Prepatellar bursitis
| Prepatellar bursitis | |
|---|---|
| Other names: Carpet layer's knee, coal miner's knee, housemaid's knee,[1] carpenters knee,[2] beat knee,[3] rug cutter's knee,[4] nun's knee[5] | |
 | |
| Aseptic prepatellar bursitis of the knee near the camera | |
| Specialty | Orthopedics, sports medicine |
| Symptoms | Swelling, redness, and tenderness in front of knee[2] |
| Complications | Infection[2] |
| Causes | Repetitive minor trauma, acute injury, gout, rheumatoid arthritis, infection[2] |
| Risk factors | Professions that require frequent kneeling, poor immune function[1][2] |
| Diagnostic method | Based on symptoms and examination, potentially aspiration to rule out infection[2] |
| Differential diagnosis | Patellar tendonitis, patellar subluxation, tibial apophysitis, septic arthritis, cellulitis,[2] Morel-Lavallée lesion[6] |
| Treatment | Rest, NSAIDS, applying ice[2] |
| Prognosis | Generally good[2] |
| Frequency | Relatively common[1] |
Prepatellar bursitis is inflammation of the prepatellar bursa at the front of the knee.[2] Symptoms generally include swelling, redness, tenderness, and possibly minor decrease in range of motion.[2][4] Cases of longer duration generally have little pain.[2]
It most commonly due to repetitive minor trauma to the knee, such as from kneeling.[1] Other causes may include a single injury, gout, rheumatoid arthritis, or infection.[2] Risk factors include professions that require frequent kneeling and poor immune function.[1][2] Diagnosis is usually based on symptoms and examination, with potentially aspiration to rule out infection.[2]
Treatment may include rest, NSAIDS, and applying ice.[2] If infected 7 days of antibiotics are generally sufficient.[7] Steroid injection maybe used for long term cases.[2] In cases that fail other measures, bursectomy may be carried out.[2] Outcomes are generally good.[2]
Prepatellar bursitis is relatively common, estimated to affect about 1 in 10,000 people a year; second in frequency only to olecranon bursitis.[1][2] It occurs more commonly in males than females.[2] Those between the ages of 40 and 60 are most commonly affected.[2] It has historically been called housemaids, carpet layers, or carpenters knee.[2]
Signs and symptoms
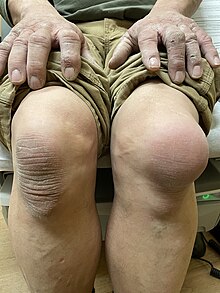
The primary symptom of prepatellar bursitis is swelling of the area around the kneecap. It generally does not produce a significant amount of pain unless pressure is applied directly.[8] The area may be red (erythema), warm to the touch, or surrounded by cellulitis, particularly if infection is present, often accompanied by fever.[9]: p. 608 Unlike arthritis, except in severe cases prepatellar bursitis generally does not affect the range of motion of the knee, though it may cause some discomfort in complete flexion of the joint.[10]: p. 360 Flexion and extension of the knee may be accompanied by crepitus, the audible grating of bones, ligaments, or particles within the excess synovial fluid.[11]: p. 20
Causes
In human anatomy, a bursa is a small pouch filled with synovial fluid. Its purpose is to reduce friction between adjacent structures. The prepatellar bursa is one of several bursae of the knee joint, and is located between the patella and the skin.[12] Prepatellar bursitis is an inflammation of this bursa. Bursae are readily inflamed when irritated, as their walls are very thin.[11]: p. 22 Along with the pes anserine bursa, the prepatellar bursa is one of the most common bursae to cause knee pain when inflamed.[13]
Prepatellar bursitis is caused by either a single instance of acute trauma to the knee, or repeated minor trauma to the knee. The trauma can cause extravasation of nearby fluids into the bursa, which stimulates an inflammatory response.[14] This response occurs in two phases: The vascular phase, in which the blood flow to the surrounding area increases, and the cellular phase, in which leukocytes migrate from the blood to the affected area.[11]: p. 22 Other possible causes include gout, sarcoidosis, CREST syndrome,[10]: p. 359 diabetes mellitus, alcohol use disorder, uremia, and chronic obstructive pulmonary disease.[11]: p. 22 Some cases are idiopathic, though these may be caused by trauma that the patient does not remember.[9]: pp. 607–8
The prepatellar bursa and the olecranon bursa are the two bursae that are most likely to become infected, or septic.[15] Septic bursitis typically occurs when the trauma to the knee causes an abrasion, though it is also possible for the infection to be caused by bacteria traveling through the blood from a pre-existing infection site.[16] In approximately 80% of septic cases, the infection is caused by Staphylococcus aureus; other common infections are Streptococcus, Mycobacterium, and Brucella.[10]: p. 359 It is highly unusual for septic bursitis to be caused by anaerobes, fungi, or Gram-negative bacteria.[9]: p. 608 In very rare cases, the infection can be caused by tuberculosis.[17]
Diagnosis

There are several types of inflammation that can cause knee pain, including sprains, bursitis, and injuries to the meniscus.[13] A diagnosis of prepatellar bursitis can be made based on a physical examination and the presence of risk factors in the person's medical history; swelling and tenderness at the front of the knee, combined with a profession that requires frequent kneeling, suggest prepatellar bursitis.[14] Swelling of multiple joints along with restricted range of motion may indicate arthritis instead.[9]: p. 608
A physical examination and medical history are generally not enough to distinguish between infectious and non-infectious bursitis; aspiration of the bursal fluid is often required for this, along with a cell culture and Gram stain of the aspirated fluid.[10]: p. 360 Septic prepatellar bursitis may be diagnosed if the fluid is found to have a neutrophil count above 1500 per microliter,[9]: p. 608 a threshold significantly lower than that of septic arthritis (50,000 cells per microliter).[10]: p. 360 A tuberculosis infection can be confirmed using a radiograph of the knee and urinalysis.[17]
Prevention
It is possible to prevent the onset of prepatellar bursitis, or prevent the symptoms from worsening, by avoiding trauma to the knee or frequent kneeling.[9]: p. 610 Protective knee pads can also help prevent prepatellar bursitis for those whose professions require frequent kneeling and for athletes who play contact sports, such as American football, basketball, and wrestling.[18]
Treatment
Non-septic prepatellar bursitis can be treated with rest, the application of ice to the affected area, and anti-inflammatory drugs, particularly ibuprofen. Elevation of the affected leg during rest may also expedite the recovery process.[18] Severe cases may require fine-needle aspiration of the bursa fluid, sometimes coupled with cortisone injections.[16] However, some studies have shown that steroid injections may not be an effective treatment option.[19] After the bursitis has been treated, rehabilitative exercise may help improve joint mechanics and reduce chronic pain.[20]: p. 2320
Opinions vary as to which treatment options are most effective for septic prepatellar bursitis.[10]: p. 360 McAfee and Smith recommend a course of oral antibiotics, usually oxacillin sodium or cephradine, and assert that surgery and drainage are unnecessary.[9]: p. 609 Wilson-MacDonald argues that oral antibiotics are "inadequate", and recommends intravenous antibiotics for managing the infection.[3] Some authors suggest surgical irrigation of the bursa by means of a subcutaneous tube.[10]: p. 360 [21] Others suggest that bursectomy may be necessary for intractable cases; the operation is an outpatient procedure that can be performed in less than half an hour.[22]: p. 357
Epidemiology
The various nicknames associated with prepatellar bursitis arise from the fact that it commonly occurs among those individuals whose professions require frequent kneeling, such as carpenters, carpet layers, gardeners, housemaids, mechanics, miners, plumbers, and roofers.[14][8][9]: p. 607 The exact incidence of the condition is not known; it is difficult to estimate because only severe septic cases require hospital admission, and mild non-septic cases generally go unreported.[9]: p. 607 Prepatellar bursitis is more common among males than females. It affects all age groups, but is more likely to be septic when it occurs in children.[23]
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Khodaee, M (15 February 2017). "Common Superficial Bursitis". American family physician. 95 (4): 224–231. PMID 28290630.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 2.17 2.18 2.19 2.20 2.21 2.22 Rishor-Olney, CR; Pozun, A (January 2022). "Prepatellar Bursitis". StatPearls. PMID 32491440.
- ↑ 3.0 3.1 Wilson-Macdonald, James (1987). "Management and outcome of infective prepatellar bursitis". Postgrad Med J. 63 (744): 851–853. doi:10.1136/pgmj.63.744.851. PMC 2428634. PMID 3447109.
- ↑ 4.0 4.1 Roberts, James R.; Hedges, Jerris R. (28 May 2013). Roberts and Hedges’ Clinical Procedures in Emergency Medicine E-Book. Elsevier Health Sciences. p. 1068. ISBN 978-1-4557-4859-4. Archived from the original on 18 January 2023. Retrieved 18 January 2023.
- ↑ "2012 ICD-9-CM Diagnosis Code 727.2 : Specific bursitides often of occupational origin". Archived from the original on 2016-10-29. Retrieved 2023-01-14.
- ↑ Greenhill, D; Haydel, C; Rehman, S (January 2016). "Management of the Morel-Lavallée Lesion". The Orthopedic clinics of North America. 47 (1): 115–25. doi:10.1016/j.ocl.2015.08.012. PMID 26614926.
- ↑ Brown, OS; Smith, TO; Parsons, T; Benjamin, M; Hing, CB (October 2022). "Management of septic and aseptic prepatellar bursitis: a systematic review". Archives of orthopaedic and trauma surgery. 142 (10): 2445–2457. doi:10.1007/s00402-021-03853-9. PMID 33721054.
- ↑ 8.0 8.1 Biundo, Joseph J (2008). "Prepatellar Bursitis". In Klippel, John H (ed.). Primer on the Rheumatic Diseases. Springer. p. 80. ISBN 9780387356648.
- ↑ 9.0 9.1 9.2 9.3 9.4 9.5 9.6 9.7 9.8 McAfee, JH; Smith, DL (November 1988). "Olecranon and prepatellar bursitis—Diagnosis and treatment". West J Med. 149 (5): 607–610. PMC 1026560. PMID 3074561.
- ↑ 10.0 10.1 10.2 10.3 10.4 10.5 10.6 Aaron, DL; et al. (June 2011). "Four common types of bursitis: diagnosis and management". J Am Acad Orthop Surg. 19 (6): 359–361. doi:10.5435/00124635-201106000-00006. PMID 21628647. Archived from the original on 2020-12-24. Retrieved 2023-01-14.
- ↑ 11.0 11.1 11.2 11.3 Price, N (June 2008). "Prepatellar bursitis". Emergency Nurse. 16 (3): 20–24. doi:10.7748/en2008.06.16.3.20.c8183. PMID 18672851.
- ↑ Chatra, Priyank (January–March 2012). "Bursae around the knee joints". Indian Journal of Radiology and Imaging. 22 (1): 27–30. doi:10.4103/0971-3026.95400. PMC 3354353. PMID 22623812.
- ↑ 13.0 13.1 Gonzales, R; Nadler, PL (2010). "Acute Knee Pain". In McPhee, SJ; Papadakis, MA (eds.). Current Medical Diagnosis & Treatment 2010. New York: McGraw-Hill Medical. p. 33. ISSN 0092-8682.
- ↑ 14.0 14.1 14.2 Madsen, James M (22 November 2004). "Prepatellar Bursitis". In Greenberg, Michael I (ed.). Greenberg's Text-Atlas of Emergency Medicine. Lippincott Williams & Wilkins. p. 922. ISBN 9780781745864.
- ↑ Hellmann, DB; Imboden, JB (2010). "Bursitis". In McPhee, SJ; Papadakis, MA (eds.). Current Medical Diagnosis & Treatment 2010. New York: McGraw-Hill Medical. p. 743. ISSN 0092-8682.
- ↑ 16.0 16.1 Shiel, William C. "Bursitis of the Knee". MedicineNet. Archived from the original on 19 November 2020. Retrieved 9 May 2012.
- ↑ 17.0 17.1 Schickendantz, MS; Watson, JT (September 1990). "Mycobacterial prepatellar bursitis". Clin Orthop Relat Res. 258 (258): 209–212. PMID 2203571.
- ↑ 18.0 18.1 "Prepatellar (Kneecap) Bursitis". American Academy of Orthopaedic Surgeons. July 2007. Archived from the original on 28 October 2017. Retrieved 10 May 2012.
- ↑ Mysnyk, MC; et al. (January 1986). "Prepatellar bursitis in wrestlers". Am J Sports Med. 14 (1): 46–54. doi:10.1177/036354658601400109. PMID 3752346.
- ↑ Butcher JD, et al. (15 May 1996). "Lower extremity bursitis". Am Fam Physician. 53 (7): 2317–24. PMID 8638508.
- ↑ Hennrikus, WL; et al. (September 1989). "Treating septic prepatellar bursitis". West J Med. 151 (3): 331–332. PMC 1026890. PMID 2627225.
- ↑ Huang, Y; Yeh, W (March 2011). "Endoscopic treatment of prepatellar bursitis". Int Orthop. 35 (3): 355–358. doi:10.1007/s00264-010-1033-5. PMC 3047636. PMID 20521045.
- ↑ Allen, Kelly L (18 January 2012). "Prepatellar Bursitis". WebMD. Archived from the original on 11 May 2012. Retrieved 21 May 2012.
External links
| Classification |
|---|