Idiopathic short stature
| Idiopathic short stature | |
|---|---|
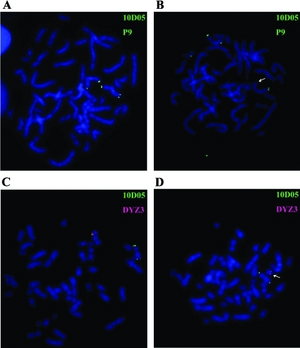 | |
| a-d) FISH analyses (Flourescent in-situ hybridization) of individuals with idiopathic short stature | |
Idiopathic short stature (ISS) refers to extreme short stature that does not have a diagnostic explanation (idiopathic designates a condition that is unexplained or not understood) after an ordinary growth evaluation. The term has been in use since at least 1975[1] without a precise percentile or statistical definition of "extreme".
Signs and symptoms
The clinical presentation is a poor adult height with no identifiable disorder/cause.[2]
Diagnosis
Definition
In 2003 Eli Lilly and Company offered a more precise definition of ISS when the pharmaceutical company submitted clinical trial data to the U.S. Food and Drug Administration (FDA) requesting approval to advertise their brand of growth hormone for the treatment of ISS.[3] They proposed a definition of a height more than 2.25 standard deviations below mean, roughly equal to the shortest 1.2% of the population. [4]
Other researchers have described a cutoff of 2.0 standard deviations.[5]
Treatment
There is some evidence that hormone treatment may not result in a significant improvement in psychosocial functioning.[6]
It is estimated that it would cost US$100,000 or more [7] to treat someone, but might only move them from the first percentile to perhaps the 10th. There is some ethical and economic concern whether such treatment would merely shift discrimination to the next most effected percentile.[citation needed]The use of insulin-like growth factor 1[8] or aromatase inhibitors[9] have been proposed as an alternative to growth hormone.
Advantage
Short stature decreases risk of venous insufficiency.[10]
See also
References
- ↑ Sizonenko PC, Rabinovitch A, Schneider P, Paunier L, Wollheim CB, Zahnd G (1975). "Plasma growth hormone, insulin, and glucagon responses to arginine infusion in children and adolescents with idiopathic short stature, isolated growth hormone deficiency, panhypopituitarism, and anorexia nervosa". Pediatr. Res. 9 (9): 733–8. doi:10.1203/00006450-197509000-00010. PMID 1105371.
- ↑ Cooke, David W.; Divall, Sara A.; Radovick, Sally (1 January 2011). "CHAPTER 24 - Normal and Aberrant Growth". Williams Textbook of Endocrinology (Twelfth Edition). W.B. Saunders. pp. 935–1053. ISBN 978-1-4377-0324-5. Retrieved 4 September 2022.
- ↑ Leschek EW, Rose SR, Yanovski JA, et al. (2004). "Effect of growth hormone treatment on adult height in peripubertal children with idiopathic short stature: a randomized, double-blind, placebo-controlled trial". J. Clin. Endocrinol. Metab. 89 (7): 3140–8. doi:10.1210/jc.2003-031457. PMID 15240584.
{{cite journal}}: CS1 maint: url-status (link) - ↑ "Idiopathic Short Stature: The FDA and Its High-Stakes Conceptual Quagmires". Michigan Technology Law Review. Michigan Technology Law Review. Archived from the original on 24 June 2021. Retrieved 23 June 2021.
- ↑ Bonioli E, Tarò M, Rosa CL, et al. (2005). "Heterozygous mutations of growth hormone receptor gene in children with idiopathic short stature". Growth Horm. IGF Res. 15 (6): 405–10. doi:10.1016/j.ghir.2005.08.004. PMID 16213173.
- ↑ Visser-van Balen H, Sinnema G, Geenen R (2006). "Growing up with idiopathic short stature: psychosocial development and hormone treatment; a critical review". Arch. Dis. Child. 91 (5): 433–9. doi:10.1136/adc.2005.086942. PMC 2082749. PMID 16632673.
- ↑ Lee JM, Davis MM, Clark SJ, Hofer TP, Kemper AR (2006). "Estimated cost-effectiveness of growth hormone therapy for idiopathic short stature". Arch Pediatr Adolesc Med. 160 (3): 263–9. doi:10.1001/archpedi.160.3.263. PMID 16520445. Archived from the original on 2011-08-10. Retrieved 2021-10-25.
- ↑ Savage MO, Camacho-Hübner C, David A, et al. (2007). "Idiopathic short stature: will genetics influence the choice between GH and IGF-I therapy?". Eur. J. Endocrinol. 157 Suppl 1: S33–7. doi:10.1530/EJE-07-0292. PMID 17785695.
- ↑ Damiani D, Damiani D (2007). "Pharmacological management of children with short stature: the role of aromatase inhibitors". J Pediatr (Rio J). 83 (5 Suppl): S172–7. doi:10.2223/JPED.1699. PMID 17901908.
- ↑ "Tall height". Archived from the original on 2020-07-30. Retrieved 2021-10-25.
External links
| Classification |
|---|