Synovial osteochondromatosis
| Synovial osteochondromatosis | |
|---|---|
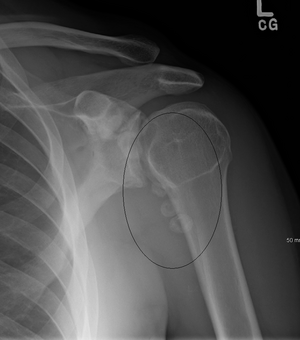 | |
| Synovial osteochondromatosis | |
Synovial osteochondromatosis (SOC) (synonyms include synovial chondromatosis, primary synovial chondromatosis, synovial chondrometaplasia) is a rare disease that creates a benign change or proliferation in the synovium or joint-lining tissue, which changes to form bone-forming cartilage. In most occurrences, there is only one joint affected, either the knee, the hip, or the elbow. Rarely involves the TMJ.[1]
The cause is unknown.
In this condition, cartilaginous metaplasia takes place within the synovial membrane of the joint. Metaplastic synovium organizes into nodules. With minor trauma, nodules are shed as small bodies into the joint space. In some patients, the disease process may involve tendon sheaths and bursal sacs.
Cartilaginous intra-articular bodies float freely within the synovial fluid, which they require for nutrition and growth. Progressive enlargement and ossification occur with time. If they remain free, they continue to grow larger and more calcified. In severe cases, they may occupy the entire joint space or penetrate to adjacent tissues. Also, they can deposit in the synovial lining, reestablish a blood supply, and become replaced by bone. On occasion, synovial reattachment can lead to complete reabsorption of the cartilage fragment.
Signs and symptoms
Chronic, progressive pain and swelling of the affected joint are exacerbated by physical activity. Joint effusion and limited range of motion are common associated features. It affects primarily large joints, including knee (>50% of cases), elbow, hip, and shoulder. SOC is twice as common in men as women. Some patients have intra-articular bodies resting in stable positions within joint recesses or bursae. These patients may be asymptomatic, with SOC merely as an incidental finding at imaging.[citation needed]
Complications
Malignant transformation to synovial chondrosarcoma. This is a very rare complication occurring in chronic cases. Treatment entails synovial excision and total joint replacement.[citation needed]
Clicking, grating, or locking may result from acute mechanical problems due to intra-articular bodies within the affected joint. Locking may destroy articular cartilage, resulting in secondary osteoarthritis. Symptoms such as joint stiffness and aching are the result of osteoarthritis that sets in after years of persistent joint irritation.[2]
Cause
The cause of synovial osteuchondromatosis is likely due to synovial metaplasia and results in multiple calcified periarticular bodies[3]
Diagnosis
Radiography
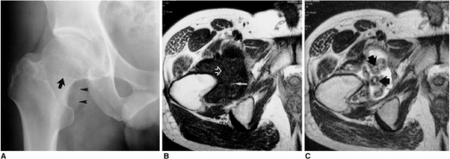
Typical finding is of multiple, smooth, oval-shaped calcified masses within the joint space or bursa. They have a characteristic popcorn-ball appearance of calcified cartilage. With serial imaging, masses may be found to change in size, disappear, or migrate to recessed areas of the joint. They may pass from the main joint cavity into a neighboring synovial cyst. For this reason, a mass may not be appreciated within the actual joint space itself.[citation needed]
Additional radiographic findings include joint effusion and degenerative changes such as joint space narrowing, subchondral sclerosis, and osteophyte formation.[citation needed]
Computed tomography
CT is best utilized in earlier stages of the disease process before cartilaginous bodies have calcified (become filled with calcium). CT can effectively detect non-calcified masses or those with only minimal calcification, which allows the radiologist to distinguish this condition from a simple joint effusion.[citation needed]
Magnetic resonance imaging
MR appearance depends on the composition of the intra-articular body. Entirely cartilaginous bodies will appear isointense to muscle on T1 and hyperintense to muscle on T2 weighted images. Partly calcified intra-articular bodies demonstrate foci of absent signal on all pulse sequences. Like CT arthrography, MR with gadolinium may be used to detect intra-articular bodies that have not yet calcified.[citation needed]
Pathology
Cartilaginous bodies or osteocartilaginous bodies with central ossification may be noted. They are typically spherical in shape. Sizes range from several millimeters to several centimeters in diameter. The synovium of the involved joint demonstrates villous hyperplasia, which imparts a wrinkled appearance on gross examination. There may be cartilaginous bodies attached to the synovium. Synovial involvement may be focal or diffuse in nature.[4]
Differential diagnosis
- Trauma-related:
- Fracture with avulsed fragment
- Fragmentation of meniscus with calcification
- Degenerative joint disease related:
- Degenerative joint disease with detached spur
- Synovial proliferation:
- Pigmented villonodular synovitis
- Neoplastic:
- Synovial chondrosarcoma
- Other:
- Osteochondritis dissecans
- Sequestrum from osteomyelitis
- Neuropathic (Charcot) joint
Intra-articular bodies in SOC typically have popcorn calcification, with a dense sclerotic border with radiolucent central region. This distinct radiographic appearance sets it apart from other causes of intra-articular bodies. Number and size of intra-articular bodies can prove helpful as well. SOC typically presents as multiple intra-articular bodies. Few or isolated intra-articular bodies are more consistent with trauma or osteoarthritis.[citation needed]
Classification
Classification is divided into primary versus secondary SOC. Primary SOC occurs in an otherwise normal joint. It is suggested by monoarticular involvement in a patient in the third to fifth decades of life. Secondary SOC occurs in older patients in joints previously affected by joint disease such as osteoarthritis. This pattern is suggested by bilateral involvement with multiple joint intra-articular bodies.[citation needed]
Treatment
Asymptomatic patients do not require therapy. Symptomatic patients should undergo arthroscopic or surgical removal of intra-articular bodies. Patients who have recurrent intra-articular bodies or in whom the entire synovial lining is metaplastic require total synovectomy.[citation needed]
References
- ↑ Fuller E, Bharatha A, Yeung R, Kassel EE, Aviv RI, Howard P, Symons SP. Case of the month #166: synovial chondromatosis of the temporal mandibular joint. Canadian Association of Radiologists Journal. 2011 May; 62(2):151-153.
- ↑ "Chondrosarcoma". The Lecturio Medical Concept Library. Archived from the original on 9 July 2021. Retrieved 8 July 2021.
- ↑ Crotty, J. M.; Monu, J. U.; Pope, T. L. (March 1996). "Synovial osteochondromatosis". Radiologic Clinics of North America. 34 (2): 327–342, xi. ISSN 0033-8389. Archived from the original on 18 June 2022. Retrieved 6 July 2022.
- ↑ "Synovial Chondromatosis". Genetic And Rare Disease Information Centre. Archived from the original on 18 March 2021. Retrieved 8 July 2021.
Further reading
- FletcherCDM, UnniKK, MertensF, editors. Pathology and genetics of tumours of soft tissue and bone. World Health Organization classification of tumours. Lyon: IARC Press, 2002.
- Bianchi S, Martinoli C (July 1999). "Detection of loose bodies in joints". Radiol. Clin. North Am. 37 (4): 679–90. doi:10.1016/S0033-8389(05)70123-8. PMID 10442075.
- Coles MJ, Tara HH (January 1997). "Synovial chondromatosis: a case study and brief review". Am. J. Orthop. 26 (1): 37–40. PMID 9021034.
- Crotty JM, Monu JU, Pope TL (March 1996). "Synovial osteochondromatosis". Radiol. Clin. North Am. 34 (2): 327–42, xi. PMID 8633119.
- Maurice H, Crone M, Watt I (1 November 1988). "Synovial chondromatosis". J Bone Joint Surg Br. 70 (5): 807–11. doi:10.1302/0301-620X.70B5.3192585. PMID 3192585.
{{cite journal}}: CS1 maint: url-status (link) - Milgram JW, Gilden JJ, Gilula LA (January 1996). "Multiple loose bodies: formation, revascularization, and resorption. A 29-year followup study". Clin. Orthop. Relat. Res. (322): 152–7. doi:10.1097/00003086-199601000-00019. PMID 8542691. S2CID 25265519.
External links
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- All articles with unsourced statements
- Articles with unsourced statements from September 2020
- Articles with invalid date parameter in template
- Articles with unsourced statements from December 2020
- Articles with unsourced statements from September 2021
- CS1 maint: url-status
- Ailments of unknown cause
- Rare diseases
- Soft tissue disorders