Ichthyosis vulgaris
| Ichthyosis vulgaris | |
|---|---|
 | |
| Ichthyosis vulgaris | |
| Specialty | Dermatology |
| Symptoms | Very dry, scaly skin; lower legs, trunk[1] |
| Usual onset | Baby[1] |
| Causes | [2] |
| Diagnostic method | Appearance[1] |
| Treatment | Moisturisers[1] |
| Frequency | Common, 1 in 250 people[2] |
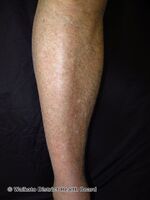
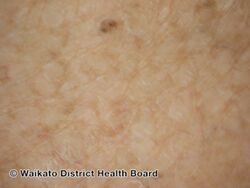
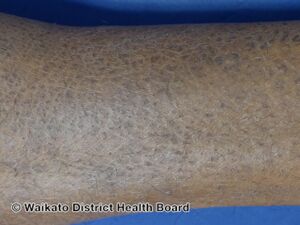
Ichthyosis vulgaris, also known as common ichthyosis and autosomal dominant ichthyosis, is a skin disorder presenting with very dry, scaly skin that may appear like fish scales.[1] It is typically noted in a baby at around 2-to-3 months of age.[1] The lower legs tend to be more severely affected than the trunk, and underarms and other folds are generally spared.[1]
The condition is an autosomal dominant inherited disease.[1] The cause is a defect in filaggerin gene which results in disruption of the barrier function of the skin.[2] Atopic dermatitis may exist simultaneously.[2]
Diagnosis is by its appearance.[1] Treatment is with thick moisturisers.[1][3] Creams containing 5%-10% urea may be effective. Other options include the application of topical keratolytics and retinoids, although used with caution in young children due to their absorption through skin.[1]
It is the most common form of ichthyosis, affecting around 1 in 250 people.[2]
Signs and symptoms
The symptoms of the inherited form of ichthyosis vulgaris are not usually present at birth but generally develop between 3 months and 5 years of age.[4][5] The symptoms will often improve with age, although they may grow more severe again in old age.[6]
The condition is not life-threatening; the impact on the patient, if it is a mild case, is generally restricted to mild itching and the social impact of having skin with an unusual appearance. People with mild cases have symptoms that include scaly patches on the shins, fine white scales on the forearms and upper arms, and rough palms. People with the mildest cases have no symptoms other than faint, tell-tale "mosaic lines" between the Achilles tendons and the calf muscles.
Severe cases, although rare, do exist. Severe cases entail the buildup of scales everywhere, with areas of the body that have a concentration of sweat glands being least affected. Areas where the skin rubs against each other, such as the armpits, the groin, and the "folded" areas of the elbow and knees, are less affected. When the buildup of scales is bad, the person with a severe case has "prickly itch" when he or she needs to sweat but cannot because of the scales. Various topical treatments are available to "exfoliate" the scales. These include lotions that contain alpha-hydroxy acids.
-
Ichthyosis vulgaris
-
Ichthyosis vulgaris
-
Mild presentation of ichthyosis vulgaris: faint, mosaic lines are visible on the calf.
Associated conditions
Many people with severe ichthyosis have problems sweating due to the buildup of scales on the skin. This may lead to problems such as "prickly itch" or problems associated with overheating. The majority of people with vulgaris can sweat at least a little. Paradoxically this means most would be more comfortable living in a hot and humid climate. Sweating helps to shed scales which improves the appearance of the skin and prevents "prickly itch".[citation needed]
The dry skin will crack on digits or extremities and create bloody cuts. Skin is painful when inflamed and/or tight. For children and adolescents: psychological precautions may include inconsistent self-image, mood fluctuates due to cyclical outbreaks, prone to addiction, may socially withdraw and/or separate when skin is noticeably infected, pre-occupation with appearance.[citation needed]
Strong air-conditioning and excessive consumption of alcohol can also increase the buildup of scales.
Over 50% of people with ichthyosis vulgaris have some type of atopic disease such as allergies, eczema, or asthma.[7] Another common condition associated with ichthyosis vulgaris is keratosis pilaris (small bumps mainly appearing on the back of the upper arms).[5]
Genetics
It is usually an autosomal dominant inherited disease (often associated with filaggrin), although a rare non-heritable version called acquired ichthyosis exists.[1]
Ichthyosis vulgaris is one of the most common genetic disorders caused by a single gene.[4] The disorder is believed to be caused by mutations to the gene encoding profilaggrin (a protein which is converted to filaggrin which plays a vital role in the structure of the skin).[8] Around 10% of the population have some detrimental mutations to the profilaggrin gene that is also linked to atopic dermatitis (another skin disorder that is often present with ichthyosis vulgaris).[5] The exact mutation is only known for some cases of ichthyosis vulgaris.[4]
It is generally considered to be an autosomal dominant condition, i.e., a single genetic mutation causes the disease and an affected person has a 50% chance of passing the condition on to their child. There is some research indicating it may be semi-dominant. This means that a single mutation would cause a mild case of ichthyosis vulgaris and mutations to both copies of the gene would produce a more severe case.[8]
See also
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 James, William D.; Elston, Dirk; Treat, James R.; Rosenbach, Misha A.; Neuhaus, Isaac (2020). "27. Genodermatoses and congenital anomalies". Andrews' Diseases of the Skin: Clinical Dermatology (13th ed.). Edinburgh: Elsevier. p. 563. ISBN 978-0-323-54753-6. Archived from the original on 2023-08-05. Retrieved 2023-08-04.
- ↑ 2.0 2.1 2.2 2.3 2.4 Morris-Jones, Rachel (2019). "10. The skin and systemic disease". In Morris-Jones, Rachael (ed.). ABC of Dermatology (7th ed.). Hoboken: Wiley Blackwell. p. 85. ISBN 978-1-119-48899-6. Archived from the original on 2023-08-05. Retrieved 2023-08-04.
- ↑ "Ichthyosis vulgaris | DermNet". dermnetnz.org. Archived from the original on 7 June 2023. Retrieved 3 August 2023.
- ↑ 4.0 4.1 4.2 Ichthyosis vulgaris Archived 2010-03-07 at the Wayback Machine, OMIM (Online Mendelian Inheritance in Man), Johns Hopkins University
- ↑ 5.0 5.1 5.2 Ichthyosis vulgaris Archived 2008-12-06 at the Wayback Machine, eMedicine.com
- ↑ "Ichthyosis vulgaris" Archived 2016-07-05 at the Wayback Machine, MedlinePlus Medical Encyclopedia.
- ↑ Ichthyosis vulgaris Archived 2009-02-26 at the Wayback Machine, Foundation for Ichthyosis and Related Skin Types (F.I.R.S.T.)
- ↑ 8.0 8.1 Ichthyosis Research (2006) Archived 2009-02-26 at the Wayback Machine, Foundation for Ichthyosis & Related Skin Types (F.I.R.S.T)
External links
- DermAtlas 28
- Photographs from Ichthyosis Information Archived 2021-04-21 at the Wayback Machine
| Classification | |
|---|---|
| External resources |