Encephalitis lethargica
| Encephalitis lethargica | |
|---|---|
| Other names: Economo's disease; von Economo's encephalitis[1] | |
 | |
| An illustration from von Economo's Die Encephalitis lethargica (1918) showing brain tissue of an affected monkey seen under a microscope | |
| Specialty | Neurology |
| Symptoms | Fever, headache, double vision, psychosis, lethargy[2] |
| Complications | Coma, Parkinson's, epilepsy[2][1] |
| Usual onset | Within 2 months of exposure[1] |
| Causes | Unknown[2] |
| Diagnostic method | Based on symptoms after ruling out other potential causes[1] |
| Treatment | Symptomatic treatment, levodopa[2] |
| Prognosis | Frequent long-term disability[1] |
| Frequency | Currently rare[1] |
| Deaths | 30% mortality[1] |
Encephalitis lethargica (EL) is a form of brain inflamation initially characterized by fever, headache, double vision, psychosis, and lethargy.[2] In most cases, this gradually results in some degree of coma.[1] Parkinson's or epilepsy may develop in the years following the initial illness.[2][1]
The cause is unknown.[2] Proposal include an infection such as influenza or an autoimmune process.[1] In at least some cases, the disease appeared to spread between people.[1] In pregnancy, the baby may also be affected.[1] The underlying mechanism involved inflammation of specific parts of the brain, the mesencephalon and the diencephalon.[1] Diagnosis was based on symptoms after ruling out other potential cases.[1]
Treatment is based on the symptoms.[2] Levodopa may result in significant, though temporary improvement.[2][1] Outcomes depend on the associated complications.[2] About a third of people died.[3] Many of those who survived were left with permanent disabled.[1]
Outbreaks of disease occurred around the world starting in 1916 until 1930 and affected about 5 million people.[2][1][3] Outbreaks are believed to have occurred prior, and less than 20 cases have been documented since.[1] The condition was first described by in 1917 by Constantin von Economo and Jean-René Cruchet.[4][5][1] It has also been called "sleeping sickness" or "sleepy sickness";[1] though is not related to tsetse fly-transmitted sleeping sickness.[3]
Signs and symptoms
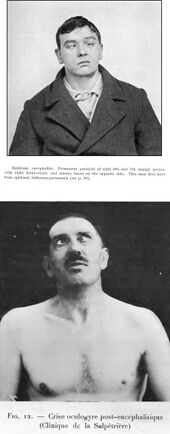
Encephalitis lethargica is characterized by high fever, sore throat, headache, lethargy, double vision, delayed physical and mental response, sleep inversion and catatonia.[6] [7] In severe cases, patients may enter a coma-like state (akinetic mutism).[citation needed] Patients may also experience abnormal eye movements ("oculogyric crises"),[8] Parkinsonism, upper body weakness, muscular pains, tremors, neck rigidity, and behavioral changes including psychosis.[citation needed] Klazomania (a vocal tic) is sometimes present.[9]
Cause

The causes of encephalitis lethargica are uncertain.[10]
Some studies have explored its origins in an autoimmune response,[6] and, separately or in relation to an immune response, links to pathologies of infectious disease – viral and bacterial,[6] e.g., in the case of influenza, where a link with encephalitis is clear.[11] Postencephalitic parkinsonism was clearly documented to have followed an outbreak of encephalitis lethargica following the 1918 influenza pandemic; evidence for viral causation of the Parkinson's symptoms is circumstantial (epidemiologic, and finding influenza antigens in encephalitis lethargica patients), while evidence arguing against this cause is of the negative sort (e.g., lack of viral RNA in postencephalitic parkinsonian brain material).[11] In reviewing the relationship between influenza and encephalitis lethargica (EL), McCall and coworkers conclude, as of 2008, that "the case against influenza [is] less decisive than currently perceived… there is little direct evidence supporting influenza in the etiology of EL," and that "[a]lmost 100 years after the EL epidemic, its etiology remains enigmatic."[12] Hence, while opinions on the relationship of encephalitis lethargica to influenza remain divided, the preponderance of literature appears skeptical.[12][13]
The German neurologist Felix Stern, who examined hundreds of encephalitis lethargica patients during the 1920s, pointed out that their encephalitis lethargica typically evolved over time. The early symptoms would be dominated by sleepiness or wakefulness. A second symptom would lead to an oculogyric crisis. The third symptom would be recovery, followed by a Parkinson-like syndrome. If patients of Stern followed this course of disease, he diagnosed them with encephalitis lethargica. Stern suspected encephalitis lethargica to be close to poliomyelitis, without evidence. Nevertheless, he experimented with the convalescent serum of survivors of the first acute syndrome. He vaccinated patients with early-stage symptoms, telling them that it might be successful. Stern is author of the definitive 1920s book, Die Epidemische Encephalitis.[14]
In 2010, in a substantial Oxford University Press compendium reviewing the historic and contemporary views on EL, its editor, Joel Vilensky, of the Indiana University School of Medicine, quotes another researcher, writing in 1930, who states, "we must confess that etiology is still obscure, the causative agent still unknown, the pathological riddle still unsolved…", and goes on to offer the following conclusion, as of that publication date:
Does the present volume solve the "riddle" of EL, which… has been referred to as the greatest medical mystery of the 20th century? Unfortunately, no: but inroads are certainly made here pertaining to diagnosis, pathology, and even treatment."[15]
Subsequent to publication of this compendium, an enterovirus was discovered in encephalitis lethargica cases from the epidemic.[16] In 2012, Oliver Sacks, the author of the book "Awakenings", about institutionalized EL survivors, acknowledged this virus as the probable cause of the disease.[17] Other sources have suggested Streptococcus pneumoniae as a cause.[18]
Diagnosis
There have been several proposed diagnostic criteria for encephalitis lethargica. One, which has been widely accepted, includes an acute or subacute encephalitic illness where all other known causes of encephalitis have been excluded. Another diagnostic criterion, suggested more recently, says that the diagnosis of encephalitis lethargica "may be considered if the patient’s condition cannot be attributed to any other known neurological condition and that they show the following signs: influenza-like signs; hypersomnolence (hypersomnia), wakeability, ophthalmoplegia (paralysis of the muscles that control the movement of the eye), and psychiatric changes."[19]
Treatment

Modern treatment approaches to encephalitis lethargica include immunomodulating therapies, and treatments to remediate specific symptoms.[20]
There is little evidence so far of a consistent effective treatment for the initial stages, though some patients given steroids have seen improvement.[21] The disease becomes progressive, with evidence of brain damage similar to Parkinson's disease.[22][needs update]
Treatment is then symptomatic. Levodopa (L-DOPA) and other anti-Parkinson drugs often produce dramatic responses; however, most people given L-DOPA experience improvements that are short lived.[23][24]
Prognosis
Many survivors of the 1915–1926 pandemic seemed to make a complete recovery and return to their normal lives. However, the majority of survivors subsequently developed neurological or psychiatric disorders, often after years or decades of seemingly perfect health. Post-encephalitic syndromes varied widely: sometimes they proceeded rapidly, leading to profound disability or death; sometimes very slowly; sometimes they progressed to a certain point and then stayed at this point for years or decades; and sometimes, following their initial onslaught, they remitted and disappeared.[25] Postencephalitic Parkinsonism is perhaps the most widely recognized of such syndromes.[citation needed]
Most of those who survived never returned to normal.
They would be conscious and aware – yet not fully awake; they would sit motionless and speechless all day in their chairs, totally lacking energy, impetus, initiative, motive, appetite, affect or desire; they registered what went on about them without active attention, and with profound indifference. They neither conveyed nor felt the feeling of life; they were as insubstantial as ghosts, and as passive as zombies.[26]
Epidemiology
Occurrences
Retrospective diagnosis tentatively suggests various historical outbreaks of encephalitis lethargica:
- In 1580, Europe was swept by a serious febrile and lethargic illness, which led to Parkinsonism and other neurological sequelae.[27]
- In 1673–1675, a similar serious epidemic occurred in London, which Thomas Sydenham described as "febris comatosa."[27]
- In 1695, a 20-year-old woman in Germany experienced oculogyric crises, Parkinsonism, diplopia, strabismus, and other symptoms following an attack of somnolent brain fever, as described by Dr. Albrecht of Hildesheim.[27]
- In 1712–1713, a severe epidemic of Schlafkrankheit (encephalitis lethargica) occurred in Tübingen, Germany, followed in many cases by persistent slowness of movement and lack of initiative (aboulia).[27]
- Between 1750 and 1800, France and Germany experienced minor epidemics of "coma somnolentum" with features of Parkinsonism , including hyperkinetic hiccough, myoclonus, chorea, and tics.
- Between 1848 and 1882, Paris-based neurologist Jean-Martin Charcot documented many isolated cases of juvenile Parkinsonism, associated with diplopia, oculogyria, tachypnoea, retropulsion, and obsessional disorders, which were almost certainly post-encephalitic in origin.[27]
- In 1890 in Italy, following the influenza epidemic of 1889–1890, a severe epidemic of somnolent illnesses (nicknamed the "Nona") appeared. For the few survivors of the Nona, Parkinsonism and other sequelae developed in almost all cases.[27]
- Between 1915 and 1926, a world-wide encephalitis lethargica pandemic occurred, impacting nearly 5 million people and killing an estimated 1.6 million people.[27]
Pandemic of 1915–1926
In the winter of 1916–1917, a "new" illness suddenly appeared in Vienna and other cities, and rapidly spread world-wide over the next three years. Earlier reports appeared throughout Europe as early as the winter of 1915–1916, but communication about the disease was slow and chaotic, given the varied manifestation of symptoms and difficulties disseminating information in wartime.[28] Until Constantin von Economo identified a unique pattern of damage among the brains of deceased patients and introduced the unifying name encephalitis lethargica, reports of the protean disease came in under a range of names: botulism, toxic ophthalmoplegia, epidemic stupor, epidemic lethargic encephalitis, acute polioencephalitis, Heine-Medin disease, bulbar paralysis, hystero-epilepsy, acute dementia, and sometimes just "an obscure disease with cerebral symptoms."[28] Just 10 days before von Economo's breakthrough in Vienna, Jean-René Cruchet described 40 cases of "subacute encephalomyelitis" in France.[28]
The number of people infected during the ten years of the pandemic is unknown, but it is estimated that more than 1 million people contracted the disease, which directly caused more than 500,000 deaths.[29][30][31] Encephalitis lethargica assumed its most virulent form between October 1918 and January 1919. The pandemic disappeared in 1927, as abruptly and mysteriously as it first appeared.[28] The great encephalitis pandemic coincided with the 1918 influenza pandemic, and it is likely that the influenza virus potentiated the effects of the causative agent of the encephalitis or lowered resistance to it in a catastrophic way.[28]
Notable cases
Notable cases include:
- Muriel "Kit" Richardson (née Hewitt), first wife of actor Sir Ralph Richardson, died of the condition in October 1942, having first shown symptoms in 1927–28.[citation needed]
- There is speculation that Adolf Hitler may have had encephalitis lethargica when he was a young adult (in addition to the more substantial case for Parkinsonism in his later years).[32][33][34][35]
- Mervyn Peake (1911–1968), author of the Gormenghast books, began his decline towards death which was initially attributed to encephalitis lethargica with Parkinson's disease-like symptoms, although others have later suggested his decline in health and eventual death may have been due to Lewy body dementia.[36][37]
- Those described in the book Awakenings by the British neurologist Oliver Sacks.[24]
- Jane Norton Grew Morgan, wife of J. P. Morgan Jr., died of encephalitis lethargica in 1925. At the time, doctors attributed her encephalitis to having contracted influenza during the 1918 pandemic.[38]
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 1.17 1.18 1.19 Berger JR, Vilensky JA (2014). "Encephalitis lethargica (von Economo's encephalitis)". Handbook of Clinical Neurology. 123: 745–761. doi:10.1016/B978-0-444-53488-0.00036-5. ISBN 9780444534880. PMID 25015515.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 "Encephalitis Lethargica Information Page | National Institute of Neurological Disorders and Stroke". www.ninds.nih.gov. Archived from the original on 4 January 2017. Retrieved 6 July 2021.
- ↑ 3.0 3.1 3.2 Harley, Trevor A. (18 February 2021). The Science of Consciousness. Cambridge University Press. p. 282. ISBN 978-1-107-12528-5. Archived from the original on 28 August 2021. Retrieved 6 July 2021.
- ↑ Economo's disease at Who Named It?
- ↑ von Economo, K. (May 10, 1917). "Die Encephalitis lethargica". Wiener klinische Wochenschrift [Vienna clinical weekly] (in Deutsch). Leipzig and Vienna: Franz Deuticke 1918. 30: 581–585.
- ↑ 6.0 6.1 6.2 Dale, Russell C.; Church, Andrew J.; Surtees, Robert A.H.; Lees, Andrew J.; Adcock, Jane E.; Harding, Brian; Neville, Brian G. R.; Giovannoni, Gavin (2004). "Encephalitis Lethargica Syndrome: 20 New Cases and Evidence of Basal Ganglia Autoimmunity". Brain. 127 (1): 21–33. doi:10.1093/brain/awh008. PMID 14570817.
- ↑ Koch, Christof (March–April 2016). "Sleep without End". Scientific American Mind. 27 (2): 22–25. doi:10.1038/scientificamericanmind0316-22.
- ↑ Vilensky, J.A.; Goetz, C.G.; Gilman, S. (2006). "Movement Disorders Associated with Encephalitis Lethargica: A Video Compilation". Mov. Disord. 21 (1, January): 1–8. doi:10.1002/mds.20722. PMID 16200538. S2CID 34382398.
- ↑ Jankovic, J.; Mejia, N.I. (2006). "Tics Associated with Other Disorders". Adv. Neurol. 99: 61–68. PMID 16536352.
- ↑ McCall, S.; Vilensky, J.A.; Gilman, S.; Taubenberger, J.K. (2008). "The Relationship Between Encephalitis Lethargica and Influenza: A Critical Analysis". J. Neurovirol. 14 (3, May): 177–185. doi:10.1080/13550280801995445. PMC 2778472. PMID 18569452.
- ↑ 11.0 11.1 Haeman, Jang; Boltz, D.; Sturm-Ramirez, K.; Shepherd, K.R.; Jiao, Y.; Webster, R.; Smeyne, Richard J. (2009). "Highly Pathogenic H5N1 Influenza Virus Can Enter the Central Nervous System and Induce Neuroinflammation and Neurodegeneration". Proceedings of the National Academy of Sciences. 106 (33, August 10): 14063–14068. doi:10.1073/pnas.0900096106. PMC 2729020. PMID 19667183. Archived from the original on 28 August 2021. Retrieved 8 December 2015.
- ↑ 12.0 12.1 Reid, A.H.; McCall, S.; Henry, J.M.; Taubenberger, J.K. (2001). "Experimenting on the Past: The Enigma of von Economo's Encephalitis Lethargica". J. Neuropathol. Exp. Neurol. 60 (7): 663–670. doi:10.1093/jnen/60.7.663. PMID 11444794.
- ↑ Vilensky, J.A.; Foley, P.; Gilman, S. (2007). "Children and Encephalitis Lethargica: A Historical Review". Pediatr. Neurol. 37 (2, August): 79–84. doi:10.1016/j.pediatrneurol.2007.04.012. PMID 17675021. Archived from the original on 17 April 2020. Retrieved 8 December 2015.
- ↑ "Auf der Spur der Schlaf-Epidemie". Spektrum.de (in Deutsch). 2019-01-25. Archived from the original on 2019-01-26. Retrieved 2019-01-28.
- ↑ Vilensky, J.A.; Gilman, S. (2010). "Introduction". In Vilensky, Joel A. (ed.). Encephalitis Lethargica: During and After the Epidemic. Oxford: Oxford University Press. pp. 3–7, esp. 6f. ISBN 978-0190452209. Retrieved 8 December 2015.
- ↑ Dourmashkin, Robert R.; Dunn, Glynis; Castano, Victor; McCall, Sherman A. (2012-01-01). "Evidence for an enterovirus as the cause of encephalitis lethargica". BMC Infectious Diseases. 12: 136. doi:10.1186/1471-2334-12-136. ISSN 1471-2334. PMC 3448500. PMID 22715890.
- ↑ Letter from Oliver Sacks to Professor Joel A. Vilensky, 9 Sept 2012.
- ↑ "Mystery of the forgotten plague". 27 July 2004. Archived from the original on 13 May 2008. Retrieved 3 June 2021 – via news.bbc.co.uk.
- ↑ Easton, Ava. "Encephalitis Lethargica". The Encephalitis Society. Archived from the original on 28 December 2017. Retrieved 27 December 2017.
- ↑ Lopez-Alberola, R.; Georgiou, M.; Sfakianakis, G.N.; Singer, C.; Papapetropoulos, S. (2009). "Contemporary Encephalitis Lethargica: Phenotype, Laboratory Findings and Treatment Outcomes". J. Neurol. 256 (3, March): 396–404. doi:10.1007/s00415-009-0074-4. PMID 19412724. S2CID 38388333.
- ↑ Blunt, S.B.; Lane, R.J.; Turjanski, N.; Perkin, G.D. (1997). "Clinical Features and Management of Two Cases of Encephalitis Lethargica". Mov. Disord. 12 (3): 354–359. doi:10.1002/mds.870120314. PMID 9159730. S2CID 14741885.
- ↑ Kohnstamm, P. (1934). "Über die Beteiligung der beiden Schichten der Substantia nigra am Prozeß der Encephalitis epidemica". J Psychol Neurol (in Deutsch). 46 (1): 22–37.
- ↑ "Encephalitis Lethargica Information Page". National Institute of Neurological Disorders and Stroke. August 9, 2018. Archived from the original on January 4, 2017. Retrieved June 3, 2021.
- ↑ 24.0 24.1 (Sacks 1990)[page needed]
- ↑ (Sacks 1990, pp. 20–21)
- ↑ (Sacks 1990, p. 14)
- ↑ 27.0 27.1 27.2 27.3 27.4 27.5 27.6 (Sacks 1990, pp. 319–321)
- ↑ 28.0 28.1 28.2 28.3 28.4 (Sacks 1990, pp. 12–19)
- ↑ Ravenholt, R. T; Foege, WilliamH (1982-10-16). "1918 Influenza, Encephalitis Lethargica, Parkinsonism". The Lancet. Originally published as Volume 2, Issue 8303. 320 (8303): 860–864. doi:10.1016/S0140-6736(82)90820-0. ISSN 0140-6736. PMID 6126720. S2CID 45138249. Archived from the original on 2021-07-12. Retrieved 2021-06-03.
- ↑ McCall, Sherman; Vilensky, Joel A; Gilman, Sid; Taubenberger, Jeffery K (May 2008). "The relationship between encephalitis lethargica and influenza: A critical analysis". Journal of Neurovirology. 14 (3): 177–185. doi:10.1080/13550280801995445. ISSN 1355-0284. PMC 2778472. PMID 18569452.
- ↑ Hoffman, Leslie A.; Vilensky, Joel A. (2017-08-01). "Encephalitis lethargica: 100 years after the epidemic". Brain. 140 (8): 2246–2251. doi:10.1093/brain/awx177. ISSN 0006-8950. PMID 28899018. Archived from the original on 2021-03-04. Retrieved 2021-06-03.
- ↑ Lieberman, A (April 1996). "Adolf Hitler Had Post-Encephalitic Parkinsonism". Parkinsonism Relat Disord. 2 (2): 95–103. doi:10.1016/1353-8020(96)00005-3. PMID 18591024.
- ↑ Boettcher, L.B.; Bonney, P.A.; Smitherman A.D.; Sughrue, M.E. (2015). "Hitler's Parkinsonism". Neurosurg Focus. 39 (1, July): E8. doi:10.3171/2015.4.FOCUS1563. PMID 26126407.
- ↑ Gupta, R; Kim, C; Agarwal, N; Lieber, B & Monaco, E.A. (2015). "Understanding the Influence of Parkinson's Disease on Adolf Hitler's Decision-Making During World War II". World Neurosurg. 84 (5, November): 1447–1452. doi:10.1016/j.wneu.2015.06.014. PMID 26093359.
{{cite journal}}: CS1 maint: uses authors parameter (link) - ↑ Rosen, Denis (2010). "Review: "Asleep: the Forgotten Epidemic That Remains One of Medicine's Greatest Mysteries" [Molly Caldwell Crosby". J. Clin. Sleep Med. 6 (3, 15 June): 299. doi:10.5664/jcsm.27831. PMC 2883045.
- ↑ Demetrios J. Sahlas (2003). "Dementia With Lewy Bodies and the Neurobehavioral Decline of Mervyn Peake". Arch. Neurol. 60 (6): 889–892. doi:10.1001/archneur.60.6.889. PMID 12810496.
- ↑ McMillan, Roy; Peake (20 July 2011) [1959]. Butcher Sara (ed.). Publisher's Liner Notes on Mervyn Peake for 'Titus Alone' (Liner Notes/ Reference Guide for Abridged Audiobook of Titus Alone). Audible.com (PDF, Liner Notes) (Abridged, Audio ed.). Germany: Naxos Audiobooks. p. 7. ISBN 978-184-379-542-1. Retrieved 2 May 2018.
But the plays were not the financial winners he had hoped for, and he suffered another nervous breakdown in 1957. This led to the more evident display of the symptoms of a type of Parkinson’s Disease which, alongside the effects of encephalitis lethargica that he contracted in childhood, was slowly to kill him over more than a decade.
[permanent dead link] - ↑ Chernow, Ron (1990). The House of Morgan: An American Banking Dynasty and the Rise of Modern Finance. United States: Atlantic Monthly Press. ISBN 0-87113-338-5.
External links
| Classification |
|---|
- Sacks, Oliver (1990). Awakenings. Vintage Books. ISBN 978-0-375-70405-5. OCLC 21910570.
- Sacks O (1983). "The origin of 'Awakenings'". Br. Med. J. (Clin. Res. Ed.). 287 (6409): 1968–1969. doi:10.1136/bmj.287.6409.1968. PMC 1550182. PMID 6418286.
- Reid, A.H.; McCall, S.; Henry, J.M.; Taubenberger, J.K. (2001). "Experimenting on the Past: The Enigma of von Economo's Encephalitis Lethargica". J. Neuropathol. Exp. Neurol. 60 (7): 663–670. doi:10.1093/jnen/60.7.663. PMID 11444794.
- Vilensky, J.A.; Foley, P.; Gilman, S. (2007). "Children and Encephalitis Lethargica: A Historical Review". Pediatr. Neurol. 37 (2, August): 79–84. doi:10.1016/j.pediatrneurol.2007.04.012. PMID 17675021.
- Vilensky, Joel A., ed. (2010). Encephalitis Lethargica: During and After the Epidemic. Oxford, UK: Oxford University Press. ISBN 978-0190452209.
- Crosby, Molly Caldwell (2010). 'Asleep: The Forgotten Epidemic that Remains One of Medicine's Greatest Mysteries. New York: Penguin/Berkley.[ISBN missing] – Describes the history of the disease, and the epidemic of the 1920s.
- Mystery of the Forgotten Plague Archived 2008-05-13 at the Wayback Machine: BBC news item about the tracing of the infectious agent in encephalitis lethargica
- Pages with script errors
- CS1: Julian–Gregorian uncertainty
- CS1 Deutsch-language sources (de)
- Wikipedia articles needing page number citations from June 2021
- Articles with invalid date parameter in template
- CS1 maint: uses authors parameter
- All articles with dead external links
- Articles with dead external links from March 2022
- Articles with permanently dead external links
- All articles with unsourced statements
- Articles with unsourced statements from December 2015
- Wikipedia articles in need of updating from December 2015
- All Wikipedia articles in need of updating
- Articles with unsourced statements from October 2020
- Pages with missing ISBNs
- Webarchive template wayback links
- Encephalitis
- Unsolved problems in neuroscience
- Ailments of unknown cause
- Viral infections of the central nervous system
- RTT