Melkersson–Rosenthal syndrome
| Melkersson–Rosenthal syndrome | |
|---|---|
| Other names: MRO, Miescher–Melkersson–Rosenthal syndrome[1] | |
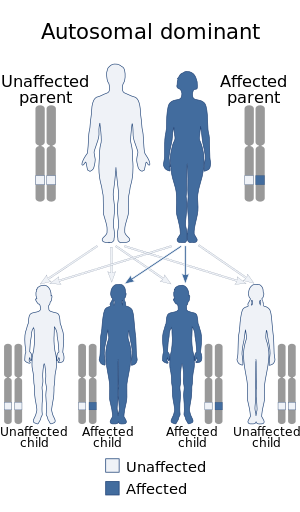 | |
| This condition is inherited in an autosomal dominant manner. | |
Melkersson–Rosenthal syndrome is a rare neurological disorder characterized by recurring facial paralysis, swelling of the face and lips (usually the upper lip: cheilitis granulomatosis) and the development of folds and furrows in the tongue (fissured tongue).[2]: 799 Onset is in childhood or early adolescence. After recurrent attacks (ranging from days to years in between), swelling may persist and increase, eventually becoming permanent.[3] The lip may become hard, cracked, and fissured with a reddish-brown discoloration. The cause of Melkersson–Rosenthal syndrome is unknown, but there may be a genetic predisposition. It has been noted to be especially prevalent among certain ethnic groups in Bolivia. It can be symptomatic of Crohn's disease or sarcoidosis.[citation needed] Approximately 400 cases have been reported worldwide.
Signs and symptoms
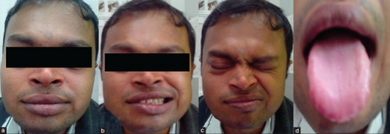
The clinical presentation of this condition is consistent with:[4]
- Facial palsy
- Grooved tongue
- Macroglossia
- Cheilitis
- Skin inflammation
- Oligosacchariduria
- Nystagmus
- Fever
Cause
Not to be confused with Rosenthal syndrome a.k.a. hemophilia C which is caused by clotting factor XI deficiency. Only genetic causation is established as it is associated with twins and family members.[citation needed]
Diagnosis
Diagnosis is mainly based on clinical features. However, biopsy has been useful in diagnosis as well as in differentiating between the different types of the disease.[citation needed]
Treatment
Treatment is symptomatic and may include nonsteroidal anti-inflammatory drugs (NSAIDs) and corticosteroids to reduce swelling, antibiotics and immunosuppressants. Surgery may be indicated to relieve pressure on the facial nerves and reduce swelling, but its efficacy is uncertain. Massage and electrical stimulation may also be prescribed.[citation needed]
Prognosis
Melkersson–Rosenthal syndrome may recur intermittently after its first appearance. It can become a chronic disorder. Follow-up care should exclude the development of Crohn's disease or sarcoidosis.[citation needed]
Eponym
The condition is named after Ernst Melkersson and Curt Rosenthal.[5][6][7]
Research
The NINDS supports research on neurological disorders such as Melkersson–Rosenthal syndrome. Much of this research is aimed at increasing knowledge of these disorders and finding ways to treat, prevent, and ultimately cure them.[citation needed]
See also
References
- ↑ Ngan V. "Granulomatous cheilitis". DermNet New Zealand Trust. Archived from the original on 2016-07-07. Retrieved 2020-12-05.
- ↑ James, William D.; Berger, Timothy G.; et al. (2006). Andrews' Diseases of the Skin: Clinical Dermatology. Saunders Elsevier. ISBN 978-0-7216-2921-6.
- ↑ Bakshi SS. Melkersson–Rosenthal Syndrome. J Allergy Clin Immunol Pract. 2017 Mar - Apr;5(2):471-472. doi: 10.1016/j.jaip.2016.09.034
- ↑ "Melkersson-Rosenthal syndrome | Genetic and Rare Diseases Information Center (GARD) – an NCATS Program". rarediseases.info.nih.gov. Archived from the original on 18 March 2021. Retrieved 24 September 2021.
- ↑ synd/9 at Who Named It?
- ↑ Melkersson, E. (1928). "Ett fall av recidiverande facialispares i samband med ett angioneurotiskt ödem". Hygiea. Stockholm. 90: 737–741.
- ↑ Rosenthal, C. (1931). "Klinisch-erbbiologischer Beitrag zur Konstitutionspathologie. Gemeinsames Auftreten von Facialislähmung, angioneurotischem Gesichtsödem und Lingua plicata in Arthritismus-Familien". Zeitschrift für die Gesamte Neurologie und Psychiatrie. 131: 475–501. doi:10.1007/bf02865984.
- The original version of this article was taken from the public domain source at Melkersson–Rosenthal syndrome at nih.gov Archived 2016-12-16 at the Wayback Machine
External links
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- All articles with unsourced statements
- Articles with unsourced statements from January 2013
- Articles with invalid date parameter in template
- Articles with unsourced statements from November 2020
- Articles with unsourced statements from June 2009
- Webarchive template wayback links
- Conditions of the mucous membranes
- Rare syndromes
- Syndromes affecting the nervous system
- Syndromes affecting the tongue