Port-wine stain
| Port-wine stain | |
|---|---|
| Other names: Nevus flammeus, firemark | |
 | |
| The back of a hand with prominent port-wine staining | |
| Specialty | Dermatology |
| Symptoms | Dark red or purple area of skin with defined borders[1] |
| Complications | Glaucoma[2] |
| Usual onset | Present at birth[3] |
| Duration | Long-term |
| Causes | Genetic mutation in early development[2] |
| Risk factors | None known[4] |
| Diagnostic method | Based on appearance[4] |
| Differential diagnosis | Naevus simplex (salmon patch)[5] |
| Treatment | Laser therapy[1][6] |
| Prognosis | Generally harmless, though may darken and thicken over time[4][2] |
| Frequency | 3 in a 1,000 newborns[5] |
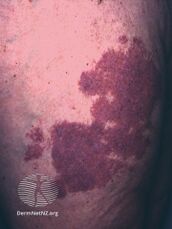
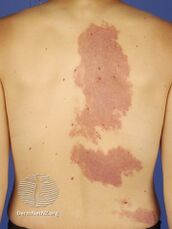
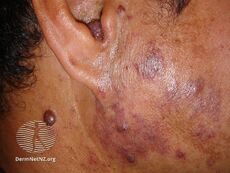
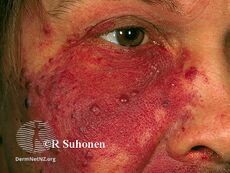
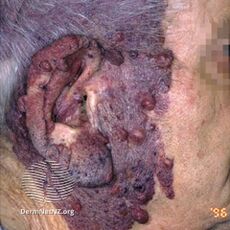
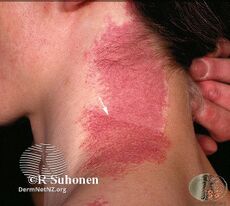
Port-wine stain, also known as nevus flammeus, is a birth mark that presents as a dark red or purple area of skin.[1][3] They occur most often on one side of the face or neck;[1][3] though, any part of the body may be involved.[2] They generally have defined borders and over time may become darker and thicken.[2] Complications may include glaucoma.[2]
They occur due to a genetic mutation in early development, and are not generally inherited from a person's parents.[2] They may occur as part of conditions such as Sturge–Weber syndrome or Klippel–Trénaunay–Weber syndrome.[1] The underlying mechanism involves the formation of a capillary malformation.[2] Diagnosis is generally based on its appearance; though, in unclear cases this may be supported by a skin biopsy.[4]
They may be improved with laser therapy.[1][6] This is most effective if performed early in life.[7] They result in concerns primarily due to their effect on appearances.[8] They generally persist throughout life; with the area of affected skin growing proportionally to general growth.[2][9]
Port-wine stain affect about 3 in a 1,000 newborns.[5] They may negatively affect a person's confidence or have negative financial effects.[5][9] They are so named for their color, which is similar to port wine, a type of fortified red wine.[10] They were associated with supernatural causes in the medieval ages.[11] Notable cases include that of Mikhail Gorbachev in the 1990s.[12]
Signs and symptoms
They generally presents as a dark red or purple area of skin at birth.[1][3] They occur most often on one side of the face or neck;[1][3] though, any part of the body may be involved.[2] They generally have defined borders and over time may become darker and thicken.[2] Complications may include glaucoma.[2]
-
Port-wine stain
-
Port-wine stain
-
Port-wine stain
-
Port-wine stain
-
Port-wine stain
-
Port-wine stain
-
Port-wine stain
-
Mikhail Gorbachev, last leader of the Soviet Union, with a prominent port-wine stain on his forehead
Genetics
Port-wine stains were shown to be caused by a somatic activating c.548G→A mutation in the GNAQ gene.[13] An association with RASA1 has also been described.[14]
Diagnosis
Diagnosis is typically based upon the history and appearance. In unusual cases, a skin biopsy may be needed to confirm the diagnosis. Depending on the location of the birthmark and other associated symptoms, a physician may choose to order a measurement of intraocular pressure or X-ray of the skull.
An MRI of the brain may be performed (under anesthesia) on infants who have a port-wine stain in the head area in order to check for signs of Sturge-Weber syndrome.[2]
If the port-wine stain is inside the mouth, a provider may check the insides of a newborn baby's throat with a scope to see if there are any changes (growths) other than just the color.
If the port-wine stain is around the eye or on the eyelid, a referral may be made to an optometrist or ophthalmologist for a test of the ocular pressures in that eye. If swelling occurs in the port-wine stain, it may cause vision problems, glaucoma, or blindness.
Treatment
Many treatments have been tried for port-wine stains including freezing, surgery, radiation, and tattooing; port-wine stains can also be covered with cosmetics.
Lasers may be able to destroy the capillaries without significant damage to the overlying skin. Lasers and other light sources may therefore be able to reduce the redness of port-wine stains, although there is not enough evidence to recommend one form over another.
For most people in trials of pulsed dye laser, more than 25% of the redness was reduced by laser after one to three treatments. Adverse effects were rare in these trials, although some people had changes to the color of the skin, especially Chinese people with darker skin. There can be pain, crusting, and blistering in the two weeks after treatment. The trials only followed people for six months, so long-term outcomes are not known.[6] Up to 10 treatments may be necessary for improvement, but complete removal may not result.[15] The use of topical rapamycin as an adjunct to pulsed dye laser may improve results.[16]
Treatment is generally given before one year of age.[17] However, as it is recommended to be performed under anesthesia (15 minutes) on small children, it is not always possible to get frequent treatments. For example in Finland a child gets treated 2-3 times per year, resulting in a target of "being ready before school age" (7 years).[citation needed]
After the laser treatment the skin is filled with black marks, the size of a pen. This is due to the laser instrument's size; the black marks disappear within 1–3 weeks. The treated area can be sore and swollen for a couple of days.
Prognosis
In the absence of successful treatment, hypertrophy (increased tissue mass) of the stains may cause problems later in life, such as loss of function (especially if the stain is near the eye or mouth), bleeding, and increasing disfigurement. Lesions on or near the eyelid can be associated with glaucoma.[2] If the port-wine stain is on the face or other highly visible part of the body, its presence can also cause emotional and social problems for the affected person.
Epidemiology
They occur in about 3–5 cases per 1,000 newborn babies.[18][19][20]
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 "Birthmarks". nhs.uk. 20 October 2017. Archived from the original on 19 May 2021. Retrieved 2 October 2023.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 Primary Care Dermatology Society, UK. "Port-wine stain". Clinical Guidance. Primary Care Dermatology Society, UK. Archived from the original on 25 August 2018. Retrieved 8 July 2013.
- ↑ 3.0 3.1 3.2 3.3 3.4 McLaughlin, MR; O'Connor, NR; Ham, P (1 January 2008). "Newborn skin: Part II. Birthmarks". American family physician. 77 (1): 56–60. PMID 18236823.
- ↑ 4.0 4.1 4.2 4.3 "Department of Surgery". froemkelab.med.nyu.edu. Archived from the original on 20 October 2023. Retrieved 2 October 2023.
- ↑ 5.0 5.1 5.2 5.3 "Capillary vascular malformation (red birthmarks, port wine stain) | DermNet". dermnetnz.org. Archived from the original on 1 June 2023. Retrieved 29 September 2023.
- ↑ 6.0 6.1 6.2 Faurschou, A.; Olesen, AB; Leonardi-Bee, J.; Haedersdal, M. (9 November 2011). "Lasers or light sources for treating port-wine stains". Cochrane Database of Systematic Reviews (11): CD007152. doi:10.1002/14651858.CD007152.pub2. PMID 22071834. Archived from the original on 24 December 2013. Retrieved 26 May 2021.
- ↑ Minkis, K.; Geronemus, R. G.; Hale, E. K. (2009). "Port wine stain progression: A potential consequence of delayed and inadequate treatment?". Lasers in Surgery and Medicine. 41 (6): 423–6. doi:10.1002/lsm.20788. PMC 4690461. PMID 19588535.
- ↑ Ryan, E; Warren, L (May 2012). "Birthmarks--identification and management". Australian Family Physician. 41 (5): 274–277. PMID 22558616. Archived from the original on 2023-03-20. Retrieved 2023-10-02.
- ↑ 9.0 9.1 "Kids Health Information : Port wine stains". www.rch.org.au. Archived from the original on 11 May 2023. Retrieved 2 October 2023.
- ↑ Blumer, Steven L.; Biko, David M.; Halabi, Safwan (26 October 2017). Pediatric Imaging: A Core Review. Lippincott Williams & Wilkins. p. PT736. ISBN 978-1-4963-4017-7. Archived from the original on 20 October 2023. Retrieved 2 October 2023.
- ↑ Barrau, Julie; Bates, David (7 October 2021). Lives, Identities and Histories in the Central Middle Ages. Cambridge University Press. p. 102. ISBN 978-1-107-16080-4. Archived from the original on 20 October 2023. Retrieved 2 October 2023.
- ↑ Mangione, Salvatore (21 April 2012). Physical Diagnosis Secrets: With STUDENT CONSULT Online Access. Elsevier Health Sciences. p. 167. ISBN 978-0-323-11211-6. Archived from the original on 20 October 2023. Retrieved 2 October 2023.
- ↑ Shirley, Matthew D.; Tang, Hao; Gallione, Carol J.; Baugher, Joseph D.; Frelin, Laurence P.; Cohen, Bernard; North, Paula E.; Marchuk, Douglas A.; Comi, Anne M.; Pevsner, Jonathan (8 May 2013). "Sturge–Weber Syndrome and Port-Wine Stains Caused by Somatic Mutation in". New England Journal of Medicine. 368 (21): 1971–9. doi:10.1056/NEJMoa1213507. PMC 3749068. PMID 23656586.
- ↑ Eerola I, Boon LM, Mulliken JB, et al. (December 2003). "Capillary malformation-arteriovenous malformation, a new clinical and genetic disorder caused by RASA1 mutations". Am. J. Hum. Genet. 73 (6): 1240–9. doi:10.1086/379793. PMC 1180390. PMID 14639529.
- ↑ Patel, AM; Chou, EL; Findeiss, L; Kelly, KM (Jun 2012). "The horizon for treating cutaneous vascular lesions". Seminars in Cutaneous Medicine and Surgery. 31 (2): 98–104. doi:10.1016/j.sder.2012.02.001. PMC 3570568. PMID 22640429.
- ↑ Marques L, Nunez-Cordoba JM, Aguado L, et al. Topical rapamycin combined with pulsed dye laser in the treatment of capillary vascular malformations in Sturge-Weber syndrome: phase II, randomized double-blind, intraindividual placebo controlled trial. JAAD 2015.
- ↑ McLaughlin, MR; O'Connor, NR; Ham, P. (1 January 2008). "Newborn skin: Part II. Birthmarks". American Family Physician. 77 (1): 56–60. PMID 18236823.
- ↑ Jacobs, A. H.; Walton, R. G. (1976). "The incidence of birthmarks in the neonate". Pediatrics. 58 (2): 218–22. PMID 951136.
- ↑ Alper, J. C.; Holmes, L. B. (1983). "The incidence and significance of birthmarks in a cohort of 4,641 newborns". Pediatric Dermatology. 1 (1): 58–68. doi:10.1111/j.1525-1470.1983.tb01093.x. PMID 6679890.
- ↑ Dr Thajudheen MD (Dr Thaj laser skin hair clinic), Kannangath Jyothy, Arul Priyadarshini, "Treatment of port-wine stains with flash lamp pumped pulsed dye laser on Indian skin: A six year study" Archived 2018-06-02 at the Wayback Machine, Dr. Thaj Laser Skin-Hair Clinic, 2 April 2014
External links
| Classification | |
|---|---|
| External resources |