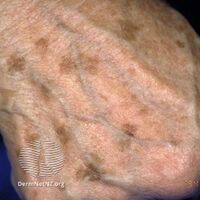
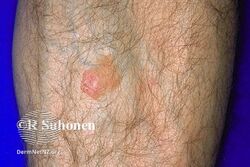
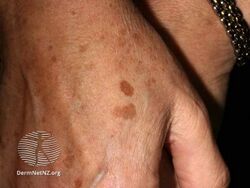
Age spot
| Age spot | |
|---|---|
| Other names: Liver spot, solar lentigo,[1] lentigo senilis,[1]: 686 old age spot,[2] senile freckle[2] | |
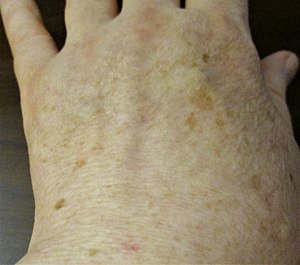 | |
| Age spots on the left hand of a 63-year-old light-skinned man | |
| Specialty | Dermatology |
| Symptoms | Dark spot on skin[3] |
| Usual onset | Older age[4] |
| Duration | Long-term[3] |
| Causes | Sun exposure[3] |
| Diagnostic method | Based on examination[3] |
| Differential diagnosis | Melanoma, freckles, seborrheic keratosis, multiple lentigines syndrome[3][5] |
| Prevention | Sunscreen, avoiding the sun[3] |
| Treatment | Cryotherapy, laser therapy[6] |
| Prognosis | Good[3] |
| Frequency | Very common[3] |
Age spot, also known as solar lentigo, is a dark spot associated with aging.[4] They range in color from light yellow, to brown, to black.[3][7] Their shape may be variable and up to several centimeters across.[3] They usually have a distinct border.[3] They may occur as groups on skin that is frequently exposed to the sun.[3]
The cause is sun exposure.[3][8] The underlying mechanism involves a build up of the pigment melanin.[3] Diagnosis is often based on examination.[3] In unclear cases a biopsy may be done.[3]
The condition is not serious.[3] Treatments involve the use of cryotherapy or laser therapy.[6] Use of 30% trichloroacetic acid on the area may be helpful.[7] Attempts at skin whitening with hydroquinone are not effective.[3] Without treatment, it is a long term condition.[3] Prevention is by using sunscreen or avoiding the sun.[3]
They are very common, particularly after the age of 40.[3] They are most common in Caucasians and Asians.[5] While sometimes referred to as "liver spots", they have no association with liver issues.[6]
Signs and symptoms
They range in color from pink, to light brown, to black.[3] Their shape may be variable and up to several centimeters across.[3] They have a distinct border.[3] They may occur as groups on skin that is frequently exposed to the sun.[3]
-
Solar lentigo
-
Solar lentigo
-
Solar lentigo
Causes

Differently from the melanotic nevi and the verrucous nevi on the skin, age spots change in color and in shape with time. Michelitsch and Michelitsch propose an hypothesis inspired by their misrepair-accumulation aging theory[9][10] for the development of age spots.[11] They propose that aged basal cells contain lipofuscin bodies cannot be removed and might promote the aging of neighboring, generating a feedback loop whereby more and more neighbor cells become aged and lipofuscin-containing.[11] Such cells might then aggregate into a spot with an irregular shape.[11] They propose that the protruding of a flat spot is a result of the death of aged cells in the spot and release of lipofuscin bodies.[11] The aggregating cells would form a capsule, and the dense lipofuscin bodies make the protruding spot soft and dark in color.[11] However, this proposal appeared as a preprint in 2015, has little direct empirical support, and has never been published in a peer reviewed journal.
Another group[12] has reported that "age spots" taken from human skin biopsies of patients facial senile lentigo of Fitzpatrick skin type III or IV aged 55–62 are enriched with senescent fibroblasts compared to surrounding skin. The dark coloration appeared to be due to higher melanin levels and activity of tyrosinase in the senescent fibroblasts than in the controls, potentially related to lower SDF1 expression.[12] Patients were then administered six weekly treatments of microneedle fractional radiofrequency aimed at eliminating dermal senescent fibroblasts; this led to a marked decrease in epidermal pigmentation compared to baseline, accompanied by a decrease in the synthesis of collagen and the normalization of suppressed SDF1 expression.[12]
Treatment
Treatment for liver spots is almost never done for health-related reasons, though it is sometimes done for aesthetic ones. Skin-bleaching products that inhibit pigmentation or cosmetic creams containing the ingredients alpha hydroxy acids or retinoids are known to be effective. Liver spots can also be frozen off with liquid nitrogen; that is, via cryosurgery.[13]
See also
References
- ↑ 1.0 1.1 James, William D.; Berger, Timothy G.; et al. (2006). Andrews' Diseases of the Skin: Clinical Dermatology. Saunders Elsevier. ISBN 0-7216-2921-0.
- ↑ 2.0 2.1 Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. pp. 1716–17. ISBN 1-4160-2999-0.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 3.14 3.15 3.16 3.17 3.18 3.19 3.20 3.21 3.22 3.23 3.24 "Solar lentigo | DermNet NZ". dermnetnz.org. Archived from the original on 16 January 2021. Retrieved 10 June 2021.
- ↑ 4.0 4.1 DE, Elder; D, Massi; RA, Scolyer; R, Willemze (2018). "1. Keratinocytic/epidermal tumours: Benign acanthomas/keratoses - Solar lentigo". WHO Classification of Skin Tumours. Vol. 11 (4th ed.). Lyon (France): World Health Organization. p. 59. ISBN 978-92-832-2440-2. Archived from the original on 2022-07-11. Retrieved 2023-04-29.
- ↑ 5.0 5.1 "Solar Lentigo". fpnotebook.com. Archived from the original on 4 March 2021. Retrieved 10 June 2021.
- ↑ 6.0 6.1 6.2 "Hyperpigmentation - Dermatologic Disorders". Merck Manuals Professional Edition. Archived from the original on 14 April 2021. Retrieved 10 June 2021.
- ↑ 7.0 7.1 Plensdorf, S; Livieratos, M; Dada, N (2017-12-15). "Pigmentation Disorders: Diagnosis and Management". American family physician. 96 (12): 797–804. PMID 29431372.
- ↑ "Ultraviolet (UV) Radiation". www.cancer.org. Archived from the original on 2021-04-30. Retrieved 2020-07-07.
- ↑ Wang, Jicun; Michelitsch, Thomas; Wunderlin, Arne; Mahadeva, Ravi (2009). "Aging as a consequence of Misrepair – a novel theory of aging". 0904: 9. arXiv:0904.0575. Bibcode:2009arXiv0904.0575W.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ Wang-Michelitsch, Jicun; Michelitsch, Thomas (2015). "Aging as a process of accumulation of Misrepairs". 1503: 13. arXiv:1503.07163. Bibcode:2015arXiv150307163W.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ 11.0 11.1 11.2 11.3 11.4 Wang-Michelitsch, Jicun; Michelitsch, Thomas (2015). "Development of age spots as a result of accumulation of aged cells in aged skin". 1505: 9. arXiv:1505.07012. Bibcode:2015arXiv150507012W.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ 12.0 12.1 12.2 Yoon JE, Kim Y, Kwon S, Kim M, Kim YH, Kim JH, Park TJ, Kang HY (September 9, 2018). "Senescent fibroblasts drive ageing pigmentation: A potential therapeutic target for senile lentigo". Theranostics. 8 (17): 4620–4632. doi:10.7150/thno.26975. PMC 6160768. PMID 30279727. Archived from the original on 26 December 2019. Retrieved 26 December 2019.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ↑ Karen J. Carlson, Stephanie A. Eisenstat (2004). The New Harvard Guide to Women's Health. p. 337.
{{cite book}}: CS1 maint: uses authors parameter (link)
External links
| Classification | |
|---|---|
| External resources |