Non-ossifying fibroma
| Non-ossifying fibroma | |
|---|---|
| Other names: Not recommended: fibrous cortical defect, metaphyseal fibrous defect, benign fibrous histiocytoma.[1] Fibroxanthoma, nonosteogenic fibroma, cortical desmoid, fibromatosis[2] | |
 | |
| X-ray of nonossifying fibroma of distal tibia. | |
| Symptoms | Usually none, fracture[1] |
| Usual onset | Childhood[3] |
| Diagnostic method | X-ray, MRI[1] |
| Treatment | Usually none, surgical removal and bone grafting if large[4] |
| Prognosis | Most resolve without treatment[1] |
| Frequency | 30-40% of children, 2M;F[3] |
Non-ossifying fibroma (NOF) is a non-cancerous bone tumor of the osteoclastic giant cell-rich type. It generally occurs in the neck portion of long bones in the legs of children.[1][3] Typically, there are no symptoms unless a bone breaks.[3] It can occur as part of a syndrome such as when multiple fibromas occur in neurofibromatosis, or Jaffe-Campanacci syndrome in combination with cafe-au-lait spots, intellectual disability, hypogonadism, eye and cardiovascular abnormalities.[3][2]
Diagnosis is by X-ray or MRI, usually when investigating a person for something else.[3] Medical imaging typically shows a well marginated radiolucent lesion, with a distinct multilocular appearance, sometimes looking like bubbles.[3] It is usually around 1-2cm in size, but be as large as 7cm.[4] They consist of foci consist of collagen rich connective tissue, fibroblasts, histiocytes and osteoclasts.[3] Usually no treatment is required.[4] Surgical curettage and bone grafting may be required if it is large.[4]
It is found in 30-40% of children and adolescents, but rare in adults as most have resolved by this time.[3] They do not become cancerous.[3] It affects twice as many males as females.[3] A NOF was identified on the mandible of Qafzeh 9, an early anatomically modern human dated to 90–100 000 yrs B.P.[5]
Signs and symptoms
Most people with non-ossifying fibroma have no symptoms.[1] If the tumor is large, there may be pain over the affected area, the bone may break easily, and the affected limb might not function properly.[1] It can occur as part of a syndrome such as when multiple non-ossifying fibromas occur in neurofibromatosis, or Jaffe-Campanacci syndrome in combination with cafe-au-lait spots, mental retardation, hypogonadism, eye and cardiovascular abnormalities.[2][3]
It has been seen to affect the jaw bone, but rarely.[6]
Diagnosis
It is usually iagnosed by x-ray or MRI, when investigating another problem.[1] The tumor presents as a well defined radiolucent lesion, with a distinct multilocular appearance, sometimes looking like a "soap bubble".[2] If small and no symptoms, then biopsy is not needed.[1]
-
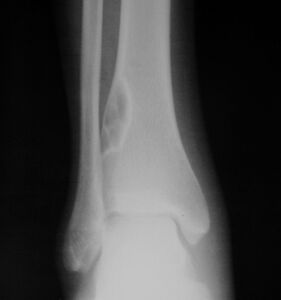
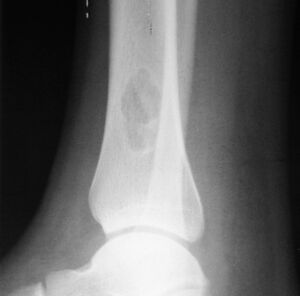
1. a. Front view X-ray: NOF of the lower leg bone near ankle, with well-defined tumor
-
1. b. Side view X-ray: NOF of the lower leg bone near ankle, with well-defined tumor
-
2. An ossified non-ossifying fibroma on CT
Mechanism
The cause is unknown.[1] The foci consist of collagen rich connective tissue, fibroblasts, histiocytes and osteoclasts. They originate from the growth plate, and are located in adjacent parts of the metaphysis and diaphysis of long bones, most often of the legs.[3]
Treatment
Treatment is generally not required if the NOF is small, and the bone usually returns to normal. If more than half of the bone width is affected or the bone is broken, the NOF can be scraped out and bone grafting performed.[1][4]
Outcome
The outcome is good, biopsy is not usually necessary if medical imaging reveals typical findings.[1] Recurrence is rare and it does not become a cancer.[1]
Epidemiology
It is the most common tumor of bone, the exact incidence however, is unknown as most are too small to be known about.[1][7] Males are affected twice as much as females.[3] Studies of X-rays in children up to the age of 4 years, show that 22% of girls and 54% of boys have a NOF.[1] NOFs are rarely observed in adult X-rays.[1]
History
The oldest case of non-ossifying fibroma has been identified on the mandible of Qafzeh 9, an early anatomically modern human dated to 90–100 000 yrs B.P.[5]
See also
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 WHO Classification of Tumours Editorial Board, ed. (2020). "Nonossifying fibroma". Soft Tissue and Bone Tumours: WHO Classification of Tumours. Vol. 3 (5th ed.). Lyon (France): International Agency for Research on Cancer. pp. 447–448. ISBN 978-92-832-4503-2. Archived from the original on 2021-06-13. Retrieved 2021-05-11.
- ↑ 2.0 2.1 2.2 2.3 Ahn, Leah; O'Donnell, Patrick. "Non-Ossifying Fibroma - Pathology - Orthobullets". www.orthobullets.com. Archived from the original on 5 May 2021. Retrieved 5 May 2021.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 Murali, Sundaram; Ilaslan, Hakan; Holden, Darlene M. (2015). "2. An imaging approach to bone tumors". In Santini-Araujo, Eduardo; Kalil, Ricardo K.; Bertoni, Franco; Park, Yong-Koo (eds.). Tumors and Tumor-Like Lesions of Bone: For Surgical Pathologists, Orthopedic Surgeons and Radiologists. Springer. p. 15. ISBN 978-1-4471-6577-4. Archived from the original on 2021-06-27. Retrieved 2021-05-05.
- ↑ 4.0 4.1 4.2 4.3 4.4 Paulos, Jaime (2021). "Non Ossifying Fibroma". Bone Tumors: Diagnosis and Therapy Today. Springer. pp. 139–139. ISBN 978-1-4471-7501-8. Archived from the original on 2021-08-28. Retrieved 2021-08-03.
- ↑ 5.0 5.1 Coutinho Nogueira D, Dutour O, Coqueugniot H, Tillier A.-m., (2019) Qafzeh 9 mandible (ca 90–100 kyrs BP, Israel) revisited : μ-CT and 3D reveal new pathological conditions, International Journal of Paleopathology, Vol 26, pp.104-110, https://doi.org/10.1016/j.ijpp.2019.06.002 Archived 2021-08-28 at the Wayback Machine
- ↑ Bowers, Leah M.; Cohen, Donald M.; Bhattacharyya, Indraneel; Pettigrew, James C.; Stavropoulos, Mary F. (25 September 2012). "The Non-ossifying Fibroma: A Case Report and Review of the Literature". Head and Neck Pathology. 7 (2): 203–210. doi:10.1007/s12105-012-0399-7. ISSN 1936-055X. PMC 3642261. PMID 23008139.
- ↑ Choi, Joon Hyuk; Ro, Jae Y. (1 May 2021). "The 2020 WHO Classification of Tumors of Bone: An Updated Review". Advances in Anatomic Pathology. 28 (3): 119–138. doi:10.1097/PAP.0000000000000293. ISSN 1533-4031. PMID 33480599. Archived from the original on 23 May 2021. Retrieved 29 June 2021.
External links
- Wheeless' Textbook of Orthopaedics: Nonossifying Fibroma Archived 2010-02-01 at the Wayback Machine
| Classification | |
|---|---|
| External resources |