Patellar tendinitis
| Patellar tendinitis | |
|---|---|
| Other names: Quadriceps tendinopathy, patellar tendinopathy, jumper's knee, patellar tendinosis, patellar tendinitis | |
 | |
| Location of the pain in patellar tendinitis | |
| Specialty | Orthopedics, sports medicine |
| Symptoms | Pain at the front of the knee[1] |
| Complications | Patellar tendon rupture[2] |
| Risk factors | Jumping sports, being overweight[1] |
| Diagnostic method | Based on symptoms and examination[2] |
| Differential diagnosis | Chondromalacia patella, Osgood-Schlatter disease, patellofemoral syndrome, infrapatellar bursitis[1][2] |
| Treatment | Rest, physical therapy[2] |
| Prognosis | Recovery can be slow[2] |
| Frequency | 14% of athletes[1] |
Patellar tendinitis, also known as jumper's knee, is an overuse injury of the tendon that straightens the knee.[1] Symptoms include pain in the front of the knee.[1] Typically the pain and tenderness is at the lower part of the kneecap, though the upper part may also be affected.[2] Generally there is not pain when the person is at rest.[2] Complications may include patellar tendon rupture.[2]
Risk factors include being involved in athletics and being overweight.[1] It is particularly common in athletes who are involved in jumping sports such as basketball and volleyball.[1][2] The underlying mechanism involves small tears in the tendon connecting the kneecap with the shinbone.[2] Diagnosis is generally based on symptoms and examination.[2] Other conditions that can appear similar include infrapatellar bursitis, chondromalacia patella and patellofemoral syndrome.[1][2]
Treatment often involves resting the knee and physical therapy.[2] Evidence for treatments, including rest, however is poor.[3][4] Recovery can take a year.[2] It is relatively common with about 14% of athletes currently affected.[1] Males are more commonly affected than females.[2] The term "jumper's knee" was coined in 1973.[2]
Signs and symptoms
People report anterior knee pain, often with an aching quality. The symptom onset is insidious. Rarely is a discrete injury described. Usually, the problem is below the kneecap but it may also be above. Jumper's knee can be classified into 1 of 4 stages, as follows:[2]
- Stage 1 – Pain only after activity, without functional impairment
- Stage 2 – Pain during and after activity, although the person is still able to perform satisfactorily in his or her sport
- Stage 3 – Prolonged pain during and after activity, with increasing difficulty in performing at a satisfactory level
- Stage 4 – Complete tendon tear requiring surgical repair
It begins as inflammation in the patellar tendon where it attaches to the patella and may progress by tearing or degenerating the tendon. People present with an ache over the patella tendon.[5]
Causes
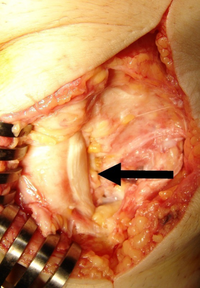
It is an overuse injury from repetitive overloading of the extensor mechanism of the knee. The microtears exceed the body's healing mechanism unless the activity is stopped.[6]
This condition may also be due to a para-articular/extraskeletal osteochondroma[citation needed]
Risk factors
Among the risk factors for patellar tendonitis are low ankle dorsiflexion, weak gluteal muscles, and muscle tightness, particularly in the calves, quadriceps muscle, and hamstrings.[7]
It may be associated with stiff ankle movement and ankle sprains.[8]
Diagnosis
Diagnosis is generally based on symptoms and a physical examination.[2]
Ultrasound or magnetic resonance imaging may help clarify how severe the problem is.[2]
Magnetic resonance imaging can reveal edema (increased T2 signal intensity) in the proximal aspect of the patellar tendon.[9]
Treatment
Evidence for treatment is poor.[3] In the early stages rest, ice, compression, and elevation may be tried. Tentative evidence supports exercises involving eccentric muscle contractions of the quadriceps on a decline board.[10] Specific exercises and stretches to strengthen the muscles and tendons may be recommended, eg. cycling or swimming. Use of a strap for jumper's knee and suspension inlays for shoes may also reduce the problems. Corticosteroid injections and NSAIDs are not generally recommended.[2]
Procedures
Dry needling, sclerosing injections, platelet-rich plasma, extracorporeal shock wave treatment, and heat therapy have been tried.[2]
Surgery
Surgery may be tried if other measures fail.[2] This is reserved for people with severe pain for months despite conservative measures. Knee operations in most cases have no better effects than exercise programs, however in refractory cases they do produce a better prognosis[5]
Epidemiology
It is relatively common with about 14% of athletes currently affected.[1] Males are more commonly affected than females.[2]
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 King, D; Yakubek, G; Chughtai, M; Khlopas, A; Saluan, P; Mont, MA; Genin, J (February 2019). "Quadriceps tendinopathy: a review-part 1: epidemiology and diagnosis". Annals of Translational Medicine. 7 (4): 71. doi:10.21037/atm.2019.01.58. PMC 6409230. PMID 30963066.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 2.17 2.18 2.19 2.20 2.21 2.22 Santana, JA; Sherman, Al (January 2019). "Jumpers Knee". StatPearls. PMID 30422564.
- ↑ 3.0 3.1 Mendonça, LM; Leite, HR; Zwerver, J; Henschke, N; Branco, G; Oliveira, VC (6 June 2019). "How strong is the evidence that conservative treatment reduces pain and improves function in individuals with patellar tendinopathy? A systematic review of randomised controlled trials including GRADE recommendations". British Journal of Sports Medicine. 54 (2): bjsports–2018–099747. doi:10.1136/bjsports-2018-099747. PMID 31171514.
- ↑ Saithna, Adnan; Gogna, Rajiv; Baraza, Njalalle; Modi, Chetan; Spencer, Simon (30 November 2012). "Eccentric Exercise Protocols for Patella Tendinopathy: Should we Really be Withdrawing Athletes from Sport? A Systematic Review". The Open Orthopaedics Journal. 6 (1): 553–557. doi:10.2174/1874325001206010553. ISSN 1874-3250. PMC 3522085. PMID 23248727.
- ↑ 5.0 5.1 Schwartz, Aaron; Watson, Jonathan N.; Hutchinson, Mark R. "Patellar Tendinopathy". Sports Health. 7 (5): 415–420. doi:10.1177/1941738114568775. ISSN 1941-7381. Archived from the original on 29 August 2021. Retrieved 12 October 2020.
- ↑ Brotzman, S. Brent. "59 - Overuse Syndromes of the Knee". Clinical Orthopaedic Rehabilitation: a Team Approach (Fourth Edition). Content Repository Only!. p. 397. ISBN 978-0-323-39370-6. Archived from the original on 7 November 2020. Retrieved 12 October 2020.
- ↑ Koban, Martin (2013). Beating Patellar Tendonitis. pp. 20–25. ISBN 978-1491049730.
- ↑ Backman LJ, Danielson P (December 2011). "Low range of ankle dorsiflexion predisposes for patellar tendinopathy in junior elite basketball players: a 1-year prospective study". The American Journal of Sports Medicine. 39 (12): 2626–33. doi:10.1177/0363546511420552. PMID 21917610.
- ↑ Pedowitz, Robert; Chung, Christine B.; Resnick, Donald. Magnetic Resonance Imaging in Orthopedic Sports Medicine. Springer Science & Business Media. p. 331. ISBN 978-0-387-48897-4. Archived from the original on 29 August 2021. Retrieved 12 October 2020.
- ↑ Visnes H, Bahr R (April 2007). "The evolution of eccentric training as treatment for patellar tendinopathy (jumper's knee): a critical review of exercise programmes". British Journal of Sports Medicine. 41 (4): 217–23. doi:10.1136/bjsm.2006.032417. PMC 2658948. PMID 17261559.
External links
| Classification | |
|---|---|
| External resources |