Atriotemporal nerve syndrome]. Rev. Neurol. (in français). 2: 97–104.
External links
| Classification |
|---|