Hypophosphatasia
| Hypophosphatasia | |
|---|---|
| Other names: Phosphoethanolaminuria; Rathbun's syndrome[1] | |
 | |
| Ribbon diagram of the alkaline phosphatase protein, which is deficient in individuals with hypophosphatasia | |
| Pronunciation |
|
| Specialty | Orthopedics, pediatrics, endocrinology |
| Symptoms | Variable—may include osteopenia, skeletal hypomineralization, respiratory compromise |
| Onset | Birth |
| Duration | Lifelong |
| Types | Infantile, childhood, adult, and odontohypophosphatasia |
| Causes | Mutation of the ALPL gene[2] |
| Diagnostic method | Comprehensive metabolic panel test for serum alkaline phosphatase level; examination of X-rays; genetic tests of ALPL |
| Differential diagnosis | Osteogenesis imperfecta, congenital dwarfisms, skeletal dysplasias |
| Treatment | Asfotase alfa |
| Prognosis | Severe perinatal forms are lethal without treatment; adult forms may only show moderate symptoms |
| Frequency | Rare (1 in 100,000);[3] more common in some populations[4] |
Hypophosphatasia (HPP),[5] also called deficiency of alkaline phosphatase, phosphoethanolaminuria,[6] or Rathbun's syndrome,[1] is a rare, and sometimes fatal, metabolic bone disease.[7] Clinical symptoms are heterogeneous, ranging from the rapidly fatal, perinatal variant, with profound skeletal hypomineralization, respiratory compromise or vitamin B6 dependent seizures[5] to a milder, progressive osteomalacia later in life. Tissue non-specific alkaline phosphatase (TNSALP) deficiency in osteoblasts and chondrocytes impairs bone mineralization, leading to rickets or osteomalacia. The pathognomonic finding is subnormal serum activity of the TNSALP enzyme, which is caused by one of 388 genetic mutations identified to date, in the gene encoding TNSALP. Genetic inheritance is autosomal recessive for the perinatal and infantile forms but either autosomal recessive or autosomal dominant in the milder forms.
Hypophosphatasia's frequency is not known; though one study estimated the severe form affects 1:100,000 births.[3] Others report a higher rate of milder disease.[8]
Signs and symptoms
There is a remarkable variety of symptoms that depends, largely, on the age of the patient at initial presentation, ranging from death in utero to relatively mild bone problems with or without dentition symptoms[9] in adult life although neurological and extra-skeletal symptoms are also reported.[10] Although several clinical sub-types of the disease have been characterized, based on the age at which skeletal lesions are discovered, the disease is best understood as a single continuous spectrum of severity.
As the presentation of adult disease is highly variable, incorrect or missed diagnosis may occur.[9] In one study, 19% of patients diagnosed with fibromyalgia had laboratory findings suggestive of possible hypophosphatasia.[11]
One case report details a 35-year old female with low serum ALP and mild pains but no history of rickets, fractures or dental problems. Subsequent evaluation showed osteopenia and renal microcalcifications and an elevation of PEA. The genetic mutations found in this case were previously reported in perinatal, infantile and childhood hypophosphatasia, but not adult hypophosphatasia.[12]
Perinatal hypophosphatasia
Perinatal hypophosphatasia is the most lethal form. Profound hypomineralization results in caput membranaceum (a soft calvarium), deformed or shortened limbs during gestation and at birth, and rapid death due to respiratory failure.[13] Stillbirth is not uncommon and long-term survival is rare. Neonates who manage to survive suffer increasing respiratory compromise due to softening of the bones (osteomalacia) and underdeveloped lungs (hypoplastic). Ultimately, this leads to respiratory failure. Epilepsy (seizures) can occur and can prove lethal.[14] Regions of developing, unmineralized bone (osteoid) may expand and encroach on the marrow space, resulting in myelophthisic anemia.[citation needed]
In radiographic examinations, perinatal hypophosphatasia can be distinguished from even the most severe forms of osteogenesis imperfecta and congenital dwarfism. Some stillborn skeletons show almost no mineralization; others have marked undermineralization and severe osteomalacia. Occasionally, there can be a complete absence of ossification in one or more vertebrae. In the skull, individual bones may calcify only at their centers. Another unusual radiographic feature is bony spurs that protrude laterally from the shafts of the ulnae and fibulae. Despite the considerable patient-to-patient variability and the diversity of radiographic findings, the X-ray can be considered diagnostic.[citation needed]
Infantile hypophosphatasia
Infantile hypophosphatasia presents in the first 6 months of life, with the onset of poor feeding and inadequate weight gain. Clinical manifestations of rickets often appear at this time. Although cranial sutures appear to be wide, this reflects hypomineralization of the skull, and there is often “functional” craniosynostosis. If the patient survives infancy, these sutures can permanently fuse. Defects in the chest, such as flail chest resulting from rib fractures, lead to respiratory compromise and pneumonia. Elevated calcium in the blood (hypercalcemia) and urine (hypercalcenuria) are also common, and may explain the renal problems and recurrent vomiting seen is this disease.[15]
Radiographic features in infants are generally less severe than those seen in perinatal hypophosphatasia. In the long bones, there is an abrupt change from a normal appearance in the shaft (diaphysis) to uncalcified regions near the ends (metaphysis), which suggests the occurrence of an abrupt metabolic change. In addition, serial radiography studies suggest that defects in skeletal mineralization (i.e. rickets) persist and become more generalized. Mortality is estimated to be 50% in the first year of life.
Childhood hypophosphatasia
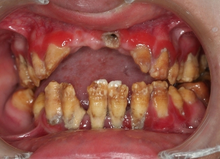
Hypophosphatasia in childhood has variable clinical expression. As a result of defects in the development of the dental cementum, the deciduous teeth (baby teeth) are often lost before the age of 5. Frequently, the incisors are lost first; occasionally all of the teeth are lost prematurely. Dental radiographs can show the enlarged pulp chambers and root canals that are characteristic of rickets.[citation needed]
Patients may experience delayed walking, a characteristic waddling gait, stiffness and pain, and muscle weakness (especially in the thighs) consistent with nonprogressive myopathy. Typically, radiographs show defects in calcification and characteristic bony defects near the ends of major long bones. Growth retardation, frequent fractures, and low bone density (osteopenia) are common. In severely-affected infants and young children, cranial bones can fuse prematurely, despite the appearance of open fontanels on radiographic studies. The illusion of open fontanels results from hypomineralization of large areas of the calvarium. Premature bony fusion of the cranial sutures may elevate intracranial pressure.[citation needed]
Adult hypophosphatasia
Adult hypophosphatasia can be associated with rickets, premature loss of deciduous teeth, or early loss of adult dentation followed by relatively good health. Osteomalacia results in painful feet due to poor healing of metatarsal stress fractures. Discomfort in the thighs or hips due to femoral pseudofractures can be distinguished from other types of osteomalacia by their location in the lateral cortices of the femora.[citation needed]
Some patients suffer from calcium pyrophosphate dihydrate crystal depositions with occasional attacks of arthritis (pseudogout), which appears to be the result of elevated endogenous inorganic pyrophosphate (PPi) levels. These patients may also suffer articular cartilage degeneration and pyrophosphate arthropathy. Radiographs reveal pseudofractures in the lateral cortices of the proximal femora and stress fractures, and patients may experience osteopenia, chondrocalcinosis, features of pyrophosphate arthropathy, and calcific periarthritis.[citation needed]
Odontohypophosphatasia
Odontohypophosphatasia is present when dental disease is the only clinical abnormality, and radiographic and/or histologic studies reveal no evidence of rickets or osteomalacia. Although hereditary leukocyte abnormalities and other disorders usually account for this condition, odontohypophosphatasia may explain some “early-onset periodontitis” cases.
Causes
Hypophosphatasia is associated with a molecular defect in the gene encoding tissue non-specific alkaline phosphatase (TNSALP). TNSALP is an enzyme that is tethered to the outer surface of osteoblasts and chondrocytes. TNSALP hydrolyzes several substances, including inorganic pyrophosphate (PPi) and pyridoxal 5’-phosphate (PLP), a major form of vitamin B6.
When TSNALP is low, inorganic pyrophosphate (PPi) accumulates outside of cells, and inhibits formation of hydroxyapatite, one of the main components of bone, causing rickets in infants and children and osteomalacia (soft bones) in adults. PLP is the principal form of vitamin B6 and must be dephosphorylated by TNSALP before it can cross the cell membrane. Vitamin B6 deficiency in the brain impairs synthesis of neurotransmitters, which can cause seizures. In some cases, a build-up of calcium pyrophosphate dihydrate (CPPD) crystals in the joint can cause pseudogout.
Genetics
Perinatal and infantile hypophosphatasia are inherited as autosomal recessive traits with homozygosity or compound heterozygosity for two defective TNSALP alleles. The mode of inheritance for childhood, adult, and odonto forms of hypophosphatasia can be either autosomal dominant or recessive. Autosomal transmission accounts for the fact that the disease affects males and females with equal frequency. Genetic counseling is complicated by the disease’s variable inheritance pattern, and by incomplete penetration of the trait.[16]
Hypophosphatasia is a rare disease that has been reported worldwide and appears to affect individuals of all ethnicities.[3] The prevalence of severe hypophosphatasia is estimated to be 1:100,000 in a population of largely Anglo-Saxon origin. The frequency of mild hypophosphatasia is more challenging to assess because the symptoms may escape notice or be misdiagnosed. The highest incidence of hypophosphatasia has been reported in the Mennonite population in Manitoba, Canada where one in every 25 individuals are considered carriers and one in every 2,500 newborns exhibits severe disease.[4] Hypophosphatasia is considered particularly rare in people of African ancestry in the U.S.[17]
Diagnosis
Teeth
Hypophosphatasia is often discovered because of an early loss of deciduous (baby or primary) teeth with the root intact. Researchers have recently documented a positive correlation between dental abnormalities and clinical phenotype. Poor dentition is also noted in adults.[18]
Laboratory testing
The symptom that best characterizes hypophosphatasia is low serum activity of alkaline phosphatase enzyme (ALP). In general, lower levels of enzyme activity correlate with more severe symptoms. The decrease in ALP activity leads to an increase in pyridoxal 5’-phosphate (PLP), which is the major form of Vitamin B6, in the blood, although tissue levels of Vitamin B6 may be unremarkable[19] and correlates with disease severity.[citation needed] Urinary inorganic pyrophosphate (PPi) levels are elevated in most hypophosphatasia patients and, although it remains only a research technique, this increase has been reported to accurately detect carriers of the disease. In addition, most patients have an increased level of urinary phosphoethanolamine (PEA) although some may not.[5] PLP screening is preferred over PEA due to cost and sensitivity.[citation needed]
Tests for serum tissue-non-specific ALP (sometimes referred to as TNSALP) levels are part of the standard comprehensive metabolic panel (CMP) that is used in routine exams, although bone-specific ALP testing may be indicative of disease severity.[20]
Radiography
Despite patient-to-patient variability and the diversity of radiographic findings, the X-ray is diagnostic in infantile hypophosphatasia.[21] Skeletal defects are found in nearly all patients and include hypomineralization, rachitic changes, incomplete vertebrate ossification and, occasionally, lateral bony spurs on the ulnae and fibulae.
In newborns, X-rays readily distinguish hypophosphatasia from osteogenesis imperfecta and congenital dwarfism. Some stillborn skeletons show almost no mineralization; others have marked undermineralization and severe rachitic changes. Occasionally there can be peculiar complete or partial absence of ossification in one or more vertebrae. In the skull, individual membranous bones may calcify only at their centers, making it appear that areas of the unossified calvarium have cranial sutures that are widely separated when, in fact, they are functionally closed. Small protrusions (or "tongues") of radiolucency often extend from the metaphyses into the bone shaft.
In infants, radiographic features of hypophosphatasia are striking, though generally less severe than those found in perinatal hypophosphatasia. In some newly diagnosed patients, there is an abrupt transition from relatively normal-appearing diaphyses to uncalcified metaphases, suggesting an abrupt metabolic change has occurred. Serial radiography studies can reveal the persistence of impaired skeletal mineralization (i.e. rickets), instances of sclerosis, and gradual generalized demineralization.
In adults, X-rays may reveal bilateral femoral pseudofractures in the lateral subtrochanteric diaphysis. These pseudofractures may remain for years, but they may not heal until they break completely or the patient receives intramedullary fixation. These patients may also experience recurrent metatarsal fractures. DXA may show abnormal bone mineral density which may correlate with disease severity, although bone mineral density in HPP patients may not be systemically reduced.[22]
Genetic analysis
All clinical sub-types of hypophosphatasia have been traced to genetic mutations in the gene encoding TNSALP, which is localized on chromosome 1p36.1-34 in humans (ALPL; OMIM#171760). Approximately 388 distinct mutations have been described in the TNSALP gene.[2] An up-to-date list of mutations is available online at The Tissue Nonspecific Alkaline Phosphatase Gene Mutations Database Archived 2016-03-04 at the Wayback Machine. About 80% of the mutations are missense mutations. The number and diversity of mutations results in highly variable phenotypic expression, and there appears to be a correlation between genotype and phenotype in hypophosphatasia”.[23] Mutation analysis is possible and available in 3 laboratories.[24]
Treatment
As of October 2015, asfotase alfa (Strensiq) has been approved by the FDA for the treatment of hypophosphatasia.
Some evidence exists to support the use of teraparatide in adult-HPP.[25][26][27][28]
Current management consists of palliating symptoms, maintaining calcium balance and applying physical, occupational, dental and orthopedic interventions, as necessary.[7]
- Hypercalcemia in infants may require restriction of dietary calcium or administration of calciuretics. This should be done carefully so as not to increase the skeletal demineralization that results from the disease itself.[29] Vitamin D sterols and mineral supplements, traditionally used for rickets or osteomalacia, should not be used unless there is a deficiency, as blood levels of calcium ions (Ca2+), inorganic phosphate (Pi) and vitamin D metabolites usually are not reduced.[30]
- Craniosynostosis, the premature closure of skull sutures, may cause intracranial hypertension and may require neurosurgical intervention to avoid brain damage in infants.[31]
- Bony deformities and fractures are complicated by the lack of mineralization and impaired skeletal growth in these patients. Fractures and corrective osteotomies (bone cutting) can heal, but healing may be delayed and require prolonged casting or stabilization with orthopedic hardware. A load-sharing intramedullary nail or rod is the best surgical treatment for complete fractures, symptomatic pseudofractures, and progressive asymptomatic pseudofractures in adult hypophosphatasia patients.[32]
- Dental problems: Children particularly benefit from skilled dental care, as early tooth loss can cause malnutrition and inhibit speech development. Dentures may ultimately be needed. Dentists should carefully monitor patients’ dental hygiene and use prophylactic programs to avoid deteriorating health and periodontal disease.[18]
- Physical Impairments and pain: Rickets and bone weakness associated with hypophosphatasia can restrict or eliminate ambulation, impair functional endurance, and diminish ability to perform activities of daily living. Nonsteroidal anti-inflammatory drugs may improve pain-associated physical impairment and can help improve walking distance[33]]
- Bisphosphonate (a pyrophosphate synthetic analog) in one infant had no discernible effect on the skeleton, and the infant’s disease progressed until death at 14 months of age.[34]
- Bone marrow cell transplantation in two severely affected infants produced radiographic and clinical improvement, although the mechanism of efficacy is not fully understood and significant morbidity persisted.[35][36]
- Enzyme replacement therapy with normal, or ALP-rich serum from patients with Paget’s bone disease, was not beneficial.[37][38]
- Phase 2 clinical trials of bone targeted enzyme-replacement therapy for the treatment of hypophosphatasia in infants and juveniles have been completed, and a phase 2 study in adults is ongoing.[39][40]
- Pyridoxine, or Vitamin B6 may be used as adjunctive therapy in some cases, which may be referred to as Pyridoxine responsive seizures.[14][41]
History
It was discovered initially in 1936 but was fully named and documented by a Canadian pediatrician, John Campbell Rathbun (1915-1972), while examining and treating a baby boy with very low levels of alkaline phosphatase in 1948. The genetic basis of the disease was mapped out only some 40 years later. Hypophosphatasia is sometimes called Rathbun's syndrome after its principal documenter.[42][1]
See also
References
- ↑ 1.0 1.1 1.2 Rogers K, Chauhan Y (2013-09-30). "Hypophosphatasia". Encyclopedia Britannica. Archived from the original on 2021-08-23. Retrieved 2021-08-23.
{{cite web}}: CS1 maint: uses authors parameter (link) - ↑ 2.0 2.1 Choida V, Bubbear JS (2019-01-01). "Update on the management of hypophosphatasia". Therapeutic Advances in Musculoskeletal Disease. 11: 1759720X19863997. doi:10.1177/1759720X19863997. PMC 6676257. PMID 31413732.
- ↑ 3.0 3.1 3.2 Fraser D (May 1957). "Hypophosphatasia". The American Journal of Medicine. 22 (5): 730–46. doi:10.1016/0002-9343(57)90124-9. PMID 13410963.
- ↑ 4.0 4.1 Greenberg CR, Taylor CL, Haworth JC, Seargeant LE, Philipps S, Triggs-Raine B, Chodirker BN (July 1993). "A homoallelic Gly317-->Asp mutation in ALPL causes the perinatal (lethal) form of hypophosphatasia in Canadian mennonites". Genomics. 17 (1): 215–7. doi:10.1006/geno.1993.1305. PMID 8406453.
- ↑ 5.0 5.1 5.2 "Hypophosphatasia". NORD (National Organization for Rare Disorders). Archived from the original on 2020-11-26. Retrieved 2020-12-24.
- ↑ "hypophosphatasia". Genetics Home Reference. Archived from the original on 2019-09-08. Retrieved 2021-09-16.
- ↑ 7.0 7.1 Whyte MP (2001). "Hypophosphatasia". In Scriver CR, Beaudet AL, Sly WS, Valle D, Vogelstein B (eds.). The Metabolic & Molecular Bases of Inherited Disease. Vol. 4 (8th ed.). New York: McGraw-Hill. pp. 5313–29. ISBN 978-0-07-913035-8.
- ↑ García-Fontana C, Villa-Suárez JM, Andújar-Vera F, González-Salvatierra S, Martínez-Navajas G, Real PJ, et al. (July 2019). "Epidemiological, Clinical and Genetic Study of Hypophosphatasia in A Spanish Population: Identification of Two Novel Mutations in The Alpl Gene". Scientific Reports. 9 (1): 9569. Bibcode:2019NatSR...9.9569G. doi:10.1038/s41598-019-46004-2. PMC 6606844. PMID 31267001.
- ↑ 9.0 9.1 Fukushima K, Kawai-Kowase K, Yonemoto Y, Fujiwara M, Sato H, Sato M, et al. (April 2019). "Adult hypophosphatasia with compound heterozygous p.Phe327Leu missense and c.1559delT frameshift mutations in tissue-nonspecific alkaline phosphatase gene: a case report". Journal of Medical Case Reports. 13 (1): 101. doi:10.1186/s13256-019-2045-4. PMC 6480864. PMID 31014398.
- ↑ Colazo JM, Hu JR, Dahir KM, Simmons JH (February 2019). "Neurological symptoms in Hypophosphatasia". Osteoporosis International. 30 (2): 469–480. doi:10.1007/s00198-018-4691-6. PMID 30215116. S2CID 52273027.
- ↑ "Hypophosphatasia May Be Misdiagnosed as Fibromyalgia: A Single Center Experience". ACR Meeting Abstracts. Archived from the original on 2021-01-06. Retrieved 2021-01-05.
- ↑ Fukushima, Kazunori; Kawai-Kowase, Keiko; Yonemoto, Yukio; Fujiwara, Makoto; Sato, Hiroko; Sato, Mahito; Kubota, Takuo; Ozono, Keiichi; Tamura, Junich (2019-04-24). "Adult hypophosphatasia with compound heterozygous p.Phe327Leu missense and c.1559delT frameshift mutations in tissue-nonspecific alkaline phosphatase gene: a case report". Journal of Medical Case Reports. 13 (1): 101. doi:10.1186/s13256-019-2045-4. ISSN 1752-1947. PMC 6480864. PMID 31014398.
- ↑ Jaruratanasirikul S, Chanvitan P (December 1999). "Hypophosphatasia: the importance of alkaline phosphatase in bone mineralization". Journal of the Medical Association of Thailand = Chotmaihet Thangphaet. 82 (12): 1268–72. PMID 10659574.
- ↑ 14.0 14.1 Baumgartner-Sigl S, Haberlandt E, Mumm S, Scholl-Bürgi S, Sergi C, Ryan L, et al. (June 2007). "Pyridoxine-responsive seizures as the first symptom of infantile hypophosphatasia caused by two novel missense mutations (c.677T>C, p.M226T; c.1112C>T, p.T371I) of the tissue-nonspecific alkaline phosphatase gene". Bone. 40 (6): 1655–61. doi:10.1016/j.bone.2007.01.020. PMID 17395561.
- ↑ "Hypophosphatasia Signs and Symptoms". Hypophosphatasia.com. Archived from the original on 15 October 2014. Retrieved 10 September 2014.
- ↑ Simon-Bouy B, Taillandier A, Fauvert D, Brun-Heath I, Serre JL, Armengod CG, et al. (November 2008). "Hypophosphatasia: molecular testing of 19 prenatal cases and discussion about genetic counseling". Prenatal Diagnosis. 28 (11): 993–8. doi:10.1002/pd.2088. PMID 18925618. S2CID 33682973.
- ↑ Whyte MP, Essmyer K, Geimer M, Mumm S (June 2006). "Homozygosity for TNSALP mutation 1348c>T (Arg433Cys) causes infantile hypophosphatasia manifesting transient disease correction and variably lethal outcome in a kindred of black ancestry". The Journal of Pediatrics. 148 (6): 753–8. doi:10.1016/j.jpeds.2006.01.031. PMID 16769381.
- ↑ 18.0 18.1 Reibel A, Manière MC, Clauss F, Droz D, Alembik Y, Mornet E, Bloch-Zupan A (February 2009). "Orodental phenotype and genotype findings in all subtypes of hypophosphatasia". Orphanet Journal of Rare Diseases. 4: 6. doi:10.1186/1750-1172-4-6. PMC 2654544. PMID 19232125.
- ↑ "Pediatric hypophosphatasia: lessons learned from a retrospective single-center chart review of 50 children". Journal of Clinical Investigation. May 1988. doi:10.1172/JCI113440. Archived from the original on 2021-09-28. Retrieved 2021-09-16.
- ↑ Whyte, M. P.; Walkenhorst, D. A.; Fedde, K. N.; Henthorn, P. S.; Hill, C. S. (June 1996). "Hypophosphatasia: levels of bone alkaline phosphatase immunoreactivity in serum reflect disease severity". The Journal of Clinical Endocrinology and Metabolism. 81 (6): 2142–2148. doi:10.1210/jcem.81.6.8964842. ISSN 0021-972X. PMID 8964842. Archived from the original on 2021-09-28. Retrieved 2021-09-16.
- ↑ Shohat M, Rimoin DL, Gruber HE, Lachman RS (1991). "Perinatal lethal hypophosphatasia; clinical, radiologic and morphologic findings". Pediatric Radiology. 21 (6): 421–7. doi:10.1007/BF02026677. PMID 1749675. S2CID 1088742.
- ↑ Genest F, Claußen L, Rak D, Seefried L (September 2020). "Bone mineral density and fracture risk in adult patients with hypophosphatasia". Osteoporosis International. 32 (2): 377–385. doi:10.1007/s00198-020-05612-9. PMC 7838076. PMID 32879991.
- ↑ Zurutuza L, Muller F, Gibrat JF, Taillandier A, Simon-Bouy B, Serre JL, Mornet E (June 1999). "Correlations of genotype and phenotype in hypophosphatasia". Human Molecular Genetics. 8 (6): 1039–46. doi:10.1093/hmg/8.6.1039. PMID 10332035.
- ↑ "geneteset.org homepage". Archived from the original on 2020-11-06. Retrieved 2022-03-05.
- ↑ Lawrence, John E.; Saeed, Danish; Bartlett, Jonathan; Carrothers, Andrew D. (2017). "Adult-onset hypophosphatasia diagnosed following bilateral atypical femoral fractures in a 55-year-old woman". Clinical Cases in Mineral and Bone Metabolism. 14 (3): 347–353. doi:10.11138/ccmbm/2017.14.3.347. ISSN 1724-8914. PMC 5762228. PMID 29354166.
- ↑ Whyte, Michael P. (April 2016). "Hypophosphatasia - aetiology, nosology, pathogenesis, diagnosis and treatment". Nature Reviews. Endocrinology. 12 (4): 233–246. doi:10.1038/nrendo.2016.14. ISSN 1759-5037. PMID 26893260. S2CID 20805434. Archived from the original on 2021-05-25. Retrieved 2021-09-16.
- ↑ Camacho, Pauline M.; Mazhari, Alaleh M.; Wilczynski, Cory; Kadanoff, Ruth; Mumm, Steven; Whyte, Michael P. (August 2016). "Adult Hypophosphatasia Treated with Teriparatide: Report of 2 Patients and Review of the Literature". Endocrine Practice. 22 (8): 941–950. doi:10.4158/EP15890.OR. ISSN 1530-891X. PMID 27042741. Archived from the original on 2021-08-29. Retrieved 2021-09-16.
- ↑ Whyte, Michael P.; Mumm, Steven; Deal, Chad (April 2007). "Adult hypophosphatasia treated with teriparatide". The Journal of Clinical Endocrinology and Metabolism. 92 (4): 1203–1208. doi:10.1210/jc.2006-1902. ISSN 0021-972X. PMID 17213282. Archived from the original on 2021-08-29. Retrieved 2021-09-16.
- ↑ Barcia JP, Strife CF, Langman CB (May 1997). "Infantile hypophosphatasia: treatment options to control hypercalcemia, hypercalciuria, and chronic bone demineralization". The Journal of Pediatrics. 130 (5): 825–8. doi:10.1016/S0022-3476(97)80029-7. PMID 9152296.
- ↑ Opshaug O, Maurseth K, Howlid H, Aksnes L, Aarskog D (May 1982). "Vitamin D metabolism in hypophosphatasia". Acta Paediatrica Scandinavica. 71 (3): 517–21. doi:10.1111/j.1651-2227.1982.tb09466.x. PMID 6291316. S2CID 25957674.
- ↑ Collmann H, Mornet E, Gattenlöhner S, Beck C, Girschick H (February 2009). "Neurosurgical aspects of childhood hypophosphatasia". Child's Nervous System. 25 (2): 217–23. doi:10.1007/s00381-008-0708-3. PMID 18769927. S2CID 9470770.
- ↑ Coe JD, Murphy WA, Whyte MP (September 1986). "Management of femoral fractures and pseudofractures in adult hypophosphatasia". The Journal of Bone and Joint Surgery. American Volume. 68 (7): 981–90. doi:10.2106/00004623-198668070-00004. PMID 3745261.
- ↑ Girschick HJ, Seyberth HW, Huppertz HI (November 1999). "Treatment of childhood hypophosphatasia with nonsteroidal antiinflammatory drugs". Bone. 25 (5): 603–7. doi:10.1016/S8756-3282(99)00203-3. PMID 10574582.
- ↑ Deeb AA, Bruce SN, Morris AA, Cheetham TD (June 2000). "Infantile hypophosphatasia: disappointing results of treatment". Acta Paediatrica. 89 (6): 730–3. doi:10.1080/080352500750044106. PMID 10914973.
- ↑ Whyte MP, Kurtzberg J, McAlister WH, Mumm S, Podgornik MN, Coburn SP, et al. (April 2003). "Marrow cell transplantation for infantile hypophosphatasia". Journal of Bone and Mineral Research. 18 (4): 624–36. doi:10.1359/jbmr.2003.18.4.624. PMID 12674323.
- ↑ Cahill RA, Wenkert D, Perlman SA, Steele A, Coburn SP, McAlister WH, et al. (August 2007). "Infantile hypophosphatasia: transplantation therapy trial using bone fragments and cultured osteoblasts". The Journal of Clinical Endocrinology and Metabolism. 92 (8): 2923–30. doi:10.1210/jc.2006-2131. PMID 17519318.
- ↑ Whyte MP, Valdes R, Ryan LM, McAlister WH (September 1982). "Infantile hypophosphatasia: enzyme replacement therapy by intravenous infusion of alkaline phosphatase-rich plasma from patients with Paget bone disease". The Journal of Pediatrics. 101 (3): 379–86. doi:10.1016/S0022-3476(82)80061-9. PMID 7108657.
- ↑ Whyte MP, McAlister WH, Patton LS, Magill HL, Fallon MD, Lorentz WB, Herrod HG (December 1984). "Enzyme replacement therapy for infantile hypophosphatasia attempted by intravenous infusions of alkaline phosphatase-rich Paget plasma: results in three additional patients". The Journal of Pediatrics. 105 (6): 926–33. doi:10.1016/S0022-3476(84)80079-7. PMID 6502342.
- ↑ "Clinical Trials website". U.S. National Institutes of Health. Archived from the original on 2018-07-04. Retrieved 2022-03-05.
- ↑ "Alexion Pharmaceuticals website". Archived from the original on 2021-04-10. Retrieved 2022-03-05.
- ↑ Güzel Nur B, Çelmeli G, Manguoğlu E, Soyucen E, Bircan İ, Mıhçı E (September 2016). "Pyridoxine-Responsive Seizures in Infantile Hypophosphatasia and a Novel Homozygous Mutation in ALPL Gene". Journal of Clinical Research in Pediatric Endocrinology. 8 (3): 360–4. doi:10.4274/jcrpe.2798. PMC 5096504. PMID 27086862.
- ↑ Taillefer D. "Our Mission". Soft Bones Canada Inc. Archived from the original on 2018-08-15. Retrieved 2021-09-16.
{{cite web}}: CS1 maint: uses authors parameter (link)
Further reading
- Rathbun JC (June 1948). "Hypophosphatasia; a new developmental anomaly". American Journal of Diseases of Children. 75 (6): 822–31. doi:10.1001/archpedi.1948.02030020840003. PMID 18110134.
- Mornet E, Nunes ME (2007). Pagon RA, Bird TD, Dolan CR, Stephens K (eds.). "Hypophosphatasia". GeneReviews. Archived from the original on 2017-01-18. Retrieved 2021-09-16.
External links
| Classification | |
|---|---|
| External resources |
- Pages with script errors
- CS1 maint: uses authors parameter
- All articles with unsourced statements
- Articles with unsourced statements from September 2021
- Articles with invalid date parameter in template
- Articles with unsourced statements from February 2021
- Webarchive template wayback links
- Enzyme defects
- Rare diseases