Nasopharyngeal angiofibroma
| Nasopharyngeal angiofibroma | |
|---|---|
| Other names: Juvenile nasopharyngeal angiofibroma[1][2] | |
 | |
| Micrograph of a nasopharyngeal angiofibroma H&E stain. | |
| Specialty | ENT surgery |
| Usual onset | Adolescent males[3] |
| Diagnostic method | Medical imaging[3] |
| Frequency | Rare, 1 in 1,500000 (incidence)[3] |
Nasopharyngeal angiofibroma, also known as juvenile nasal angiofibroma, is a non-cancerous, locally aggressive vascular tumor of the nasopharynx.[3]
It arises from the superior margin of the sphenopalatine foramen and grows in the back of the nasal cavity. It can invade the nose, cheek, orbit (frog face deformity), or brain.[4] Diagnosis is by medical imaging; X-ray, CT scan, MRI, angiography.[3]
It is rare.[3] It most commonly affects adolescent males.[3] Hippocrates described the condition in the fifth century.[3]
Signs and symptoms
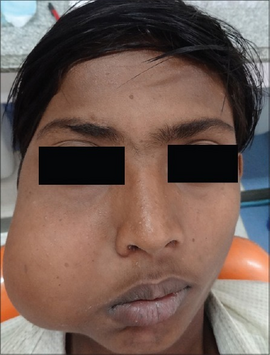
The clinical presentation of this condition is as follows:[citation needed]
- Frequent chronic epistaxis or blood-tinged nasal discharge
- Nasal obstruction and rhinorrhea
- Facial dysmorphism (when locally invasive)
- Conductive hearing loss from eustachian-tube obstruction
- Diplopia, which occurs secondary to erosion into superior orbital fissure and due to third and sixth nerve palsy.
- Proptosis when having intraorbital extension.
- Rarely anosmia, recurrent otitis media, and eye pain.
Diagnosis
If nasopharyngeal angiofibroma is suspected based on physical examination (a smooth vascular submucosal mass in the posterior nasal cavity of an adolescent male), imaging studies such as CT or MRI should be performed. Biopsy should be avoided as to avoid extensive bleeding since the tumor is composed of blood vessels without a muscular coat.[citation needed]
Antral sign or Holman-Miller sign (forward bowing of posterior wall of maxilla) is pathognomic of angiofibroma.[citation needed]
DSA (digital subtraction angiography) of carotid artery to see the extension of tumors and feeding vessels[citation needed]
Differential diagnosis
- Antro-choanal polyp (benign non neoplastic growth)[5]
- Rhinosporidiosis (as bleeding point is here too)
- Malignancy—nasopharyngeal carcinoma, lymphoma, plasmacytoma, rhabdomyosarcoma
- Chordoma
- Nasopharyngeal cyst
- Pyogenic granuloma
Staging
There are many different staging- systems published.[6] One of the most used is that of Radkowsky:[7]
| Stage | Tumor Extension |
|---|---|
| IA | Limited to the nose or the nasopharynx |
| IB | Extension into one or more paranasal sinus |
| IIA | Minimal extension through sphenopalatine foramen into and including a minimal part of the medial-most part of pterygomaxillary fossa |
| IIB | Full involvement of the pterygomaxillary fossa, displacing posterior wall of maxillary antrum forward. Lateral or anterior displacement of the branches of maxillary artery. Superior extension may occur, eroding the orbital bones |
| IIC | Extension through the pterygomaxillary fossa into the cheek and temporal fossa or posterior to the pterygoid plates |
| IIIA | Erosion of the skull base with minimal intracranial extension |
| IIIB | Erosion of skull base with extensive intracranial involvement with or without cavernous sinus involvement |
Treatment
Treatment for Nasopharyngeal angiofibroma (JNA) is primarily surgical. The tumor is primarily excised by external or endoscopic approach. Medical treatment and radiation therapy are only of historical interest.[citation needed]
External approaches:[citation needed]
- transpalatine approach
- transpalatine + sublabial (Sardana's) Approach
- infratemporal Approach
- nasal endoscopic Approach
- transmaxillary Approach
- maxillary swing Approach or Facial translocation
Endoscopic approach is an excellent tool in primary and recurrent JNA, it allows visualisation and precise removal of the lesion. Preoperative embolisation of tumour may be of some use in reducing intraoperative bleeding.[citation needed]
Direct visualization is not common-[citation needed]
- If the tumor is limited to nasopharynx and nose, for endoscopic approach or Wilson's transpalatal approach is used. It can be extended into Sardana's approach if the tumor extends laterally.
- For tumors of infratemporal fossa, Maxillary Swing approach is used.
- Transmaxillary Le Fort 1 approach is used for tumors extending into maxillary and ethmoid sinuses and pterygopalatine fossa.
- If the tumor extend up to the cheek, for Weber–Ferguson approach should be used.
Prognosis
Prognosis for nasopharyngeal angiofibroma is favorable. Because these tumors are benign, metastasis to distal sites does not occur. However, these tumors are highly vascularized and grow rapidly. Removal is important in preventing nasal obstruction and recurrent epistaxis. Mortality is not associated with nasopharyngeal angiofibroma.[8]
References
- ↑ 00021 at CHORUS
- ↑ "juvenile nasopharyngeal angiofibroma" at Dorland's Medical Dictionary
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 Midyett, F. Allan; Mukherji, Suresh K. (2020). "Juvenile Nasopharyngeal Angiofibroma". Skull Base Imaging: The Essentials. Springer International Publishing: 91–96. doi:10.1007/978-3-030-46447-9_15. Archived from the original on 2023-04-29. Retrieved 2023-04-29.
- ↑ Raphael Rubin; David S. Strayer; Emanuel Rubin (2008). Rubin's Pathology: clinicopathologic foundations of medicine. Lippincott Williams & Wilkins. pp. 1071–. ISBN 978-0-7817-9516-6. Retrieved 29 June 2010.
- ↑ Tos, Mirko; Larsen, Per L.; Larsen, Knud; Cayé-Thomasen, Per (2000), Stamm, Aldo Cassol; Draf, Wolfgang (eds.), "Nasal Polyps", Micro-endoscopic Surgery of the Paranasal Sinuses and the Skull Base, Springer Berlin Heidelberg, pp. 103–125, doi:10.1007/978-3-642-57153-4_8, ISBN 9783642571534
- ↑ Alshaikh, Nada Ali; Eleftheriadou, Anna (2015). "Juvenile nasopharyngeal angiofibroma staging: An overview". Ear, Nose, & Throat Journal. 94 (6): E12–22. doi:10.1177/014556131509400615. ISSN 1942-7522. PMID 26053985. Archived from the original on 2021-09-29. Retrieved 2021-04-19.
- ↑ Radkowski, D.; McGill, T.; Healy, G. B.; Ohlms, L.; Jones, D. T. (1996). "Angiofibroma. Changes in staging and treatment". Archives of Otolaryngology–Head & Neck Surgery. 122 (2): 122–129. doi:10.1001/archotol.1996.01890140012004. ISSN 0886-4470. PMID 8630204. Archived from the original on 2015-04-25. Retrieved 2021-04-19.
- ↑ Textbook of Family Medicine, 8th Edition. Chapter 19 p.329. Rakel, MD. ISBN 978-1-4377-1160-8
External links
| Classification | |
|---|---|
| External resources |