Osteophyte
| Osteophyte | |
|---|---|
 | |
| Small marginal osteophytes (arrows) of the processus anconeus of the ulna can be seen in this gross pathological specimen of a sow. | |
| Specialty | Orthopedics |
Osteophytes are exostoses (bony projections) that form along joint margins.[1] They should not be confused with enthesophytes, which are bony projections that form at the attachment of a tendon or ligament.[2] Osteophytes are not always distinguished from exostoses in any definite way, although in many cases there are a number of differences.[3] Osteophytes are typically intra-articular (within the joint capsule).[4]
Classification
The classification of osteophytes can be either vertebral or extraspinal[5]
Cause
A range of bone-formation processes are associated with aging, degeneration, mechanical instability, and disease (such as diffuse idiopathic skeletal hyperostosis). Osteophyte formation has classically been related to sequential and consequential changes in such processes. Often osteophytes form in osteoarthritic joints as a result of damage and wear from inflammation. Calcification and new bone formation can also occur in response to mechanical damage in joints.[6] >
Pathophysiology
Osteophytes form because of the increase in a damaged joint's surface area. This is most common from the onset of arthritis. Osteophytes usually limit joint movement and typically cause pain.[7]
Osteophytes form naturally on the back of the spine as a person ages and are a clinical sign of degeneration in the spine. In this case, the osteophytes are commonly not the source of back pains, but instead are a sign of an underlying problem. However, osteophytes on the spine can impinge on nerves that leave the spine for other parts of the body. This impingement can cause pain in both upper and lower limbs and a numbness or tingling sensations in the hands and feet because the nerves are supplying sensation to their dermatomes.[7]
Osteophytes on the fingers or toes are known as Heberden's nodes (if on the distal interphalangeal joint) or Bouchard's nodes (if on the proximal interphalangeal joints).
Diagnosis
The evaluation of osteophytes can be done via radiographs[8]
-
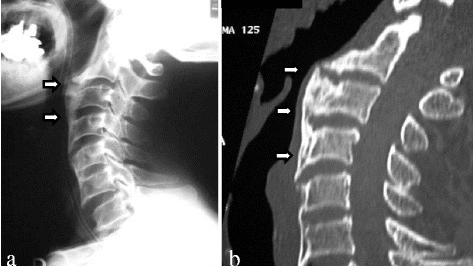
a) Recurrent ossification of anterior longitudinal ligament with anterior osteophytes arrows was present from C2 to C6 b) computed tomographic images of the cervical spine
-
X-ray showing osteophytes of spondylosis of the lumbar spine
Treatments
Normally, asymptomatic cases are not treated. Non-steroidal anti inflammatory drugs and surgery are two typical options for cases requiring treatment.
References
- ↑ "osteophyte" at Dorland's Medical Dictionary
- ↑ Rogers J, Shepstone L, Dieppe P (Feb 1997). "Bone formers: osteophyte and enthesophyte formation are positively associated". Annals of the Rheumatic Diseases. 56 (2): 85–90. doi:10.1136/ard.56.2.85. PMC 1752321. PMID 9068279.
- ↑ "The Medico-chirurgical Review and Journal of Medical Science". Burgess and Hill. 1 January 1844. Archived from the original on 27 February 2023. Retrieved 10 September 2022.
- ↑ Alonge TO, Rooney P, Oni OO (2005). "The ultrastructure of the peri-articular osteophytes - an evaluation by scanning electron microscopy". West Afr J Med. 24 (2): 147–50. doi:10.4314/wajm.v24i2.28186. PMID 16092317. Archived from the original on 2023-02-27. Retrieved 2022-09-10.
- ↑ Wong, Siu Him Janus; Chiu, Kwong Yuen; Yan, Chun Hoi (December 2016). "Review Article: Osteophytes". Journal of Orthopaedic Surgery (Hong Kong). 24 (3): 403–410. doi:10.1177/1602400327. ISSN 2309-4990. Archived from the original on 2 January 2022. Retrieved 27 February 2023.
- ↑ Nathan M, Pope MH, Grobler LJ (Aug 1994). "Osteophyte formation in the vertebral column: a review of the etiologic factors--Part II". Contemporary Orthopaedics. 29 (2): 113–9. PMID 10150240.
- ↑ 7.0 7.1 Bone spurs Archived 2008-10-28 at the Wayback Machine MayoClinic.com
- ↑ Cite error: Invalid
<ref>tag; no text was provided for refs namedref1
External links
| Classification |
|---|
- Mayo Clinic website Archived 2008-10-28 at the Wayback Machine concise information on bone spurs