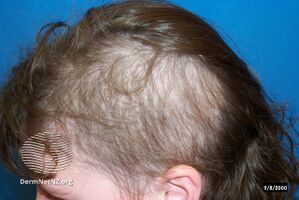
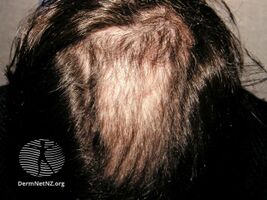
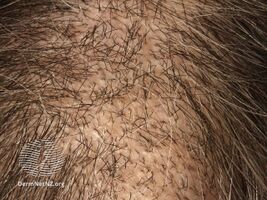
Trichotillomania
| Trichotillomania | |
|---|---|
| Other names: Trichotillosis, hair pulling disorder,[1] compulsive hair pulling | |
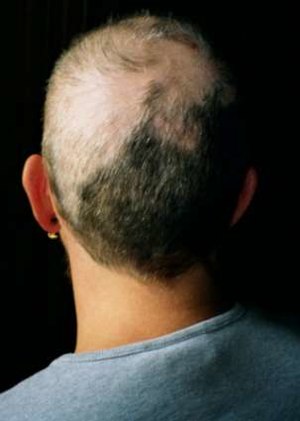 | |
| A pattern of incomplete hair loss on the scalp of a person with trichotillomania | |
| Pronunciation | |
| Specialty | Dermatology, psychiatry |
| Symptoms | Visible hair loss, distress[1][2] |
| Usual onset | Childhood or adolescence[2] |
| Risk factors | Family history, anxiety, obsessive compulsive disorder[1] |
| Diagnostic method | Based on symptoms, seeing broken hairs[1] |
| Differential diagnosis | Body dysmorphic disorder[1] |
| Medication | Cognitive behavioral therapy, clomipramine[3] |
| Frequency | ~2%[2][3] |
Trichotillomania (TTM), also known as hair pulling disorder or compulsive hair pulling, is a mental disorder characterized by a long-term urge that results in the pulling out of one's hair.[2][4] This occurs to such a degree that hair loss can be seen.[2] A brief positive feeling may occur as hair is removed.[5] Efforts to stop pulling hair typically fail.[1] Hair removal may occur anywhere; however, the head and around the eyes are most common.[1] The hair pulling is to such a degree that it results in distress.[1]
The disorder may run in families.[1] It occurs more commonly in those with obsessive compulsive disorder.[1] Episodes of pulling may be triggered by anxiety.[1] People usually acknowledge that they pull their hair.[1] On examination broken hairs may be seen.[1] Other conditions that may present similarly include body dysmorphic disorder, however in that condition people remove hair to try to improve what they see as a problem in how they look.[1]
Treatment is typically with cognitive behavioral therapy.[3] The medication clomipramine may also be helpful.[3] Trichotillomania is estimated to affect one to four percent of people.[2][3] Trichotillomania most commonly begins in childhood or adolescence.[2] Women are affected about 10 times more often than men.[1] The name was created by François Henri Hallopeau in 1889, from the Greek θριξ/τριχ; thrix (meaning "hair"), along with τίλλειν; tíllein (meaning "to pull"), and μανία; mania (meaning "madness").[6]
Signs and symptoms
Trichotillomania is usually confined to one or two sites,[7] but can involve multiple sites. The scalp is the most common pulling site, followed by the eyebrows, eyelashes, face, arms, and legs.[8] Some less common areas include the pubic area, underarms, beard, and chest.[9] The classic presentation is the "Friar Tuck" form of vertex and crown alopecia.[10] Children are less likely to pull from areas other than the scalp.[8]
People who suffer from trichotillomania often pull only one hair at a time and these hair-pulling episodes can last for hours at a time. Trichotillomania can go into remission-like states where the individual may not experience the urge to "pull" for days, weeks, months, and even years.[11]
Individuals with trichotillomania exhibit hair of differing lengths; some are broken hairs with blunt ends, some new growth with tapered ends, some broken mid-shaft, or some uneven stubble. Scaling on the scalp is not present, overall hair density is normal, and a hair pull test is negative (the hair does not pull out easily). Hair is often pulled out leaving an unusual shape. Individuals with trichotillomania may be secretive or shameful of the hair pulling behavior.[8]
An additional psychological effect can be low self-esteem, often associated with being shunned by peers and the fear of socializing, due to appearance and negative attention they may receive.[12] Some people with trichotillomania wear hats, wigs, false eyelashes, eyebrow pencil, or style their hair in an effort to avoid such attention.[3] There seems to be a strong stress-related component. In low-stress environments, some exhibit no symptoms (known as "pulling") whatsoever. This "pulling" often resumes upon leaving this environment.[13] Some individuals with trichotillomania may feel they are the only person with this problem due to low rates of reporting.[14]
For some people, trichotillomania is a mild problem, merely a frustration. But for many, shame and embarrassment about hair pulling causes painful isolation and results in a great deal of emotional distress, placing them at risk for a co-occurring psychiatric disorder, such as a mood or anxiety disorder. Hair pulling can lead to great tension and strained relationships with family members and friends. Family members may need professional help in coping with this problem.[15]
Other medical complications include infection, permanent loss of hair, repetitive stress injury, carpal tunnel syndrome, and gastrointestinal obstruction as a result of trichophagia.[7] In trichophagia, people with trichotillomania also ingest the hair that they pull; in extreme (and rare) cases this can lead to a hair ball (trichobezoar).[8] Rapunzel syndrome, an extreme form of trichobezoar in which the "tail" of the hair ball extends into the intestines, can be fatal if misdiagnosed.[8][16][17][18]
Environment is a large factor which affects hair pulling.[19] Sedentary activities such as being in a relaxed environment are conducive to hair pulling.[19][20] A common example of a sedentary activity promoting hair pulling is lying in a bed while trying to rest or fall asleep.[19] An extreme example of automatic trichotillomania is found when some patients have been observed to pull their hair out while asleep.[19] This is called sleep-isolated trichotillomania.[21]
-
Trichotillomania
-
Trichotillomania
-
Trichotillomania
Causes
Anxiety, depression and obsessive–compulsive disorder are more frequently encountered in people with trichotillomania.[7][22] Trichotillomania has a high overlap with post traumatic stress disorder, and some cases of trichotillomania may be triggered by stress. Another school of thought emphasizes hair pulling as addictive or negatively reinforcing, as it is associated with rising tension beforehand and relief afterward.[7] A neurocognitive model — the notion that the basal ganglia plays a role in habit formation and that the frontal lobes are critical for normally suppressing or inhibiting such habits — sees trichotillomania as a habit disorder.[7]
Abnormalities in the caudate nucleus are noted in OCD, but there is no evidence to support that these abnormalities can also be linked to trichotillomania.[7] One study has shown that individuals with trichotillomania have decreased cerebellar volume.[7][23] These findings suggest some differences between OCD and trichotillomania.[7] There is a lack of structural MRI studies on trichotillomania.[7] In several MRI studies that have been conducted, it has been found that people with trichotillomania have more gray matter in their brains than those who do not suffer from the disorder.[24]
It is likely that multiple genes confer vulnerability to trichotillomania.[7] One study identified mutations in the SLITRK1 gene.[7][25]
Diagnosis
Patients may be ashamed or actively attempt to disguise their symptoms. This can make diagnosis difficult as symptoms are not always immediately obvious, or have been deliberately hidden to avoid disclosure.[7] If the patient admits to hair pulling, diagnosis is not difficult; if patients deny hair pulling, a differential diagnosis must be pursued.[8] The differential diagnosis will include evaluation for alopecia areata, iron deficiency, hypothyroidism, tinea capitis, traction alopecia, alopecia mucinosa, thallium poisoning, and loose anagen syndrome.[3][8] In trichotillomania, a hair pull test is negative.[8]
A biopsy can be performed and may be helpful; it reveals traumatized hair follicles with perifollicular hemorrhage, fragmented hair in the dermis, empty follicles, and deformed hair shafts. Multiple catagen hairs are typically seen. An alternative technique to biopsy, particularly for children, is to shave a part of the involved area and observe for regrowth of normal hairs.[26]
Classification
Trichotillomania is defined as a self-induced and recurrent loss of hair.[8] It includes the criterion of an increasing sense of tension before pulling the hair and gratification or relief when pulling the hair.[7] However, some people with trichotillomania do not endorse the inclusion of "rising tension and subsequent pleasure, gratification, or relief" as part of the criteria[7] because many individuals with trichotillomania may not realize they are pulling their hair, and patients presenting for diagnosis may deny the criteria for tension prior to hair pulling or a sense of gratification after hair is pulled.[8]
Trichotillomania may lie on the obsessive-compulsive spectrum,[3] also encompassing obsessive-compulsive disorder (OCD), body dysmorphic disorder (BDD), nail biting (onychophagia) and skin picking (dermatillomania), tic disorders and eating disorders. These conditions may share clinical features, genetic contributions, and possibly treatment response; however, differences between trichotillomania and OCD are present in symptoms, neural function and cognitive profile.[7] In the sense that it is associated with irresistible urges to perform unwanted repetitive behavior, trichotillomania is akin to some of these conditions, and rates of trichotillomania among relatives of OCD patients is higher than expected by chance.[7] However, differences between the disorder and OCD have been noted, including: differing peak ages at onset, rates of comorbidity, gender differences, and neural dysfunction and cognitive profile.[7] When it occurs in early childhood, it can be regarded as a distinct clinical entity.[7]
Because trichotillomania can be present in multiple age groups, it is helpful in terms of prognosis and treatment to approach three distinct subgroups by age: preschool age children, preadolescents to young adults, and adults.[8]
In preschool age children, trichotillomania is considered benign. For these children, hair-pulling is considered either a means of exploration or something done subconsciously, similar to nail-biting and thumb-sucking, and almost never continues into further ages.[27]
The most common age of onset of trichotillomania is between ages 9 and 13. In this age range, trichotillomania is usually chronic, and continues into adulthood. Trichiotillomania that begins in adulthood most commonly arises from underlying psychiatric causes.[27]
Trichotillomania is often not a focused act, but rather hair pulling occurs in a "trance-like" state;[19] hence, trichotillomania is subdivided into "automatic" versus "focused" hair pulling.[8] Children are more often in the automatic, or unconscious, subtype and may not consciously remember pulling their hair. Other individuals may have focused, or conscious, rituals associated with hair pulling, including seeking specific types of hairs to pull, pulling until the hair feels "just right", or pulling in response to a specific sensation.[8] Knowledge of the subtype is helpful in determining treatment strategies.[8]
Treatment
Treatment is based on a person's age. Most pre-school age children outgrow the condition if it is managed conservatively. In young adults, establishing the diagnosis and raising awareness of the condition is an important reassurance for the family and patient. Non-pharmacological interventions, including behavior modification programs, may be considered; referrals to psychologists or psychiatrists may be considered when other interventions fail. When trichotillomania begins in adulthood, it is often associated with other mental disorders, and referral to a psychologist or psychiatrist for evaluation or treatment is considered best. The hair pulling may resolve when other conditions are treated.[8]
Psychotherapy
Habit reversal training (HRT) has the highest rate of success in treating trichotillomania.[8] HRT has also been shown to be a successful adjunct to medication as a way to treat trichotillomania.[7][28] With HRT, the individual is trained to learn to recognize their impulse to pull and also teach them to redirect this impulse. In comparisons of behavioral versus pharmacologic treatment, cognitive behavioral therapy (including HRT) have shown significant improvement over medication alone.[7][8] It has also proven effective in treating children.[8] Biofeedback, cognitive-behavioral methods, and hypnosis may improve symptoms.[29] Acceptance and Commitment Therapy (ACT) is also demonstrating promise in trichotillomania treatment.[30] A systematic review from 2012 found tentative evidence for "movement decoupling".[31]
Medication
The United States Food and Drug Administration (FDA) has not approved any medications for trichotillomania treatment.[32]
Medications can be used to treat trichotillomania. Treatment with clomipramine, a tricyclic antidepressant, was shown in a small double-blind study to improve symptoms,[33] but results of other studies on clomipramine for treating trichotillomania have been inconsistent.[8] Naltrexone may be a viable treatment.[34] Fluoxetine and other selective serotonin reuptake inhibitors (SSRIs) have limited usefulness in treating trichotillomania, and can often have significant side effects.[35] Behavioral therapy has proven more effective when compared to fluoxetine.[8] There is little research on the effectiveness of behavioral therapy combined with medication,[36] and robust evidence from high-quality studies is lacking.[7] Acetylcysteine treatment stemmed from an understanding of glutamate's role in regulation of impulse control.[37]
Different medications, depending on the individual, may increase hair pulling.[32]
Devices
Technology can be used to augment habit reversal training or behavioral therapy. Several mobile apps exist to help log behavior and focus on treatment strategies.[38] There are also wearable devices that track the position of a user's hands. They produce sound or vibrating notifications so that users can track rates of these events over time.[39]
Prognosis
When it occurs in early childhood (before five years of age), the condition is typically self-limiting and intervention is not required.[7] In adults, the onset of trichotillomania may be secondary to underlying psychiatric disturbances, and symptoms are generally more long-term.[8]
Secondary infections may occur due to picking and scratching, but other complications are rare.[8] Individuals with trichotillomania often find that support groups are helpful in living with and overcoming the disorder.[8]
Epidemiology
Although no broad-based population epidemiologic studies had been conducted as of 2009, the lifetime prevalence of trichotillomania is estimated to be between 0.6% and 4.0% of the overall population.[3] With a 1% prevalence rate, 2.5 million people in the U.S. may have trichotillomania at some time during their lifetimes.[40]
Trichotillomania is diagnosed in all age groups; onset is more common during preadolescence and young adulthood, with mean age of onset between 9 and 13 years of age,[8] and a notable peak at 12–13.[7] Among preschool children the genders are equally represented; there appears to be a female predominance among preadolescents to young adults, with between 70% and 93% of patients being female.[8] Among adults, females typically outnumber males by 3 to 1.[7]
"Automatic" pulling occurs in approximately three-quarters of adult patients with trichotillomania.[8]
History
Hair pulling was first mentioned by Aristotle in the fourth century B.C.,[41] was first described in modern literature in 1885,[42] and the term trichotillomania was coined by the French dermatologist François Henri Hallopeau in 1889.[3][7]
In 1987, trichotillomania was recognized in the Diagnostic and Statistical Manual of the American Psychiatric Association, third edition-revised (DSM-III-R).[43]
Society and culture
Support groups and internet sites can provide recommended educational material and help persons with trichotillomania in maintaining a positive attitude and overcoming the fear of being alone with the disorder.[7][8]
Media
A documentary film exploring trichotillomania, Bad Hair Life, was the 2003 winner of the International Health & Medical Media Award for best film in psychiatry and the winner of the 2004 Superfest Film Festival Merit Award.[44][45][46]
Trichster is a 2016 documentary that follows seven individuals living with trichotillomania, as they navigate the complicated emotions surrounding the disorder, and the effect it has on their daily lives.[47]
See also
- Noncicatricial alopecia
- Psychogenic alopecia, a form of baldness that is caused by excessive grooming in cats
- Feather-plucking
- Self-harm
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 American Psychiatric Association (2013), Diagnostic and Statistical Manual of Mental Disorders (5th ed.), Arlington: American Psychiatric Publishing, pp. 217–221, 938, ISBN 978-0890425558
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 Franklin, Martin E; Zagrabbe, Kathryn; Benavides, Kristin L (9 January 2014). "Trichotillomania and its treatment: a review and recommendations". Expert Review of Neurotherapeutics. 11 (8): 1165–1174. doi:10.1586/ern.11.93. PMC 3190970. PMID 21797657.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 3.8 3.9 Huynh M, Gavino AC, Magid M (June 2013). "Trichotillomania". Semin Cutan Med Surg. 32 (2): 88–94. doi:10.12788/j.sder.0007. PMID 24049966.
- ↑ Pittenger, Christopher (2017). Obsessive-compulsive Disorder: Phenomenology, Pathophysiology, and Treatment. Oxford University Press. p. 541. ISBN 9780190228163. Archived from the original on 2021-08-29. Retrieved 2019-08-20.
- ↑ Woods, Douglas; Miltenberger, Raymond (2007). Tic Disorders, Trichotillomania, and Other Repetitive Behavior Disorders: Behavioral Approaches to Analysis and Treatment. Springer Science & Business Media. p. 134. ISBN 9780387459448. Archived from the original on 2021-08-29. Retrieved 2019-08-20.
- ↑ Aboujaoude, Elias (2008). Compulsive Acts: A Psychiatrist's Tales of Ritual and Obsession. University of California Press. p. 42. ISBN 9780520255678.
- ↑ 7.00 7.01 7.02 7.03 7.04 7.05 7.06 7.07 7.08 7.09 7.10 7.11 7.12 7.13 7.14 7.15 7.16 7.17 7.18 7.19 7.20 7.21 7.22 7.23 7.24 7.25 Chamberlain SR, Menzies L, Sahakian BJ, Fineberg NA (April 2007). "Lifting the veil on trichotillomania". Am J Psychiatry. 164 (4): 568–74. doi:10.1176/appi.ajp.164.4.568. PMID 17403968.
- ↑ 8.00 8.01 8.02 8.03 8.04 8.05 8.06 8.07 8.08 8.09 8.10 8.11 8.12 8.13 8.14 8.15 8.16 8.17 8.18 8.19 8.20 8.21 8.22 8.23 8.24 8.25 8.26 Sah, Deborah E; Koo, John; Price, Vera H (January 2008). "Trichotillomania". Dermatologic Therapy. 21 (1): 13–21. doi:10.1111/j.1529-8019.2008.00165.x. PMID 18318881.
- ↑ What is Trichotillomania "What is Trichotillomania (Hair Pulling Disorder)?". Archived from the original on 2016-07-02. Retrieved 2016-07-12.. 2016
- ↑ James, William; Berger, Timothy; Elston, Dirk (2005). Andrews' Diseases of the Skin: Clinical Dermatology (10th ed.). Saunders. p. 62. ISBN 978-0-7216-2921-6.
- ↑ "Trichotillomania: 12 Facts You Should Know About Trich". Pullfreeatlast.com. Archived from the original on 2013-02-28. Retrieved 2013-02-22.
- ↑ Chamberlain, Samuel. "Trichotillomania". National Organization for Rare Disorders. National Organization for Rare Disorders. Archived from the original on 3 June 2019. Retrieved 12 June 2019.
- ↑ Christenson GA, Mackenzie TB, Mitchell JE (1991). "Characteristics of 60 adult chronic hair pullers". The American Journal of Psychiatry. 148 (3): 365–70. doi:10.1176/ajp.148.3.365. PMID 1992841. Archived from the original on 2021-08-29. Retrieved 2019-12-30.
- ↑ Christenson GA, MacKenzie TB, Mitchell JE (1994). "Adult men and women with trichotillomania. A comparison of male and female characteristics". Psychosomatics. 35 (2): 142–9. doi:10.1016/S0033-3182(94)71788-6. PMID 8171173.
- ↑ "What is Trichotillomania" "What is Trichotillomania (Hair Pulling Disorder)?". Archived from the original on 2016-07-02. Retrieved 2016-07-12.. 2016
- ↑ Ventura DE, Herbella FA, Schettini ST, Delmonte C (2005). "Rapunzel syndrome with a fatal outcome in a neglected child". J. Pediatr. Surg. 40 (10): 1665–7. doi:10.1016/j.jpedsurg.2005.06.038. PMID 16227005.
- ↑ Pul N, Pul M (1996). "The Rapunzel syndrome (trichobezoar) causing gastric perforation in a child: a case report". Eur. J. Pediatr. 155 (1): 18–9. doi:10.1007/bf02115620. PMID 8750804.
- ↑ Matejů E, Duchanová S, Kovac P, Moravanský N, Spitz DJ (September 2009). "Fatal case of Rapunzel syndrome in neglected child". Forensic Sci. Int. 190 (1–3): e5–7. doi:10.1016/j.forsciint.2009.05.008. PMID 19505779.
- ↑ 19.0 19.1 19.2 19.3 19.4 Tay, Y.-K.; Levy, M. L.; Metry, D. W. (30 April 2004). "Trichotillomania in Childhood: Case Series and Review". Pediatrics. 113 (5): e494–e498. doi:10.1542/peds.113.5.e494. PMID 15121993.
- ↑ Diefenbach GJ, Mouton-Odum S, Stanley MA (November 2002). "Affective correlates of trichotillomania". Behav Res Ther. 40 (11): 1305–15. doi:10.1016/S0005-7967(02)00006-2. PMID 12384325.
- ↑ "What is Trichotillomania?". Archived from the original on July 13, 2010. Retrieved August 20, 2010.
- ↑ Christenson GA, Crow SJ (1996). "The characterization and treatment of trichotillomania". The Journal of Clinical Psychiatry. 57 Suppl 8: 42–7, discussion 48–9. PMID 8698680.
- ↑ Keuthen NJ, Makris N, Schlerf JE, et al. (2007). "Evidence for reduced cerebellar volumes in trichotillomania". Biol. Psychiatry. 61 (3): 374–81. doi:10.1016/j.biopsych.2006.06.013. PMID 16945351.
- ↑ Chamberlain, Samuel R.; Menzies, Lara A.; Fineberg, Naomi A.; Del Campo, Natalia; Suckling, John; Craig, Kevin; Müller, Ulrich; Robbins, Trevor W.; Bullmore, Edward T.; Sahakian, Barbara J. (2008). "Grey matter abnormalities in trichotillomania: morphometric magnetic resonance imaging study". British Journal of Psychiatry. 193 (3): 216–221. doi:10.1192/bjp.bp.107.048314. PMC 2806575. PMID 18757980.
- ↑ Zuchner S, Cuccaro ML, Tran-Viet KN, et al. (October 2006). "SLITRK1 mutations in trichotillomania". Mol. Psychiatry. 11 (10): 887–9. doi:10.1038/sj.mp.4001865. PMID 17003809. Lay summary.
{{cite journal}}: Cite uses deprecated parameter|lay-url=(help); Unknown parameter|laydate=ignored (help); Unknown parameter|laysource=ignored (help) - ↑ James, William; Berger, Timothy; Elston, Dirk (2005). Andrews' Diseases of the Skin: Clinical Dermatology (10th ed.). Saunders. p. 63. ISBN 978-0-7216-2921-6.
- ↑ 27.0 27.1 Khan Mohammad Beigi, Pooya (2018). "Trichotillomania (Hair Pulling Disorder)". Alopecia Areata. pp. 63–66. doi:10.1007/978-3-319-72134-7_10. ISBN 978-3-319-72133-0.
- ↑ Woods DW, Wetterneck CT, Flessner CA (2006). "A controlled evaluation of acceptance and commitment therapy plus habit reversal for trichotillomania". Behaviour Research and Therapy. 44 (5): 639–56. doi:10.1016/j.brat.2005.05.006. PMID 16039603.
- ↑ Shenefelt PD (2003). "Biofeedback, cognitive-behavioral methods, and hypnosis in dermatology: is it all in your mind?". Dermatol Ther. 16 (2): 114–22. doi:10.1046/j.1529-8019.2003.01620.x. PMID 12919113.
- ↑ Ruiz, F. J. (2010). "A review of Acceptance and Commitment Therapy (ACT) empirical evidence: Correlational, experimental psychopathology, component and outcome studies". International Journal of Psychology and Psychological Therapy. 10 (1): 125–62. Archived from the original on 2012-02-23.
- ↑ Sarris, Jerome; Camfield, David; Berk, Michael (May 2012). "Complementary medicine, self-help, and lifestyle interventions for Obsessive Compulsive Disorder (OCD) and the OCD spectrum: A systematic review". Journal of Affective Disorders. 138 (3): 213–221. doi:10.1016/j.jad.2011.04.051. PMID 21620478.
- ↑ 32.0 32.1 "Trichotillomania Treatment Options". Trichstop.com. Archived from the original on 2 March 2015. Retrieved 21 March 2015.
- ↑ Swedo SE, Leonard HL, Rapoport JL, Lenane MC, Goldberger EL, Cheslow DL (1989). "A double-blind comparison of clomipramine and desipramine in the treatment of trichotillomania (hair pulling)". N. Engl. J. Med. 321 (8): 497–501. doi:10.1056/NEJM198908243210803. PMID 2761586.
- ↑ A.D.A.M. Medical Encyclopedia. Trichotillomania Trichotillosis; Compulsive hair pulling. Last reviewed: February 13, 2012. Archived July 31, 2013, at the Wayback Machine
- ↑ Christenson GA, Mackenzie TB, Mitchell JE, Callies AL (November 1991). "A placebo-controlled, double-blind crossover study of fluoxetine in trichotillomania". Am J Psychiatry. 148 (11): 1566–71. doi:10.1176/ajp.148.11.1566. PMID 1928474.
- ↑ Rothbart, Rachel; Amos, Taryn; Siegfried, Nandi; Ipser, Jonathan C; Fineberg, Naomi; Chamberlain, Samuel R; Stein, Dan J (8 November 2013). "Pharmacotherapy for trichotillomania". Cochrane Database of Systematic Reviews (11): CD007662. doi:10.1002/14651858.CD007662.pub2. PMID 24214100.
- ↑ Grant, Jon E.; Odlaug, Brian L.; Won Kim, Suck (1 July 2009). "N-Acetylcysteine, a Glutamate Modulator, in the Treatment of Trichotillomania". Archives of General Psychiatry. 66 (7): 756–63. doi:10.1001/archgenpsychiatry.2009.60. PMID 19581567.
- ↑ "Mental Health Apps Resources for Psychologists, MFTs, Counselors, LPCs and Social Workers". www.zurinstitute.com. Archived from the original on 2016-05-10. Retrieved 2016-05-17.
- ↑ Lerman, Rachel (October 30, 2016). "Brothers' bracelet helps treat hair-pulling condition". Seattle Times. Archived from the original on 21 April 2017. Retrieved 23 March 2019.
- ↑ Diefenbach GJ, Reitman D, Williamson DA (April 2000). "Trichotillomania: a challenge to research and practice". Clin Psychol Rev. 20 (3): 289–309. doi:10.1016/S0272-7358(98)00083-X. PMID 10779896.
- ↑ Nicomachean Ethics Archived 2015-10-09 at the Wayback Machine, 1148b25-30, where Aristotle uses the term: "τριχῶν τίλσεις Archived 2016-03-16 at the Wayback Machine."
- ↑ Salaam, Karriem; Carr, Joel; Grewal, Harsh; Sholevar, Ellen; Baron, David (July 2005). "Untreated Trichotillomania and Trichophagia: Surgical Emergency in a Teenage Girl". Psychosomatics. 46 (4): 362–366. doi:10.1176/appi.psy.46.4.362. PMID 16000680.
- ↑ Bouwer, Colin; Stein, Dan J. (1998). "Trichobezoars in Trichotillomania". Psychosomatic Medicine. 60 (5): 658–660. doi:10.1097/00006842-199809000-00025. PMID 9773774.
- ↑ "Bad Hair Life: A Documentary". Trichotillomania Learning Center. Archived from the original on October 26, 2009. Retrieved November 27, 2009.
- ↑ "Superfest XXIV Winners". CDT Inc. Archived from the original on May 25, 2010. Retrieved November 27, 2009.
- ↑ "Hannah Sussman's Art Imitates Life Join Her For a Screening October 3rd". Century City News. September 28, 2009. Archived from the original on December 16, 2009. Retrieved November 27, 2009.
- ↑ Koning, Patricia (2012-07-27). "Documentary Film Project to Portray Living with Trichotillomania - The Independent: Community". Independentnews.com. Archived from the original on 2017-09-08. Retrieved 2014-04-10.
External links
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- CS1: long volume value
- CS1 errors: unsupported parameter
- CS1 errors: deprecated parameters
- Webarchive template wayback links
- Articles with Curlie links
- Body-focused repetitive behavior
- Conditions of the skin appendages
- Habit and impulse disorders
- Hair diseases
- Hair removal
- Human hair
- Mania
- Neurocutaneous conditions
- Psychiatric diagnosis
- Self-harm
- RTT
- RTTNEURO