List of types of fungal infection
Jump to navigation
Jump to search
Fungal infection, also known as mycosis, is disease caused by fungi.[1] Dermatophytosis is a group fungal infections of the skin, caused by dermatophytes; species of Trichophyton, Microsporum, and Epidermophyton.[2][3][4] These fungi characteristically affect the outer outer layer of skin, hair shaft and the nail.[1] Non-dermatophyte superficial dermatomycoses includes pityriasis versicolor and tinea nigra.[1]
| Mycosis[1] | ICD-11 code[1] | Type[1] | Sub-type[1] | Signs and symptoms | Cause | Image |
|---|---|---|---|---|---|---|
| Aspergillosis[1] | 1F20 | Invasive | Aspergillus[1] | 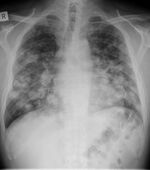
| ||
| Non-invasive | ||||||
| Aspergilloma[5] | 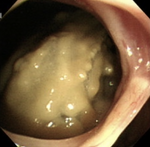
| |||||
| CA82.4 | Aspergillus-induced allergic or hypersensitivity conditions | |||||
| KA63.1 | Neonatal aspergillosis | |||||
| 1F20.Z | Aspergillosis, unspecified | |||||
| Basidiobolomycosis[1] | 1F21 | Basidiobolus ranarum | 
| |||
| Blastomycosis[1] | 1F22 | Blastomyces dermatitidis | 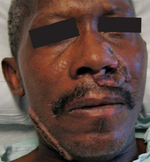
| |||
| Candidiasis[1] | 1F23 | Candidosis of lips or oral mucous membranes | Candida | 
| ||
| Candidosis of skin or mucous membranes | ||||||
| Candidosis of gastrointestinal tract | ||||||
| Systemic or invasive candidosis | ||||||
| Other specified and unspecified candidosis | ||||||
| Neonatal candidosis | ||||||
| EH12 | Congenital cutaneous candidiasis | 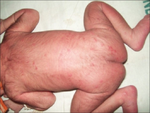
| ||||
| Chromoblastomycosis[1] | 1F24 | 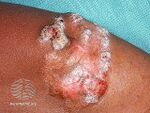
| ||||
| Coccidioidomycosis[1] | 1F25 | Coccidioides immitis or Coccidioides posadasii | 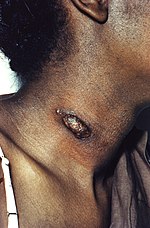
| |||
| Conidiobolomycosis[1] | 1F26 | Conidiobolus coronatus | 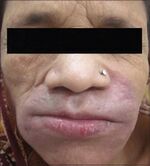
| |||
| Cryptococcosis[1] | 1F27 | Cryptococcus neoformans | 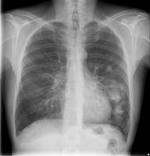
| |||
| Dermatophytosis[2]
(Trichophyton, Microsporum, Epidermophyton) Stratum corneum, hair, nails |
1F28 | Disseminated dermatophytosis | ||||
| Tinea barbae
(beard) Tinea sycosis[2] |
Patch[2]
Scale Hair loss |
Trichophyton violaceum, Trichophyton rubrum | 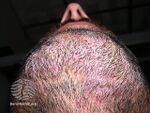
| |||
| Tinea capitis
(scalp) |
Trichophyton, Microsporum[2] | 
| ||||
| Kerion | Trichophyton, Microsporum[2] | 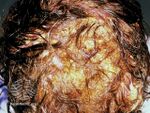
| ||||
| Favus | 
| |||||
| Tinea cruris
(groin) |
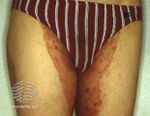
| |||||
| Tinea unguium
(nail) |
||||||
| Dermatophytes, Fusarium | 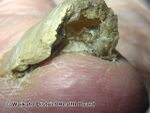
| |||||
| Tinea faciei
(face) |
Photosensitive[2]
Red Scale Indistinct border |
T. rubrum, T. mentagrophytes, T. tonsurans, M. gypseum, M.canis | 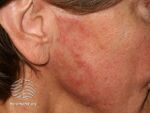
| |||
| Tinea imbricata
(Tokelau) |
Rings[2] | Trichophyton concentricum | 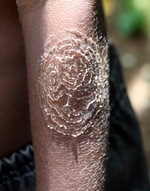
| |||
| Tinea corporis
(body) |
Trichophyton concentricum | Patch (circular)[2]
Red or pale Scale at edge
|
Trichophyton, Microsporum, Epidermophyton | 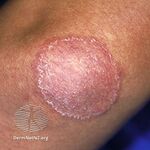
| ||
| Tinea pedis
(feet) |
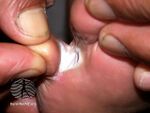
| |||||
| Tinea manuum
(hands) |
Trichophyton rubrum | 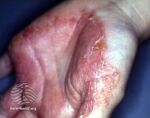
| ||||
| Emmonsiosis | 1F2L | Disseminated adiaspiromycosis | Emmonsia | |||
| Pulmonary adiaspiromycosis | ||||||
| Eumycetoma | 1F29 | Madurella mycetomatis, Madurella grisea, Leptosphaeria senegalensis, Curvularia lunata, Scedosporium apiospermum, Neotestudina rosatii, Acremonium spp. and Fusarium spp.. | 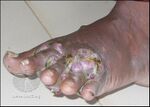
| |||
| Histoplasmosis | 1F2A | Histoplasma capsulatum[6] | 
| |||
| Pulmonary histoplasmosis capsulati | ||||||
| Histoplasmosis due to Histoplasma duboisii | ||||||
| Lobomycosis | 1F2B | Lacazia loboi | 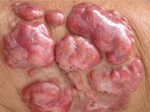
| |||
| Mucormycosis | 1F2C | Mucorales | 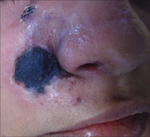
| |||
| Myelitis due to fungus | 1D02.2 | |||||
| Non-dermatophyte superficial dermatomycoses | 1F2D | Pityriasis versicolor | 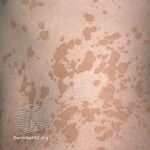
| |||
| Malassezia folliculitis | 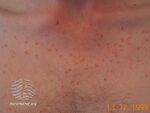
| |||||
| White piedra | 
| |||||
| Black piedra | ||||||
| Tinea nigra | Brown macules that scrape off easily[2]
Palms, soles |

| ||||
| Onychomycosis due to non-dermatophyte | Onychomycosis due to non-dermatophyte mould | |||||
| Candida onychomycosis | ||||||
| Paracoccidioidomycosis | 1F2E | Pulmonary paracoccidioidomycosis | 'Paracoccidioides | |||
| Disseminated paracoccidioidomycosis | 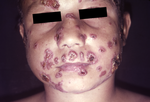
| |||||
| Phaeohyphomycosis | 1F2F | 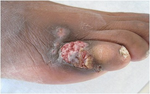
| ||||
| Pneumocystosis | 1F2G | Pulmonary pneumocystosis | Pneumocystis jirovecii | 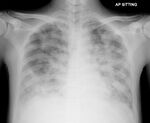
| ||
| Scedosporiosis (Lomentospora prolificans) | 1F2H | Scedosporium | ||||
| Sporotrichosis[7] | 1F2J | Lymphocutaneous sporotrichosis | Sporothrix schenckii | |||
| Fixed cutaneous sporotrichosis | Sporothrix schenckii | 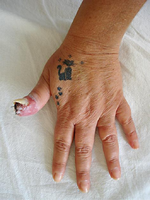
| ||||
| Disseminated sporotrichosis | ||||||
| Other specified sporotrichosis | ||||||
| Sporotrichosis, unspecified | ||||||
| Talaromycosis | 1F2K | Talaromyces marneffei | 
|
See also
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 "ICD-11 - ICD-11 for Mortality and Morbidity Statistics". icd.who.int. Archived from the original on 1 August 2018. Retrieved 25 May 2021.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 2.9 James, William D.; Elston, Dirk; Treat, James R.; Rosenbach, Misha A.; Neuhaus, Isaac (2020). "15. Diseases resulting from fungi and yeasts". Andrews' Diseases of the Skin: Clinical Dermatology (13th ed.). Edinburgh: Elsevier. pp. 291–323. ISBN 978-0-323-54753-6. Archived from the original on 2023-07-01. Retrieved 2023-06-26.
- ↑ Begum, Jubeda; Mir, Nasir A.; Lingaraju, Madhu C.; Buyamayum, Bidyarani; Dev, Kapil (2020). "Recent advances in the diagnosis of dermatophytosis". Journal of Basic Microbiology. 60 (4): 293–303. doi:10.1002/jobm.201900675. ISSN 1521-4028. Archived from the original on 2023-07-01. Retrieved 2021-11-03.
- ↑ "Dermatophytosis (Tinea Infections). Medical information. Patient". patient.info. Archived from the original on 21 May 2021. Retrieved 21 May 2021.
- ↑ Chakraborty, Rebanta K.; Baradhi, Krishna M. (2023). "Aspergilloma". StatPearls. StatPearls Publishing. Archived from the original on 2022-08-17. Retrieved 2023-07-30.
- ↑ Toscanini, María Agustina; Nusblat, Alejandro David; Cuestas, María Luján (March 2021). "Diagnosis of histoplasmosis: current status and perspectives". Applied Microbiology and Biotechnology. 105 (5): 1837–1859. doi:10.1007/s00253-021-11170-9. ISSN 1432-0614. PMID 33587157. Archived from the original on 2023-05-18. Retrieved 2023-06-16.
- ↑ "Sporotrichosis". www.cdc.gov. CDC. 9 February 2022. Archived from the original on 13 March 2023. Retrieved 22 June 2023.