AL amyloidosis
| AL amyloidosis | |
|---|---|
| Other names: Primary systemic amyloidosis (PSA), primary amyloidosis | |
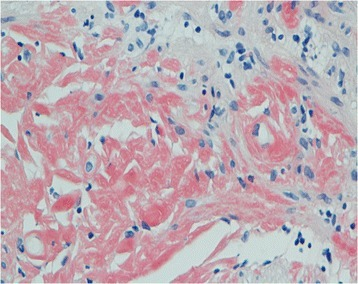 | |
| Primary systemic amyloidosis initially presenting with digestive symptoms-gastric mucosa showed orange-red positivity | |
| Specialty | Hematology |
Amyloid light-chain (AL) is a type of amyloidosis, which may present with small bumps in the skin, lungs, urinary tract, and gastrointestinal tracts.[1]
The disease is caused when a person's antibody-producing cells do not function properly and produce abnormal protein fibers made of components of antibodies called light chains. These light chains come together to form amyloid deposits which can cause serious damage to different organs.[2][3] Abnormal light chains in urine are sometimes referred to as "Bence Jones protein".
It is the most common form of systemic amyloidosis in the US.[4]
Signs and symptoms
AL amyloidosis can affect a wide range of organs, and consequently present with a range of symptoms. The kidneys are the most commonly affected organ in AL amyloidosis. Symptoms of kidney disease and kidney failure can include fluid retention, swelling, and shortness of breath.[5]
In addition to kidneys, AL amyloidosis may affect the heart, peripheral nervous system, gastrointestinal tract, blood, lungs and skin. Heart complications, which affect more than a third of AL patients, include heart failure and irregular heart beat. Other symptoms can include stroke, gastrointestinal disorders, enlarged liver, diminished spleen function, diminished function of the adrenal and other endocrine glands, skin color change or growths, lung problems, bleeding and bruising problems, fatigue, and weight loss.[5][6]
Causes
AL amyloidosis is caused by the deposition of abnormal antibody free light chains. The abnormal light chains are produced by monoclonal plasma cells, and, although AL amyloidosis can occur without diagnosis of another disorder, it is often associated with other plasma cell disorders, such as multiple myeloma and Waldenström's macroglobulinemia.[5] About 10% to 15% of patients with multiple myeloma may develop overt AL amyloidosis.[7]
Diagnosis
Both blood and the urine can be tested for the light chains, which may form amyloid deposits, causing disease. However, the diagnosis requires a sample of an affected organ.[5][8] Other diagnosis can be tissue biopsy. Tissue biopsy tests a tissue sample to look for amyloid deposits. The tissue is stained with red dye, and under a microscopic examination, amyloid proteins can be detected if the tissue turns an apple-green color. [9]
Treatment
The most effective treatment is autologous bone marrow transplants with stem cell rescues. However many patients are too weak to tolerate this approach.[10][11]
Other treatments can involve application of chemotherapy similar to that used in multiple myeloma.[11] A combination of melphalan and dexamethasone has been found effective in those who are ineligible for stem cell transplantation,[10] and a combination of bortezomib and dexamethasone is now in widespread clinical use.[12][13]
Prognosis
Median survival for patients diagnosed with AL amyloidosis was 13 months in the early 1990s, but had improved to c. 40 months a decade later.[14]
Epidemiology
AL amyloidosis is a rare disease; only 1200 to 3200 new cases are reported each year in the United States. Two thirds of patients with AL amyloidosis are male and less than 5% of patients are under 40 years of age.[5][15]
See also
References
- ↑ Johnstone, Ronald B. (2017). "14. Cutaneous deposits". Weedon's Skin Pathology Essentials (2nd ed.). Elsevier. p. 285. ISBN 978-0-7020-6830-0. Archived from the original on 2021-05-25. Retrieved 2022-09-27.
- ↑ "Amyloidosis Causes, Diagnosis, Symptoms, and Treatment on MedicineNet.com". Archived from the original on 2022-02-05. Retrieved 2022-03-15.
- ↑ "Amyloidosis and Kidney Disease". National Institute of Diabetes and Digestive and Kidney Diseases. Archived from the original on 20 November 2011. Retrieved 23 November 2011.
- ↑ Gertz MA (June 2004). "The classification and typing of amyloid deposits". Am. J. Clin. Pathol. 121 (6): 787–9. doi:10.1309/TR4L-GLVR-JKAM-V5QT. PMID 15198347. Archived from the original on 2016-05-30.
- ↑ 5.0 5.1 5.2 5.3 5.4 UNC. "AL Amyloidosis". UNC. Archived from the original on 22 December 2011. Retrieved 22 November 2011.
- ↑ "Amyloidosis". University of Maryland Medical Center. Archived from the original on 30 November 2011. Retrieved 23 November 2011.
- ↑ Madin, Sumit; Dispenzieri, Angela (2010). "Clinical Features and Treatment Response of Light Chain (AL) Amyloidosis Diagnosed in Patients With Previous Diagnosis of Multiple Myeloma". Mayo Clinic Proceedings. 83 (3): 232–238. doi:10.4065/mcp.2009.0547. PMC 2843113. PMID 20194151.
- ↑ Sanchorawala, Vaishali (2006). "Light-Chain (AL) Amyloidosis: Diagnosis and Treatment". Clinical Journal of the American Society of Nephrology. 1 (6): 1334–1341. doi:10.2215/cjn.02740806. PMID 17699366. Archived from the original on 19 November 2011. Retrieved 1 December 2011.
- ↑ "AL Amyloidosis". Amyloidosis Foundation. Archived from the original on 9 January 2022. Retrieved 9 January 2022.
- ↑ 10.0 10.1 Palladini G, Perfetti V, Obici L, et al. (April 2004). "Association of melphalan and high-dose dexamethasone is effective and well tolerated in patients with AL (primary) amyloidosis who are ineligible for stem cell transplantation". Blood. 103 (8): 2936–8. doi:10.1182/blood-2003-08-2788. PMID 15070667.
- ↑ 11.0 11.1 "BU: Amyloid Treatment & Research Program". Archived from the original on 2008-07-20.
- ↑ Chakra P. Chaulagain, MD; Raymond L. Comenzo, MD (May 2015). "How We Treat Systemic Light-Chain Amyloidosis". Clinical Advances in Hematology & Oncology. 13 (5): 315–24. PMID 26352777.
- ↑ Kastritis E, Anagnostopoulos A, Roussou M, et al. (October 2007). "Treatment of light chain (AL) amyloidosis with the combination of bortezomib and dexamethasone". Haematologica. 92 (10): 1351–8. doi:10.3324/haematol.11325. PMID 18024372.
- ↑ Ashutosh D. Wechalekar (2007). "Perspectives in treatment of AL amyloidosis". British Journal of Haematology. 140 (4): 365–377. doi:10.1111/j.1365-2141.2007.06936.x. PMID 18162121.
- ↑ "Primary AL". Amyloidosis Foundation. Archived from the original on 3 October 2011. Retrieved 23 November 2011.
External links
| Classification | |
|---|---|
| External resources |