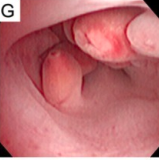
Endometrial polyp
| Endometrial polyp | |
|---|---|
| Other names: Uterine polyp | |
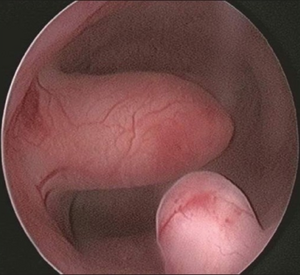 | |
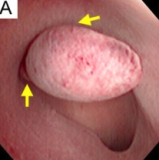
| Endometrial polyp at hysteroscopy | |
| Specialty | Gynaecology |
| Symptoms | None, abnormal vaginal bleeding, infertility[1] |
| Usual onset | Around menopause[1] |
| Causes | Unknown[1] |
| Risk factors | Tamoxifen[1] |
| Diagnostic method | Transvaginal ultrasonography, color doppler, hysteroscopy, histology[2] |
| Differential diagnosis | Uterine fibroid[3] |
| Treatment | Surgery (Polypectomy)[2] |
| Prognosis | 11% to 30% hyperplasia, 0.5% to 3% cancer, some resolve without treatment[1][3] |
| Frequency | Common[4] |
An endometrial polyp, also known as a uterine polyp is a growth attached to the inside of the uterus.[1] There may be no symptoms, or it may result in abnormal vaginal bleeding and difficulty becoming pregnant.[1] They can vary in size from very small to large enough to fill the entire uterine cavity.[2] There may be one or several, and they typically have a stalk which may have a narrow or wide base.[1] If the stalk is long enough, it may protrude into the vagina.[3]
The cause is not known.[1] It is an overgrowth of endocrine glands, also containing stroma and blood vessels and typically situated at the inner top of uterus.[1][3] Most occur in the 40s and 50s, around and after menopause, and particularly if taking the medicine tamoxifen, when the polyps are more likely to be multiple and larger.[1] Diagnosis is by transvaginal ultrasonography, the accuracy of which is improved with color doppler.[2] Confirmation is by microscopic examination of the polyp once cut out during hysteroscopy.[2]
Some resolve without treatment.[3] The majority are noncancerous, however 11% to 30% have or develop hyperplasia, and 0.5% to 3% become cancer.[1] Endometrial polyps are common.[4] Most occur in the 40s and 50s, around menopause.[1]
Signs and symptoms
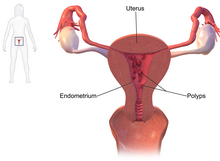
An endometrial polyp is a growth attached to the inside of the uterus.[1]
They often cause no symptoms.[1] Where they occur, symptoms include irregular menstrual bleeding, bleeding between menstrual periods, excessively heavy menstrual bleeding (menorrhagia), and vaginal bleeding after menopause.[5][6] Bleeding from the blood vessels of the polyp contributes to an increase of blood loss during menstruation and blood "spotting" between menstrual periods, or after menopause.[7] If the polyp protrudes through the cervix into the vagina, pain (dysmenorrhea) may result.[8]
Cause
No definitive cause of endometrial polyps is known, but they appear to be affected by hormone levels and grow in response to circulating estrogen.[3] Risk factors include obesity, high blood pressure and a history of cervical polyps.[5] Taking tamoxifen or hormone replacement therapy can also increase the risk of uterine polyps.[5][9] The use of an intrauterine system containing levonorgestrel in women taking tamoxifen may reduce the incidence of polyps.[10] Pedunculated polyps are more common than sessile ones.[11]
Diagnosis
Initial tests
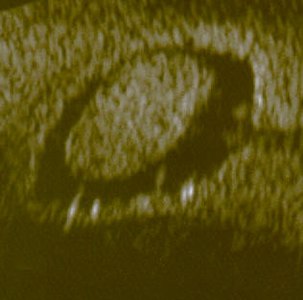
Diagnosis is by transvaginal ultrasonography and accuracy is improved with color doppler.[2]
-
Endometrial polyp, viewed by sonography
Hysteroscopy
Other tests include hysteroscopy.[2]
-
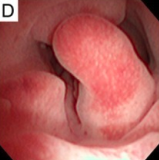
Pedunculated endometrial polyp
-
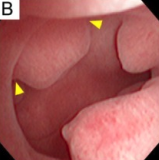
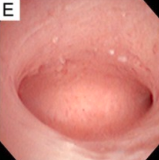
Sessile endometrial polyp
-
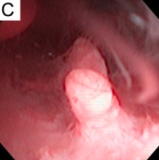
Bleeding and endometrial polyp
-
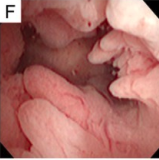
Multiple endometrial polyps
-
Multiple endometrial polyp
Pathology
Endometrial polyps can be solitary or occur with others.[12] They are round or oval and measure between a few millimeters and several centimeters in diameter.[7][12] They are usually the same red/brown color of the surrounding endometrium although large ones can appear to be a darker red.[7] The polyps consist of dense, fibrous tissue (stroma), blood vessels and glandlike spaces lined with endometrial epithelium.[7] If they are pedunculated, they are attached by a thin stalk (pedicle). If they are sessile, they are connected by a flat base to the uterine wall.[12] Pedunculated polyps are more common than sessile ones.[11]
-
Micrograph of an endometrial polyp. H&E stain
-
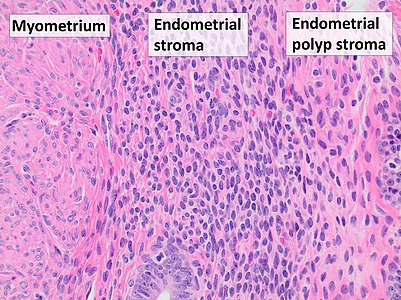
Myometrium (smooth muscle cells) versus endometrial stroma (more cellular) versus endometrial polyp stroma (more collagenous). H&E stain
Treatment
Polyps can be surgically removed using curettage with or without hysteroscopy.[13] When curettage is performed without hysteroscopy, polyps may be missed. To reduce this risk, the uterus can be first explored using grasping forceps at the beginning of the curettage procedure.[7] Hysteroscopy involves visualising the endometrium (inner lining of the uterus) and polyp with a camera inserted through the cervix. Large polyps can be cut into sections before each section is removed.[7] The presence of cancerous cells may suggest a hysterectomy (surgical removal of the uterus).[5] A hysterectomy is usually not considered when cancer is not present.[7] In either procedure, general anesthetic is typically supplied.[14]
The effects of polyp removal on fertility is not clear.[15]
-
No recurrence after removal
-
Recurrence after removal
Prognosis
Some resolve without treatment.[2] The majority are noncancerous, but a few may have hyperplasia or develop hyperplasia and a minority may have or develop carcinoma.[1] Hence, all require histopathological analysis.[2]
Polyps can increase the risk of miscarriage in women undergoing IVF treatment.[5] If they develop near the fallopian tubes, they may lead to difficulty in becoming pregnant.[5] Although treatments such as hysteroscopy usually cure the polyp concerned, recurrence of endometrial polyps is frequent.[7]
Epidemiology
Endometrial polyps are common.[4] Most are harmless; however 11% to 30% have or develop hyperplasia, and 0.5% to 3% turn into a cancer.[1]
See also
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 WHO Classification of Tumours Editorial Board, ed. (2020). "6. Tumours of the uterine corpus: Endometrial polyp". Female genital tumours: WHO Classification of Tumours. Vol. 4 (5th ed.). Lyon (France): International Agency for Research on Cancer. p. 268. ISBN 978-92-832-4504-9. Archived from the original on 2022-06-17. Retrieved 2022-08-01.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 Vitale, Salvatore Giovanni; Haimovich, Sergio; Laganà, Antonio Simone; Alonso, Luis; Di Spiezio Sardo, Attilio; Carugno, Jose (May 2021). "Endometrial polyps. An evidence-based diagnosis and management guide". European Journal of Obstetrics, Gynecology, and Reproductive Biology. 260: 70–77. doi:10.1016/j.ejogrb.2021.03.017. ISSN 1872-7654. PMID 33756339. Archived from the original on 2022-08-02. Retrieved 2022-08-01.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 Nijkang, NP; Anderson, L; Markham, R; Manconi, F (2019). "Endometrial polyps: Pathogenesis, sequelae and treatment". SAGE open medicine. 7: 2050312119848247. doi:10.1177/2050312119848247. PMID 31105939. Archived from the original on 2022-05-24. Retrieved 2022-08-01.
- ↑ 4.0 4.1 4.2 Raz, Nili; Feinmesser, Larissa; Moore, Omer; Haimovich, Sergio (October 2021). "Endometrial polyps: diagnosis and treatment options - a review of literature". Minimally invasive therapy & allied technologies: MITAT: official journal of the Society for Minimally Invasive Therapy. 30 (5): 278–287. doi:10.1080/13645706.2021.1948867. ISSN 1365-2931. PMID 34355659. Archived from the original on 2022-08-02. Retrieved 2022-08-01.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 "Uterine polyps". MayoClinic.com. 2006-04-27. Archived from the original on 2012-07-28. Retrieved 2022-05-02.
- ↑ "Endometrial Polyp". GPnotebook. Archived from the original on 2008-01-07. Retrieved 2007-10-20.
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 7.6 7.7 DeCherney, Alan H.; Lauren Nathan (2003). Current Obstetric & Gynecologic Diagnosis & Treatment. McGraw-Hill Professional. p. 703. ISBN 0-8385-1401-4.
- ↑ Dysmenorrhea: Menstrual abnormalities at Merck Manual of Diagnosis and Therapy Professional Edition
- ↑ Edmonds, D. Keith; Sir John Dewhurst (2006). Dewhurst's Textbook of Obstetrics and Gynaecology. Blackwell Publishing. p. 637. ISBN 1-4051-5667-8. Archived from the original on 2020-06-15. Retrieved 2022-05-02.
- ↑ Chan SS, Tam WH, Yeo W, et al. (2007). "A randomised controlled trial of prophylactic levonorgestrel intrauterine system in tamoxifen-treated women". BJOG. 114 (12): 1510–5. doi:10.1111/j.1471-0528.2007.01545.x. PMID 17995495. S2CID 21145823.
- ↑ 11.0 11.1 Sternberg, Stephen S.; Stacey E. Mills; Darryl Carter (2004). Sternberg's Diagnostic Surgical Pathology. Lippincott Williams & Wilkins. p. 2460. ISBN 0-7817-4051-7. Archived from the original on 2020-06-15. Retrieved 2022-05-02.
- ↑ 12.0 12.1 12.2 Bajo Arenas, José M.; Asim Kurjak (2005). Donald School Textbook Of Transvaginal Sonography. Taylor & Francis. p. 502. ISBN 1-84214-331-X. Archived from the original on 2022-04-07. Retrieved 2022-05-02.
- ↑ "Uterine bleeding – Signs and Symptoms". UCSF Medical Center. 2007-05-08. Archived from the original on 2008-04-11. Retrieved 2007-10-20.
- ↑ Macnair, Trisha. "Ask the doctor – Uterine polyps". BBC Health. Archived from the original on 2007-10-17. Retrieved 2007-10-21.
- ↑ Jayaprakasan, K; Polanski, L; Sahu, B; Thornton, JG; Raine-Fenning, N (Aug 30, 2014). "Surgical intervention versus expectant management for endometrial polyps in subfertile women" (PDF). The Cochrane Database of Systematic Reviews. 8 (8): CD009592. doi:10.1002/14651858.CD009592.pub2. PMC 6544777. PMID 25172985. Archived (PDF) from the original on November 4, 2018. Retrieved May 2, 2022.
External links
| Classification |
|---|