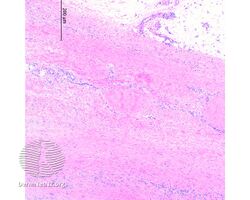
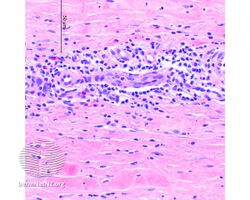
Eosinophilic fasciitis
| Eosinophilic fasciitis | |
|---|---|
| Other names: Shulman syndrome[1] | |
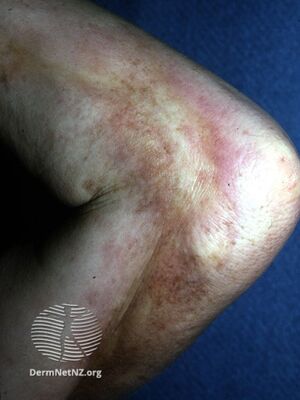 | |
| Eosinophilic fasciitis | |
Eosinophilic fasciitis (/ˌiːəˌsɪnəˈfɪlɪk ˌfæʃiˈaɪtɪs, ˌiːoʊ-, -ˌfæsi-/[2][3]), also known as Shulman's syndrome,[4] is an inflammatory disease that affects the fascia, other connective tissues, surrounding muscles, blood vessels and nerves. Unlike other forms of fasciitis, eosinophilic fasciitis is typically self-limited and confined to the arms and legs, although it can require treatment with corticosteroids, and some cases are associated with aplastic anemia.[5]
The condition was first characterized in 1974,[6] but it is not yet known whether it is actually a distinct condition or merely a variant presentation of another syndrome. The presentation is similar to that of scleroderma or systemic sclerosis. However, unlike scleroderma, eosinophilic fasciitis affects the deeper fascial layers, rather than the dermis; the characteristic and severe effects of scleroderma and systemic sclerosis, such as Raynaud's syndrome, involvement of the extremities, prominent small blood vessels (telangiectasias), and visceral changes such as swallowing problems, are absent. Nevertheless, the term remains used for diagnostic purposes.[citation needed]
Signs and symptoms
Because the disease is rare and clinical presentations vary, a clear set of symptoms is difficult to define. Severe pain and swelling are often reported, and skin can resemble orange peel in appearance.[7]
Less common features include joint pain and carpal tunnel syndrome.[citation needed]
Cause
Most cases are idiopathic, but strenuous exercise,[6] initiation of hemodialysis,[8] infection with Borrelia burgdorferi,[9] and certain medications, such as statins, phenytoin, ramipril, and subcutaneous heparin,[10] may trigger the condition.[11]
Diagnosis
The key to diagnosis is the observation of skin changes in combination with eosinophilia, but the most accurate test is a biopsy of skin, fascia, and muscle.[citation needed]
Treatment
Common treatments include corticosteroids[12] such as prednisone, although medications such as hydroxychloroquine[13] have also been used. Early initiation of treatment usually portends a good prognosis if there is no visceral involvement.[7][14]
Epidemiology
Typical age of onset is around forty to fifty years, although cases in children have been observed. It remains unclear whether the condition is more common in women or men; patient numbers are small, and studies conflict in their reports of preponderance.[15]
Additional images
-
Eosinophilic fasciitis/pathology
-
Eosinophilic fasciitis/pathology
-
Eosinophilic fasciitis/pathology
See also
References
- ↑ "Eosinophilic fasciitis: MedlinePlus Medical Encyclopedia". medlineplus.gov. Archived from the original on 29 October 2019. Retrieved 29 October 2019.
- ↑ "Eosinophilic". Oxford Dictionaries UK Dictionary. Oxford University Press. Retrieved 2016-01-21. "fasciitis". Oxford Dictionaries UK Dictionary. Oxford University Press. Retrieved 2016-01-21.
- ↑ "Eosinophilic". Merriam-Webster Dictionary. Retrieved 2016-01-21. "fasciitis". Merriam-Webster Dictionary. Retrieved 2016-01-21.
- ↑ Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. ISBN 978-1-4160-2999-1.[page needed]
- ↑ "Merck Manual, Professional Edition, Eosinophilic Fasciitis". Archived from the original on 2015-03-20. Retrieved 2021-04-27.
- ↑ 6.0 6.1 Shulman, L. E (1975). "Diffuse fasciitis with eosinophilia: A new syndrome?". Transactions of the Association of American Physicians. 88: 70–86. PMID 1224441.
- ↑ 7.0 7.1 Bischoff, Lindsay; Chris T. Derk (January 2008). "Eosinophilic fasciitis: demographics, disease pattern and response to treatment: report of 12 cases and review of the literature". International Journal of Dermatology. 47 (1): 29–35. doi:10.1111/j.1365-4632.2007.03544.x. PMID 18173597. S2CID 25791443. Archived from the original on 2017-09-22. Retrieved 2021-04-27.
- ↑ Florell, Scott R; Egan, Conleth A; Gregory, Martin C; Zone, John J; Petersen, Marta J (2016). "Eosinophilic Fasciitis Occurring Four Weeks after the Onset of Dialysis in a Renal Failure Patient". Journal of Cutaneous Medicine and Surgery. 5 (1): 33–6. doi:10.1177/120347540100500108. PMID 11281432. S2CID 208066832.
- ↑ Mosconi, Sandro; Streit, Markus; Brönimann, Marcel; Braathen, Lasse R (2002). "Eosinophilic Fasciitis (Shulman Syndrome)". Dermatology. 205 (2): 204–6. doi:10.1159/000063916. PMID 12218249. S2CID 37435478.
- ↑ Long, Hai; Zhang, Guiying; Wang, Ling; Lu, Qianjin (2015). "Eosinophilic Skin Diseases: A Comprehensive Review". Clinical Reviews in Allergy & Immunology. 50 (2): 189–213. doi:10.1007/s12016-015-8485-8. PMID 25876839. S2CID 30806009.
- ↑ Pinal-Fernandez, I; Selva-O'Callaghan, A; Grau, J.M (2014). "Diagnosis and classification of eosinophilic fasciitis". Autoimmunity Reviews. 13 (4–5): 379–82. doi:10.1016/j.autrev.2014.01.019. PMID 24424187.
- ↑ Antic M, Lautenschlager S, Itin PH (2006). "Eosinophilic fasciitis 30 years after - what do we really know? Report of 11 patients and review of the literature". Dermatology. 213 (2): 93–101. doi:10.1159/000093847. PMID 16902285. S2CID 29769383.
- ↑ Lakhanpal S, Ginsburg WW, Michet CJ, Doyle JA, Moore SB (1988). "Eosinophilic fasciitis: clinical spectrum and therapeutic response in 52 cases". Semin. Arthritis Rheum. 17 (4): 221–31. doi:10.1016/0049-0172(88)90008-X. PMID 3232080.
- ↑ Valadares, Diana; Joao Neves; Isabel Almeida; Carlos Lopes; Carlos Vasconcelos (February 2011). "Iron Lady: A Case of Eosinophilic Fasciitis". Journal of Medical Case Reports. 2: 34–36. doi:10.4021/jmc118w.
- ↑ Wojas-Pelc, Anna; Wielowieyska-Szybińska, Dorota; Lipko-Godlewska, Sylwia (2004). "Eozynofilowe zapalenie powięzi - aktualny stan wiedzy" [Eosinophilic fasciitis--current database]. Polski Merkuriusz Lekarski (in polski). 16 (96): 585–8. PMID 15510903.
Further reading
- Lakhanpal, Sharad; Ginsburg, William W.; Michet, Clement J.; Doyle, John A.; Moore, S.Breanndan (1988). "Eosinophilic fasciitis: Clinical spectrum and therapeutic response in 52 cases". Seminars in Arthritis and Rheumatism. 17 (4): 221–231. doi:10.1016/0049-0172(88)90008-X. ISSN 0049-0172. PMID 3232080.
- Barnes L, Rodnan GP, Medsger TA, Short D (August 1979). "Eosinophilic fasciitis. A pathologic study of twenty cases". The American Journal of Pathology. 96 (2): 493–518. PMC 2042453. PMID 474708.
- Doyle JA, Ginsburg WW (September 1989). "Eosinophilic fasciitis". The Medical Clinics of North America. 73 (5): 1157–66. doi:10.1016/S0025-7125(16)30625-3. PMID 2671538.
- Michet CJ, Doyle JA, Ginsburg WW (January 1981). "Eosinophilic fasciitis: report of 15 cases". Mayo Clinic Proceedings. 56 (1): 27–34. PMID 7453247.
- Bennett, R M; Herron, A; Keogh, L (1977). "Eosinophilic fasciitis. Case report and review of the literature". Annals of the Rheumatic Diseases. 36 (4): 354–359. doi:10.1136/ard.36.4.354. ISSN 0003-4967. PMC 1006697. PMID 901033.
- Falanga, Vincent; Medsger, Thomas A. (1987). "Frequency, levels, and significance of blood eosinophilia in systemic sclerosis, localized scleroderma, and eosinophilic fasciitis". Journal of the American Academy of Dermatology. 17 (4): 648–656. doi:10.1016/S0190-9622(87)70251-5. ISSN 0190-9622. PMID 3668010.
- Varga J, Kähäri VM (November 1997). "Eosinophilia-myalgia syndrome, eosinophilic fasciitis, and related fibrosing disorders". Current Opinion in Rheumatology. 9 (6): 562–70. doi:10.1097/00002281-199711000-00013. PMID 9375286.
- Kent, Lawrence T.; Cramer, Stewart F.; Moskowitz, Roland W. (1981). "Eosinophilic fasciitis". Arthritis & Rheumatism. 24 (5): 677–683. doi:10.1002/art.1780240508. ISSN 0004-3591. PMID 6972219.
- Moulton SJ, Kransdorf MJ, Ginsburg WW, Abril A, Persellin S (March 2005). "Eosinophilic fasciitis: spectrum of MRI findings". AJR. American Journal of Roentgenology. 184 (3): 975–8. doi:10.2214/ajr.184.3.01840975. PMID 15728627.
External links
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- Wikipedia articles needing page number citations from January 2018
- Articles with invalid date parameter in template
- CS1 polski-language sources (pl)
- All articles with unsourced statements
- Articles with unsourced statements from April 2021
- Articles with unsourced statements from March 2021
- Articles with unsourced statements from August 2020
- Disorders of fascia
- Eosinophilic cutaneous conditions
- Inflammations
- Steroid-responsive inflammatory conditions
- Systemic connective tissue disorders
- Autoimmune diseases
- Immune system disorders