Retained products of conception
| Retained products of conception | |
|---|---|
| Other names: Retained placenta | |
 | |
| MRI showing retained products of conception in the first trimester[1] | |
| Specialty | Obstetrics |
| Symptoms | Bleeding, infection[2] |
| Causes | Uterine atony, placenta accreta, early closure of the cervix[2] |
| Risk factors | Multiple prior deliveries, previous surgery of the uterus, preterm delivery[2] |
| Diagnostic method | Based on symptoms, examination of the placenta[3] |
| Differential diagnosis | Gestational trophoblastic disease[4] |
| Treatment | Oxytocin, dilation and curettage, manual removal[3][2][4] |
| Frequency | 2% of term pregnancies[2] |
Retained products of conception (RPOC) is when part or all of the placenta or membranes remain in the uterus in association with significant bleeding or for more than about 30 to 60 minutes following delivery of the baby.[2][3] The condition may also occur after miscarriage or abortion.[4] Symptoms may include postpartum bleeding, either at the time of delivery or later, pelvic pain, or infection.[3][2][4]
Causes can include uterine atony, placenta accreta, or early closure of the cervix.[2] Risk factors include multiple prior deliveries, previous surgery of the uterus, and preterm delivery.[2] The underlying mechanism may involved failed separation of the placenta from the uterus or a separated but retained placenta.[3] Diagnosis can be supported by symptoms or examination of the placenta for missing parts.[3] Other measures may include ultrasound.[4]
Treatment is generally by manual removal of the products under anesthesia or by dilation and curettage.[3][2][4] Injecting the cord with oxytocin may be of benefit but requires further study as of 2020.[3][5] Blood loss may require blood transfusions, uterine balloon tamponade, or hysterectomy.[2] In rural areas of the developing world, it is associated with a 10% risk of death.[6] It affects about 2% of term pregnancies; though may affect up to 40% of preterm pregnancies.[2][4]
Signs and symptoms
Symptoms of retained placenta include bleeding and infection. After the placenta is delivered, the uterus should contract down to close off all the blood vessels inside the uterus. If the placenta only partially separates, the uterus cannot contract properly, so the blood vessels inside will continue to bleed.[7]
Management
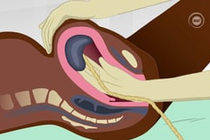
Treatment, such as intraumbilical oxytocin, are often used in management of placental retention.[9] It is useful to ensure the bladder is empty.[10] However, ergometrine should not be given as it causes tonic uterine contractions which may delay placental expulsion.[10]
Controlled cord traction has been recommended as a second alternative after more than 30 minutes have passed after stimulation of uterine contractions, provided the uterus is contracted.[10] Manual extraction may be required if cord traction also fails,[10] or if heavy ongoing bleeding occurs. There is currently uncertainty about the effectiveness of anaesthesia or analgesia for manual extraction, in terms of pain and the risk of postpartum haemorrhage.[11] Very rarely a curettage is necessary to ensure that no remnants of the placenta remain (in rare conditions with very adherent placenta such as a placenta accreta).
It is common to wait for the placenta's birth up to 2 hours in some instances.
Other animals
Retention of fetal membranes (afterbirth) is observed more frequently in cattle than in other animals. In a normal condition, a cow’s placenta is expelled within a 12-hour period after calving.[12]
See also
References
- ↑ Balachandran, G. "Incomplete miscarriage (MRI) | Radiology Case | Radiopaedia.org". Radiopaedia. Archived from the original on 16 December 2023. Retrieved 20 February 2024.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 Perlman, NC; Carusi, DA (2019). "Retained placenta after vaginal delivery: risk factors and management". International journal of women's health. 11: 527–534. doi:10.2147/IJWH.S218933. PMID 31632157.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 "GPnotebook". gpnotebook.com. Archived from the original on 19 February 2024. Retrieved 19 February 2024.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 Radswiki, The. "Retained products of conception | Radiology Reference Article | Radiopaedia.org". Radiopaedia. Archived from the original on 16 December 2023. Retrieved 19 February 2024.
- ↑ "WHO recommendation on umbilical vein injection of oxytocin for the treatment of retained placenta". World Health Organization. 2020. PMID 33263970. Archived from the original on 22 February 2024. Retrieved 20 February 2024.
{{cite journal}}: Cite journal requires|journal=(help) - ↑ Weeks, AD (August 2001). "The retained placenta". African health sciences. 1 (1): 36–41. PMID 12789132.
- ↑ Retained placenta Archived 2023-11-09 at the Wayback Machine, April 2015, BabyCenter, L.L.C.
- ↑ "Manual Removal of the Placenta - ORB". health-orb.org. Retrieved 19 February 2024.
- ↑ Duffy, James (2014). "What is the optimal pharmacological management of retained placenta?". BMJ. 349: g4778. doi:10.1136/bmj.g4778. PMID 25069774. S2CID 220110807. Archived from the original on 2024-02-19. Retrieved 2023-11-08.
- ↑ 10.0 10.1 10.2 10.3 Maternity - Prevention, Early Recognition & Management of Postpartum Haemorrhage (PPH) Archived 2017-01-20 at the Wayback Machine From Department of Health, NSW. 21-Oct-2010
- ↑ Kongwattanakul, K; Rojanapithayakorn, N; Laopaiboon, M; Lumbiganon, P (12 June 2020). "Anaesthesia/analgesia for manual removal of retained placenta". The Cochrane Database of Systematic Reviews. 6: CD013013. doi:10.1002/14651858.CD013013.pub2. PMC 7388333. PMID 32529658.
- ↑ "Retained Placentas" (PDF). Archived (PDF) from the original on 2012-07-17. Retrieved 2023-11-08.