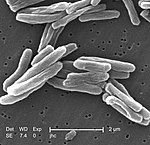
Extensively drug-resistant tuberculosis
| Extensively drug-resistant tuberculosis | |
|---|---|
 | |
| Description of extensively drug-resistant tuberculosis. | |
| Symptoms | Same as tuberculosis |
| Causes | Mycobacterium tuberculosis |
| Risk factors | Improperly treated tuberculosis |
| Diagnostic method | To evaluate drug susceptibility, the bacteria need to be cultivated and tested in a suitable laboratory. Final diagnosis in this way for TB, and especially for XDR-TB, may take from 6 to 16 weeks |
| Prevention | BCG vaccine (limited) |
| Treatment | Can be cured, but depends on extent of drug resistance, the severity of disease and if immune system is compromised. |
Extensively drug-resistant tuberculosis (XDR-TB) is a form of tuberculosis caused by bacteria that are resistant to some of the most effective anti-TB drugs. XDR-TB strains have arisen after the mismanagement of individuals with multidrug-resistant TB (MDR-TB).[1]
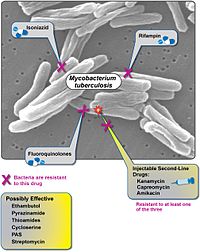
Almost one in four people in the world is infected with TB bacteria.[2] Only when the bacteria become active do people become ill with TB. Bacteria become active as a result of anything that can reduce the person's immunity, such as HIV, advancing age, or some medical conditions. TB can usually be treated with a course of four standard, or first-line, anti-TB drugs (i.e., isoniazid, rifampin and any fluoroquinolone). If these drugs are misused or mismanaged, multidrug-resistant TB (MDR-TB) can develop. MDR-TB takes longer to treat with second-line drugs (i.e., amikacin, kanamycin, or capreomycin), which are more expensive and have more side-effects. XDR-TB can develop when these second-line drugs are also misused or mismanaged and become ineffective. The World Health Organization (WHO) defines XDR-TB as MDR-TB that is resistant to at least one fluoroquinolone and a second-line injectable drug (amikacin, capreomycin, or kanamycin).[3]
The true scale of XDR-TB is unknown as many countries lack the necessary equipment and capacity to accurately diagnose it. By June 2008, 49 countries had confirmed cases of XDR-TB.[4] By the end of 2017, 127 WHO Member States reported a total of 10,800 cases of XDR-TB, and 8.5% of cases of MDR-TB in 2017 were estimated to have been XDR-TB.[3]
In August 2019, the Food and Drug Administration (FDA) approved the use of Pretomanid in combination with bedaquiline and linezolid for treating a limited and specific population of adult patients with extensively drug resistant, treatment-intolerant or nonresponsive multidrug resistant pulmonary TB.[5]
Signs and symptoms
Symptoms of XDR-TB are no different from ordinary or drug-susceptible TB: a cough with thick, cloudy mucus (or sputum), sometimes with blood, for more than two weeks; fever, chills, and night sweats; fatigue and muscle weakness; weight loss; and in some cases shortness of breath and chest pain. A person with these symptoms does not necessarily have XDR-TB, but they should see a physician for diagnosis and a treatment plan. TB patients whose symptoms do not improve after a few weeks of treatment for TB and are taking treatment should inform their clinician or nurse.[6]
XDR-TB and HIV/AIDS
TB is one of the most common infections in people living with HIV/AIDS.[7] In places where XDR-TB is most common, people living with HIV are at greater risk of becoming infected with XDR-TB, compared with people without HIV, because of their weakened immunity. If there are a lot of HIV-infected people in these places, then there will be a strong link between XDR-TB and HIV.[8]
Cause

Multiple drug resistant-TB can become resistant to the major second-line TB drug groups: fluoroquinolones (moxifloxacin, ofloxacin) and injectable aminoglycoside or polypeptide drugs (amikacin, capreomycin, kanamycin). [9]
When MDR-TB is resistant to at least one drug from each group, it is classified as extensively drug-resistant tuberculosis (XDR-TB).[9]
WHO has revised the definitions of pre-XDR-TB and XDR-TB in 2021 as following:[10]
- Pre-XDR-TB: TB caused by Mycobacterium tuberculosis (M.tuberculosis) strains that fulfill the definition of MDR/RR-TB and which are also resistant to any fluoroquinolone
- XDR-TB: TB caused by Mycobacterium tuberculosis (M. tuberculosis) strains that fulfill the definition of MDR/RR-TB and which are also resistant to any fluoroquinolone and at least one additional Group A drug
The Group A drugs are currently levofloxacin or moxifloxacin, bedaquiline and linezolid. [11]
Therefore XDR-TB is MDR/RR-TB that is resistant to a fluoroquinolone and at least one of bedaquiline or linezolid [11]
Transmission

Like other forms of TB, XDR-TB is spread through the air. When a person with infectious TB coughs, sneezes, talks or spits, they propel TB germs, known as bacilli, into the air. XDR-TB cannot be spread by kissing, sharing food or drinks, or shaking someone's hand. The bacterium has the ability to stay in the air for several hours.[13]
A person needs only to inhale a small number of these to be infected. People infected with TB bacilli will not necessarily become sick with the disease. The immune system "walls off" the TB bacilli which, protected by a thick waxy coat, can lie dormant for years.[14][15]
The spread of TB bacteria depends on factors such as the number and concentration of infectious people in any one place together with the presence of people with a higher risk of being infected (such as those with HIV/AIDS). The risk of becoming infected increases with the longer the time that a previously uninfected person spends in the same room as the infectious case.[14][16][17]
The risk of spread increases where there is a high concentration of TB bacteria, such as can occur in closed environments like overcrowded houses, hospitals or prisons; the risk will be further increased if ventilation is poor.[14][16][17]
Diagnosis

Successful diagnosis of XDR-TB depends on the patient's access to quality health-care services. If TB bacteria are found in the sputum, the diagnosis of TB can be made in a day or two, but this finding will not be able to distinguish between drug-susceptible and drug-resistant TB. To evaluate drug susceptibility, the bacteria need to be cultivated and tested in a suitable laboratory. Final diagnosis in this way for TB, and especially for XDR-TB, may take from 6 to 16 weeks.[6]
The original method used to test for MDR-TB and XDR-TB was the Drug Susceptibility Testing (DST). DST is capable of determining how well four primary antitubercular drugs inhibit the growth of Mycobacterium Tuberculosis. The four primary antitubercular drugs are Isoniazid, Rifampin, Ethambutol and Pyrazinamide.[18] Drug Susceptibility testing is done by making a Lowenstein-Jensen medium plate and spreading the bacteria on the plate.[19]
As Mycobacterium tuberculosis evolved new strains of resistant bacteria were being found such as XDR-TB. The problem was that primary DST was not suitable for testing bacteria strains that were extensively drug resistant. This problem was starting to be fixed when drug susceptibility tests started including not just the four primary drugs, but secondary drugs. This secondary test is known as Bactec MGIT 960 System.[20] Although Bactec MGIT 960 System was accurate it was still slow at determining the level of resistance.[20]Diagnosis of MDR and XDR-TB in children is challenging. With an increasing number of cases being reported worldwide there is a great need for better diagnostic tools available for pediatric patients.[21]
In recent years drug resistant tuberculosis testing has shown a lot of progress. Some studies have found an in-house assay that could rapidly detect resistance to drugs involved in the definition of XDR-TB directly from smear-positive specimens. The assay is called Reverse Line Blot Hybridization Assay also known as RLBH.[22] The study showed that the results of RLBH were as accurate as other drug susceptibility tests, but at the same time didn't take weeks to get results. RLBH testing only took 3 days to determine how resistant the strain of bacteria was.[22]
The current research has shown progress in the testing of drug resistance. A recent study found that a research technique known as direct nitrate reductase assay (D-NRA) showed efficient accuracy for the rapid and simultaneous detection of resistance to isoniazid (INH), rifampicin (RIF), kanamycin (KAN) and ofloxacin (OFL). D-NRA results were obtained in 16.9 days,[23] comparably less than other drug susceptibility testing. At the same time the study mentioned how D-NRA is a low-cost technology, easy to set up in clinical laboratories and suitable to be used for DST of M. tuberculosis in all smear-positive samples.[23]
Prevention

Countries aim to prevent XDR-TB by ensuring that the work of their national TB control programmes, and of all practitioners working with people with TB, is carried out according to the International Standards for TB Care.[24]
These emphasize providing proper diagnosis and treatment to all TB individuals, including those with drug-resistant TB; assuring regular, timely supplies of all anti-TB drugs; proper management of anti-TB drugs and providing support to such people, to maximize adherence to prescribed regimens; caring for XDR-TB cases in a centre with proper ventilation, and minimizing contact with others, particularly those with HIV, especially in the early stages before treatment has had a chance to reduce the infectiousness. Also an effective disease control infrastructure is necessary for the prevention of XDR tuberculosis. Increased funding for research, and strengthened laboratory facilities are much required. Immediate detection through drug susceptibility testing's are vital, when trying to stop the spread of XDR tuberculosis.[24][25][26]
BCG vaccine
The BCG vaccine prevents severe forms of TB in children, such as TB meningitis. It would be expected that BCG would have the same effect in preventing severe forms of TB in children, even if they were exposed to XDR-TB. The vaccine has shown to be less effective at preventing the most common strains of TB and in blocking TB in adults.[13]
Enforced quarantine
Carriers who refuse to wear a mask in public have been indefinitely involuntarily committed to regular jails, and cut off from contacting the world.[27][28] Some have run away from the USA, complaining of abuse.[29]
Treatment

The principles of treatment for MDR-TB and for XDR-TB are the same. Second-line drugs are more toxic than the standard anti-TB regimen and can cause a range of serious side-effects including hepatitis, depression, hallucinations, and deafness.[30]
People are often hospitalized for long periods, in isolation. In addition, second-line drugs are extremely expensive compared with the cost of drugs for standard TB treatment.[31]
XDR-TB is associated with a much higher mortality rate than MDR-TB, because of a reduced number of effective treatment options.[32] A 2008 study in the Tomsk oblast of Russia, reported that 14 out of 29 (48.3%) patients with XDR-TB successfully completed treatment.[33] In 2018, the WHO reported that the treatment success rate for XDR-TB was 34% for the 2015 cohort, compared to 55% for MDR/RR-TB (2015 cohort), 77% for HIV-associated TB (2016 cohort), and 82% for TB (2016 cohort).[3]
A 2018 meta-analysis of 12,030 patients from 25 countries in 50 studies has demonstrated that treatment success increases and mortality decreases when treatment includes bedaquiline, later generation fluoroquinolones, and linezolid.[34][35] One regimen for XDR-TB called Nix-TB, a combination pretomanid, bedaquiline, and linezolid,[36] has shown promise in early clinical trials.[37]
Successful outcomes depend on a number of factors including the extent of the drug resistance, the severity of the disease and whether the patient's immune system is compromised. It also depends on access to laboratories that can provide early and accurate diagnosis so that effective treatment is provided as soon as possible. Effective treatment requires that all six classes of second-line drugs be available to clinicians who have special expertise in treating such cases.[21]
The majority of people with HIV who develop TB will have drug-susceptible or ordinary TB, and can be treated with standard first-line anti-TB drugs. For those with HIV infection, treatment with antiretroviral drugs may reduce the risk of becoming infected with XDR-TB, just as it does with ordinary TB.A research study titled "TB Prevalence Survey and Evaluation of Access to TB Care in HIV-Infected and Uninfected TB Patients in Asembo and Gem, Western Kenya", says that HIV/AIDS is fueling large increases in TB incidence in Africa, and a large proportion of cases are not diagnosed.[31][16][38]
Epidemiology
Studies have found that men have a higher risk of getting XDR-TB than women.[39] One study showed that the male to female ratio was more than threefold, with statistical relevance (P<0.05)[40] Studies done on the effect of age and XDR-TB have revealed that individuals who are 65 and up are less likely to get XDR-TB.[41] A study in Japan found that XDR-TB patients are more likely to be younger.[42]
History
XDR-TB is defined as TB that has developed resistance to at least rifampicin and isoniazid (resistance to these first line anti-TB drugs defines Multi-drug-resistant tuberculosis, or MDR-TB), as well as to any member of the quinolone family and at least one of the following second-line anti-TB injectable drugs: kanamycin, capreomycin, or amikacin.[43] This definition of XDR-TB was agreed by the World Health Organization (WHO) Global Task Force on XDR-TB in October 2006.[44] The earlier definition of XDR-TB as MDR-TB that is also resistant to three or more of the six classes of second-line drugs,[32] is no longer used, but may be referred to in older publications.[45]
South African epidemic
XDR-TB was first widely publicised following the report of an outbreak in South Africa in 2006. 53 patients in a rural hospital in Tugela Ferry were found to have XDR-TB of whom 52 died.[46] The median survival from sputum specimen collection to death was only 16 days and that the majority of patients had never previously received treatment for tuberculosis suggesting that they had been newly infected by XDR-TB strains, and that resistance did not develop during treatment.[46] This was the first epidemic for which the acronym XDR-TB was used, and although TB strains that fulfill the current definition have been identified retrospectively,[47][48] this was the largest group of linked cases ever found. Since the initial report in September 2006, cases have now been reported in most provinces in South Africa. As of 16 March 2007, there were 314 cases reported, with 215 deaths.[49]
It is clear that the spread of this strain of TB is closely associated with a high prevalence of HIV and poor infection control; in other countries where XDR-TB strains have arisen, drug resistance has arisen from mismanagement of cases or poor patient compliance with drug treatment instead of being transmitted from person to person.[50] It is now clear that the problem has been around for much longer than health department officials have suggested, and is far more extensive.[51]
See also
- Multi-drug-resistant tuberculosis (MDR-TB)
- Totally drug-resistant tuberculosis (TDR-TB)
References
- ↑ "Extensively Drug-Resistant Tuberculosis (XDR TB)" (PDF). Centers for Disease Control and Prevention. Archived (PDF) from the original on 1 September 2022. Retrieved 11 September 2022.
- ↑ Houben, Rein M. G. J.; Dodd, Peter J. (25 October 2016). Metcalfe, John Z. (ed.). "The Global Burden of Latent Tuberculosis Infection: A Re-estimation Using Mathematical Modelling". PLOS Medicine. 13 (10): e1002152. doi:10.1371/journal.pmed.1002152. ISSN 1549-1676. PMC 5079585. PMID 27780211.
- ↑ 3.0 3.1 3.2 "Global tuberculosis report". World Health Organization (WHO). 28 February 2019. Archived from the original on 30 December 2013. Retrieved 18 August 2019.
- ↑ World Health Organization (2008). "Countries with XDR-TB confirmed cases as of June 2008" [1] Archived 2016-03-04 at the Wayback Machine
- ↑ "FDA approves new drug for treatment-resistant forms of tuberculosis that affects the lungs" (Press release). Food and Drug Administration (FDA). 14 August 2019. Archived from the original on 19 August 2019. Retrieved 18 August 2019.
- Lay summary in: "Scientists Discover New Cure for the Deadliest Strain of Tuberculosis". The New York Times. August 14, 2019.
- ↑ 6.0 6.1 World Health Organization (2006). "Frequently asked questions – XDR-TB" [2] Archived 2008-10-06 at the Wayback Machine
- ↑ Alexander, Paul E; De, Prithwish (2017-01-30). "The emergence of extensively drug-resistant tuberculosis (TB): TB/HIV coinfection, multidrug-resistant TB and the resulting public health threat from extensively drug-resistant TB, globally and in Canada". The Canadian Journal of Infectious Diseases & Medical Microbiology. 18 (5): 289–291. doi:10.1155/2007/986794. ISSN 1712-9532. PMC 2533560. PMID 18923728.
- ↑ Drug-resistant TB and HIV. World Health Organization. 2014. Archived from the original on 2 March 2022. Retrieved 9 September 2022.
- ↑ 9.0 9.1 Millard, James; Ugarte-Gil, Cesar; Moore, David A. J. (26 February 2015). "Multidrug resistant tuberculosis". BMJ. 350: h882. doi:10.1136/bmj.h882. ISSN 1756-1833. Archived from the original on 28 June 2022. Retrieved 8 September 2022.
- ↑ Viney, Kerri; Linh, Nguyen Nhat; Gegia, Medea; Zignol, Matteo; Glaziou, Philippe; Ismail, Nazir; Kasaeva, Tereza; Mirzayev, Fuad (2021). "New definitions of pre-extensively and extensively drug-resistant tuberculosis: update from the World Health Organization". The European Respiratory Journal. 57 (4): 2100361. doi:10.1183/13993003.00361-2021. ISSN 1399-3003. PMID 33833074. Archived from the original on 11 December 2021. Retrieved 15 March 2022.
- ↑ 11.0 11.1 "Meeting report of the WHO expert consultation on the definition of extensively drug-resistant tuberculosis". www.who.int. Archived from the original on 13 September 2022. Retrieved 11 September 2022.
- ↑ Liebenberg, Dale; Gordhan, Bhavna Gowan; Kana, Bavesh Davandra (23 September 2022). "Drug resistant tuberculosis: Implications for transmission, diagnosis, and disease management". Frontiers in Cellular and Infection Microbiology. 12. doi:10.3389/fcimb.2022.943545. ISSN 2235-2988.
- ↑ 13.0 13.1 "Extensively Drug-Resistant Tuberculosis (XDR TB)". Centers for Disease Control and Prevention (CDC). 4 May 2016. Archived from the original on 2019-04-12. Retrieved 2017-01-30.
- ↑ 14.0 14.1 14.2 Churchyard, Gavin; Kim, Peter; Shah, N. Sarita; Rustomjee, Roxana; Gandhi, Neel; Mathema, Barun; Dowdy, David; Kasmar, Anne; Cardenas, Vicky (3 November 2017). "What We Know About Tuberculosis Transmission: An Overview". The Journal of Infectious Diseases. 216 (suppl_6): S629–S635. doi:10.1093/infdis/jix362. ISSN 1537-6613. Archived from the original on 26 May 2022. Retrieved 9 September 2022.
- ↑ Shah, N. Sarita; Auld, Sara C.; Brust, James C. M.; Mathema, Barun; Ismail, Nazir; Moodley, Pravi; Mlisana, Koleka; Allana, Salim; Campbell, Angela; Mthiyane, Thuli; Morris, Natashia; Mpangase, Primrose; van der Meulen, Hermina; Omar, Shaheed V.; Brown, Tyler S.; Narechania, Apurva; Shaskina, Elena; Kapwata, Thandi; Kreiswirth, Barry; Gandhi, Neel R. (19 January 2017). "Transmission of Extensively Drug-Resistant Tuberculosis in South Africa". The New England Journal of Medicine. 376 (3): 243–253. doi:10.1056/NEJMoa1604544. ISSN 1533-4406. Archived from the original on 16 August 2022. Retrieved 15 September 2022.
- ↑ 16.0 16.1 16.2 "HIV and Tuberculosis (TB) | NIH". hivinfo.nih.gov. Archived from the original on 15 August 2022. Retrieved 18 September 2022.
- ↑ 17.0 17.1 Mathema, Barun; Andrews, Jason R.; Cohen, Ted; Borgdorff, Martien W.; Behr, Marcel; Glynn, Judith R.; Rustomjee, Roxana; Silk, Benjamin J.; Wood, Robin (3 November 2017). "Drivers of Tuberculosis Transmission". The Journal of Infectious Diseases. 216 (suppl_6): S644–S653. doi:10.1093/infdis/jix354. ISSN 1537-6613. Archived from the original on 27 July 2022. Retrieved 19 September 2022.
- ↑ Richter, Elvira; Rüsch-Gerdes, Sabine; Hillemann, Doris (2009). "Drug-susceptibility testing in TB: Current status and future prospects". Expert Review of Respiratory Medicine. 3 (5): 497–510. doi:10.1586/ers.09.45. PMID 20477339. S2CID 207222707.
- ↑ "Missouri Department of Health & Senior Services." Drug Susceptibility Testing (DST). N.p., n.d. Jan. 2014. <http://health.mo.gov/lab/dst.php Archived 2022-09-08 at the Wayback Machine>
- ↑ 20.0 20.1 Rodrigues, C.; Jani, J.; Shenai, S.; Thakkar, P.; Siddiqi, S.; Mehta, A. (2008). "Drug susceptibility testing of Mycobacterium tuberculosis against second-line drugs using the Bactec MGIT 960 System". The International Journal of Tuberculosis and Lung Disease. 12 (12): 1449–1455. PMID 19017456.
- ↑ 21.0 21.1 Salazar-Austin N, Ordonez AA, Hsu AJ, et al. (2015). "Extensively drug-resistant tuberculosis in a young child after travel to India". The Lancet Infectious Diseases. 15 (12): 1485–1491. doi:10.1016/S1473-3099(15)00356-4. PMC 4843989. PMID 26607130.
- ↑ 22.0 22.1 Ajbani, Kanchan; Shetty, Anjali; Mehta, Ajita; Rodrigues, Camilla (2011). "Rapid Diagnosis of Extensively Drug-Resistant Tuberculosis by Use of a Reverse Line Blot Hybridization Assay". Journal of Clinical Microbiology. 49 (7): 2546–2551. doi:10.1128/JCM.02511-10. PMC 3147869. PMID 21613436.
- ↑ 23.0 23.1 Imperiale BR, Morcillo NS, Palomino JC, Vandamme P, Martin A (April 2014). "Predictive value of direct nitrate reductase assay and its clinical performance in the detection of multi- and extensively drug-resistant tuberculosis". J Med Microbiol. 63 (Pt 4): 522–527. doi:10.1099/jmm.0.070219-0. PMID 24445510.
- ↑ 24.0 24.1 "WHO | International standards for tuberculosis care". www.who.int. Archived from the original on December 19, 2015. Retrieved 2017-01-30.
- ↑ "Extensively drug-resistant tuberculosis (XDR-TB): recommendations for prevention and control". Releve Epidemiologique Hebdomadaire. 81 (45): 430–432. 10 November 2006. ISSN 0049-8114. Archived from the original on 19 July 2022. Retrieved 17 September 2022.
- ↑ Brett, Kendra; Dulong, Camille; Severn, Melissa (2020). Prevention of Tuberculosis: A Review of Guidelines. Canadian Agency for Drugs and Technologies in Health. Archived from the original on 20 September 2022. Retrieved 19 September 2022.
- ↑ "Man Isolated with Deadly Tuberculosis Strain". NPR. Archived from the original on 2019-04-12. Retrieved 2022-09-05.
- ↑ "Drug-proof TB strain poses ethical bind - Health - Infectious diseases _ NBC News.htm". NBC News. Archived from the original on 2017-12-17. Retrieved 2022-09-05.
- ↑ "TB Patient Flees U.S. "Abuse" For Russia". www.cbsnews.com. Archived from the original on 2019-04-12. Retrieved 2022-09-08.
- ↑ Jason Beaubien (June 4, 2013). "Moldova Grapples With Whether To Isolate TB Patients". Special Series: Tuberculosis Returns With A Deadly Twist. NPR. Archived from the original on November 26, 2018. Retrieved January 29, 2015.
- ↑ 31.0 31.1 Treatment strategies for MDR-TB and XDR-TB. World Health Organization. 2014. Archived from the original on 18 June 2022. Retrieved 12 September 2022.
- ↑ 32.0 32.1 Center for Disease Control (2006). "Emergence of Mycobacterium tuberculosis with extensive resistance to second-line drug—Worldwide, 2000–2004". MMWR Weekly. 55 (11): 301–305.
- ↑ Keshavjee, S; Gelmanova, I; Farmer, P; Mishustin, S; Strelis, A; Andreev, Y; Pasechnikov, A; Atwood, S; et al. (2008). "Treatment of extensively drug-resistant tuberculosis in Tomsk, Russia: a retrospective cohort study". The Lancet. 372 (9647): 1403–9. doi:10.1016/S0140-6736(08)61204-0. PMID 18723218. S2CID 22875399.
- ↑ Lange, Christoph; Chesov, Dumitru; Furin, Jennifer; Udwadia, Zarir; Dheda, Keertan (2018). "Revising the definition of extensively drug-resistant tuberculosis". The Lancet Respiratory Medicine. 6 (12): 893–895. doi:10.1016/s2213-2600(18)30428-4. ISSN 2213-2600. PMID 30420247. S2CID 53292407.
- ↑ Collaborative Group for the Meta-Analysis of Individual Patient Data in MDR-TB treatment–2017; Ahmad, Nafees; Ahuja, Shama D (2018-09-08). "Treatment correlates of successful outcomes in pulmonary multidrug-resistant tuberculosis: an individual patient data meta-analysis". Lancet. 392 (10150): 821–834. doi:10.1016/S0140-6736(18)31644-1. ISSN 1474-547X. PMC 6463280. PMID 30215381.
- ↑ "Nix-TB". TB Alliance. 19 July 2015. Archived from the original on 12 April 2019. Retrieved 5 September 2022.
- ↑ Cohen, Jon (2017). "Simpler, safer treatment hailed as 'breakthrough' against drug-resistant TB". Science. doi:10.1126/science.aal0769. S2CID 242708581.
- ↑ Fitzgerald, Monica; Health, JH Bloomberg School of Public. "TB Western Kenya". Johns Hopkins Bloomberg School of Public Health. Archived from the original on 20 September 2022. Retrieved 20 September 2022.
- ↑ Flor de Lima, Bárbara; Tavares, Margarida (22 July 2013). "Risk factors for extensively drug-resistant tuberculosis: a review". The Clinical Respiratory Journal. 8 (1): 11–23. doi:10.1111/crj.12044. ISSN 1752-6981. PMID 23875862. S2CID 205036864.
- ↑ Velayati, Ali Akbar; Masjedi, Mohammad Reza; Farnia, Parissa; Tabarsi, Payam; Ghanavi, Jalladein; Ziazarifi, Abol Hassan; Hoffner, Sven Eric (2009). "Emergence of New Forms of Totally Drug-Resistant Tuberculosis Bacilli". Chest. 136 (2): 420–425. doi:10.1378/chest.08-2427. PMID 19349380.
- ↑ Shah, N. Sarita; Pratt, R.; Armstrong, L.; Robison, V.; Castro, K. G.; Cegielski, J. P. (2008). "Extensively Drug-Resistant Tuberculosis in the United States, 1993-2007". JAMA. 300 (18): 2153–2160. doi:10.1001/jama.300.18.2153. PMID 19001626.
- ↑ Murase, Yoshiro; Maeda, Shinji; Yamada, Hiroyuki; Ohkado, Akihiro; Chikamatsu, Kinuyo; Mizuno, Kazue; Kato, Seiya; Mitarai, Satoshi (2010). "Clonal Expansion of Multidrug-Resistant and Extensively Drug-Resistant Tuberculosis, Japan". Emerging Infectious Diseases. 16 (6): 948–954. doi:10.3201/eid1606.091844. PMC 3086214. PMID 20507745.
- ↑ "WHO Global Task Force outlines measures to combat XDR-TB worldwide". World Health Organization (WHO). 17 October 2006. Archived from the original on October 17, 2006. Retrieved 18 August 2019.
- ↑ "Report of the Meeting of the WHO Global Task Force on XDR-TB" (PDF). 2006. Archived (PDF) from the original on 2017-02-02. Retrieved 2022-09-05.
- ↑ Centers for Disease Control and Prevention (2006). "Notice to Readers: Revised Definition of Extensively Drug-Resistant Tuberculosis". JAMA: The Journal of the American Medical Association. 296 (23): 2792. doi:10.1001/jama.296.23.2792-a.
- ↑ 46.0 46.1 Gandhi, NR; Moll, A; Sturm, AW; Pawinski, Robert; Govender, Thiloshini; Lalloo, Umesh; Zeller, Kimberly; Andrews, Jason; Friedland, Gerald (2006). "Extensively drug-resistant tuberculosis as a cause of death in patients co-infected with tuberculosis and HIV in a rural area of South Africa". The Lancet. 368 (9547): 1575–80. doi:10.1016/S0140-6736(06)69573-1. PMID 17084757. S2CID 12590249.
- ↑ Shah NS, Wright A, Drobniewski F, Rusch-Gerdes S, Havelkova M, Gilpin C (2005). "Extreme drug resistance in tuberculosis (XDR-TB): Global survey of supranational reference laboratories for Mycobacterium tuberculosis with resistance to second-line drugs". International Journal of Tuberculosis and Lung Disease. 9 (Suppl 1): S77.
- ↑ "Emergence of Mycobacterium tuberculosis with extensive resistance to second-line drugs-worldwide, 2000-2004". Morb Mortal Wkly Rep. 55: 301–5. 2006.
- ↑ Angela Quintal. "314 XDR-TB cases reported in SA". Cape Times. Retrieved on 2007-04-04.
- ↑ Migliori, Giovanni Battista; Ortmann, Johannes; Girardi, Enrico; Besozzi, Giorgio; Lange, Christoph; Cirillo, Daniela M.; Ferrarese, M.; De Iaco, Giuseppina; Gori, Andrea (May 2007). "Extensively Drug-resistant Tuberculosis, Italy and Germany". Emerging Infectious Diseases. 13 (5): 780–782. doi:10.3201/eid1305.070200. ISSN 1080-6040. PMC 2738462. PMID 18044040.
- ↑ Sidley, P. (2006). "South Africa acts to curb spread of lethal strain of TB". Br Med J. 333 (7573): 825. doi:10.1136/bmj.333.7573.825-a. PMC 1618468. PMID 17053232.
External links
- World Health Organization Stop TB Department
- International Standards of TB Care
- Video: Drug-Resistant TB in Russia Archived 2011-06-05 at the Wayback Machine July 24, 2007, Woodrow Wilson Center event featuring Salmaan Keshavjee and Murray Feshbach
- TB Drug Resistance Mutation Database Archived 2012-02-20 at the Wayback Machine
- British Red Cross helps combat TB
- The Strange, Isolated Life of a Tuberculosis Patient in the 21st Century Archived 2022-01-21 at the Wayback Machine